request an appointment online.
- Diagnosis & Treatment
- Cancer Types
- Leukemia
Get details about our clinical trials that are currently enrolling patients.
View Clinical TrialsLeukemia is an umbrella term for several different cancers of the blood and the blood-forming tissues of the body. All start with problems in the creation of blood cells.
Leukemia is an umbrella term for several different cancers of the blood and the blood-forming tissues of the body. All start with problems in the creation of blood cells.
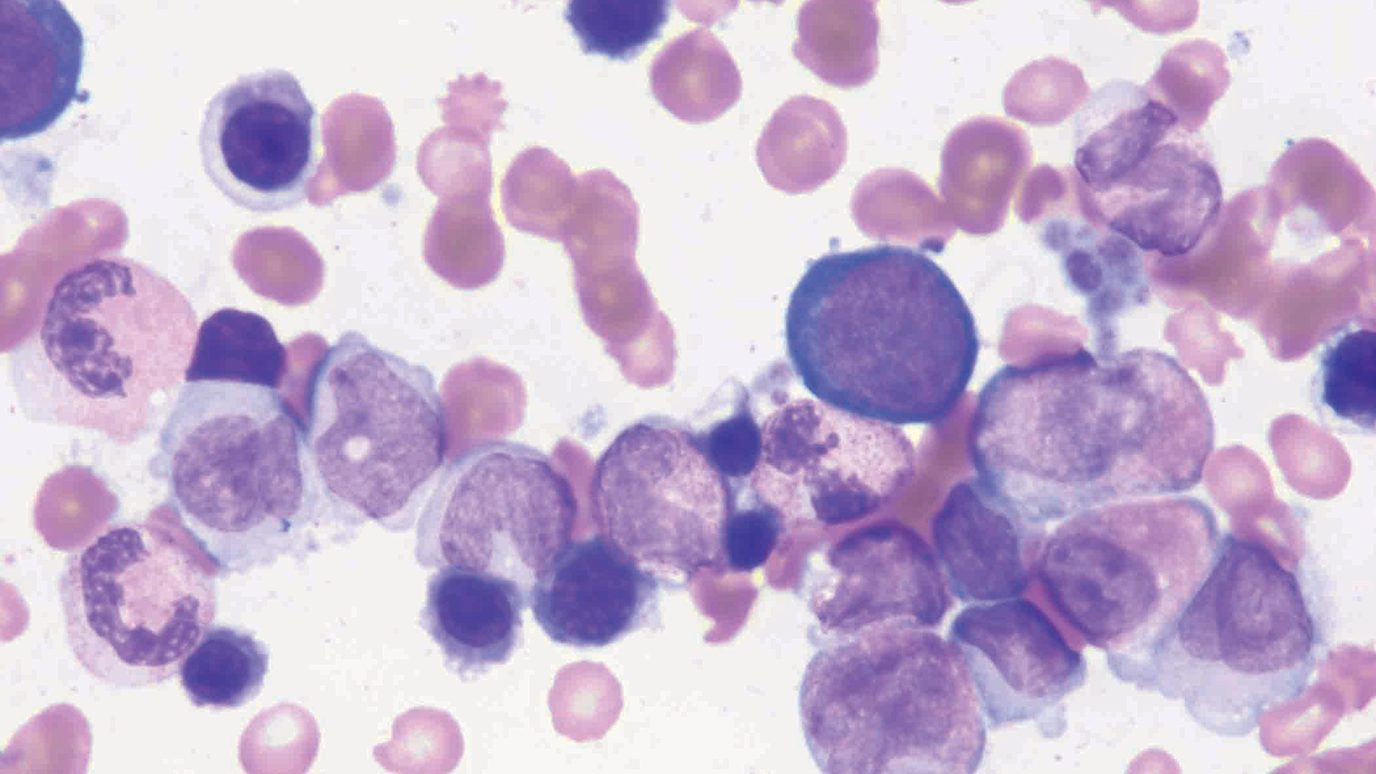
Blood cell creation
The body produces millions of blood cells each day. Most develop in the bone marrow, the spongy interior of bones that contains immature stem cells.
In a healthy person, these immature stem cells first become either lymphoid stem cells or myeloid stem cells.
Lymphoid stem cells develop into white blood cells, which are immune system cells. They start by becoming immature white blood cells known as lymphoblasts, then mature into lymphocytes. The two types of lymphocytes that are usually involved in leukemia are B cells and T cells. B cells produce the antibodies responsible for attacking bacteria and viruses that invade the body. T cells help alert other immune cells to the presence of infection or fight infection directly.
Myeloid stem cells also develop into white blood cells. The myeloid stem cells first become immature white blood cells known as myeloblasts. They then mature into monocytes and granulocytes, including neutrophils, all of which fight disease. Other myeloid stem cells develop into red blood cells, which carry oxygen throughout the body; and platelets, which help the blood clot.
Leukemia occurs when the DNA (the genetic instructions that control cell activity) of a bone marrow stem cell mutates at some point in its development. The cell becomes cancerous, begins multiplying rapidly and crowds out healthy cells in the blood and bone marrow. These diseased cells can also gather in specific parts of the body, including the liver, lymph nodes, spleen and skin.
How is leukemia classified?
While there are many types of leukemia, they are typically classified by the type of stem cell that has turned cancerous, either lymphoid or myeloid.
Many types are also classified as either chronic or acute. Acute leukemia impacts immature cells, preventing them from developing and carrying out their function. These cells tend to multiply rapidly, making acute leukemia more aggressive.
Chronic leukemia involves mature or partially mature cells. These cells multiply more slowly and are less aggressive, making chronic leukemia less aggressive than acute leukemia.
Learn more about leukemia:
Types of leukemia
Acute lymphocytic leukemia (ALL)
ALL is an aggressive form of leukemia that develops from immature lymphoid stem cells. It can impact adult and pediatric patients. Learn more about childhood ALL and adult ALL.
Acute myeloid leukemia (AML)
AML is an aggressive type of leukemia developing from lymphoid stem cells. Like ALL, both adults and children can develop AML, though the prognosis is different for the two groups. Learn more about childhood AML and adult AML.
Chronic lymphocytic leukemia (CLL)
CLL is a slow-growing type of leukemia. It develops from lymphoid stem cells that are further along in their development than ALL cells. This disease primarily impacts older patients and is nearly unheard of in children. Learn more about CLL.
Chronic myeloid leukemia (CML)
CML grows from more mature myeloid stem cells. It is a slower growing form of leukemia. Treatment for the disease has advanced rapidly over the past few decades. It is rare in children and is usually diagnosed in older adults. Learn more about CML.
B-Cell prolymphocytic leukemia (B-PLL)
B-PLL is a rare leukemia developing from B cells, a type of white blood cell, that rapidly multiply. The disease can be difficult to diagnose and is often confused with other bone marrow and blood cancers, including different leukemias and lymphomas.
The disease is typically aggressive, though around 10% of patients do not have any symptoms when they are diagnosed. Instead of immediate treatment, in some cases doctors recommend active surveillance, in which the disease is closely monitored. Treatment begins when the disease advances to a set point.
When treatment is needed, options include chemotherapy and targeted therapy.
Blastic plasmacytoid dendritic cell neoplasm (BPDCN)
BPDCN is an aggressive subtype of acute leukemia that impacts approximately 500 to 1,000 people in the U.S. each year. Though it can affect people of any age, the disease is most common among older patients, with about half of new diagnoses coming in patients age 70 or older. Historically, it has been associated with poor survival rates.
BPDCN is a cancer of a specific type of cell known as plasmacytoid dendritic cells. This rare type of immune system cell is usually found in the skin, bone marrow, blood, lymph nodes and spleen. As a result, symptoms usually can impact these areas. Skin lesions are the most common BPDCN symptom. These can show up anywhere on the body but often appear on the arms, legs, face and neck. Other symptoms include low counts of healthy blood cells and swollen lymph nodes.
Traditionally, BPDCN has been treated with chemotherapy, while younger, fitter patients have been given the option of a stem cell transplant. The Food and Drug Administration has recently approved a new targeted therapy drug that attacks CD123, a molecule commonly found on the surface of BPDCN cells. This targeted therapy is now considered a standard treatment for the disease. Learn more about BPDCN.
Chronic myelomonocytic leukemia (CMML)
CMML is a rare, slow-growing type of leukemia that mainly impacts people in their 60s and older. Patients with CMML have low counts of healthy blood cells and high counts of diseased monocytes. Monocytes are a type of white blood cell that helps other immune system cells respond to infection. They also surround and consume bacteria that invade the body.
About 1,100 CMML cases are diagnosed in the U.S. each year. In 15% to 30% of patients, the disease will progress to acute myeloid leukemia.
CMML is typically treated with stem cell transplantation, which can cure the disease, or chemotherapy, which can’t cure the disease but can kill cancer cells and make room for healthy blood cells to develop. To address low blood counts, patients can also receive blood transfusions and drugs that stimulate the growth of healthy blood cells.
Hairy cell leukemia
In hairy cell leukemia, lymphoid stem cells produce too many diseased B cells. These cells have thin growths on their surface that look like hairs, giving the disease its name. The disease typically is diagnosed in patients age 50 and older and is more likely to arise in males.
Hairy cell leukemia is typically slow to develop and progress. In some cases, it may never progress at all. Because of this, doctors often recommend active surveillance in which they closely monitor the disease. Other treatments include chemotherapy, immunotherapy and targeted therapy.
Juvenile myelomonocytic leukemia (JMML)
Juvenile myelomonocytic leukemia (JMML) is a rare type of leukemia, mostly found in children age 4 and younger. In JMML, the diseased cells are monocytes, a type of white blood cell. JMML is faster growing than chronic leukemia and slower growing than acute. It shares many symptoms with other types of leukemia, including a pale complexion, fever and infections.
Since JMML cells gather in certain organs, symptoms can also include an enlarged spleen and difficulty breathing caused by cancer cells accumulating in the lungs. A stem cell transplant is the recommended treatment for JMML, though about half of patients who undergo a successful transplant relapse.
Large granular lymphocytic leukemia (LGLL)
LGLL is a rare leukemia that develops from mature T cells or natural killer (NK) cells. Both are lymphocytes, white blood cells that help fight disease.
In LGLL, the diseased T cells or NK cells begin to multiply rapidly, crowding out healthy cells.
This leukemia is primarily diagnosed in older patients. In about 20% of cases, the patient also has an autoimmune disorder such as rheumatoid arthritis.
Though the NK cell version can be more aggressive than the T cell version, LGLL in general is slow growing. Because of this, doctors may recommend active surveillance, in which the disease is closely monitored, instead of immediate treatment. Treatment begins when the disease advances to a set point.
Because LGLL involves the overproduction of immune system cells, it is often treated with drugs meant to suppress the immune system. Chemotherapy is another treatment option. Patients are also given medicines to treat cytopenias, or low counts of healthy blood cells.
Systemic mastocytosis (SM)
Systemic mastocytosis (SM) is a rare blood disorder in which the body
makes too many mast cells, a type of immune system cell. These cells can build
up in organs, most commonly the bone marrow, but also the skin, liver, spleen,
gastrointestinal tract and lymph nodes. Learn more about systemic mastocytosis.
T-cell prolymphocytic leukemia (T-PLL)
T-cell prolymphocytic leukemia is an aggressive, extremely rare form of leukemia involving T-lymphoid stem cells.
The cause of T-PLL is not known, but recent research has uncovered several chromosome and genetic abnormalities associated with the disease. These abnormalities can be used to help diagnose T-PLL and could lead to the development of new treatments for the disease.
Much like CLL, T-PLL can be slow growing when it is first diagnosed. In most cases, though, it progresses to a more advanced, aggressive disease. Symptoms include high white blood cell counts; enlarged lymph nodes, liver and spleen; rashes; and an accumulation of fluid around the lungs and heart.
The recommendation for early, slow-growing T-PLL is active surveillance. During this phase, the patient does not receive treatment, but is closely monitored for signs that the disease is advancing. When these signs develop, T-PLL needs to be treated rapidly, often in the hospital.
While there are no medications specifically approved for T-PLL, a monoclonal antibody drug produces a high response rate. Doctors recommend a stem cell transplantation for patients who are in remission and eligible for the procedure.
Leukemia risk factors
- Sex: Men are more likely to develop leukemia than women.
- Age: Most types of leukemia impact older adults, though some are common among pediatric patients.
- Past treatment with chemotherapy or radiation therapy for a previous cancer: While these therapies can cause leukemia, their benefits as cancer treatments far outweigh their risks.
- Family history: People with a parent, sibling or child who have certain types leukemia are more likely to develop the disease.
- Myeloproliferative neoplasms (MPNs): MPNs are chronic cancers of the bone marrow and blood. While they are not classified as leukemia, MPNs (especially myelofibrosis) can transform to acute myeloid leukemia. MPNs are treated in the Leukemia Center by our experts at the Clinical Research Center for Myeloproliferative Neoplasms. Learn more about MPNs.
- Genetic disorders: Individuals with certain genetic disorders are at a higher risk of developing leukemia. These include:
- Ataxia telangiectasia
- Bloom syndrome
- Down syndrome
- Fanconi anemia
- Klinefelter syndrome
- Li-Fraumeni syndrome, a hereditary cancer syndrome
- Wiskott-Aldrich syndrome
- Chemical exposure: Long-term exposure to benzene, a chemical used in the petroleum industry, can cause leukemia. People who have been exposed to Agent Orange, which was used in the Vietnam War, are also at an increased risk for leukemia.
- Radiation exposure: After World War II, people in Japan who were exposed to radiation from nuclear bombs were more likely to develop leukemia. People who have been exposed to radiation through accidents at nuclear power plants also have a higher chance of developing leukemia.
Some cases of leukemia can be passed down from one generation to the next. Genetic counseling may be right for you. Learn more about the risk to you and your family on our genetic testing page.
Frequently asked questions
What is leukemia?
Leukemia is an umbrella term for cancers of the blood and the blood-forming tissues of the body. These cancers start with problems in the creation of blood cells. There are many types of leukemia, including lymphoid, myeloid, chronic, and acute.
What causes leukemia?
Leukemia is caused by a mutation in the DNA of a bone marrow stem cell at some point in its development. When this mutation occurs, the cell becomes cancerous, begins multiplying rapidly, and crowds out healthy cells in the blood and bone marrow.
Is leukemia curable?
Leukemia is curable in some cases. Patients who remain in remission (meaning no cancer is detectable in the body) for an extended period are considered cured. This means they have an extremely low chance of recurrence. For leukemia, complete remission usually means that the patient’s bone marrow has no detectable microscopic evidence of the disease and their blood counts have returned to normal.
How is leukemia diagnosed?
A leukemia diagnosis usually starts with a simple blood test, called a complete blood count. If the test shows the presence of leukemia cells or abnormal levels of red blood cells, white blood cells, or platelets, doctors may order a biopsy, genetic and molecular testing, lumbar puncture, or imaging exams to get a definitive leukemia diagnosis.
Is leukemia genetic?
Yes, in some cases, leukemia is related to genetics. People with a parent, sibling, or child who has certain types of leukemia are more likely to develop the disease. People with certain genetic disorders are also at a higher risk of developing leukemia.
Is leukemia cancer?
Yes, leukemia is a type of cancer. Leukemia is an umbrella term for cancers of the blood and the blood-forming tissues of the body. These cancers start with problems in the creation of blood cells.
What are the symptoms of leukemia?
Leukemia symptoms include weakness, tiredness, and fatigue; fever and frequent infections; excessive sweating or night sweats; easy bleeding or bruising; recurrent nosebleeds; petechiae (tiny red spots on the skin); shortness of breath; swollen lymph nodes; loss of appetite; unexplained weight loss; bone and joint pain; and longer than normal or heavier than normal menstruation.
Is leukemia treatable?
Yes, leukemia is treatable with chemotherapy, radiation therapy, stem cell transplantation, CAR T-cell therapy, targeted therapy, and other methods. The goal of leukemia treatment is to put the disease into remission (where no cancer is detectable in the patient’s body) and, ultimately, to cure the patient.
What do leukemia spots look like?
Leukemia can cause petechiae, a rash-like collection of pinpoint red spots on the skin. Petechiae are caused by bleeding into the skin and low levels of platelets. Learn more about petechiae and other skin rashes associated with leukemia.
Is leukemia contagious?
Leukemia is not contagious. It can be genetic and may be passed down from one generation to the next in some cases, but leukemia is not caused by a virus or other contagious substance. Leukemia occurs when the DNA of a bone marrow stem cell mutates at some point in its development so that the cell becomes cancerous, begins multiplying rapidly, and crowds out healthy cells in the blood and bone marrow.
What causes leukemia in children?
Leukemia in children is caused by a mutation in the DNA of a bone marrow stem cell at some point in its development. The cell becomes cancerous, begins multiplying rapidly, and crowds out healthy cells in the blood and bone marrow. Risk factors include exposure to X-rays before birth, certain past cancer treatments, certain genetic disorders, a family history of leukemia, and chemical exposure.
UT MD Anderson is #1 in Cancer Care

Leukemia nurse fulfills promise to her late mother
For Clinical Nurse Mikela Pettigrew, MD Anderson is more than a workplace – it’s a place of healing, hope and a promise fulfilled.
“MD Anderson is the reason my father is a cancer survivor, and it gave my mother five extra years,” she says. “It’s also the reason I became a nurse.”
While she was a teenager, both her parents were diagnosed with cancer. Her mother, Christine, faced terminal kidney cancer, while her father, Mike, was treated for colorectal cancer. Thanks to MD Anderson, Pettigrew’s mother got to see her graduate from high school.
Sitting at her mother’s bedside, Pettigrew found her purpose and made a promise: she would become a nurse at MD Anderson.
Caring with heart and purpose
Pettigrew has been a leukemia nurse on MD Anderson’s G16 unit for over five years, caring for patients with the same skill and compassion she experienced firsthand.
“I treat all my patients like they are my parents,” she says. “I want them to feel accepted, loved and at home here.”
Pettigrew’s purpose now extends beyond the bedside. As chair of MD Anderson’s Nursing Practice Congress, she is passionate about elevating the oncology nursing profession by collaborating with nurses and colleagues to improve patient care and advance nursing practice. Pettigrew splits her time between patient care on the leukemia unit and leading initiatives to amplify nurses’ voices in decision-making. Her enthusiasm has only grown with the establishment of the Meyers Institute for Oncology Nursing in November 2023.
Shaping the future of oncology nursing
Through a generous donation from Howard Meyers and additional philanthropic gifts, MD Anderson has invested $50 million toward the Meyers Institute, which is dedicated to building strong educational, professional, scientific, innovative and wellness-based programs to advance oncology nursing throughout the institution.
“The Meyers Institute is a game-changer,” says Pettigrew. “It’s an investment in our future as nurses and in the patients who depend on us.”
Pettigrew sees firsthand how oncology nursing contributes to remarkable advancements in leukemia treatments, with patients now living longer and benefiting from groundbreaking therapies.
For her, every step forward is a fulfillment of the promise she made to her mother, a source of hope for her patients and an example of why her purpose matters.
“There are many more wins than losses,” she says. “Every day, we’re getting closer to ending cancer.”

Common leukemia symptoms: What to look for
Some cancer symptoms are fairly straightforward. With breast cancer, it’s often a lump. With skin cancer, it may be a mole that changes shape or a strange-looking sore that won’t heal.
But because blood cancers like leukemia affect the entire body, their symptoms can often be mistaken for signs of other conditions. So, it’s usually a number of symptoms taken together that lead to a formal leukemia diagnosis.
Common leukemia symptoms
Leukemia symptoms can vary, based on whether the leukemia is lymphocytic or myeloid, and whether the disease is considered “chronic” (slow-growing) or “acute” (sudden-onset).
However, some symptoms are common to most types of leukemia:
- Abnormal blood counts – could be a very high white cell count or a very low platelet count; this has to do with the functioning of your immune system/propensity for infections
- Bleeding/bruising – spontaneous bleeding either internally or externally (often from the nose or gums); bruising very easily
- Fatigue – sometimes a low-level fatigue that’s not relieved by sleep or rest; other times, a sudden-onset exhaustion; often cannot be distinguished from other causes of fatigue
- Fever – may be constant low-level fevers or a sudden spike in temperature
- Infections – could be a sequence of infections or a single infection that’s resistant to treatment
- Shortness of breath – often due to low platelet count, which reduces the blood’s oxygen-carrying capacity
- Breakdown of the skin – lesions/rashes that do not resolve, bleeding/bruising of the skin, infections
Acute leukemia symptoms can often appear suddenly
With acute leukemia, symptoms tend to develop very quickly. You may suddenly spike a fever that won’t go away, develop an infection for no apparent reason, or start bleeding spontaneously from your nose or gums and not be able to stop it. You may also just wake up feeling wiped out one morning, or find yourself so exhausted that it’s hard to function.
This is the way we tend to see most of our acute leukemia patients. Often, they show up at the hospital extremely ill and need to start treatment right away.
Sometimes, we’re able to spot acute leukemia before it gets to that point, though, because the people who develop it are already patients at MD Anderson and under close observation. Patients who’ve been treated with chemotherapy or high doses of radiation therapy for previous cancers, for instance, can sometimes develop secondary blood cancers as a result: acute myeloid leukemia or myelodysplastic syndrome being the most common.
So, if a blood test shows that a breast cancer survivor’s platelets are low during a routine check-up, for example, then we know to start looking for that.
Chronic leukemia symptoms are more subtle
Chronic leukemia symptoms can also involve infections, bleeding and fatigue. But they tend to develop more slowly than with acute leukemia cases, so they’re not as noticeable. Symptoms are often attributed to other things, too, such as stress, allergies or a virus.
Sometimes, patients with chronic leukemia finally seek a doctor’s help because they can’t shake an infection, they’re feeling short of breath, or their low-level fatigue just won’t go away. But these patients are also identified through routine bloodwork that’s done for other reasons. You might discover you have leukemia at an annual physical, for instance, or because you need clearance for an upcoming orthopedic surgery or are simply changing insurance providers.
Again, the key is to listen to your body. Get to know what is normal and abnormal for you. And if something isn’t quite right, get it checked out. It’s important to listen to the clues your body may be giving you.
Why I’m optimistic about leukemia treatment advances
Regardless of which type of leukemia you might have, there is much cause for hope.
One reason is that chronic leukemia is being caught more frequently now, both because doctors see more cases of it and know what to look for, and because cancer survivors are living longer than ever after their initial diagnoses and treatment. That means patients who develop leukemia as a result of receiving chemotherapy or radiation therapy for other cancers can be identified earlier, when the disease is often easier to treat.
Another encouraging development is that the Food and Drug Administration (FDA) has approved several drugs in the past five years, many of which are oral therapies targeting various genetic mutations in patients with acute myeloid leukemia.
These breakthroughs are the direct result of scientific advances made based on cutting-edge research. Many – if not all – of these drugs were developed through clinical trials led by doctors here at MD Anderson.
And a lot of leukemia patients being prescribed these medications today didn’t even have an oral option available until just a few years ago. Now, these treatments can be administered at home. And that is definite progress.
Request an appointment at MD Anderson online or by calling 1-877-632-6789.

A leukemia survivor’s perspective on aligning care with what matters most
When Britt Mayo received a phone call from his doctor at 7:15 a.m. after a routine physical, he knew it wouldn’t be good news.
“I remember hearing the diagnosis and my brain going completely blank,” he says. “In that moment, my world shrank. I went from long-term life plans to wondering if I’d make it to the next year.”
Diagnosed with chronic lymphocytic leukemia (CLL) in 2010, Britt quickly realized that understanding his treatment options wasn’t enough. He needed his care team to understand what mattered most to him.
Protecting what matters most
Britt’s top priority was clear: live as long as possible — without compromising the parts of life that defined who he was.
Protecting the function of his hands was essential for the lifelong pianist and computer user. He wanted to avoid neuropathy. He also hoped to prevent cognitive side effects, such as chemobrain, that could affect his work and thinking. With family spread across the globe, travel mattered deeply to him and his wife, Diana.
At the time, the standard treatment for CLL involved chemotherapy. Britt was hesitant. Through open conversations with his care team, he learned about an emerging clinical trial that might be available in the future, allowing him to potentially avoid chemotherapy.
Together, he and his care team developed a watch-and-wait strategy designed to safely delay treatment until he could qualify for the clinical trial.
Why early conversations about cancer care matter
Looking back, Britt believes those early conversations were critical.
“If I had received even one round of chemotherapy, I would have been ineligible for the trial,” he says. “That conversation changed everything.”
Britt eventually enrolled in an immunotherapy clinical trial and achieved remission — without compromising his life expectancy or the activities he valued most.
Today, immunotherapy has become a standard treatment for many patients with CLL. For Britt, aligning care with his priorities brought emotional relief as well as clinical benefits.
“Before we had that conversation, there was tension between what I wanted and what I thought I had to do,” he says. “Once the plan matched my goals, I felt at ease. That’s a liberating feeling.”
He has since spoken with hundreds of fellow patients during clinical trials and clinic visits. Many, he says, didn’t realize they had choices.
“I can’t tell you how many times people told me they didn’t know there were options,” he says. “Early communication could have sent them down a very different path.”
He emphasizes that every diagnosis is different. Some cancers have multiple treatment options, while others require a specific approach.
“At a place like UT MD Anderson that has deep experience and offers many treatment approaches, patients often have options,” he says. “But even when choices are limited, understanding a patient’s goals helps the care team support quality of life, symptom management and family needs.”
Why choose UT MD Anderson for your leukemia treatment?
Choosing the right cancer center may be the most important decision you can make as a leukemia patient. At UT MD Anderson’s Leukemia Center and Stem Cell Transplantation and Cellular Therapy Center, you’ll get treatment from one of nation’s the largest, most experienced leukemia teams at a top-ranked cancer center.
Using a comprehensive team approach, we work together to give you customized care that includes the most advanced diagnostic methods and treatments. These include clinical trials of new drugs and drug combinations. We offer clinical trials for all situations – from patients receiving their first treatment, to patients who have exhausted all standard treatment options.
As a leading center for leukemia care, we offer access to innovative new therapies and clinical trials that may help increase your chances for successful treatment. Many of these were developed by our own researchers.
Treatment designed specifically for you
Successful leukemia treatment begins with accurate and precise diagnosis. Many of our leukemia patients have been misdiagnosed before they come to UT MD Anderson. We have the expertise and experience gained from being one of the most active programs in the world, and our specialized pathologists are highly skilled in diagnosing leukemia.
Our approach to leukemia is customized especially for you. We carefully evaluate your risk factors and the specific characteristics of your leukemia to determine if immediate treatment is necessary. If it is, we recommend the most effective therapies while aiming to limit treatment side effects.
Whether you are treated as an inpatient or outpatient, our comprehensive program offers all the services needed to care for leukemia and respond to its impact on your body. We aim to accomplish as much care as possible on an outpatient basis. If hospitalization is needed, our expert staff is specially trained to care for patients at every phase of the treatment journey.
UT MD Anderson is my hope. I know that without it, I wouldn’t be alive today.
Kenneth Woo
Survivor
Treatment at UT MD Anderson
Featured Articles

Rare double-hit leukemia survivor: ‘Go straight to UT MD Anderson’
5 things to know about clonal hematopoiesis

Leukemia specialists: How advances in measurable residual disease (MRD) are improving cancer care

Personalized treatment helps retired physician overcome dual cancer diagnoses
What’s new in leukemia research?
What is composite remission?
Clinical Trials
UT MD Anderson patients have access to clinical trials offering promising new treatments that cannot be found anywhere else.
Becoming Our Patient
Get information on patient appointments, insurance and billing, and directions to and around UT MD Anderson.
myCancerConnection
Talk to someone who shares your cancer diagnosis and be matched with a survivor.
Prevention & Screening
Many cancers can be prevented with lifestyle changes and regular screening.
Counseling
UT MD Anderson has licensed social workers to help patients and their loved ones cope with cancer.
Help #EndCancer
Give Now
Donate Blood
Our patients depend on blood and platelet donations.
Shop UT MD Anderson
Show your support for our mission through branded merchandise.