request an appointment online.
- Diagnosis & Treatment
- Cancer Types
- Stomach Cancer
Get details about our clinical trials that are currently enrolling patients.
View Clinical TrialsStomach cancer, or gastric cancer, is a rare but potentially dangerous form of cancer. Because stomach cancer symptoms can be mistaken for less serious problems such as indigestion or heartburn, stomach cancer is often not found until its advanced stages.
Stomach cancer, or gastric cancer, is a rare but potentially dangerous form of cancer. Because stomach cancer symptoms can be mistaken for less serious problems such as indigestion or heartburn, stomach cancer is often not found until its advanced stages.
What is stomach cancer?
Many times, people refer to the entire region between the hips and chest as the stomach. In medical terms, however, the word ‘stomach’ refers only to the muscular, sac-like organ that sits in the upper abdomen.
After you chew and swallow food, it moves through a hollow tube called the esophagus into the stomach. There, the stomach mixes this food with gastric juices to begin the digestion process.
Stomach cancer occurs when the cells in the stomach's lining divide uncontrollably, forming a tumor. As cancer progresses, the tumor may invade and destroy surrounding tissue, block the passage of food, or break off and spread (metastasize) to other organs.
Around the world, the majority of stomach cancer cases affect the main portion of the stomach, called the body. Stomach cancer can also affect the distal stomach, close to where the stomach meets the small intestine. In the United States, stomach cancer usually affects the gastroesophageal junction (also known as the cardia), where the stomach meets the esophagus. While the rates of stomach cancer, in general, are declining, cancers in the gastroesophageal junction are increasing.
Stomach cancer types
There are different types of stomach cancer, depending on the cells in which cancer starts. These include:
Adenocarcinomas: Adenocarcinoma refers to cancer that starts in gland cells. The cancer begins in the stomach’s mucosal —or inner— layer and grows outward, invading the other layers of the stomach wall. This is the most common type of stomach cancer, accounting for 90% of all stomach cancer cases.
Gastrointestinal stromal tumors (GIST): Cancer that affects a type of cells (Interstitial cells of Cajal) in the gastrointestinal tract, most often the stomach or small intestine. They are also called gastric sarcomas.
Carcinoid tumors: Carcinoid tumors affect the hormone-producing cells of the stomach. They are also called neuroendocrine tumors.
Stomach cancer statistics
According to the National Cancer Institute, an estimated 27,600 new cases of stomach cancer will be diagnosed in the United States in 2020. More than 60% of these diagnoses will be for people age 65 or older. The five-year survival rate for the disease is 32%. Because stomach cancer symptoms can be mistaken for less serious problems such as indigestion or heartburn, stomach cancer is often not found until its advanced stages. This can lead to worse outcomes.
Stomach cancer risk factors
Although the exact cause of stomach cancer is not known, certain factors seem to increase your risk of developing the disease. These include:
Gender: The majority of stomach cancer patients are male.
Age: Most individuals who develop stomach cancer are older than 55, although stomach cancer can be diagnosed in younger individuals. According to the National Cancer Institute, the median age at diagnosis is 68 years old.
Ethnicity: In the United States, stomach cancer occurs more often in Hispanic Americans, African Americans, and Asian/Pacific Islanders than in non-Hispanic whites.
Geography: Stomach cancer is more prevalent in Japan, China, Southern and Eastern Europe, and Central and South America than in Northern and Western Africa, South Central Asia, and North America. This may be due to differences in diet, the rate of infection with Helicobacter pylori (a type of bacteria), and the environment.
Infection with Helicobacter pylori (H. pylori): This type of bacteria is a common cause of stomach ulcers and may cause chronic inflammation in the stomach lining. This sometimes leads to pre-cancerous changes in cells, increasing the risk of stomach cancer.
Exposure to chemicals: People who work around certain chemicals have a higher risk for stomach cancer. These include:
- Those working in the rubber, metal, coal and timber industries
- Those who have been exposed to asbestos fibers
Obesity: People who are obese have a higher risk of cancer in the part of the stomach nearest the esophagus.
Tobacco and alcohol abuse: Smoking and drinking excessive amounts of alcohol appear to increase the likelihood of cancer in the upper part of the stomach. Some studies have shown that smoking doubles the risk of stomach cancer.
Food preservation and improper food storage and preparation: Eating foods preserved through pickling, salting and drying or that contain nitrates can be a risk factor. Eating foods that have not been stored or prepared correctly is also a risk factor.
Medical conditions: Having any of the following may increase your risk for stomach cancer:
- Pernicious anemia
- Chronic stomach inflammation (gastritis) and intestinal polyps
- Acid reflux or chronic indigestion
- Menetrier disease
- Epstein-Barr virus infection
- History of stomach lymphoma, a type of cancer that affects the lymph nodes, which are small, bean-shaped organs that help transport immune cells and remove waste from tissue
- Type A blood
- Prior stomach surgery
Family history: In rare cases, stomach cancer can be passed down from one generation to the next. Additionally, if close relatives have had stomach cancer or have hereditary cancer syndromes such as Hereditary Diffuse Gastric Cancer syndrome (caused by CDH1 mutation), hereditary non-polyposis colon cancer (HNPCC) or Li-Fraumeni syndrome, you may be at a higher risk of stomach cancer. Genetic testing may be used to identify genetic predisposition for stomach cancer.
Not everyone with risk factors gets stomach cancer. However, if you have risk factors, you should discuss them with your doctor.
Learn more about stomach cancer:
Learn more about clinical trials for stomach cancer.
UT MD Anderson is #1 in Cancer Care
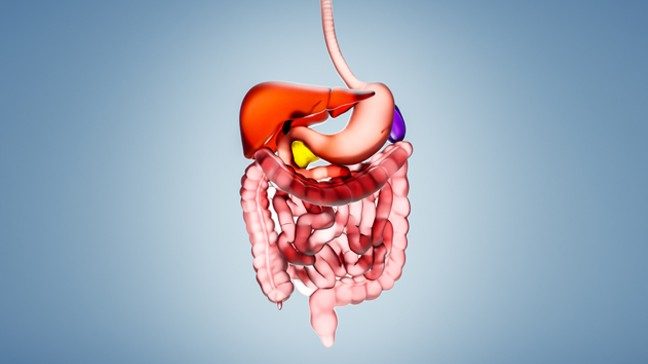
Gastrointestinal stromal tumors (GISTs): What are they, and how are they treated?
A gastrointestinal stromal tumor is a type of sarcoma that develops in the connective tissue of the gastrointestinal tract. It’s often referred to as GIST.
GISTs are usually found in adults between the ages of 30 and 50. Though rare, GISTs can also be found in children and young adults.
We spoke with sarcoma medical oncologist Neeta Somaiah, M.D., to learn more about this rare type of cancer, including how it develops, how it’s treated and if it’s curable.
Where do gastrointestinal stromal tumors develop?
Gastrointestinal stromal tumors form when interstitial cells of Cajal grow abnormally and turn into cancer. Interstitial cells of Cajal are special cells in the muscle of the digestive tract.
Most GISTs start in the stomach, but they can be found anywhere in the gastrointestinal tract. In very rare cases, GISTs can appear to start in the peritoneum, the tissue that lines the abdominal wall.
What causes a GIST?
Most GISTs arise because of a random mutation in a cell’s KIT or PDGFR gene that occurs sporadically, meaning there’s no known cause. They often start as one tumor. In rare cases, people can be prone to developing multiple tumors at a younger age, or multiple family members can have a GIST. This usually happens in patients who have certain inherited mutations in the KIT, PDGFRA or SDH genes, or have the inherited disorder neurofibromatosis type 1.
Is a GIST likely to spread?
This depends on several factors, including:
Size of the tumor
This also correlates with how long the tumor has been inside of your body. The longer it’s been in your body, the more likely it is to have spread to the bloodstream.
Growth rate of the tumor
The mitotic count of a tumor refers to how many cells are actively dividing in a defined area of tumor tissue when viewed under a microscope.
Location of the tumor
If the GIST is in a larger organ like the stomach, it can often grow larger without spreading to other organs, especially if the mitotic rate is low. But if the GIST is in the small intestine or rectum, a more vascular area with a lot of nearby structures, it’s more likely to metastasize or spread.
GISTs usually spread to the liver or peritoneal cavity. They mostly spread through the bloodstream.
A GIST can be life-threatening if left untreated. It can metastasize and lead to death.
What are the symptoms of GISTs?
Some GISTs are small and may not cause symptoms. Often, a person doesn’t show symptoms until the cancer is at a late stage.
The top three symptoms of GISTs are:
- Gastrointestinal bleeding or anemia
- Feeling full quickly or after eating only a little bit
- Pain near the tumor site
How are GISTs diagnosed?
Because people with gastrointestinal stromal tumors usually do not have any symptoms during the disease’s earliest stages, GISTs are often found when a doctor is looking for something else.
If your doctor suspects you may have GIST, they may order any of the following tests:
- Imaging tests: A CT scan is used to look for a mass, or an MRI is done on the abdomen and pelvis.
- Upper endoscopy or colonoscopy: These can detect a mass in the esophagus, stomach, parts of the small intestine, colon or rectum.
- Biopsy: This is when tissue is removed and tested for cancer cells.
If the patient has a tumor large enough to where we’re considering systemic treatment, we will run genetic testing on the biopsied tissue. Usually, we look for mutations in the KIT and PDGFRA genes. If those are negative, we’ll do additional testing. If we plan to treat the patient using targeted therapy, it’s important to know the GIST’s mutation type because some rare GISTs don’t respond to certain drugs.
How are GISTs treated?
Treatment for GISTs usually involves surgery and/or targeted therapy.
For GISTs that have not spread to other parts of the body, surgery is used to remove all of the cancer.
Sometimes, targeted therapy is used to shrink the tumor(s) before surgery. Targeted therapy is also used to treat GISTs that are advanced or have spread to other parts of the body. The drugs used are oral tyrosine kinase inhibitors.
Imatinib works well in 60% to 70% of patients, so it is the first-line treatment for most GISTs. The type of mutation and location of the mutation in the KIT or PDGFR gene determines how well the GIST will respond to the drug. About 5% to 8% of GISTs have mutations in the PDGFRA gene in the exon 18 location, which doesn’t respond to imatinib. 10% to 15% of GISTs might have mutations in genes other than KIT or PDGFR that make them less responsive to imatinib. Often, GISTs that respond to imatinib might eventually stop responding. This resistance to imatinib occurs because the GIST can develop secondary mutations. These secondary mutations are important because they can determine a patient’s response to later lines of therapy. We can test for mutations on biopsied tissue or through a liquid biopsy in certain cases.
If initial treatment doesn’t work or stops working, patients may be given sunitinib, a second-line treatment. If those drugs don’t work, regorafenib may be given as a third-line treatment. And if none of those drugs work, ripretinib may be given as a fourth-line treatment. This treatment sequence is evolving as we learn more about the secondary mutations and as newer drugs are being tested. Avapritinib is the only drug approved to treat GIST patients with the PDGFRA exon 18 mutation.
If the cancer doesn’t respond to standard treatments, the patient may need to try other targeted therapy drugs or enroll in a clinical trial.
Before 2001, chemotherapy was used to treat GISTs, but it did not work in shrinking the tumors. The chemotherapy drug temozolamide has shown success in treating a small subset of gastrointestinal stromal tumors called SDH-deficient GIST and is being tested in clinical trials.
Are GISTs curable?
GISTs can be cured if they’re caught early and can be removed by surgery. Often, patients with GISTs will also need to take imatinib if their risk of recurrence is high. The risk is calculated based on the GIST’s:
- size,
- mitotic count and
- location.
Even patients with metastatic disease can be cured if the tumor is not bulky or large. For these patients, it’s important to understand that ‘cured’ means we can get to no evidence of disease (NED), but you need to keep taking the medication. We have patients who remain NED for a long time by continuing to take treatment. GISTs can be managed by treatment, and it lowers the risk of recurrence.
It’s more challenging to treat large, bulky tumors that are getting bigger on imatinib because subsequent therapies may not offer long-lasting benefits. This is often due to the presence of new secondary mutations.
Localized treatments, like embolization, ablation or surgery are used on a case-by-case basis to manage residual cancer cells or a limited area of growth that develops in patients who have metastatic disease and are on oral targeted therapy.
Catching GISTs early and treating them based on the mutation type can improve your chances of survival. It’s important to seek care for these rare types of tumors at a center like MD Anderson that has specialists who focus on treating these tumors. We can personalize your treatment, so you get the best possible results.
What research is being done to advance GIST treatment?
We are testing new treatments for GISTs through clinical trials.
Once imatinib stops working for a patient, we want to determine if we can sequence the next treatment based on the drug that works best for the specific secondary mutations that are causing resistance. This can help ensure the tumor better responds to subsequent treatment.
MD Anderson is participating in a clinical trial looking at combining sunitinib with bezuclastinib to block more mutations in GISTs. I’m also leading a study to see if regorafenib can be used as a second-line treatment in patients with certain genetic mutations. IDRX-42 and NB003 are promising new drugs being tested in clinical trials.
This new research should give hope to patients and caregivers who may soon have more options for GIST treatment.
Request an appointment at MD Anderson online or call 1-877-632-6789.

10 cancer symptoms women shouldn't ignore
If you’re a relatively healthy young woman, cancer may not even be on your radar yet. But it should be, regardless of your age or family history.
Why? Because each year, more than 375,000 women in the United States are diagnosed with breast cancer or ductal carcinoma in situ (DCIS). Another 106,000 are diagnosed with gynecologic cancers, such as endometrial cancer, ovarian cancer or cervical cancer. And while most of these diagnoses occur after menopause, gynecologic cancers can strike women at any age.
“Your risk for all types of cancer rises as you get older,” says Therese Bevers, M.D., medical director of the Lyda Hill Cancer Prevention Center.
Why it’s important to stay alert
The signs of many gynecologic cancers can be vague and very similar to those of other conditions. Only breast cancer and cervical cancer can be detected through screening.
So, it’s important to recognize cancer symptoms and talk about them quickly with your gynecologist or primary care doctor. This can increase your odds of finding cancer early, when it’s most treatable.
“Sometimes, the signs are very subtle,” notes Bevers. “But if you know what to watch for, you can tell your doctor about them right away.”
Here are 10 potential cancer symptoms that every woman should be aware of.
1. Abnormal vaginal bleeding
More than 90% of women diagnosed with post-menopausal endometrial cancer experience irregular vaginal bleeding. It’s also one of the most common symptoms of cervical cancer. So, see a doctor if you experience any of the following:
- Before menopause: bleeding between periods or bleeding during or after sex
- After menopause: any bleeding at all, including spotting
2. Changes in your breasts
Most palpable breast cancers are detected by women themselves during routine daily activities, such as bathing, shaving or even scratching. So, practice breast self-awareness and be alert for any lumps in your breast or armpit. Also, be on the lookout for any unusual discharge, changes in your breasts’ appearance or skin texture, and abnormalities of the nipple, such as retraction or scaling.
3. Unexplained weight loss
Talk to your doctor if you suddenly lose more than 10 pounds without changing your diet or exercise habits.
4. Bloody vaginal discharge
Bloody, dark or smelly vaginal discharge is usually a sign of infection. But sometimes, it’s a warning sign of cervical, vaginal or endometrial cancer.
5. Constant fatigue
A busy week can wear anyone out. But in most cases, a little rest should cure your fatigue. See a doctor if your fatigue is becoming severe or constant, especially if it’s interfering with your work or leisure activities.
6. Loss of appetite or feeling full all the time
Appetite changes can be symptoms of both ovarian cancer and those unrelated to the reproductive system. If you notice you’re eating a lot less than usual but still feeling full quickly, talk to a doctor.
7. Persistent indigestion or nausea
Usually, persistent indigestion and nausea are related to conditions like stomach ulcers or acid reflux. But sometimes, these can signal a gynecologic cancer. Play it safe, and see a doctor if you feel queasy more often than usual.
8. Pain in the pelvis or abdominal area
Ongoing abdominal pain or discomfort — including gas, indigestion, pressure, bloating and cramps — is usually due to gastrointestinal issues. They can be caused by normal hormonal fluctuations during your menstrual cycle, too. But sometimes, they are a sign of ovarian or endometrial cancer. So, see a doctor if yours lasts for more than two weeks.
9. Frequent urination or pelvic pressure
Suddenly need to urinate all the time or feeling constant pressure on your bladder? Odds are, you’ve got a urinary tract infection. But if your doctor has already ruled that out, you’re not pregnant, and you haven’t been drinking more fluids, this could be a sign of a gynecologic cancer.
10. Changes in your bowel habits
If you start noticing changes in the size, shape or frequency of your bowel movements, don’t just dismiss them. These could be a sign of a tumor pressing on the colon and distorting your stool. Talk to your doctor if you start experiencing diarrhea or constipation when you never have before, too.
Having one or more of these symptoms doesn’t necessarily mean you have cancer. But it’s important to get them checked out if you notice them.
“Most cancers are asymptomatic at their earliest stages,” notes Bevers. “So, be sure to get any screenings available at the recommended intervals, and mention any symptoms you might be having to your doctor, especially if they last more than two weeks.”
Request an appointment at MD Anderson online or call 1-877-632-6789.

5 foods and drinks linked to cancer
Learning about cancer risk factors can be scary, especially when these risk factors can be something as common as food.
This knowledge can also raise a lot of questions: Why do certain foods increase cancer risk? Should these foods be avoided completely? What are healthier swaps for these foods?
Clinical dietitian Alyssa Tatum shares five food groups that have been linked to cancer and gives tips on how to approach your relationship with these foods going forward.
Red meats
Red meat such as beef, pork, venison and lamb has been linked to colorectal cancer, Tatum says.
But this doesn’t mean saying a permanent goodbye to favorites like hamburgers. Instead, Tatum encourages diners to eat red meat less frequently and in smaller portions.
“We're not entirely saying ‘Don't eat it,’ but we're saying, ‘Try to reduce the frequency of red meat intake and choose smaller portions,’” Tatum says.
MD Anderson’s dietitians recommend a diet that is largely plant-based. Vegetables, whole grains, beans, fruits, nuts and seeds should make up 2/3 of what you eat, with lean animal protein and dairy products as the remaining third.
Dietitians also recommend eating under 18 ounces of red meat a week. Not sure what that looks like? It can help to visualize 18 ounces of meat as either six decks of cards or two softballs.
Tatum also notes that the temperature at which red meat is cooked can increase cancer risk. For example, chargrilled meats such as burgers and steaks have more potential carcinogens than the same items prepared at a lower temperature using methods such as baking or sous vide.
“When they are being cooked at such a high temperature, they can produce carcinogens that are linked to cancer,” Tatum says.
When opting to eat red meat, she suggests choosing an option with less marbling, trimming the fat or marinating meat before cooking. Other good sources of protein include plant protein, and lean protein options such as poultry and seafood.
Processed meats
Another category of meat that comes with a heightened cancer risk is processed meat.
Processed meat refers to any meat that has been preserved, or undergone changes to its shape and flavor. This includes most of the meat options found behind the deli counter, as well as hotdogs, ham, bacon and sausage.
These options are often preserved using nitrates and nitrites which Tatum says can increase the risk of colorectal and stomach cancers.
Making changes to your diet can feel overwhelming, so Tatum says to start small. When shopping for deli meats, that might look like choosing nitrite and nitrate-free options, or those with lower sodium and fat contents.
“I recommend seeing if there are healthy swaps available for that food and reading labels to compare products,” she says.
Alcohol
There are many stories debating the health risks and benefits of drinking alcohol. But as far as cancer experts are concerned, alcohol has been linked to an increased risk for several diseases including stomach, colorectal, esophageal, liver, pancreatic and breast cancers.
“Alcohol causes damage to the tissues over time which can lead to changes in the cell's DNA and increased risk for cancer,” Tatum says.
While Tatum notes that newer recommendations encourage avoiding alcohol entirely, that may not be desirable for everyone. For those who wish to drink alcohol, do so in moderation with a maximum of one drink a day for women or two drinks a day for men.
Ultra-processed food and drinks
Ultra-processed food and drinks are indirectly linked to cancer risk due to increased levels of sugar and sodium, which can lead to weight gain and obesity.
“Eating these ultra-processed foods that are high in calories and low in nutritional value can increase your cancer risk by causing weight gain and obesity. Obesity can increase your risk for cancer,” Tatum says.
She recommends reducing the amount of ultra-processed food in your diet by focusing on moderation and opting for smaller portion sizes.
“It's hard to say 100% never eat any ultra-processed foods again. That can be challenging or not realistic for some,” she says.
Food and drinks with added sugar
Products with added sugar or artificial sweeteners are indirectly linked to cancer.
Much like ultra-processed options, these sweetened options can lead to weight gain and obesity, which can lead to heightened cancer risk.
While there have been some studies on whether artificial sweeteners pose a direct cancer risk, Tatum says the results are mixed.
She recommends approaching artificial sweeteners the same way she recommends using sugar: in moderation.
How your diet impacts cancer risk
Because these foods are so common, odds are you've probably eaten them before. But before you panic over the glass of wine you enjoyed on date night or the burgers you grilled at a tailgate, Tatum emphasizes the importance of habit in the link between diet and cancer risk.
“It’s not like if you had smoked meats last week at a barbeque that you’re going to have cancer now. It’s not necessarily that one-time exposure. It’s a repeated exposure over time and that’s the concern, so just try to eat those in moderation,” she says.
Request an appointment at MD Anderson online or by calling 1-877-632-6789.

Stomach cancer survivor to complete cross-country bike trip
When Daniel ‘Joe’ Einspahr, M.D., and his son bike into Virginia Beach next summer, they will have more than one reason to celebrate. Not only will the day mark the completion of a father-son cross-country bike trip that has spanned eight summers, 11 states, and over 3,000 miles, but also triumph over one major obstacle: stomach cancer.
Starting a cross-country bike trip
The cross-country journey began in summer 2014 when Joe and his younger son, Chase, biked from Florence, Oregon, to Boise, Idaho. “Every year since then, we've added a segment to our trip,” says Joe. “We go to where we finished and ride another segment."
Over the next three summers, Joe and Chase dedicated one week to completing another part of their journey. Biking between 100 and 200 miles each day, they went from Boise, Idaho, to Salt Lake City, Utah, in 2015; Salt Lake City to Imperial, Nebraska, in 2016; and Imperial to Columbia, Missouri, in 2017.
Aside from allowing Joe to see new parts of the country, these trips have been bonding experiences for the Einspahr family with Joe’s wife, Kim, and older son, Duncan, occasionally joining them along the route in their camper.
Receiving a stomach cancer diagnosis
In the spring of 2018, about three months before Joe and Chase were scheduled to set off on the fifth leg of their trip, Joe started experiencing mild symptoms like feeling hungry after having just eaten. He chalked it up to a stomach ulcer or reflux, but when using an antacid didn’t improve his symptoms, Joe saw a gastroenterologist for an endoscopy. The results showed stomach cancer.
“If I weren’t in the medical field, I probably would’ve just continued to ignore it until something else happened. I just felt like I couldn’t explain it, so I needed to get it checked out and I did,” says Joe.
Instead of heading out on a bike trip, Joe stayed close to home for treatment, which included three rounds of chemotherapy, a partial gastrectomy surgery to remove the majority of his stomach and surrounding lymph nodes, and another three rounds of chemotherapy.
While Joe was able to use his stationary bike during pre-surgery chemotherapy, recovering from surgery kept him off his bike — at least for a time. “Once I got into the recovery from surgery, it was pretty evident that there was not going to be any bike trip that year,” says Joe. “Recovery was a motivator to get back to biking again.”
But by summer 2019, Joe was back in shape and ready for the next leg of the journey. This time, the route from Columbia, Missouri, to Lexington, Kentucky, was made all the more special because it included a stop in Paducah, Kentucky, where Joe had worked earlier in his career.
Treating stomach cancer recurrence at MD Anderson
But Joe’s cancer returned before a 2020 bike trip could take place. The chemotherapy had been so effective that, by the time of surgery, his pathology reports were negative, and it was difficult to tell where the cancer had been. A small amount of cancer was left following surgery, which caused the cancer to grow in what remained of his stomach.
“At this point, all my treatment was in Omaha and they weren't sure what to do with me. They don't see a lot of stomach cancer, and it was an unusual situation to have a local recurrence,” says Joe.
When a friend from medical school suggested MD Anderson, Joe made an appointment. In February 2020, Joe travelled to Houston where he met with surgeon Brian Badgwell, M.D.
Badgwell recommended Joe undergo chemotherapy and radiation before he would perform surgery to remove the rest of Joe’s stomach — connecting his esophagus directly to his small intestine — along with the removal of his spleen and portions of his colon and pancreas. “They knew exactly what needed to be done,” says Joe. “So, my wife and I pulled our camper down to Houston and we lived in an RV park until I had my surgery.”
During this time, Joe underwent genetic testing. The results showed he had a BRAC2 gene mutation, which can be inherited and increase the risk of certain cancers. Joe’s mother, who is adopted, also has a BRAC2 mutation. While he was at MD Anderson, Joe notified his mother’s birth family about the condition. “The family wasn't really aware of the gene; they just saw it as ‘Well, there's a lot of cancer in our family.’ MD Anderson got me some information I could send out to family that I don't necessarily know well,” says Joe.
With surgery scheduled for May, Joe began radiation therapy under the care of Emma Holliday, M.D. It was at this time that COVID-19 started to spread in the United States, leading MD Anderson to limit visitors. “COVID-19 hit very shortly after we got there. MD Anderson became a ghost town,” says Joe.
While his surgery went on as planned, Joe wasn’t allowed visitors during the 10-day hospital stay after his surgery.
Fortunately, surgery went well and, after recovering in Houston, Joe and Kim returned home to Nebraska.
Getting back on the bike following a full gastrectomy
By summer 2021, Joe and Chase were back on their bikes heading from Lexington, Kentucky, to Charlottesville, Virginia, where Joe had completed his medical residency.
Of course, biking long distances after a complete gastrectomy required Joe to make some changes, particularly in regard to how he fueled himself for the journey.
“It's hard to go out and ride your bike 100 miles when you don't have a stomach. You can't get up and eat a big breakfast and hop on the bike and go; it tends to be a little bit more planning, a little more eating on the move. But we've adapted pretty well to it and didn't have any trouble this summer,” says Joe.
Continuing to live after cancer
Today, Joe has returned to working full-time as director of the hospitalist program at a hospital in Hastings, Nebraska.
He meets with his care team — which includes Badgwell, Holliday, and Mariela Blum Murphy, M.D. — at MD Anderson’s Gastrointestinal Cancer Center for follow-up scans every six months. He is also working with his care team to find clinical trials focused on the prevention of and early detection for pancreatic cancer, which he is at a higher risk for because of BRAC2 mutations.
His advice to other patients? “There's a lot of hope even though you get a diagnosis that’s pretty ominous,” Joe says. “People shouldn't lose sight of that.”
Now, with the final leg of his bike journey in sight, Joe and his wife are preparing an extra special 2022 Fourth of July celebration that will involve their entire family. And, like many of the other destinations Joe and Chase have biked through, their final destination is no accident. “When the boys were little, we'd go down to Virginia Beach frequently,” says Joe. “We've had a lot of good family vacations in Virginia Beach.”
While Chase was in high school when the pair began biking together, he is now married with a child of his own. Duncan, too, is married and a father of two. Both families will be in attendance to celebrate Joe and Chase’s accomplishment.
“It's an achievement that I didn't know that I would have an opportunity to do just a few years ago,” says Joe. “It's going to be a sense of accomplishment and completion. At the same time, I'm doing well with my cancer. I'm not looking at this as something I’ve got to get done before I die. It shows that you can continue to live and experience things even when you're dealing with adversity like cancer treatment.”
Request an appointment at MD Anderson online or by calling 1-877-632-6789.
H. pylori and your stomach cancer risk
Most stomach cancers are caused by bacteria called helicobacter pylori or H. pylori. Having H. pylori doesn’t mean you’ll get stomach cancer, but it does increase your risk.
We talked to Patrick Lynch, M.D., a gastroenterologist in Internal Medicine, about H. pylori and other stomach cancer risk factors, how to recognize symptoms and what you can do to reduce your chances of developing this disease.
What’s the link between H. pylori and stomach cancer?
H. pylori is a common bacterium. There are multiple strains, and different strains have different effects on the stomach. Most people never experience side effects or illness.
Most stomach ulcers are caused by H. pylori. Certain strains can also raise your risk for stomach cancer.
“The whole process of stomach cancer risk associated with H. pylori is one of inflammation,” says Lynch. “With H. pylori, you have an infection, which causes inflammation, then healing, then more inflammation. Over time, this cycle of constant cell regeneration can result in mistakes that lead to cancer.”
How do you know if you have H. pylori?
Symptoms of H. pylori infection include chronic dyspepsia – or indigestion – that may be accompanied by abdominal pain, bloating and the urge to burp. Lynch describes it as a “sour stomach.”
Dyspepsia should not be confused with heartburn, which feels like acid and food are coming back up from the stomach into the esophagus. This causes discomfort or pain in the chest.
“Someone with H. pylori is actually less likely to have acid reflux and heartburn, because H. pylori reduces the stomach’s ability to produce acid so it can survive,” says Lynch. “Someone with heartburn likely doesn’t have an H. pylori infection.”
It’s important to pay attention to your symptoms, where they are occurring and what they feel like, so your doctor can make a proper diagnosis. H. pylori infection can be treated with a combination of antibiotics and other drugs.
“Indigestion that is severe enough or has gone on long enough to prompt a doctor’s visit may lead to somebody being evaluated and can sometimes be the means for reducing risk of stomach cancer by identifying and treating H. pylori,” says Lynch.
Know the symptoms of stomach cancer
Stomach cancer is often found in later stages, because symptoms don’t appear until the disease is advanced.
“There are no early signs of stomach cancer,” says Lynch. “If a patient is really paying attention to their body and sees their doctor as soon as symptoms do appear, there is a better chance of successfully treating the disease,” says Lynch.
Symptoms of stomach cancer include:
- Abdominal pain or discomfort
- Loss of appetite
- Heartburn, indigestion or ulcer-type symptoms
- Nausea and vomiting
- Bloating or swelling in the abdomen
- Diarrhea or constipation
- Feeling full after eating small amounts of food
- Bloody or black stools
Having one or more of these symptoms does not mean you have cancer. However, if you notice any of them for more than two weeks, talk to your doctor. The earlier cancer is detected, the easier it is to treat.
Steps to reduce stomach cancer risk
The healthy lifestyle choices that reduce your overall cancer risk will also reduce your risk of stomach cancer and a host of other diseases. These include:
Don't smoke. People who smoke are more likely than nonsmokers to develop stomach cancer. “If you’re talking about a lifestyle intervention that makes a difference, stopping smoking is important,” says Lynch.
Maintain a healthy weight. Being overweight or obese raises the risk of at least 13 cancers, including cancer in the area where the esophagus connects with the stomach. This is likely due to the chronic inflammation caused by excess body fat.
Limit alcohol. Avoid alcohol for cancer prevention. If you choose to drink, limit yourself to no more than one drink per day if you are a woman, and two drinks per day if you are a man. The risk for stomach cancer begins to go up at three or more drinks per day.
Watch your diet. A diet heavy in foods preserved through pickling or salting or that contain nitrates can increase your risk for stomach cancer. Eating foods that have been stored or prepared in unsanitary conditions or have not been properly refrigerated raises the risk of H. pylori infection and stomach cancer.
Talk to your family about their cancer history. Some hereditary cancer syndromes can increase your risk for stomach cancer. If you are concerned, talk to your doctor. “People who have a family history of stomach cancer or the genes associated with them should undergo endoscopy, because they’re at higher risk,” says Lynch. “Even though these conditions are fairly rare, there are situations where you could really pinpoint risk to an individual.”
Request an appointment at MD Anderson online or by calling 1-877-632-6789.
Why choose MD Anderson for stomach cancer care?
When you receive treatment for stomach cancer at MD Anderson's Gastrointestinal Center, you are the focus of some of the world's leading experts. Your personal team of experts may include oncologists, surgeons and radiation oncologists, as well as specially trained nutritionists, nurses and others. Together, they create a care plan using treatments designed to provide optimum results with the least impact on your body.
World-class care
Stomach cancer surgery is often challenging, and your highest chances for a successful outcome are with a surgeon who has a high degree of experience and skill in these highly-specialized procedures. Because MD Anderson is one of the nation's most active cancer centers, our surgeons use the latest techniques to perform a large number of delicate stomach cancer surgeries each year, with outcomes higher than many other cancer centers.
Trailblazing treatment
With groundbreaking research, MD Anderson's physicians have pioneered many improvements in treating stomach cancer. We have led some of the largest international studies on chemotherapy for stomach cancer, and we continue to explore advanced techniques including:
- Robotic surgery
- Intraperitoneal chemotherapy (IP)
- Hyperthermic Intraperitoneal Chemotherapy (HIPEC)
- Intensity-modulated radiation therapy (IMRT)
- Stereotactic body radiation therapy (SBRT)
- Immunotherapy/Targeted therapy
- Genomic/Molecular Profiling
Continual support
At MD Anderson you're surrounded by the strength of one of the nation's largest and most experienced comprehensive cancer centers, which has all the support and wellness services needed to treat the whole person – not just the disease. Stomach cancer can have a marked impact on your life, and our experts guide you every step of the way to help you cope and adjust.
MD Anderson is a big organization, but it’s welcoming and it makes you feel safe. Help was always available.
Sandy Bobet
Caregiver

After my stomach removal, I've never looked back
In 2014, I learned that I carry a genetic mutation called CDH1, which markedly increases my risk of developing breast and stomach cancers. I was only 25 when I found out, so my original plan was to monitor myself carefully. I’d have my stomach examined annually with a scope and get mammograms twice a year.
I knew that a prophylactic total gastrectomy — the complete removal of my stomach as a preventive measure — was the current recommendation for people with this gene. But I was still a newlywed at the time, and my husband and I wanted to wait until after we’d had children to take such a drastic step.
Despite having two endoscopies that showed no evidence of disease, the risk of developing stomach cancer was always in the back of my mind. One day, at age 27, I finally decided I’d worried enough.
Why I chose MD Anderson for my preventive stomach cancer surgery
Anyone who hears they should have their stomach removed because there’s a good chance they’ll develop cancer in it one day is going to be a bit shocked. It definitely makes you want to find the best doctor to do it!
The first genetic counselor we met with recommended we choose a surgeon who treats lots of families with CDH1. She gave us a list of physicians and hospitals to consider, so we did some research and made some phone calls.
MD Anderson surgeon Dr. Paul Mansfield was one of the surgeons on that list. MD Anderson is the No. 1 hospital for cancer care. And because Dr. Mansfield had performed the same procedure on my mother, having him perform my surgery just made sense. My mom received such amazing care from him that I knew MD Anderson was where I wanted to go, too.
Dr. Mansfield removed my stomach on May 16, 2017.
Life after my total gastrectomy
During a total gastrectomy, the stomach is completely removed from the body and the esophagus is reattached directly to the small intestine. So, there was a lot of trial and error in figuring out which foods I could eat comfortably in the first few months after surgery.
Eating too much or too quickly now makes me feel really sick. I also have to avoid sugary and fried foods. Mostly, I just eat a high-protein diet, but with much smaller portions. I also eat frequently throughout the day.
The hardest and most surprising parts of not having a stomach
The hardest part of not having a stomach is probably that I rarely feel thirsty. So, I don't have that visceral cue anymore to prompt me to drink. I have to make a conscious effort to hydrate myself now. In the first few months after my surgery, I had a water bottle marked by the hour, just for the visual reminder.
The most surprising aspect of not having a stomach was discovering how hard it is to drink plain water. It literally feels like it’s stuck in my esophagus — and a lot of the other gastrectomy survivors I’ve talked to say the same.
Apparently, it has something to do with high surface tension, so drinking fluids with lower surface tension — like watered-down juices or sugar-free sports drinks — makes it easier. Finding the right cup, bottle and straw also helps.
Why I’ve never looked back after my gastrectomy
In the years since my surgery, the biggest lesson I’ve learned is that you don’t need a stomach to live a healthy life.
I’ve developed and maintained a new normal since 2017, even without a stomach. I do still feel “hungry” sometimes, but it’s more of a sense of emptiness (and a sign that my blood sugar is low) than anything else. I’ve regained all eight pounds I lost after surgery and have been working out and running again, which is great.
Today, I’m pregnant with my first child. And, other than a few modifications to my vitamin regimen and glucose monitoring methods, my pregnancy has been pretty normal. I even dodged the morning sickness bullet — so that was an unexpected benefit of not having a stomach!
At first, I wondered if I might’ve jumped the gun in having my stomach removed. But a few weeks after my surgery, the pathology report came back. It showed that there was already signet ring cell carcinoma in the lining of my stomach, which is consistent with the CDH1 gene mutation.
So, technically, I already had stomach cancer; I just didn’t know it yet. When I got that news, I knew I’d made the right decision. And I have never looked back.
Request an appointment at MD Anderson online or by calling 1-877-632-6789.
Treatment at MD Anderson
Stomach cancer is treated in our Gastrointestinal Center.
Clinical Trials
Becoming Our Patient
Get information on patient appointments, insurance and billing, and directions to and around UT MD Anderson.
myCancerConnection
Talk to someone who shares your cancer diagnosis and be matched with a survivor.
Prevention & Screening
Many cancers can be prevented with lifestyle changes and regular screening.
Counseling
UT MD Anderson has licensed social workers to help patients and their loved ones cope with cancer.
Help #EndCancer
Give Now
Donate Blood
Our patients depend on blood and platelet donations.
Shop UT MD Anderson
Show your support for our mission through branded merchandise.