request an appointment online.
- Diagnosis & Treatment
- Cancer Types
- Lung Cancer
Get details about our clinical trials that are currently enrolling patients.
View Clinical TrialsLung cancer is a disease in which cells in the lungs grow and multiply out of control. It most often starts in the cells that line the air passages, usually as a result of exposure to toxins like tobacco smoke.
Lung cancer is a disease in which cells in the lungs grow and multiply out of control. It most often starts in the cells that line the air passages, usually as a result of exposure to toxins like tobacco smoke.
Lung anatomy
When you breathe in, oxygen comes through your mouth and nose and then travels through the trachea, or windpipe. The trachea divides into two tubes called bronchi, which take oxygen to the left and right lungs. Inside the lungs are smaller branches, called bronchioles, and alveoli, tiny air sacks where oxygen is transferred to the blood stream.
Each lung is divided into sections called lobes. The right lung has three lobes and the left lung has two lobes. The left lung is smaller than the right lung because the heart is also located on the left side.
The pleura is a thin membrane that covers the outside of each lung and lines the inside wall of the chest. The space between the lungs and the chest wall usually contains a very small amount of fluid that allows the lungs to move smoothly during breathing.
Cellular diagnosis
Lung cancer is typically diagnosed based on the type of cell where the cancer started. This information helps doctors understand the patient’s condition and make a treatment plan. The two main categories are:
Non-small cell lung cancer (NSCLC). NSCLC makes up about 85% of all lung cancer cases. It starts in the lungs’ epithelial cells, a type of cell that lines the surface of organs. There are several sub-types of non-small cell lung cancer based on the type of epithelial cell where the disease begins. These include adenocarcinoma (the most common type of lung cancer), squamous cell carcinoma and large cell carcinoma.
Small cell lung cancer (SCLC). About 15% of lung cancers are SCLC. Most are caused by tobacco use, but a growing number of cases are diagnosed in people with no smoking history. It often starts in the more central portions of the chest. SCLC usually grows and spreads quickly to other parts of the body, including the lymph nodes, brain and bones. Because it is so aggressive, surgery is used less often for small cell lung cancer than non-small cell lung cancer.
Molecular diagnosis
Today, doctors can also diagnose the disease on a molecular level.
This approach usually looks for mutations in the DNA and RNA of cancer cells and/or proteins produced by the cancer cells. There are hundreds of different molecular diagnoses. Some important mutations for lung cancer include changes to the EGFR gene, ALK gene, KRAS gene and ROS1 gene.
These molecular subtypes can impact how quickly the disease grows and spreads. They also can predict how the disease will respond to specific treatments, including different types of chemotherapy, targeted therapy and immunotherapy.
By diagnosing a patient’s disease on a molecular level, doctors can design treatment plans with the best chance of fighting each patient’s specific cancer.
Seeking a second opinion on a lung cancer diagnosis
There are many different lung cancer subtypes. Treatment plans are often based on the patient’s exact diagnosis. A second opinion can help ensure patients are getting the best possible care. Learn more about second opinions at UT MD Anderson.
Lung metastases
Cancer that starts in another part of the body, like the breast or colon, can spread, or metastasize, to the lungs. These tumors are called lung metastases, and they are not the same as lung cancer. In these cases, they are still classified as the original type of cancer. For example, a colon cancer with lung metastases is called metastatic colon cancer.
How is lung cancer diagnosed?
Lung cancer is diagnosed by removing suspected cancer tissue and studying the cells under a microscope. Imaging exams and molecular testing also help doctors understand the patient’s condition. Read more about lung cancer diagnosis.
Young-onset Lung Cancer
The average age of a person diagnosed with lung cancer is around 70 years old. In recent years, there has been an increase in diagnoses among people under age 50. UT MD Anderson’s Young-onset Lung Cancer Program offers specialized services for these patients. Services include fertility care, genetic testing and counseling, as well as support groups for young adults.
Common symptoms
Lung cancer often has no symptoms in its early stages. When it does cause symptoms, they may include a persistent cough that gets worse over time, constant chest pain, and coughing up blood or rust-colored phlegm. Learn more symptoms, other possible diagnoses, and screening guidelines on the lung cancer symptoms page.
Typical treatment options
Surgery, radiation therapy and cancer drugs like chemotherapy and targeted therapy, immunotherapy are key treatments for lung cancer. These treatments are often given in combination. Learn more on our lung cancer treatment page.
Survival rate & prognosis for lung cancer
Lung cancer is the most common cause of cancer-related deaths and second most common cancer in both men and women in the United States. According to the National Cancer Institute, more than 225,000 people in the U.S. are diagnosed with lung and bronchus cancer each year.
While most cases are linked to tobacco smoking, a growing number of diagnoses are among people with no smoking history, especially among women. Most lung cancers are diagnosed after the disease has spread. As a result, the five-year survival rate for lung cancers is about 28%, though that number changes based on how advanced the disease is at the time it is diagnosed.
Cases caught before the disease spreads have a survival rate of around 65%.
If the cancer has spread to nearby lymph nodes, the survival rate is 37%.
If the cancer has spread to distant parts of the body, the survival rate is around 10%.
These figures do not include people diagnosed in the past few years, who may benefit from newer treatments.
Risk factors
A risk factor is anything that increases the chance that a person will develop a particular disease. The main risk factors for lung cancer are:
- A history of or current tobacco use
- Exposure to radon gas
- Exposure to secondhand smoke
- Exposure to asbestos, arsenic, chromium or other chemicals
- Living in an area with significant air pollution
- A family history of lung cancer
- Radiation exposure, including radiation therapy to the breast or chest, and radon exposure. This is a minor risk factor and the benefits of radiation therapy far outweigh the risks.
Is lung cancer hereditary?
A small number of lung cancer cases can be caused by gene changes passed down from parent to child. Visit the family history section to learn about hereditary cancer syndromes and genetic counseling.
UT MD Anderson is #1 in Cancer Care

What's the best way to quit smoking?
Smoking is on the decline. But if you are one of the 28 million Americans still smoking, you probably know how hard it is to quit.
Close to 70% of smokers report that they want to stop smoking. Of those, 53% said they tried to quit in the previous year. Only around 9% succeeded.
There are plenty of reasons to try to reduce your nicotine addiction: Tobacco use – and smoking, in particular – accounts for about one-third of all cancers, and up to 90% of lung cancer cases. It also contributes to heart disease, stroke and lung disease.
So, what's the best way to quit smoking?
“The best way to quit smoking is with a combination of medication and counseling,” says Maher Karam-Hage, M.D., medical director of the Tobacco Research and Treatment Program at MD Anderson. “They both help. But you double your chances by using both compared with one of them.”
What products can help you quit smoking?
There are several products that can help reduce your nicotine cravings.
Prescription medication
Smoking cessation options that require a doctor’s prescription include:
Varenicline (formerly sold as Chantix) works in two ways. First, it provides a mild version of nicotine’s effects. This helps reduce withdrawal symptoms and cravings. Second, it stops your brain from feeling the pleasurable effects of nicotine when you smoke. This makes smoking less appealing. Varenicline is the most effective single medication, Karam-Hage says. But it's also the most expensive.
Bupropion (also sold as Zyban or Wellbutrin) blocks the effects of nicotine in your brain. This makes smoking feel less pleasurable, but it does not replace the effect of nicotine.
Nicotine nasal spray is a nicotine replacement therapy that is sprayed into the nostril and absorbed into the nasal lining and bloodstream. This product provides nicotine without the other harmful effects of cigarettes.
Over-the-counter options
Over-the-counter nicotine replacement therapies partially satisfy nicotine cravings by giving the body small amounts of nicotine. This can help with cravings and make it easier to stop smoking.
The over-the-counter nicotine replacement therapies available in the United States are:
Nicotine patches are 3- or 4-inch-wide patches that release a steady dose of nicotine. They are applied to the upper body and changed daily. They come in 7 mg, 14 mg and 21 mg doses.
Lozenges release nicotine as they dissolve in the mouth. They are available in mini and regular sizes and 2 mg and 4 mg doses.
Nicotine gum users follow the ‘chew and park’ method. The gum is chewed for 5 to 10 seconds then parked between the teeth and cheek for another 5 to 10 seconds. This process is then repeated in different parts of the mouth. It comes in 2mg and 4 mg doses.
Why is counseling important?
Working with a counselor can help you better understand your medication. A counselor can also give you the tools to cope with setbacks, stress and cravings by building skills in several areas. These include:
Problem solving
We all run into problems in life, like personal conflicts, that can make us feel helpless. Working with a counselor to tackle them one at a time can help you build knowledge and skills that can be used in other areas.
Coping strategies
Anything from a traffic jam to a death in the family can set off a strong urge to smoke. Learning strategies like deep breathing exercises, meditation and mindfulness can help a smoker get to the other side of a crisis without smoking.
Behavior change
Smokers who quit may miss the “hand-to-mouth” act of smoking. Counseling can help them find substitutions like using a straw, cinnamon stick or gum.
Identifying triggers
Counseling can help you identify what triggers you to smoke, like that morning cup of coffee or spending time with friends who smoke. Once you identify your triggers, you can learn to deal with them or avoid them.
Once smokers start counseling, they appreciate the tools and support it provides in their effort to quit smoking, Karam-Hage says.
“Finally, somebody understands the struggle they're going through,” he says. “Someone is acknowledging that it's not a simple thing to quit. That is very helpful.”
What option should you try first?
Not sure where to start? For many, over-the-counter nicotine replacement therapies are quicker and easier to get than medication because they don’t require prescriptions and can be purchased at most pharmacies.
However, remember that nicotine replacement therapies must be used consistently to be effective. If you find it hard to regularly use options like the patch, lozenges or gum, or if they don’t help you quit, Karam-Hage says you might consider medication.
Your doctor can prescribe medication to help you quit. They can also advise you on how to combine nicotine replacement therapies. This might look like using the patch along with either nicotine gum, lozenges or nicotine nasal spray.
Additionally, a professional counselor can help you monitor what is and isn’t working and work with a prescriber on your care team to adjust the medication you take to set you up for success.
Want to quit but don't have access to a comprehensive program that includes both counseling and medication? You have options.
You can get phone and text support through the National Institutes of Health Quitline by calling 1-800-784-8669, texting QUIT to 47848, or visiting SmokeFree.gov. If you live in Texas, you can use the Texas Tobacco Quitline by calling 1-877-YES-QUIT or visiting YESQUIT.org.
Should you quit smoking cold turkey?
Knowing the health risks and addictive properties of nicotine, you might be wondering whether you should simply quit smoking cold turkey.
Karam-Hage says it’s wonderful if a smoker can quit cold turkey, but notes it is not necessarily better than using medication and counseling. This is because while it works for some, it does not work for everyone.
Most people who attempt to quit smoking on their own fail to do so, he says. Because of this, he notes people may benefit from using both medication and counseling in future attempts to quit smoking. He says the unfortunate reality is that only about 30% of people attempting to quit get either medication or counseling, and only 5% of people get both medication and counseling.
If you’ve tried and failed to quit smoking long-term, Karam-Hage recommends a combination of counseling and medication. Enrolling in a comprehensive tobacco treatment program like MD Anderson’s Tobacco Research and Treatment Program, which is open to MD Anderson patients and caregivers, can be helpful for those seeking additional support. A 2019 study showed that 45% of people enrolled in MD Anderson’s program managed to quit smoking.
What happens to your body when you quit smoking?
Let’s start with the organ that is perhaps most associated with smoking: the lungs.
Those who quit smoking might note that they can breathe a little easier – and not just metaphorically! Karam-Hage says this is because the toxins from cigarette smoke are gone.
As for whether the lungs can regenerate after you quit smoking, the answer depends on just how damaged the lung tissue is. For lung tissue that is damaged but still alive, Karam-Hage says it is possible for it to recover. However, totally damaged cells can’t be reversed.
“Whatever cells have died are gone and no regeneration is possible,” he says, noting this is why conditions like chronic obstructive pulmonary disease (COPD) are permanent.
While smoking’s effects don’t entirely go away when you quit, Karam-Hage says there are many positive health impacts that happen when you quit smoking.
These benefits include:
- Reduced heart rate and blood pressure
- Reduced level of carbon monoxide in blood
- Improved circulation and lung function
- Improved sense of taste and smell
- Reduced risk of heart disease
- Reduced risk of stroke
- Reduced risk of mouth, throat, larynx, esophageal, bladder, cervical, lung, kidney, liver, colorectal, leukemia and pancreatic cancer
“There are many benefits, and they continue to get better as time passes,” he says.
Request an appointment at MD Anderson online or call 1-877-632-6789.
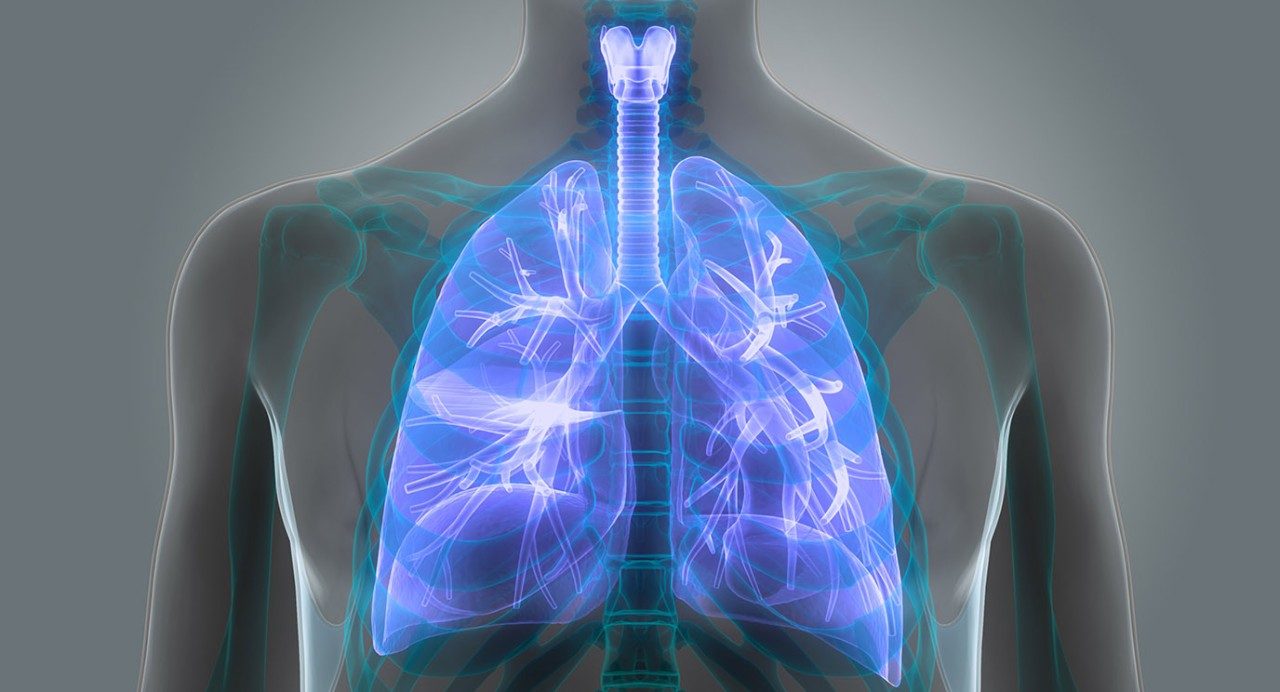
Lung nodules (pulmonary nodules): What you need to know
Lung nodules — or pulmonary nodules — are small growths that can develop in the lungs. By definition, they are no larger than 3 cm, or about 1.25” across. Anything bigger than that is considered a mass.
Lung nodules are very common. But most lung nodules are not due to cancer.
So, why do lung nodules even form? Do they ever cause any symptoms? And, what should you do if you find out you have one?
Read on to learn the answers to these and other questions about lung nodules.
How serious is a lung nodule?
The answer to that question depends on the answer to several others.
- Number: Is there only one, or are there many lung nodules?
- Size: How big is it/are they?
- Age: How old are you?
- Family history: Does any type of cancer run in your family?
- Medical history: Have you ever had a lung infection?
- Work history: Have you ever been exposed to asbestos or radon?
- Social history: Have you ever smoked, vaped or used other tobacco products?
The older you get, the more common benign — on non-cancerous — lung nodules become, particularly if you live in certain parts of North America. But it’s more concerning if you have many nodules and have had cancer before than if you only have one and have never had cancer.
Anything larger than a green pea (about 5 mm) is worth investigating, but even smaller nodules might call for monitoring. And, answering “yes” to any of the history-related questions above significantly raises the risk that a nodule might be cancerous.
Why do lung nodules even occur?
People may develop lung nodules for many reasons. These include:
- Old infections, which can cause scarring
- Chronic infections, such as tuberculosis
- Sarcoidosis and rheumatoid arthritis, both autoimmune disorders
- Prior trauma, such as a gunshot wound or auto accident
- Cysts, or hollow sacs filled with fluid
Congenital conditions
- Arterial venous malformation, which shows up as dark spots in the middle of lung
- Pulmonary sequestration, when a segment of lung has its own blood supply
- Congenital emphysema, which some babies are born with
Certain fungal infections
- Blastomycosis (Great Lakes area)
- Coccidiodomycosis or Valley Fever (San Joaquin Valley)
- Histoplasmosis (Mississippi Valley)
Lung nodules may also be cancerous. When that happens, they could either be caused by lung cancer or a different type of cancer that has spread to the lung from another place.
Unfortunately, the lung is a very common location for metastatic disease. That means many other cancers tend to spread there. Sarcomas, for instance, often spread to the lungs. So does colorectal cancer. But technically, any type of cancer can spread to the lungs.
How are lung nodules usually found?
There are four main ways:
- An X-ray taken for an unrelated reason, such as an auto accident
- Imaging related to a lung problem, such as a cough that won’t go away or pneumonia symptoms
- A lung cancer screening
- A health screening performed before an operation
A rapid CT scan of the heart called a calcium score test is done to assess coronary artery disease. Sometimes, it catches the edges of the lungs in its field of vision, revealing nodules. Abdominal CT scans can also sometimes catch nodules in the lower third of the lungs.
Do lung nodules ever go away on their own?
Yes, especially if they’re related to an infection. Not so with any of the other possible causes, though. Cancer, in particular, will not go away on its own.
Do lung nodules ever cause any symptoms?
Yes. Even if they’re benign, the nodules themselves or their underlying causes can cause some of the same symptoms as lung cancer, including:
- A nagging cough
- Shortness of breath
- Chest pain or pressure
- Persistent or recurrent upper respiratory infections
How can you tell if a lung nodule is cancerous?
If a nodule appears completely calcified on imaging, as if the whole thing has turned to stone, it is not cancer. If it has some flecks of calcium in it, it might be cancerous. But if there’s no calcium in a nodule at all, we’re always going to find that suspicious. Still, there are three approaches to learning more.
- Watch it: Also known as surveillance, this means we monitor a nodule over time to see if it grows bigger, gets smaller or just stays the same.
- Re-image it: We use advanced imaging techniques — such as PET scans and high-resolution CT scans — to take a closer look.
- Sample it: We can either stick a needle in the nodule or remove the whole thing surgically. Either way, we’ll get a piece of it so we can biopsy the tissue.
The only way to know for sure if something is cancer is to look at its cells under a microscope. But we have to balance the risk of a biopsy with the risk of it being cancer. That’s why we usually take a wait-and-see approach if your risk is very low or if there’s a clear reason for a nodule, such as a recent case of the flu.
On the other hand, if you have multiple nodules, smoke a pack a day and have a family history of lung cancer, we might go straight to biopsy, because all of those factors put you at higher risk of lung cancer.
The longer a nodule remains unchanged, the lower your risk of cancer is and the more justified continued observation is, rather than exposing you to the risk of a biopsy. If a nodule remains stable and doesn’t grow over two years or more, it is not a cancer.
How are lung nodules usually treated?
That depends on how many there are, what kind they are, and whether they are causing any problems. Even if a lung nodule is not cancerous, if it’s causing repeated infections or making breathing difficult, we’ll often remove it.
But lung cancers and those that originate in other locations are treated very differently. So, there’s no one-size-fits-all answer.
What is a lobectomy?
A lobectomy is the surgical removal of one of the five lobes — or main sections — of the lungs. It is the most common type of operation used to treat lung cancer, and it may be performed on patients with various stages of the disease.
But is a lobectomy considered major surgery? How long does it take to fully recover? And will you feel short of breath after having one?
Read on for the answers to these questions and more.
What is a lung lobe?
Think of your airway as an upside-down tree. The trachea, or windpipe, is the trunk. The first two branches leading off of it go to the left and right lungs. Branches further down lead to the upper, middle, and lower lobes on the right, and the upper and lower lobes on the left.
We have five lung lobes in all: two on the left side and three on the right. These lobes can be further subdivided into 19 smaller units called “segments.” A segmentectomy is the surgical removal of a segment rather than an entire lobe.
How long does it take to fully recover from a lobectomy?
That varies widely. It depends on many factors, including:
- Which surgical approach is being used
- Your overall health status
- How well the rest of your lung lobes are functioning
On average, you can expect to spend two to three nights in the hospital afterward and have several chest X-rays taken to monitor your progress.
A chest tube will be inserted at the time of the operation. It will be left in place to allow the lung to re-expand and drain any air or fluid that accumulates. The tube is usually removed within a day or two of surgery when the volume of fluid draining is minimal and there is no longer any air bubbling from it.
In some circumstances, you may be ready to leave the hospital before that happens. In those situations, you’d likely return to the clinic within a few days to have the tube taken out.
What will my life be like after a lobectomy? Will I always feel short of breath?
No. A lobectomy would not be performed if it would leave you unable to breathe adequately or feeling permanently short of breath.
That being said, you might feel slightly short of breath for the first few weeks after a lobectomy while your body adjusts to its new anatomy. You may also experience some discomfort when taking deep breaths, but that should improve over time.
You will be assessed for your lung function before a decision is made to perform lung surgery. We calculate your eligibility based on pre-operative lung function and what percentage of lung tissue would be removed.
Is a lobectomy considered major surgery?
Yes. Any lung surgery is considered major surgery.
Is a lobectomy considered a high-risk procedure?
No. We might describe certain tumors or patients as high-risk based on their anatomy or overall health status. But it’s a very common operation. Even in complex situations, risks can be reduced by going to an experienced center of excellence like MD Anderson, where thoracic surgeons do it every day.
What are the risks of a lobectomy?
The greatest risks associated with lung surgery are:
- Prolonged air leaks: when the lung continues to leak air for more than a few days after surgery, requiring ongoing management with a chest tube
- Pneumonia: an infection of the lungs, which can be treated with antibiotics
- Atrial fibrillation (A-fib): an abnormal heart rhythm seen in roughly 8-10% of lobectomy patients, which is treated with medications
Fortunately, most of these conditions are temporary. Air leaks, in particular, are usually self-limiting. Pneumonia can often be prevented, too, with deliberate coughing, deep breathing, and a lot of walking after surgery.
What’s the difference between a pneumonectomy and a lobectomy?
A pneumonectomy is the removal of an entire lung. A lobectomy is the removal of just part of it (a single lobe).
What’s the most important thing to know about lobectomies?
Lobectomies are the most commonly performed operation on the chest. So, it’s important to have yours done well. That’s why you should go to a place like MD Anderson, where surgeons perform these procedures all the time.
Mara Antonoff, M.D., is a thoracic surgeon who specializes in the treatment of lung cancer.
Request an appointment at MD Anderson online or call 1-877-632-6789.
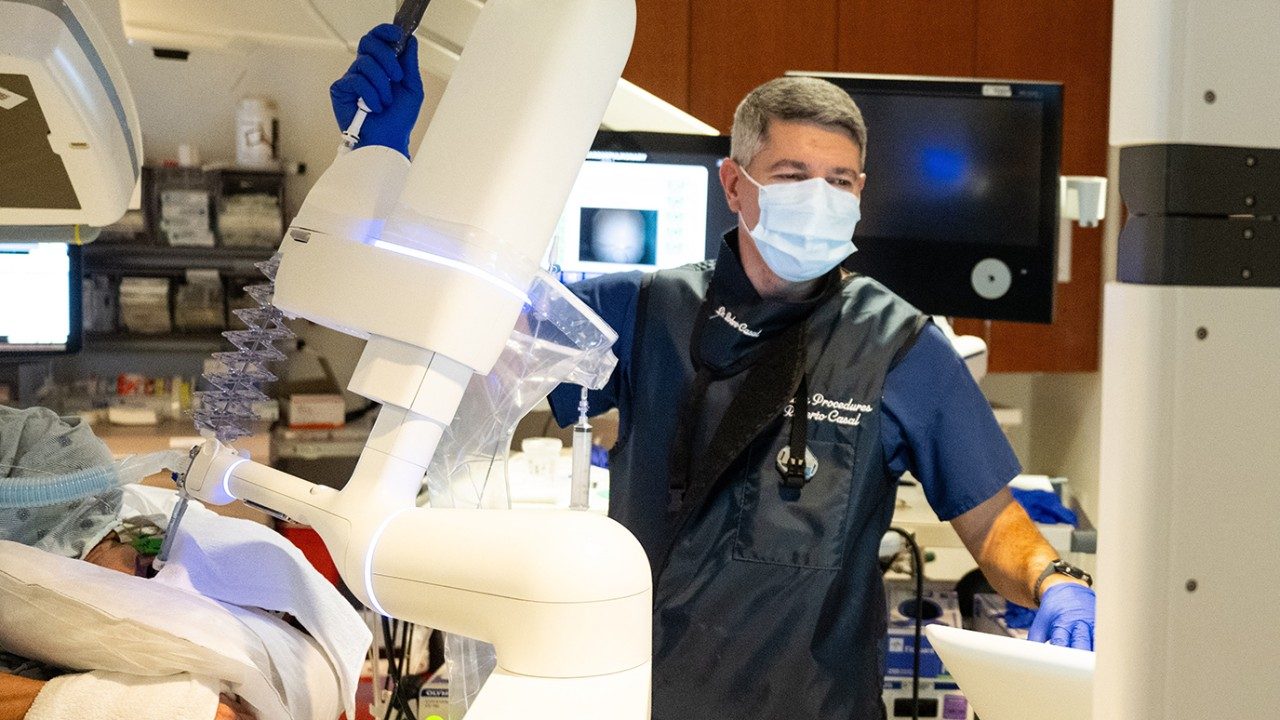
Bronchoscopy 101: How it helps diagnose and treat lung conditions
A bronchoscopy is a minimally invasive medical procedure in which doctors use a special scope to examine the inside of your lungs and airways. It is used frequently to diagnose and stage lung cancer.
But can a bronchoscopy tell us anything else? Do you have to be put to sleep to have one? And how long does it take to recover?
Read on, for answers to these questions and more.
What are the different types of bronchoscopy?
Diagnostic bronchoscopy
We use robotic bronchoscopy to biopsy lung nodules and a technique called endobronchial ultrasound (EBUS) to sample lymph nodes for cancer staging.
We also use a technique called bronchoalveolar lavage (BAL), typically in immunocompromised patients, to diagnose opportunistic infections of the lungs. To do a bronchoalveolar lavage, we wedge the bronchoscope in the section of the lung we’re interested in, flush it with a saline solution, extract the fluid, and culture it in a lab to see what grows.
Therapeutic bronchoscopy
Mostly performed via rigid bronchoscopy, this procedure is used to remove tumors that are blocking the windpipe, to cauterize bleeding tumors, or to place stents that keep the windpipe open. It won’t cure cancer, but it should make breathing easier.
How long does a bronchoscopy take?
That depends. The shortest procedure is the bronchoalveolar lavage, which can take just 10 to 20 minutes. The diagnostic bronchoscopy of a lung nodule can take 45 minutes to an hour, and the sampling of lymph nodes for staging can add another 45 minutes.
But if we’re doing it strictly for therapeutic purposes, it can take from one to two hours, depending on the complexity of the case.
Keep in mind, though, that these are all estimates. The length of each procedure is determined by the number of lung nodules or lymph nodes being biopsied, and doctors don’t know this until they are looking inside your lungs.
Are you awake during a bronchoscopy?
Not necessarily. You’ll be given general anesthesia in most cases, but moderate sedation if you only need bronchoalveolar lavage.
Is a bronchoscopy considered a serious procedure?
That depends on how you define it. I consider anything requiring general anesthesia to be a serious procedure.
But doctors will be working inside your lungs, which are the most vital organs aside from the heart. So, it is more serious than a colonoscopy, for example, but less serious than most surgeries.
Is a bronchoscopy considered a high-risk procedure?
Bronchoscopy for the diagnosis of lung nodules, sampling of lymph nodes, or bronchoalveolar lavage is commonly considered a moderate-risk procedure. On the other hand, therapeutic bronchoscopy is always considered high-risk because patients are sicker to begin with. They often have collapsed or obstructed airways, low oxygen levels, or they are actively bleeding.
What are the risks of a bronchoscopy?
With diagnostic and staging bronchoscopies, the risks are mainly from the anesthesia, rather than the procedure itself. General anesthesia can lower your blood pressure, which can be risky if you have underlying cardiovascular disease. It can also weaken the breathing muscles, so you tend to take shallower breaths when you wake up from anesthesia, and that can make your blood oxygen levels drop.
Biopsies of the lung nodules or lymph nodes have minimal risk of bleeding and infection, but biopsy of lung nodules can sometimes lead to lung collapse (pneumothorax). That’s why even if everything goes well, we prefer our patients to avoid long-distance traveling or air travel until the next day.
With therapeutic bronchoscopies, the risks are higher, and they generally involve bleeding, having low oxygen levels, and difficulty breathing. But all of these are dependent on each patient’s particular situation, and your doctor will go over which ones apply to you in detail.
How long does it take to recover from a bronchoscopy?
Most diagnostic and staging bronchoscopies are outpatient procedures. Patients remain in the recovery area for 45 minutes to an hour afterward, and then they go home. They generally feel tired on the day of their bronchoscopy, but they are back to their baseline the following day.
The recovery time is similar for therapeutic bronchoscopy patients, even if they are already admitted to the hospital.
Is a bronchoscopy painful?
No. The lungs have no pain receptors, so they do not hurt, and you are also sedated. You should not experience chest pain after bronchoscopy, either, unless you are coughing really hard.
Does a bronchoscopy have any side effects?
Some patients report having a sore throat due to the breathing tube. And patients can expect to cough up mucus tinged with blood for the next 2 or 3 days. But those are both normal and will resolve on their own.
Is a bronchoscopy better than a CT scan?
These two tests play very different roles. A CT scan is the test that generally finds out there is something wrong in your lungs. But it can only tell you that there’s an abnormality present. It cannot tell you exactly what it is. A CT scan is just the beginning.
For an accurate diagnosis, we have to examine tissue under a microscope. A bronchoscopy allows us to obtain that sample and make a diagnosis. If it turns out to be lung cancer, the tissue we obtain through a bronchoscopy can also be used for molecular profiling, so we can tailor your treatment to any specific genetic mutations. And bronchoscopy can, in addition, sample the lymph nodes to determine the stage of lung cancer.
Can a bronchoscopy detect tuberculosis?
Yes. Bronchoalveolar lavage is considered the gold standard for detecting any type of lung infection. For patients with pneumonia, we can determine exactly which pathogen is causing it.
What’s the one thing people should know about bronchoscopies?
Go to a place like MD Anderson which does a large number of complex bronchoscopies each year and has a lot of expertise in them. That level of experience will give you a better outcome.
MD Anderson is also at the forefront of using ablation therapy during bronchoscopy to treat small, peripheral lung cancers through clinical trials. We are the pioneers in this field, and only a handful of cancer centers offer it right now.
Roberto Casal, M.D., is an interventional pulmonologist specializing in bronchoscopies.
Request an appointment at MD Anderson online or call 1-877-632-6789.
Lung anatomy & lung cancer spread
Diagnosis & Treatment
Diagnosis
Early-stage lung cancer often does not have symptoms. In addition, when symptoms appear they can easily be mistaken for common respiratory illnesses like bronchitis or pneumonia. Because of this, many cases are diagnosed at an advanced stage.
Patients at high risk for lung cancer, especially those with a history of smoking, should undergo regular screenings in order to catch the disease at its early stages, when there is a better chance of cure.
If you have symptoms that signal lung cancer, your doctor will ask you questions about your medical, smoking and family history and whether you have been around certain chemicals or substances.
The following tests may be used to diagnose lung cancer or monitor how the patient responds to treatment.
Lung cancer imaging exams
Imaging exams look for cancer inside the body. They can help locate tumors and track how the body is responding to treatment. There are many types of imaging exams. The ones used for lung cancer include:
- Chest X-ray: X-rays use low doses of high-energy radiation that travel through the body to create an image. X-rays are used to image bone and can also help spot possible tumors. Chest X-rays are typically the first imaging exam used to help diagnose lung cancer.
- CT scan: A CT scan uses an X-ray machine to take several pictures from different angles. These are combined to create a highly detailed image that can confirm the presence of a tumor.
- PET scan: During a positron emission tomography scan, or PET scan, a small dose of radiolabeled sugar is injected into a patient. A scanner shows where the body distributes the sugar, allowing for the creation of an image. Cancer cells consume more of this sugar than healthy cells, so this image can help doctors find cancer throughout the body. This is a routine test for determining the cancer’s stage.
- MRI scan: Magnetic Resonance Imaging, or MRI, uses magnetic fields and radio waves to generate pictures of the body’s soft tissue and organs. Doctors use MRIs to look for the spread of lung cancer to the brain.
Learn more about imaging exams.
Lung cancer biopsy
If the findings on the imaging exams indicate cancer, the doctor will request a biopsy.
A biopsy is the only way to definitively diagnose lung cancer. During a biopsy, a small tissue or fluid sample is removed and examined under a microscope for the presence of cancer cells. Depending on tumor location, some biopsies can be done on an outpatient basis with only local anesthesia. Other times, patients must undergo a surgical biopsy under general anesthesia.
There are several ways doctors can perform biopsies of lung tumors:
- Needle biopsy: A CT-guided biopsy where a needle is inserted through the skin under local anesthesia to acquire a tumor sample. This is one of the most common biopsy procedures for lung cancer.
- Bronchoscopy: This is the standard biopsy procedure for lung cancer. A thin, flexible tube with a tiny camera is inserted through the nose or mouth and down into the lungs to obtain a small tissue sample (biopsy). This is usually performed under mild sedation. Bronchoscopies are usually performed with an endobronchial ultrasound.
- Thoracentesis: Fluid from around the lungs is drawn out with a needle and tested for cancer cells. Thoracentesis is used when imaging exams indicate the cancer may have spread to the pleura, the membrane that surrounds the lungs and chest wall. Thoracentesis is usually performed in combination with other biopsy methods.
- Endobronchial ultrasound (EBUS): A bronchoscope with an attached ultrasound device is used to check for lung cancer inside nearby chest lymph nodes. EBUS is often performed at the same time as a bronchoscopy and requires general anesthesia.
- Video-assisted thoracoscopic surgery (VATS): This minimally invasive surgical procedure uses a small camera to help retrieve tumor samples that are otherwise difficult to access. VATS requires a general anesthetic and is performed in the operating room by a thoracic surgeon. VATS is used only in limited situations.
- Thorascopy/pleuroscopy: A tiny camera is inserted through a small incision in the back (for a thorascopy) or between the ribs (for a pleuroscopy). Doctors use this device to look for and retrieve suspected cancer tissue. This procedure is used only in limited situations.
Molecular diagnosis
Different cancers have different features on the molecular level. A molecular diagnosis identifies the features that impact how the cancer responds to specific therapies. Doctors use this information to develop the most effective treatment plan for each patient.
Blood tests
Advanced blood tests, known as circulating tumor DNA (ctDNA) tests, can look for fragments of cancer cell DNA in the blood. Currently, ctDNA tests are used to help identify the cancer’s subtype.
Standard blood tests can also help monitor the cancer and how the patient is responding to treatment.
Treatment
Your treatment for lung cancer will be customized to your particular needs. It may include one or more of the following therapies to treat the cancer and help relieve symptoms.
Lung cancer surgery
Surgery is one of the primary treatments for lung cancer.
In some cases, patients get cancer drugs or radiation therapy before surgery to shrink the tumor. Patients may also get these treatments after surgery to kill any remaining cancer cells, including cells that have spread to other parts of the body.
During lung cancer surgery, part of the lung with the tumor is removed. Simple procedures remove just a small section of lung. More complicated surgeries remove larger sections or even the entire lung. In some cases, nearby structures are also removed.
There are different approaches to lung cancer surgery.
One method is open surgery. This is the traditional approach. Surgeons perform the procedure through a four- to eight-inch incision between the ribs.
Minimally invasive surgery is the other main approach. These procedures require several smaller incisions, typically between ¼ and ½ inch. Minimally invasive surgery is usually less painful and has a shorter recovery time than open surgery. The two primary methods:
- Video-assisted thoracic surgery (VATS): VATS uses a small camera and instruments that are inserted into the chest cavity. VATS is typically performed on patients with small, early-stage lung cancers.
- Robotic-assisted Surgery: This technique uses robotic arms remotely controlled by the surgeon. Compared to VATS, it can offer better images of the surgical site. The surgical instruments also have more dexterity. These features enable procedures that are more complex than possible with VATS.
The most common types of lung cancer surgery are below, starting with the simplest surgery that removes the least amount of lung tissue.
Wedge Resection
During a wedge resection, the tumor and a wedge-shaped piece of the lung that includes the tumor is removed.
Wedge resections are typically used to cure the cancer. They are a good option for patients with small, early-stage tumors. They are also performed on patients who have limited lung capacity and can’t tolerate losing a larger section of the lung.
Wedge resections are performed under general anesthesia. In most cases, doctors can use a minimally invasive technique that requires only a few small incisions. The procedure usually takes around two hours. Patients stay one to two nights in the hospital.
Segmentectomy
Segmentectomy involves removing a segment, or part, of the lobe where the cancer is located. This segment is larger than the section of lung taken during a wedge resection. These procedures are generally used to cure the cancer.
Like the wedge resection, a segmentectomy is usually performed on patients who have limited lung capacity and can’t tolerate losing a large section of the lung. This procedure is also a good option for patients with early-stage tumors generally measuring less than two centimeters.
Patients undergoing a segmentectomy are put under general anesthesia. Most surgeries use minimally invasive techniques that only need a few small incisions. The procedure usually lasts four to six hours. Patients typically spend two to three nights in the hospital after a segmentectomy.
Lobectomy
In a lobectomy, surgeons remove the lung lobe where the tumor is located. This is the standard procedure for patients whose cancer has advanced past the earliest stages. It is usually meant to help cure the cancer.
Lobectomies are performed under general anesthesia. In most cases, doctors can use minimally invasive techniques that only require a few small incisions. Based on the extent of the cancer, though, doctors may need to perform an open surgery.
Lobectomies usually last four to six hours. Patients typically stay two to five nights in the hospital, though two to three nights is the target stay.
Sleeve lobectomy
The sleeve lobectomy is a more complex form of lobectomy. It is usually part of a plan to cure the cancer.
Sleeve lobectomies are typically used when the tumor is in a more central part of the lung. This location places them near key structures like the pulmonary artery, which carries blood from the heart to the lungs, or the central bronchus, which moves air in and out of the lungs.
During the surgery, doctors remove the lobe with the tumor, along with part of the bronchus. The bronchus is then connected to the remaining lobes.
A sleeve lobectomy may not always be possible. When it is an option, it is preferred over a pneumonectomy (complete removal of the lung) since it preserves more functioning lung tissue.
Patients getting a sleeve lobectomy are put under general anesthesia. Most procedures are performed as open surgeries. Select cases may be done with minimally invasive techniques.
The full surgery usually lasts five to six hours. Patients usually stay in the hospital for three to five nights.
Pneumonectomy
Pneumonectomy involves removing the entire lung. This surgery is rarely performed. It is used only when the tumor’s location rules out other surgeries.
Pneumonectomies are performed under general anesthesia. The procedure requires an open surgery most of the time. In select cases, minimally invasive surgery is possible.
Pneumonectomies usually take five to six hours. Patients typically spend four to five nights in the hospital.
Patients who undergo a pneumonectomy need to care for their remaining lung for the rest of their lives after surgery. This includes taking steps to prevent lung infections and limit exposure to toxins like tobacco smoke.
Lymph node dissection and lung cancer surgery
Lymph node dissections are not a separate type of lung cancer surgery. Instead, they are procedures done at the same time as the surgeries above.
During a lymph node dissection, the surgeon will remove lymph nodes from the chest. Since cancer often spreads through these nodes, doctors will examine them under a microscope to find out if the lung cancer has moved outside the lungs. This will help doctors decide if you need more treatment after surgery, such as chemotherapy, radiation therapy or targeted therapy.
Recovering from a lung cancer surgery
Surgery for lung cancer permanently impacts the patient’s lung function and, in some cases, their physical capabilities. Full recovery to the patient’s “new normal” usually takes two to three months, though most improvement occurs in the first few weeks after surgery. Despite these changes, patients typically don’t face major limitations after surgery.
After their procedure, patients should start walking as soon as they can safely do so. Research shows this activity can speed up recovery.
In most cases, there are few restrictions following surgery. Patients can perform daily tasks like cooking and cleaning as soon as they feel ready. Patients who undergo simpler procedures like a lobectomy can often carry out these tasks the day they leave the hospital. If the patient had a more complex surgery, such as a sleeve lobectomy or pneumonectomy, a few days of recovery is often needed first.
People who work a desk job can return to work as soon as they feel able. After simple surgeries this usually happens a few weeks following the procedure, though some people return to work just a few days later. If the patient had a more complicated surgery, it often takes a month before they can return to work.
Returning to a job that requires physical labor takes more time. For simple procedures, the return to work is usually a few weeks after the surgery. More complex surgeries often take two to three months of recovery time before patients can start working again. These patients should start with light-duty jobs when they return.
Surgery for lung metastases
Lung cancer can often spread from the original tumor to multiple spots within the lung. Surgery may be a treatment option in these cases.
The patient’s case should be carefully reviewed by a team of doctors to determine if they are a good candidate for surgery. This decision is based on many factors, including the patient’s overall health, the condition of their lungs and the locations of the growths inside the lungs.
These patients usually undergo a wedge resection, segmentectomy or lobectomy. These operations can be challenging, so they are more likely to be done as open surgery.
Radiation Therapy
Radiation therapy uses powerful, focused beams of energy to kill cancer cells. There are several different radiation therapy techniques. Doctors use these to accurately target a tumor while limiting damage to healthy tissue.
Radiation therapy can be part of a plan to cure lung cancer. It can also be used to manage advanced disease and help relieve symptoms.
Learn more about radiation therapy.
Intensity modulated radiation therapy
Intensity modulated radiation therapy (IMRT) focuses multiple radiation beams of different intensities directly on the tumor for the highest possible dose. Volumetric modulated arc therapy (VMAT) is a type of IMRT that utilizes a rotating treatment machine to deliver radiation at multiple angles.
IMRT is the most common type of radiation used to treat lung cancer. It can be part of a plan to cure the cancer in combination with other treatments. It is also used to control the growth of advanced cancers and help relieve symptoms.
IMRT patients with lung cancer typically get three to six weeks of treatment every Monday through Friday. Each session usually lasts less than 30 minutes.
Proton therapy
Proton therapy is similar to standard radiation treatments like IMRT, but it uses a different type of energy that may allow doctors to target tumors more accurately. This limits damage to nearby healthy tissue and allows for the delivery of a more powerful dose of radiation.
For lung cancer, proton therapy is typically part of a treatment plan to cure the disease.
Patients typically get three to six weeks of proton therapy. Sessions are held every Monday through Friday. Each treatment lasts around 30 minutes.
Learn more about proton therapy.
Stereotactic body radiation therapy
Stereotactic body radiation therapy (SBRT) uses dozens of tiny radiation beams delivered at different angles to accurately target tumors with a high dose of radiation.
This treatment can be used to cure the cancer or to help control symptoms in patients with advanced disease.
Patients typically get one to five sessions, all in consecutive days. In most cases, each session takes under 45 minutes.
Read more about SBRT.
3D conformal radiation therapy
3D conformal radiation therapy uses three-dimensional scans to determine the exact shape and size of the tumor. The radiation beams are shaped by tiny metal leaves that are arranged to fit the tumor dimensions. It is typically used on its own, to help manage symptoms in patients with advanced disease.
Patients usually get this treatment daily, Monday through Friday, for up to 10 days. Each session typically lasts less than 20 minutes.
Because the treatment is designed to relieve symptoms, it has minimal side effects.
Radiation therapy side effects
Radiation therapy side effects often depend on the location of the tumor and the exact treatment the patient receives.
Short term side effects include:
- Fatigue
- Cough
- Shortness of breath
- Irritation or inflammation of lung tissue
Long term radiation therapy side effects:
- Scarring of lung tissue
- A narrowing of the esophagus, which can cause swallowing problems
- Heart damage
- Pain in the chest wall
- Rib fractures
Doctors design radiation treatment plans to prevent or limit these problems and will recommend radiation only when it is the best treatment for the patient.
Patients should talk to their care team about any side effects they experience. These side effects can often be prevented or minimized with treatment.
Targeted therapy for lung cancer
Targeted therapy drugs are designed to stop or slow the growth or spread of cancer. This happens on a cellular level. Cancer cells need specific molecules (often in the form of proteins) to survive, multiply and spread. These molecules are usually made by the genes that cause cancer, as well as the cells themselves. Targeted therapies are designed to interfere with, or target, these molecules or the cancer-causing genes that create them.
Targeted therapy can be used with surgery or radiation therapy as part of a treatment plan to cure lung cancer.
Learn more about targeted therapy.
Getting targeted therapy
Lung cancer targeted therapy drugs can be taken as pills or given as injections or IV infusions. The frequency of treatments depends on the patient’s specific needs.
Targeted therapy side effects
Side effects depend on the exact drug the patient is prescribed. Short-term side effects include:
- Dry skin and rash
- Changes to the fingernails and toenails
- Fatigue
- Diarrhea
- Liver inflammation
Long-term side effects include:
- Inflammation or infection of the skin around the nails
- Lung inflammation
- Cardiomyopathy. This is a rare side effect
In most cases, these side effects can be easily managed. Patients should talk to their care teams about any side effects they experience.
Read more about targeted therapy side effects.
Immune checkpoint inhibitors for lung cancer
Immune checkpoint inhibitors are a type of immunotherapy. They stop the immune system from turning off before cancer is completely eliminated. Patients may receive a single immunotherapy drug or multiple drugs in combination.
Immune checkpoint inhibitors can be used to help control the cancer. For patients whose cancer has metastasized, it can help manage symptoms and, in some patients, lead to remission.
Learn more about imune checkpoint inhibitors.
Getting immune checkpoint inhibitors
Immune checkpoint inhibitors are given by IV. Sessions usually last less than an hour.
Patients getting immune checkpoint inhibitors before surgery usually get three to four infusions, often with chemotherapy.
Patients treated after surgery typically get one infusion every three to four weeks for about a year.
If the cancer has spread to distant parts of the body patients generally get treatment for about two years.
Immune checkpoint inhibitor side effects
Short-term side effects for lung cancer immune checkpoint inhibitors include fatigue. Long-term side effects can include adverse reactions of the immune system, such as hypothroidism.
Patients should talk to their care teams about any serious side effects they may encounter and any side effects they are experiencing.
Read about immune checkpoint inhibotor side effects.
Chemotherapy for lung cancer
Chemotherapy drugs kill cancer cells, control their growth or relieve disease-related symptoms. Chemotherapy may involve a single drug or a combination of two or more drugs, depending on the type of cancer and how fast it is growing.
In many cases, chemotherapy is part of a treatment plan to cure the cancer. For patients with metastatic disease, the treatment can help relieve symptoms and may lead to remission.
Learn more about chemotherapy.
Getting chemotherapy
Chemotherapy is usually delivered by IV. The number of treatments varies depending on the patient’s specific condition.
Chemotherapy side effects
Short-term side effects include:
- Nausea and vomiting
- Fatigue
- Low blood counts
- Mouth sores
Long-term side effects of chemotherapy include:
- Neuropathy, which causes pain, tingling or numbness in different parts of the body
- Damage to ear tissue, which can cause hearing and balance problems
- Kidney damage
These side effects can typically be managed with medications and other interventions. Patients should talk to their care team about any side effects they experience.
Learn about the side efffects of chemotherapy.
Frequently asked questions
What is small cell lung cancer?
Lung cancer is traditionally categorized by the type of cell where it begins. Small cell lung cancers (SCLCs) make up about 15% of lung cancers and almost always are caused by smoking tobacco. The cancer often starts in the more central portions of the chest — in the bronchi, the two large tubes that carry air from the windpipe to the lungs. It usually grows and spreads quickly to other parts of the body, including the lymph nodes. Because this cancer is so aggressive, surgery is used less often for SCLC than for non-small cell lung cancers.
What are the stages of lung cancer?
Lung cancer stages are determined through various tests and procedures, including MRIs, CT scans, PET scans, and lymph node biopsies. The doctor will combine the results of these procedures to stage the cancer, using the TNM (tumor, node, metastasis) classification system.
Can you get lung cancer from smoking?
Yes, you can get lung cancer from smoking. UT MD Anderson recommends lung cancer screening if you’re age 50–80, are a current smoker (or a former smoker who quit within the past 15 years), and have a 20 pack-year smoking history (for example, one pack a day for 20 years or two packs a day for 10 years).
Is lung cancer hereditary?
Lung cancer is hereditary in some cases, and a family history of lung cancer is considered a risk factor. Some rare genetic conditions, such as Li-Fraumeni syndrome (LFS), are associated with an increased risk of developing lung cancer.
Is lung cancer curable?
Lung cancer is sometimes curable; it depends on the specific cancer a person has and how early the cancer was caught. Some lung cancers are very aggressive, while others are very responsive to targeted therapy and are curable if caught early.
How are CT scans used to diagnose lung cancer?
CT scans are used in certain instances, in combination with other tests, to help diagnose lung cancer. In the process of diagnosis, patients will typically undergo an imaging exam, usually a chest X-ray. Images alone are not enough to make a lung cancer diagnosis, but they can show areas of concern. If an image shows such an area, the doctor may order other scans, including a CT scan or a PET scan, to get additional details. If the findings of the image scans indicate cancer, the doctor will request the removal of tissue or fluid from the lung for examination. Obtaining a tissue or fluid sample is called a biopsy.
When is immunotherapy used to treat lung cancer?
Immunotherapy may be used in combination with chemotherapy as a treatment for lung cancer. However, its usefulness depends on the type of cancer being treated.
Why choose UT MD Anderson for your lung cancer treatment?
Choosing the right hospital may be the most important decision you can make as a lung cancer patient. At UT MD Anderson you’ll get treatment from one of the nation’s top-ranked cancer centers. Our expertise starts with the ability to accurately diagnose and stage even extremely rare cancers, then carries on through groundbreaking treatment and into survivorship.
As a patient at UT MD Anderson, you’ll see the benefits of care from a top-ranked cancer center. These include:
- Treatment from specialists who focus exclusively on lung cancer and other thoracic cancers, including radiation oncologists, medical oncologists, surgeons and pathologists.
- Molecular diagnosis of cancer cells, allowing doctors to identify which treatments have the best chance of success against your exact cancer.
- Expert surgical care designed to offer complete resection of your tumor and any involved lymph nodes.
- An enhanced surgical recovery program along with robotic and minimally invasive procedures that offer faster recovery times and less pain from surgery.
- Groundbreaking clinical trials that may not be available anywhere else. These include trials of new targeted therapies, immunotherapies and drug combinations.
UT MD Anderson patients also have access to all the services and support offered by one of the nation’s top-ranked comprehensive cancer centers. From counseling and support groups to integrative medicine and physical therapy, UT MD Anderson has all the support and wellness services needed to treat the whole person, not just the disease.
This support and care is available beyond UT MD Anderson’s campus in the Texas Medical Center. Through our Houston-area locations, patients throughout the region can get top-ranked care and personalized attention close to home.
They're focused on you as a person, and they're focused on fighting the disease. But they also show so much kindness and compassion.
Alexa DiVenere
Survivor


Featured Podcast:
Lung cancer in young adults: A survivor’s story
Treatment at UT MD Anderson
UT MD Anderson lung cancer patients can get treatment at the following locations.
Featured Articles

A passion for personalized medicine and lung cancer care

Stage IV lung cancer survivor: ‘Go straight to UT MD Anderson’

8 ways to say, ‘Don’t smoke around me’
Neoplasms 101: What they are and how they’re treated

Stage IV lung cancer survivor: Why you should start your treatment at MD Anderson
Advances in small cell lung cancer classification

MD Anderson helps survivor through three cancer diagnoses

Lung cancer survivor grateful for immunotherapy clinical trial
Clinical Trials
UT MD Anderson patients have access to clinical trials offering promising new treatments that cannot be found anywhere else.
Becoming Our Patient
Get information on patient appointments, insurance and billing, and directions to and around UT MD Anderson.
myCancerConnection
Talk to someone who shares your cancer diagnosis and be matched with a survivor.
Prevention & Screening
Many cancers can be prevented with lifestyle changes and regular screening.
Counseling
UT MD Anderson has licensed social workers to help patients and their loved ones cope with cancer.
Help #EndCancer
Give Now
Donate Blood
Our patients depend on blood and platelet donations.
Shop UT MD Anderson
Show your support for our mission through branded merchandise.
