- Emotional & Physical Effects
- Anemia and Cancer
- Appetite Changes
- Bleeding and Bruising
- Blood Clots and Anticoagulants
- Body Image
- Bone Health
- Bowel Management
- Cancer Pain Management
- CAR T-cell Therapy Side Effects
- Chemobrain
- Chemotherapy Treatment Side Effects
- Constipation
- Dehydration
- Diabetes Management
- Fatigue
- Hair Loss
- Heart Health
- Immune Checkpoint Inhibitor Side Effects
- Immunotherapy Treatment Side Effects
- Infections
- Lymphedema
- Managing Medications
- Mouth Sores from Chemotherapy
- Nausea
- Neutropenia
- Peripheral Neuropathy
- Pulmonary Embolism and Cancer
- Radiation Fibrosis
- Sexuality and Cancer
- Skin and Nail Changes
- Sleep Loss
- Stem Cell Transplant Treatment Side Effects
- Stress Reduction
- Targeted Therapy Side Effects
- Weight Loss
Skin and Nail Changes
You may experience changes in your skin and nails during chemotherapy treatment.
Dry skin
There are many things you can do to alleviate dry skin. Below are some tips:
- Bathe in lukewarm water. Avoid long, hot showers and bubble baths.
- Use mild soaps without fragrance. Consider a body wash, which may be more moisturizing.
- Pat yourself dry instead of rubbing.
- Use a hypoallergenic cream without fragrance to keep your skin moisturized.
- Avoid perfume, cologne or aftershave lotion. These products often contain alcohol which could dry or irritate your skin
- Drink enough liquid to stay properly hydrated.
Sensitivity to sunlight
You may be more susceptible to getting a sunburn or sun rash. Follow these tips to protect your skin from sun damage:
- Avoid prolonged exposure to sunlight.
- Do not use sunlamps or tanning beds.
- Use a PABA-free sunscreen with SPF 30 or greater and lip balm, no matter your skin tone.
- Wear protective clothing, such as long-sleeved cotton shirts, hats, sunglasses and pants, when outside.
Skin rash or itching
If you have a rash, blisters, itching, redness or peeling, report the condition to your care team immediately. The following may help you cope with the situation:
- Ask for medications to relieve itching.
- Bathe with fragrance-free body wash.
- Wear loose-fitting clothing.
Acne
It is possible that you could develop acne. Talk with your doctor about over-the-counter or prescription medications that could treat the condition without interfering with your chemotherapy.
Nails
Your nails may become darkened or develop white streaks or ridges. It's possible that they will become brittle, dry and cracked. They could lift up from the nail bed. These changes are temporary, but it is important to protect your hands and feet during that time to prevent infection or permanent nail loss. Follow the tips below:
- Gently trim or file nails. Do not cut too close to the nail bed.
- Do not get professional manicures or pedicures without your care team’s consent.
- Use lotions and creams to keep your nails and cuticles healthy.
- Wear gloves while cleaning around the house or yard.
- Do not use nail-strengthening products as they could irritate your skin or nails.
- Talk to your care team before applying artificial nails as they can breed fungal infection and mask nail changes due to treatment.
- Tell your care team if you experience redness, pain or other changes around your cuticles.
A skin infection called paronychia may occur around your fingernails or toenails. It is a common side effect of chemotherapy and usually occurs after two or more months of treatment. Signs of paronychia include:
- Painfully, red swollen area around the nail
- Pus
- Thickening or discoloration of the nail
If you need to treat paronychia, follow these tips:
- Soak your fingers or toes in a solution of one part white vinegar to 10 parts warm water for 15 minutes every night.
- Wear soft cotton gloves while working with your hands and when sleeping.
- Wear socks with soft padded shoes and slippers to protect your toes.
- Tell your doctor if your symptoms are not improving or worsen. You may need a prescription ointment or cream.
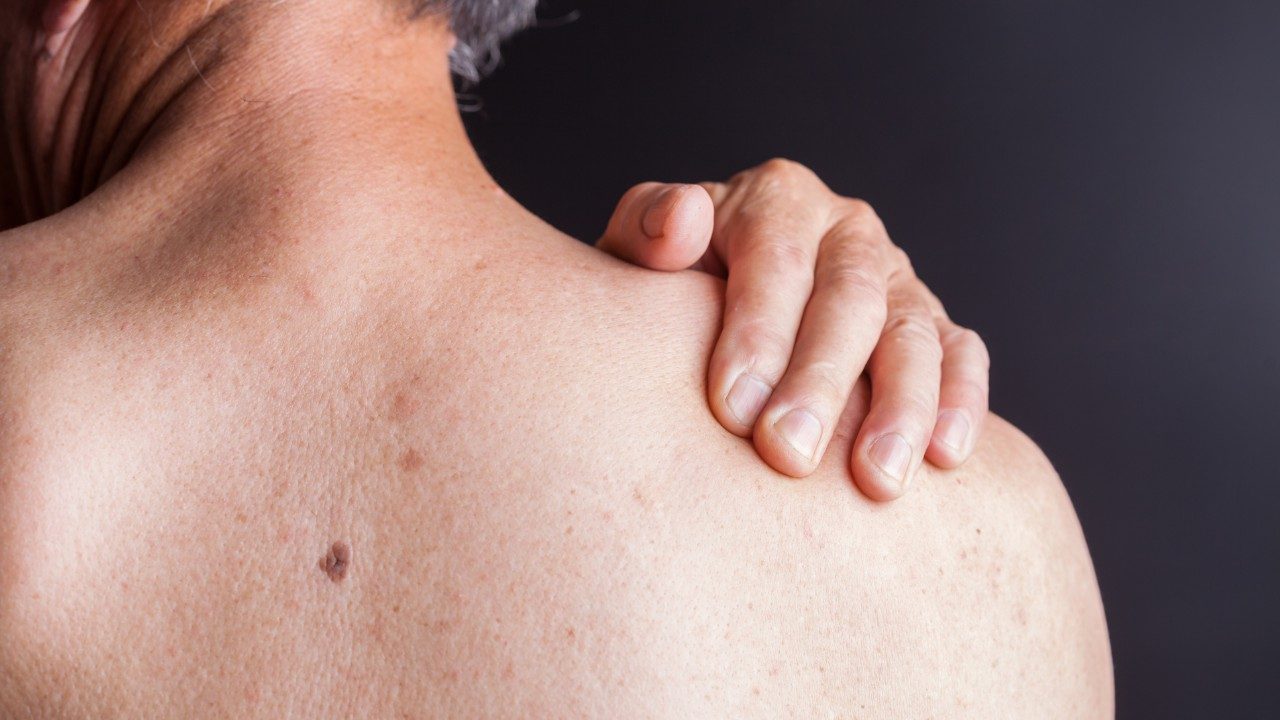
Cancer treatment side effect: skin changes
Did you know that cancer treatments can cause changes to your skin? Sometimes these changes are simply cosmetic, but other times they may require attention from your care team.
To better understand skin changes that happen during cancer treatment and how best to address these side effects, we spoke with Anisha Patel, M.D. Here’s what she had to say.
What types of cancer treatments cause skin changes?
All cancer treatments have side effects, but patients are sometimes surprised by the skin changes they see when receiving chemotherapy and immunotherapy. Since these therapies are used to treat a variety of cancers— and we’re constantly expanding and improving their use through clinical trials — skin changes are common.
What are common skin changes during cancer treatment?
The most common things we see are rashes and dry skin, which may be accompanied by itchiness or burning of the skin.
Chemotherapy and immunotherapy can also change the color, or pigment, of the skin, but it’s less common. You may not even notice. Depending on the therapy, you may see lightening or darkening of skin, hair and nails.
A less common side effect that we see with newer treatments is the development of new growths, such as moles, warts and raised areas of the skin.
It’s important to know that the type of skin side effect you may experience depends on your medical history and the type of treatment you’re receiving, so talk with your doctor about what you should expect.
Why do these skin changes happen?
Chemotherapy and immunotherapy fight cancer by targeting specific molecules in tumors. Those same molecules are also in our skin, hair and nails, so patients can experience side effects in those areas during cancer treatment.
Are these skin changes permanent?
Typically, changes to your skin related to chemotherapy and immunotherapy aren’t permanent. When you stop treatment, we’ll see your skin return to its previous state.
Also, these changes aren’t necessarily negative. Research has shown that certain rashes correlate with having a better tumor response to the treatment. So in some cases, when a patient gets a rash, despite it being uncomfortable and possibly itchy, it can be an indicator of a good overall treatment outcome.
What can I do to cope with skin changes during cancer treatment?
Unfortunately, you can’t avoid treatment-related skin changes entirely, but there are steps you can take to help reduce the discomfort. Before beginning cancer therapy, we suggest you start moisturizing your skin regularly. Also, if you have a history of eczema, psoriasis or skin cancer, see a dermatologist to address those concerns before beginning treatment so that they aren’t amplified during chemotherapy or immunotherapy.
Also, some types of chemotherapy and immunotherapy can make you more sensitive to the sun, so we commonly see sunburns. In order to prevent that, practice sun safety by limiting your time in the sun and wearing sunscreen with SPF 30 or higher, as well as sun-protective clothing, whenever your skin is exposed.
Lastly, try wearing comfortable shoes. We’ve seen a few therapies where patients experience an associated rash in areas that are under pressure such as the balls of the feet or with bunions. If your shoes are too tight and rub your feet, you’re at a higher risk of experiencing this rash.
Are any of these changes dangerous?
New growths related to cancer treatment can be concerning. Most are benign (non-cancerous), but others are malignant forms of skin cancer. It’s possible to develop skin cancer that’s caused by your cancer treatment, even if you’ve already received treatment for another type of skin cancer.
We advise our patients to conduct a monthly skin self-exam to catch these growths quickly. Let your oncologist know if something seems suspicious so that you can get a referral to a specialized dermatologist. If you’ve had a history of skin cancer or are at increased risk, make sure you see a dermatologist regularly during your cancer treatment. If you’re a patient at MD Anderson, you can ask your doctor to refer you to one of our dermatologists.
Is there anything else you’d like patients to know?
Don’t be alarmed if you experience skin changes during treatment. Helping patients cope with these changes is a big part of what MD Anderson’s dermatology team does. We may not always be able to make the change go away immediately, but we can help provide relief. Our goal is to make sure you’re as comfortable as possible so that you can continue on the best course of treatment for the cancer you’re facing.
Request an appointment at MD Anderson online or by calling 1-877-632-6789

Cancer treatment-related nail changes: 7 things to know
Cancer treatment can cause physical and emotional side effects. You may notice changes to your nails if you receive chemotherapy or certain targeted therapies as part of your cancer treatment.
But how long do these changes last, and how can they be managed? We spoke with dermatologist Anisha Patel, M.D., for answers to these questions and more.
What are the most common nail-related changes caused by cancer treatment?
The three most common are:
Ridging
Patients who receive cytotoxic chemotherapy, often used as the first treatment for breast cancer and colon cancer, may begin to see horizontal ridges on their nails. These ridges are called Beau’s lines. Every time a patient has an infusion, the nail plate stops growing. They may grow a little between infusions, but the temporary disruption creates ridges in the nails.
Nail lifting
Sometimes, patients’ nails may lift from the nailbed or come off completely. This can be caused by the chemotherapy drug taxotere or some targeted therapy drugs like fibroblast growth factor receptor (FGFR) inhibitors. It can be painful and may increase the risk of infection under the nail.
Nail fold inflammation
Certain types of chemo and targeted therapies can cause the cuticle to break down next to the nail. This is not a nail problem; rather, it’s a skin problem in which the skin on the side of the nail gets inflamed. You can also get infections on top of the inflammation.
Do these changes affect fingernails and toenails?
Yes, these changes can affect the nails on the fingers and toes. Patients will notice the effects more, depending on whether they use their hands or feet more heavily. For example, people who work in oil and gas and wear restrictive steel-toe boots may notice nail changes more on their feet.
How can these side effects be managed?
Of the three side effects mentioned, nail ridging is the least aggressive and usually doesn’t require any treatment.
If a patient’s nails are lifting, we often suggest clipping the nail back. This isn’t painful; it just looks funny to some patients.
We can do a small surgery in our clinic to help alleviate nail fold inflammation. We’ll numb the whole finger or toe, then split and pull away the lateral edges of the nail. Then we use a chemical like a high percentage phenol to remove the matrix, which is the tissue under the nail. This makes it so the nail doesn’t grow back on the lateral edges, and it gets rid of the friction point between the skin and the nail.
No matter the side effects, we don’t want infection on top of that. So, we ask all our patients to soak their nails in a rinse of one-half white vinegar and one-half water. This decreases the amount of bacteria and yeast and lessens the chance of surface infections. It’s an easy thing patients can do at home. We ask patients with nail fold inflammation to do the soaks every day and apply a steroid liquid at the edges of the nail to help it absorb in the skin.
How long do these side effects last?
Most patients’ nail changes are short-term, and their nails grow back healthy after they complete cancer treatment. But some nail changes from cytotoxic chemotherapy may be longer-term. Some patients may have a random nail that grows back thick and painful. We can take the nail off and see if it grows back normally. If it doesn’t, sometimes we’ll take the nail off and kill the whole matrix, so the nail doesn’t grow back at all. Often, patients would rather have no nails than nails that cause them pain.
It's hard to predict who will have longer-term side effects, and we won’t know until after they complete treatment. At that point, we try to address their symptoms as best we can.
What precautions should patients take with their nails during treatment?
Try to avoid getting manicures or pedicures. You do not want your cuticles manipulated. There is an increased risk of infection, and if you already have some treatment side effects, it could make them worse. Typically, the fingers and toes that experience more friction or pressure have worse inflammation.
We recommend gentle hand and foot care. Keep your hands and feet moisturized and avoid using abrasive or harsh chemicals. Lotions should be bland emollients like plain, white petrolatum. They shouldn’t contain any perfumes or active ingredients.
When should patients see their doctor about nail changes?
See your doctor if the nail changes cause symptoms, like if you’re having pain, or there’s an odor. Nail ridging is normal and doesn’t cause symptoms, so you wouldn’t need to see your doctor for that.
What else should we know about nail changes during cancer treatment?
Patients receiving chemotherapy can have increased pigmentation in their nail plate that does not go away. It’s not symptomatic, but many patients worry that they have nail melanoma, or skin cancer under their nail.
If you develop a new dark line on a single nail, you should seek medical care. But if you have reason to have pigment in your nails, such as a vitamin deficiency, and multiple nails are affected, it’s likely nothing to worry about.
Remember to be gentle and take care of your nails during cancer treatment. If you notice changes to your nails that cause symptoms like pain or an odor, see your doctor to get them checked out.
Request an appointment at MD Anderson online or call 1-877-632-6789.

Food allergies vs. cancer symptoms: How can you tell the difference?
Diarrhea, itching and rashes can all be signs of a food allergy. They could also be symptoms of some cancers, including colorectal cancer, pancreatic cancer, and leukemia.
So, how do you know if they’re due to food allergies or something else? And, when should you see a doctor about them?
We checked in with senior clinical dietitian Beverly Rodgers for advice.
What’s the difference between a food allergy and a food intolerance?
There are actually three categories to be aware of here:
- Food allergy
- Food intolerance
- Autoimmune diseases that affect the gut
A food allergy can cause gastrointestinal issues, such as gas, bloating and diarrhea. But a true allergy will also involve some degree of anaphylactic response, such as hives, itching or your airway closing up. Some people are so allergic to things like peanuts or shellfish that ingesting even the tiniest bit of them can be life-threatening. That’s why they carry around epinephrine injectors.
Food intolerances, on the other hand, are usually not dangerous — just very uncomfortable. One good example is lactose intolerance. That’s when you can’t digest milk or other dairy products because your gut lacks the enzyme needed to break down lactose properly, so you can absorb it.
Many foods — such as broccoli and beans — are known to cause gas. But they do that to almost everyone. Someone with an intolerance is going to be a little more sensitive to certain foods. They’ll experience symptoms after ingesting them that are closer to those of irritable bowel syndrome (IBS). A food intolerance can cause gas, abdominal pain, loose stools and sometimes even nausea.
IBS is one autoimmune disease that can affect the gut. Others include celiac disease, ulcerative colitis and Crohn’s disease. Since all of these involve some degree of inflammation, their symptoms tend to last much longer.
With an intolerance or an allergy, you’re usually fine once the offending food is no longer in your system. But if you have a medical condition like celiac disease, in which you absolutely cannot tolerate gluten, your body will let you know very quickly that it is not happy when you’ve ingested some. And once your gut is inflamed, it’s not tolerating much of anything after that. It’s going to take a while for a Crohn’s flare-up to calm down, too.
request an appointment online.
Help #EndCancer
Give Now
Donate Blood
Our patients depend on blood and platelet donations.
Shop UT MD Anderson
Show your support for our mission through branded merchandise.
