Learn the causes and effects of lymphedema.
- Emotional & Physical Effects
- Anemia and Cancer
- Appetite Changes
- Bleeding and Bruising
- Blood Clots and Anticoagulants
- Body Image
- Bone Health
- Bowel Management
- Cancer Pain Management
- CAR T-cell Therapy Side Effects
- Chemobrain
- Chemotherapy Treatment Side Effects
- Constipation
- Dehydration
- Diabetes Management
- Fatigue
- Hair Loss
- Heart Health
- Immune Checkpoint Inhibitor Side Effects
- Immunotherapy Treatment Side Effects
- Infections
- Lymphedema
- Managing Medications
- Mouth Sores from Chemotherapy
- Nausea
- Neutropenia
- Peripheral Neuropathy
- Pulmonary Embolism and Cancer
- Radiation Fibrosis
- Sexuality and Cancer
- Skin and Nail Changes
- Sleep Loss
- Stem Cell Transplant Treatment Side Effects
- Stress Reduction
- Targeted Therapy Side Effects
- Weight Loss
Lymphedema Prevention and Treatment
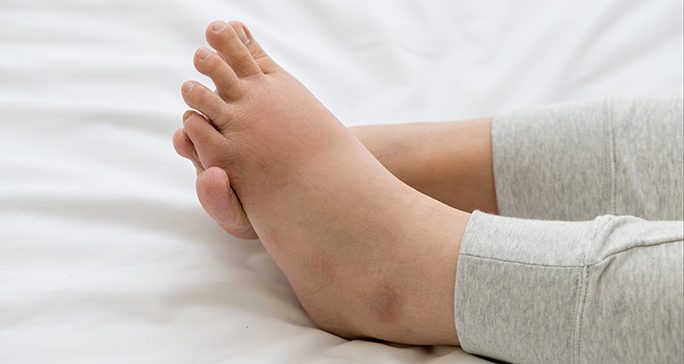
What is lymphedema?
Lymphedema is swelling, most often of the arm or leg, that occurs when fluid normally drained by the lymph vessels does not flow out of an arm or leg properly. It can occur following cancer treatment. Lymphedema can cause discomfort. It may cause clothes and jewelry to not fit well. It may also increase your risk for skin infections. If not treated, the arm or leg can become permanently swollen, hard, and heavy.
Lymphedema risk factors
You may be at risk of lymphedema if you have had surgery to remove some or all of the lymph nodes, or treated with radiation. You are at highest risk within three years of your surgery; however, the risk of getting lymphedema lasts a lifetime. You are at higher risk if you are overweight or gain weight during cancer treatment. An infection in the arm or leg can lead to lymphedema.
Lymphedema signs and symptoms
Some signs and symptoms may occur before swelling is noticed. These include a feeling of heaviness, tightness, or fullness. Rings, watches, or jewelry may feel tight.
Preventing lymphedema
There are several steps you can take to help reduce the risk of developing lymphedema.
- Avoid injury to the arm or leg, since even a small infection can trigger lymphedema.
- Treat any cuts, burns, bites or scrapes immediately.
- Wear long oven mitts when cooking and gloves when gardening or doing yard work.
- Wear high-factor sun block or long-sleeved clothing to avoid sunburn.
- Use insect repellant when outside.
- Use an electric shaver or cream for hair removal; do not use a razor.
- Whenever possible use the arm without lymphedema when checking blood pressure or for blood tests.
- Maintain an active lifestyle and healthy weight.
- Begin a weight-loss program if you are overweight.
- Call your doctor right away if you have fever, redness, tenderness, or warmth of the arm or leg. These can be the first signs of lymphedema.
- Do not move or carry very heavy objects.
- Do not use saunas.
- Check your hand and arm daily for signs of lymphedema or small injuries that could lead to the condition.
- When cleared by your doctor, do the recommended exercises to regain a full range of motion of the arm or leg.
Lymphedema Care
Lymphedema surgeries are performed by our Center for Reconstructive Surgery. Symptoms can be managed with the help of MD Anderson's Rehabilitation Services.
Manual lymph drainage: What to know about exercises for lymphedema relief
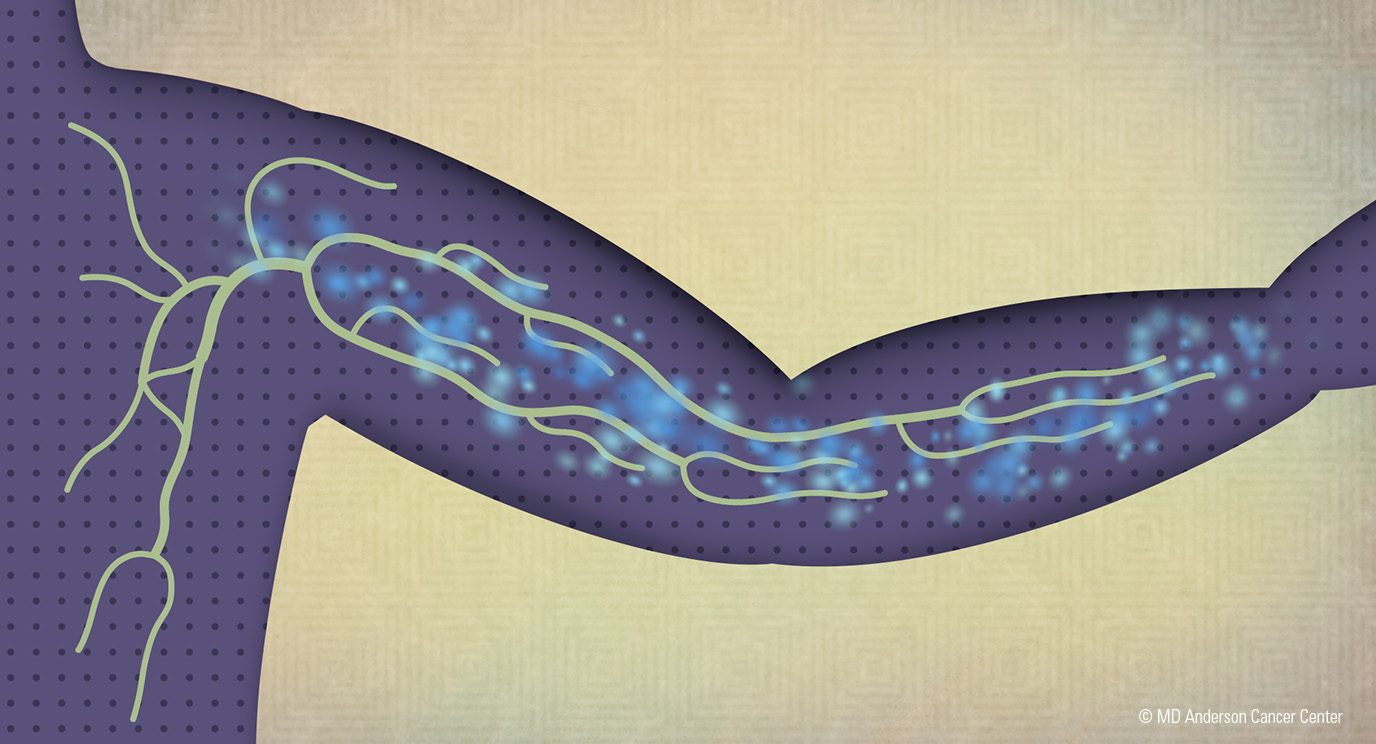
Lymphedema is the build-up of a protein-rich fluid in your arms or legs due to a disturbance in your lymphatic system.
Worldwide, its most common cause is an internal parasite transmitted by mosquitoes. Very rarely, it can be due to a birth defect. But in the United States, lymphedema is usually the result of surgery, radiation therapy and certain types of chemotherapy or immunotherapy used to treat breast cancer.
Manual lymph drainage (MLD, sometimes mistakenly called “massage”) is a tool that physical therapists use to give patients with lymphedema some relief. MLD redirects the excess fluid out of swollen limbs and into an area of the body that has not been affected, so it can be filtered out and excreted properly. There are also some exercises you can do on your own to help remove this fluid.
But which techniques are considered the best for lymphatic drainage? How often should you do them? And, are all exercises and MLD techniques safe for every cancer patient?
Read on for answers.
How do I know if I need lymphatic drainage?
Not everyone who undergoes cancer treatment or has lymph nodes removed or a biopsy will develop lymphedema. You can have a compromised lymphatic system but still have the reserve capacity to compensate for the loss. You only start seeing symptoms when your body exceeds that capacity.
Here are the early warning signs we talk to our patients about:
- Feelings of heaviness in your arms or legs
- Feeling like your arm or leg is swollen, even if it’s not visible
- Seeing swelling while looking in a mirror
- Noticing that your clothes don’t fit right (e.g., one sleeve is tighter than the other)
- Noticing that your rings don’t fit anymore
- Having to loosen up or add links to your watch or wristband
When should I see a doctor about lymphedema?
It’s much easier to treat lymphedema in its earlier stages than it is in its later stages. So, if you notice any of these issues, let your care team know immediately. Once lymphedema is very advanced, some damage may be irreversible.
Which exercise is the best for lymphatic drainage?
There’s no one-size-fits-all answer because no one thing works well for everybody. Both the manual lymph drainage techniques we use and the exercises we give to patients to do on their own are highly customized.
Physical therapists here at MD Anderson have a list of 18 distinct steps we can take to relieve lymphedema through MLD. But we don’t necessarily use all of them every time because each patient is different. Sometimes, patients can’t do certain steps, whether due to scarring or a limited range of motion. Others might have a particular condition that would cause additional issues if we took a particular step. So, we create individualized plans for every patient.
That’s why I highly recommend contacting your MD Anderson care team and asking for a referral to Physical Therapy as soon as you notice any of these symptoms.
Can I drain excess lymph myself?
We do sometimes teach people how to do this themselves. But again, any exercises we might recommend would be highly customized to you. There’s nothing universal we can share.
What happens to your body after manual lymph drainage or exercise?
Both of these activities redirect excess fluid into an area that can safely return it to the body. So, if you followed a drop of that fluid from, say, the end of your fingertip to its final destination, it would travel up your arm and into what’s known as a terminus in your neck. From there, it would enter your circulatory system, and either be carried along in the bloodstream until it was no longer needed or sent to your kidney for immediate excretion.
Lymphedema Treatment and Surgery
Lymphedema treatment
If you think that you have lymphedema, ask your doctor to refer you to Rehabilitation Services at MD Anderson, where a lymphedema therapist will evaluate you, give you information, and create a treatment plan. This plan may include one or more of the following:
- Skin care: Good hygiene and proper moisturization can help prevent injury and infection.
- Massage: Two basic types of massage are used to treat lymphedema.
- Manual lymphatic drainage is a precise and gentle form of massage that helps mobilize the fluid and direct it to other pathways.
- Soft tissue mobilization is a type of massage used to release scar tissue and other tightness that might be contributing to the swelling. Sometimes massage is taught to patients or family members to carry out at home.
- Exercise: You may be instructed in stretching exercises to loosen the tissues in the region or specialized exercises to help move the fluid out. You will be given written instructions for these exercises.
- Bandaging: This is a precise technique using cotton low-stretch bandages to apply constant pressure on the limb. Bandaging is usually done in combination with other methods.
- Compression garments: These are elastic fabric garments similar to a girdle or support stocking. They apply pressure to the arm or leg to help move fluid out and keep new fluid from collecting.
- Medicine: Sometimes antibiotics or other medications are prescribed as part of your lymphedema treatment plan.
Lymphedema surgery
If these therapies aren’t effective, surgery may help reduce the symptoms and swelling of lymphedema. Surgeons at MD Anderson's Center for Reconstructive Surgery specialize in lymphedema surgery and perform pioneering procedures to treat the condition. These procedures improve drainage of the lymph fluid, lessening the effects of lymphedema and keeping it from getting worse.
Patients who have less severe lymphedema for a shorter time tend to have better results from surgery. In some cases, patients may be able to stop using compression garments completely. All lymphedema surgeries are effective in reducing the number of infections you may have.
While these surgeries may result in significant improvement of lymphedema, you should continue all therapies and treatments unless your doctor or rehabilitation specialist tells you otherwise. This includes compression, massage, skin care and exercise.
Your surgeon will review your medical history, physical examination findings, and test results to determine the best procedure for you. Lymphedema surgical procedures include:
Lymphovenous bypass: This is a minimally invasive procedure using a high-powered microscope, specialized instruments and sutures. Blocked lymphatic vessels less than half a millimeter in size are redirected to small veins. This improves the flow of lymphatic fluid out of the arm or leg and reduces the discomfort and swelling.
Vascularized lymph node transfer: The doctor removes lymph nodes from your trunk, neck, groin area, or from within the abdomen, preserving their delicate blood supply. These are reattached to blood vessels in the affected arm or leg using microsurgery. The lymph nodes continue to function normally and drain fluid from the arm or leg. If you have undergone a mastectomy, it may be possible to combine this procedure with breast reconstruction to treat your lymphedema. Tests are performed to reduce the risk of lymphedema if the lymph nodes are taken from near an extremity.
Liposuction debulking procedure: In chronic lymphedema, surgery to improve the fluid drainage may not be possible. Excess tissue that has grown due to the fluid can be removed with surgery. This is done using liposuction with minimal scarring. The appearance and function of the arm or leg are improved. The risk of future infections is reduced. The swelling will not return if compression garments are worn lifelong.
Information and Self Care for Lymphedema
request an appointment online.
Help #EndCancer
Give Now
Donate Blood
Our patients depend on blood and platelet donations.
Shop UT MD Anderson
Show your support for our mission through branded merchandise.