request an appointment online.
- Diagnosis & Treatment
- Cancer Types
- Oral Cancer
Get details about our clinical trials that are currently enrolling patients.
View Clinical TrialsOral cancer (also known as mouth cancer or oral cavity cancer) is most often found in the tongue, the lips and the floor of the mouth.
Oral cancer (also known as mouth cancer or oral cavity cancer) is most often found in the tongue, the lips and the floor of the mouth.
It also can begin in the gums, the minor salivary glands, the lining of the lips and cheeks, the roof of the mouth or the area behind the wisdom teeth.
Most oral cancers arise in the squamous cells, which line the mouth, tongue, gums and lips. These are called squamous cell carcinomas (cancers).
Salivary gland cancers are not squamous cell carcinoma. These cancers develop deeper in the tissue. Most form from mucoepidermoid cells, which line the minor salivary glands.
Learn more about salivary gland cancer.
Cancer can also develop in the bones of the mouth. Learn more about bone cancer.
Not all tumors or growths in the mouth are cancer. Some are benign (not cancer), while others are precancerous, meaning they may become cancer but are not currently cancer.
Oral cancer risk factors
Anything that increases your chances of getting cancer is called a risk factor. Many cases of oral cancers are linked to risk factors. Some patients will develop oral cancers without any known risk factors. The main risk factors for oral cancer are:
Tobacco use: Many people diagnosed with oral cancer use tobacco in some form. These include cigarettes, cigars, pipes and chewing tobacco. The longer people use tobacco and the amount they use increases that risk.
The type of tobacco people use can influence where oral cancer develops. Cigarette smoking can cause oral cancer anywhere in the mouth. People who use chewing tobacco or snuff are more likely to develop cancer of the gums, cheek and lips. Pipe smoking increases the risk for cancer of the lip and the soft palate. Living with a smoker or working in a smoking environment can cause secondhand or passive smoking, which also may increase risk.
Alcohol: Many people diagnosed with oral cancer are heavy drinkers, consuming more than 21 alcoholic drinks each week. The combination of tobacco and alcohol is particularly dangerous. People who drink alcohol and smoke are far more likely to get oral cancer than people who do not drink or smoke.
Other risk factors include:
- Gender: About two-thirds of people diagnosed with oral cancer are men.
- Age: These cancers are found most often in people over 45.
- Prolonged sun exposure, which can lead to lip cancer.
- Long-term irritation caused by poor dental hygiene, including irritation caused by ill-fitting dentures.
- Poor nutrition, especially a diet low in fruits and vegetables.
- Taking immunosuppressive drugs.
- Having a previous head and neck cancer.
- Lichen planus, an auto-immune condition that affects the cells that line the mouth.
- Drinking maté, a beverage made from a type of holly tree common in South America.
- Chewing quids of betel, a stimulant common in Asia.
- Several genetic disorders, including Fanconi’s Anemia and Dyskeratosis Congenita.
Learn more about hereditary cancer syndromes. - Graft vs. Host disease: This is a serious side effect of stem cell transplantation. It can cause immune cells to target tissue in the oral cavity and lead to oral cancer.
Oral cancer prevention
Many oral cancers can be prevented. Some ways to minimize the risk of developing oral cancer include:
- Avoiding tobacco in all forms.
- Visiting a dentist at least once a year for a complete oral examination.
- Drinking alcohol only in moderation.If you have dentures, removing them at night and clean them daily. Have them evaluated by a dentist at least every five years.
- Eating a well-rounded, healthy diet with a variety of fruits and vegetables.
Because early diagnosis gives you the best chance of successful treatment, the Oral Cancer Prevention Clinic provides a specialized setting for diagnosis, monitoring and treatment of precancerous lesions. New optical techniques, which are less-invasive alternatives to biopsy, may help find some oral cancers earlier.
Learn more about oral cancer:
Oral cancer pictures

Leukoplakia, or white patch, of the bottom right side of the tongue. Pre-cancerous growths often present in this way.

Cancer of the lower lip.

A cancer of the tongue.
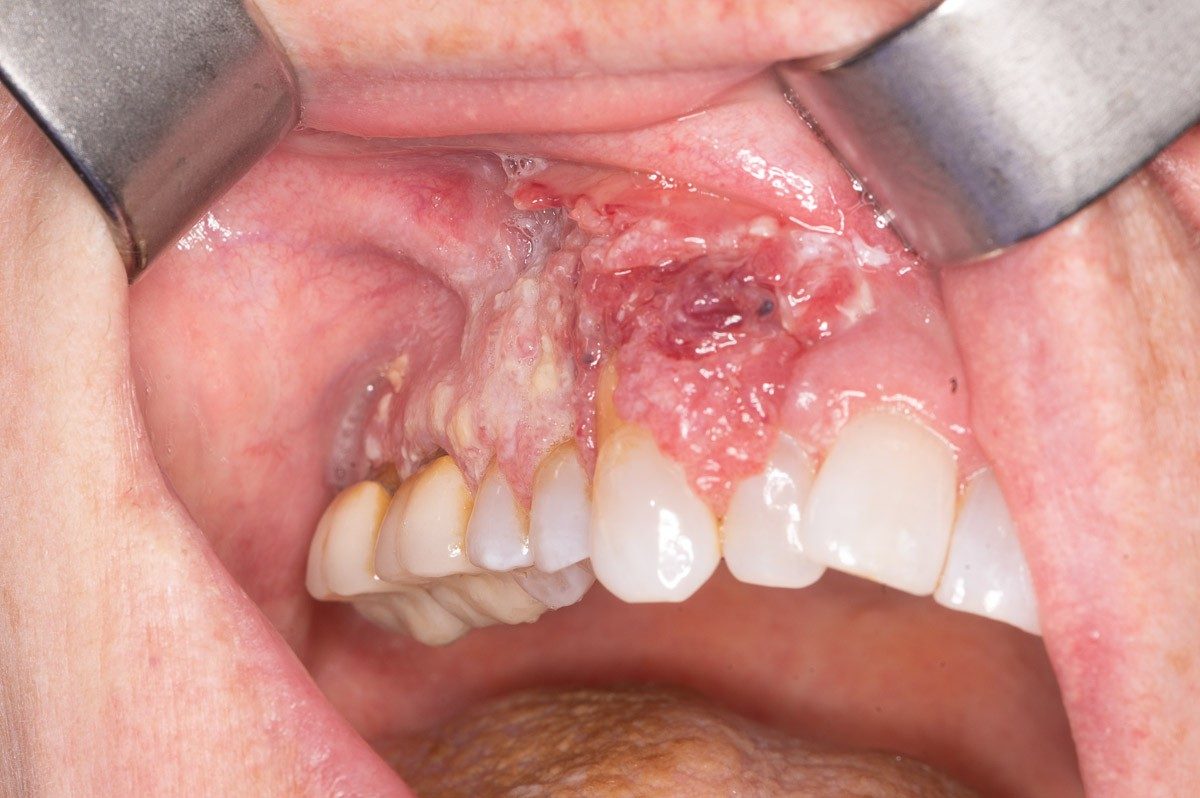
A cancer of the upper gingiva, or gum.

Cancer of the lower gums, behind the front teeth.

A cancerous lesion on the floor of the mouth, under the tongue.

A cancerous growth behind the last molar.
UT MD Anderson is #1 in Cancer Care

Tongue cancer survivor thriving after minimally invasive surgery
After Tim Turner began feeling pain in his jaw, doctors discovered an ulcer underneath his tongue. A CT scan and biopsy in early 2023 confirmed he had tongue cancer – again.
Because he’d had radiation therapy and chemotherapy to treat the initial cancer in 2021, Tim’s options were limited. His local doctors suggested surgery. Tim wanted a second opinion.
“My wife asked the radiologist where he would go for a second opinion if his wife had cancer,” Tim recalls. “He said, ‘MD Anderson.’”
Choosing MD Anderson for tongue cancer surgery
Tim requested an appointment online and received a call from MD Anderson within 30 minutes. He had an appointment a couple of weeks later with a multidisciplinary team led by head and neck surgeon Neil Gross, M.D. During the initial visit, Gross and the team laid out a plan that included undergoing a few rounds of chemotherapy and immunotherapy to shrink the tumor before surgery. Tim and his wife, Michele, discussed the plan and decided it was the best option.
Starting that March, Tim underwent three sessions of immunotherapy and chemotherapy. The tumor shrank, and as a result, he had less of his tongue removed during his surgery in May 2023.
Transoral single-port robotic surgery for tongue cancer
Tim underwent single-port robotic surgery, a minimally invasive approach through the mouth that helps patients recover faster.
“For selected patients with cancers of the tonsil or the base of the tongue, transoral single-port robotic surgery is better,” Gross says. “Using the robot allows us to avoid the old-fashioned approach of splitting the jaw.” During Tim’s 13-hour surgery, Gross used a single port robot to remove the tumor from the base of his tongue before plastic surgeon Z-Hye Lee, M.D., performed reconstructive microsurgery.
Tim stayed in the hospital for about a week after surgery. He used a feeding tube for three months, re-learning how to swallow, because of the prior radiation. A nurse ensured he knew how to set up his feeding tube when he returned home. Tim says learning how to eat and swallow again was the most difficult part after surgery.
“The feeding tube was a bit of a struggle and more boring than anything,” he says. “But at this point, I can eat just about anything I want to, and other than that, I don't have a complaint.”
Thriving after tongue cancer treatment
Today, Tim is back to work as a professional artist and enjoying his favorite activities like working out, hiking and visiting his grandchildren in Washington, D.C., and Switzerland. He created a series of paintings called “Songs of Celebration” that showcases collage work with teapots, flowers and wine cups – items that he associates with celebration.
“Making art has been good for me in many ways,” says Tim, who works in his studio every day. “It takes my mind off things as it did to get me through cancer treatment.”
Tim is grateful for his care team and that he chose MD Anderson for surgery.
“It absolutely could not be any better,” he says. “Everyone at MD Anderson is very informative, very compassionate. We couldn’t ask for a better team.”
Request an appointment at MD Anderson online or call 1-877-632-6789.

Proton therapy saved my ability to taste during treatment for tongue cancer
For Carlos Morera, the only symptom of oral cancer was a small lump beneath his jaw when shaving.
With a history of cancer, he knew that a swollen lymph node or a painless lump in the neck was among the most common symptoms of oral cancer.
“My first reaction was fear,” says Carlos. “I had undergone surgery for thyroid cancer the year before and was told the cancer was gone.”
His ENT told him not to worry but recommended a CT scan and a biopsy from a local surgeon near his home in Miami, Florida. That’s when he received the news that it was HPV-related tongue cancer, specifically squamous cell carcinoma of the right base of the tongue.
“I felt very nervous after receiving the news,” recalls Carlos. “I did not feel comfortable with the treatment plan I initially received. I wanted to explore other options because of the anticipated side effects.”
After talking it over with his wife, Edleen, he decided to look for a second opinion. He wanted to go to MD Anderson because of its reputation as the top cancer hospital in the nation and its expertise in proton therapy. Carlos knew about this advanced type of radiation therapy, which minimizes the impact of treatment on healthy surrounding tissues.
Settling in at MD Anderson for head and neck cancer treatment
In October 2023, Carlos traveled to Houston for his first appointment at MD Anderson to see head and neck surgeon Ryan Goepfert, M.D.
“Dr. Goepfert reassured me that I was at the best place for my care, and that made me feel comfortable,” says Carlos. Goepfert did not recommend surgery. Instead, he referred Carlos to radiation oncologist Steven Frank, M.D., who specializes in proton therapy, along with head and neck medical oncologist Renata Ferrarotto, M.D., for chemotherapy.
After meeting with Dr. Frank, Carlos felt better about his upcoming treatment. “I knew I was being treated by the best of the best and felt thankful for proton therapy,” says Carlos.
His care team talked to him about all the extra things that could help during treatment, such as yoga and acupuncture. “It’s not just about MD Anderson being the best. It’s how they treated us – it was phenomenal,” says Edleen. “From the time we got there, attention to detail was impeccable.”
Carlos and Edleen rented a house in Houston from November until his last treatment in January 2024. Their four children remained in Miami and joined them in Houston for the holidays. “It was a relief to know they did not have to see me go through treatment,” recalls Carlos.
Managing side effects from treatment
In November, Carlos began 33 daily proton therapy treatments, concurrent with six rounds of weekly doses of cisplatin, a type of chemotherapy. “I was expecting to feel bad from the chemotherapy medication, but I never did,” says Carlos. “My nurse, Shef Ghandi, and nurse practitioner, Ian Moore, kept me informed about preventive medicine to help me stay ahead of side effects.”
Carlos did not develop mouth sores, but his care team asked every day to make sure they only gave him the medication he needed and nothing unnecessary. To avoid losing weight, he made every effort to keep his diet the same. He maintained his normal exercise routine of walking twice a day for 15 minutes, along with doing yoga a few times a week.
Carlos feared losing his sense of taste from the radiation, but he only lost his taste for sweet foods. “My wife and I got to experience the different types of food at restaurants in Houston,” he says. He scheduled his treatments in the morning and would look forward to eating after treatment.
“Treating Carlos with proton therapy gave us the ability to reduce the radiation dose to the anterior tongue, which then allowed him to maintain his taste,” says Frank.
Carlos remembers the worst part of proton therapy was the anxiety he would feel before each treatment. His care team prescribed anti-anxiety medication. That helped prepare him for wearing the mask and mouthpiece needed to protect his teeth and jaw.
Doing the recommended exercises not only helped keep side effects to a minimum but also helped him manage his mental health. “Once you let your mind take over with worry, it makes it hard,” he says. “I kept getting mentally stronger with each week, as I found out it wasn’t as bad as I anticipated.”
Life after tongue cancer treatment
Almost a year has gone by since Carlos completed treatment. He is back to his normal routine with no major side effects, except for a change of perspective. “Now, when my kids drive me crazy, I appreciate them and everything we have so much more,” says Carlos. “I’m so thankful to be back to everyday life.”
Carlos met a fellow patient of Dr. Frank who was undergoing the same type of treatment he was. They talked every week. “Having a peer to talk to helped me prepare for what to expect throughout the process,” recalls Carlos.
Carlos also credits Edleen for being with him every step of the way. “She is my rock and the reason I did so well throughout treatment,” he says. “Her faith and support made me stronger every day.”
Carlos encourages others to do their research and understand their treatment options. “Take it day by day. It is hard not to worry, but stay positive and do not think the worst,” he says. “Be patient, pray and have a lot of faith. I was blessed to have found MD Anderson and the right team of doctors.”
Request an appointment at MD Anderson online or call 1-877-632-6789.
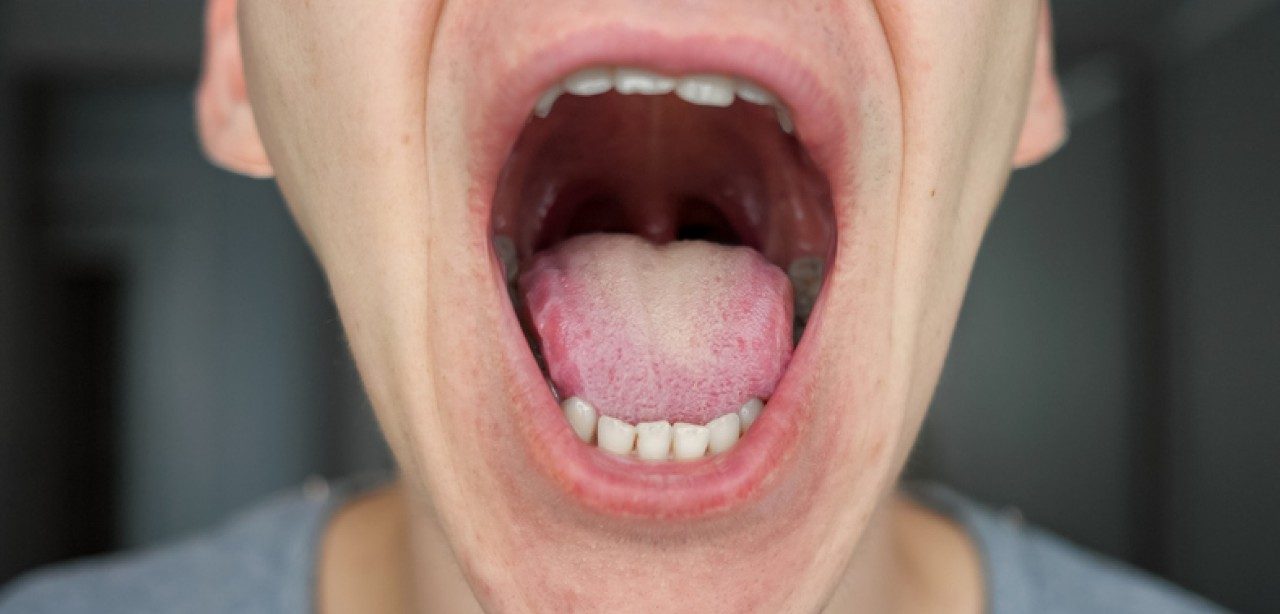
What does mouth cancer look like?
From eating and drinking to talking and breathing, you use your mouth constantly. With all that movement, you probably notice when something doesn’t feel right on your tongue, lips, gums or cheeks.
But what does mouth cancer look like? And when is a growth in your mouth something to worry about?
“Anything out of the ordinary should be shared with your doctor,” says head and neck cancer specialist Neal Akhave, M.D.
Here, he explains what mouth cancer, also called oral cancer, looks like. Use these insights so you know what to watch for.
Red or white spots in the mouth could be cancerous
To know what oral cancer looks like, you must first know what a healthy mouth looks like. Akhave points out that the inside of your mouth should be roughly the same color all over.
“If you notice any abnormal coloring in your mouth, that’s a red flag,” he adds.
Your care team may use the following medical terms to describe these spots:
Leukoplakia: From the Greek word for “white,” leukoplakia are light-colored spots inside the mouth. They can be cancerous or pre-cancerous and may be found on the lining of your gums or your tongue.
Erythroplakia: From the Greek word for “red,” these red spots appear on the inner lining of your mouth, tongue or cheeks.
Akhave suggests getting familiar with what the inside of your mouth looks like, from the roof to under your tongue and from cheek to cheek and along your gums. Cancerous spots may differ depending on their location:
Tongue: Look for a lump or ulcer on the top or bottom of the tongue, as well as any discoloration on either side.
Cheeks: Watch for small ulcers or tumors, as well as redness or bleeding.
Salivary glands: Check for bumps on your neck or the outside of the cheeks. These are often found while shaving or washing your face.
Gums: Look for redness, bleeding or lumps, especially without any injury to those areas. These can be in the bed of a tooth or on the surface of the gums.
Lips: Watch for discoloration, bleeding or bumps on the inside or outside.
Mouth cancer isn’t usually painful
Although mouth cancer can look like an ulcer or inflamed spot, it usually isn’t painful, especially early on.
“Tumors in the mouth usually just feel like a bump,” Akhave says. You may also have trouble swallowing if a tumor is deep in the mouth.
Leukoplakia or erythroplakia anywhere in the mouth may bleed if they’re irritated – but the bleeding isn’t painful either.
Rather, painful spots in your mouth are often signs of injury or infection. For example, canker sores can be quite painful, but they often go away after about 10 days.
If you notice anything in your mouth that lasts longer than that, Akhave recommends getting it checked out by a doctor.
Regular dental exams can screen for mouth cancer
Unfortunately, because mouth cancer doesn’t often cause severe symptoms, it’s often not diagnosed until it’s more advanced. That’s why Akhave stresses the importance of regular dental checkups, which can detect the earliest signs of mouth cancer.
“Your dentist can take note of any changes they see in your mouth,” he says.
If there’s anything suspicious, your care team may suggest a biopsy to test for cancer cells. Most cancers found in the mouth are squamous cell carcinoma since squamous cells cover many of the surfaces inside your mouth.
Reduce your risk of mouth cancer
Tobacco and alcohol use are the most common causes of mouth cancer, so avoiding these products can help reduce your risk.
Rarely, oral cancers can be caused by the human papillomavirus (HPV), but HPV is the most common cause of tonsil cancer or cancer on the back of the tongue. You should get the HPV vaccine if you are eligible. It’s recommended for everyone ages 9-26. Adults ages 27-45 should talk with their doctor about the potential benefits.
Although regular dental care can help detect oral cancer, Akhave says there’s no clear link between oral hygiene and cancer risk. “We know there are lots of bacteria in our mouths, but we don’t know how or if those bacteria interact with cancer cells.”
He adds that research is underway to better understand how bacteria affect oral cancers, like the research looking at the gut microbiome’s effect on patients with colorectal cancer.
“There’s still a lot we don’t know about mouth cancer, but clinical trials are changing that,” Akhave says.
Request an appointment at MD Anderson online or by calling 1-877-632-6789.
Why choose UT MD Anderson for oral cancer treatment?
Where you go first for cancer treatment matters.
At UT MD Anderson, your care for oral cancer is personalized. Your care team in the Head and Neck Center will include a surgeon, medical oncologist and radiation oncologist. They will work together, and with you, to develop a care plan customized to your specific needs and wishes. They can offer the most advanced therapies and pay special attention to minimizing side effects.
Treatments may include advanced surgical and reconstructive surgery techniques; cutting-edge cancer drugs like immunotherapy and targeted therapy; and highly targeted radiation treatments including proton therapy. As a top-ranked cancer center, UT MD Anderson also has multiple clinical trials covering all stages of oral cancer. Some of these trials may not be available anywhere else.
Oral cancer care teams also include specialists who can help improve your quality of life during and after treatment. These include speech pathologists who can help you maximize your ability to speak, chew and swallow.
UT MD Anderson also has dentists who specialize in caring for cancer patients. They evaluate patients with oral cancer and conduct any pre-treatment procedures necessary for their long-term oral health. Dental care after oral cancer treatment can be particularly challenging, so these treatments are essential to your quality of life. Our dental team also crafts custom-made prosthetics for patients who have portions of their jaw or other bones removed as part of cancer treatment.
And at UT MD Anderson, you're surrounded by the strength of the nation's largest and most experienced comprehensive cancer center. From support groups to integrative medicine services to social work counseling, we have the services needed to treat the whole person – not just the disease.
Cancer changed me. I see the beauty in all of this. I see life in a different perspective.
Phil Gonzalez
Survivor
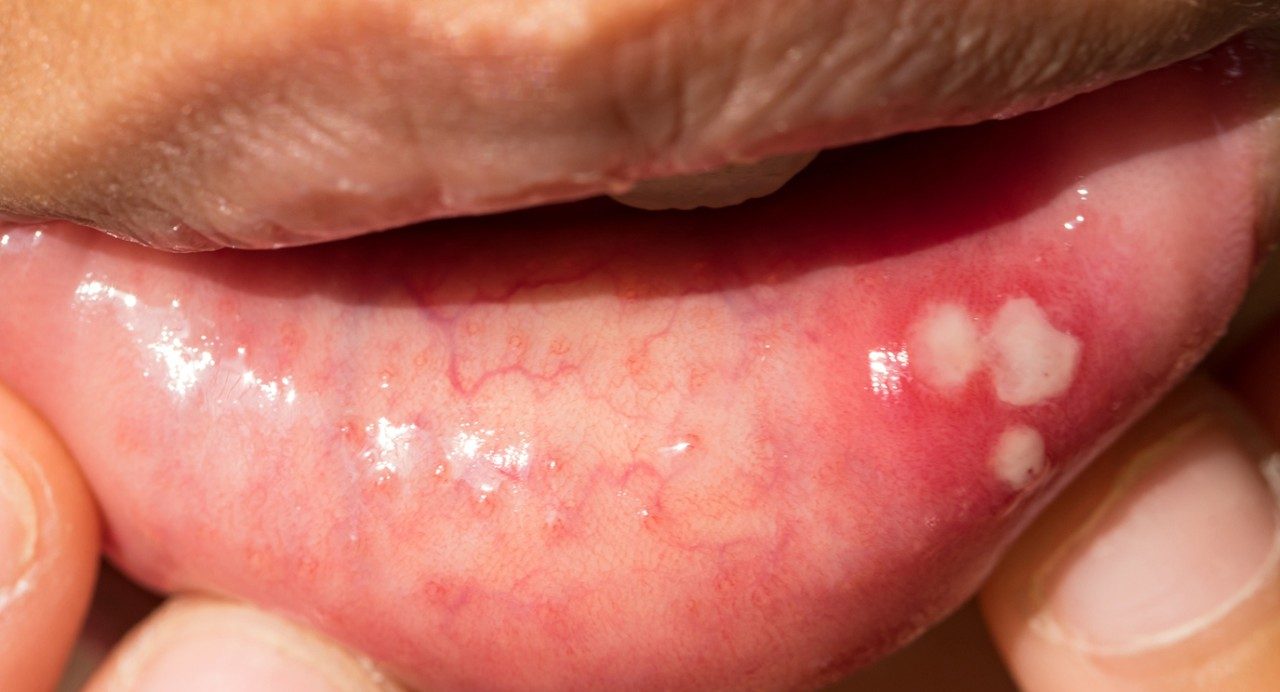
Canker sore vs. oral cancer: How can you tell the difference?
Most people experience a canker sore at some point in their lives. These small, often painful lesions can appear on any moist, fleshy surface inside the mouth. This includes the cheek, tongue, roof or gums.
Normally, canker sores heal on their own in about two to three weeks. So, how do you know if a mouth ulcer is a symptom of oral cancer or a harmless canker sore?
We checked in with Ann Gillenwater, M.D., director of MD Anderson’s Oral Cancer Prevention Clinic.
How do canker sores differ from oral cancers?
First of all, “canker sores” is not a medical term. It’s a term that some people use to describe many different unrelated conditions. We can continue to call them that here, for the sake of this article, but it’s important to note that the scientific name for what we’re discussing is actually “aphthous ulcers.”
Aphthous ulcers are painful little sores that develop inside the mouth. We don’t know exactly what causes them, but most resolve on their own pretty quickly.
Do canker sores develop in other locations on the body, too?
No. Aphthous ulcers only develop on the moist surfaces inside the oral cavity.
The painful cracks that sometimes develop in the corners of your mouth are called angular cheilitis or perlèche, and they tend to be caused by an overgrowth of yeast called “candida” or a vitamin B deficiency.
Ulcers that develop on the lips or as clusters of blisters around the mouth are usually caused by the herpes virus, especially if they’re preceded by a tingling sensation. These are also known as fever blisters or cold sores.
Are there any other conditions that can cause ulcers inside the mouth?
Oh, yes. Many things that aren’t cancer can cause ulcers inside the mouth. These include chickenpox, shingles, an inflammatory condition called lichen planus, and hand, foot and mouth disease, to name just a few.
How can someone tell if a mouth ulcer is an oral cancer instead of just a canker sore?
Here are the qualities I look for:
Appearance
The edges of a canker sore are often red and angry looking because the surrounding tissue is inflamed. That's not usually the case with cancers. Canker sores also tend to be flat. Oral cancers often have a tiny lump or bump under the lesions that you can feel.
Behavior
Oral cancer in its earliest stages is not usually painful. But canker sores often are. They become less painful as they heal.
Changes
See a doctor if you have a small spot that grows larger, a white spot that turns red, or a lesion that bleeds when it didn't use to.
Development
Does the lesion get worse or better over time? Most canker sores will heal on their own within two or three weeks. If yours doesn't, it's time to see a doctor.
Is there anything that cancer patients should know about canker sores?
Cancer patients who are receiving chemotherapy often develop mouth ulcers. I do a fair number of consultations each month with patients who are worried that these might be cancer.
The good news is that this type of mouth sore is just the body’s reaction to chemotherapy. So, it’s nothing to be worried about; it’s a well-known side effect of that particular treatment.
Request an appointment at MD Anderson online or by calling 1-877-632-6789.
Treatment at UT MD Anderson
Oral cancer is treated in our Head and Neck Center.
Featured Articles

Two-time tongue cancer survivor: Why I support research at UT MD Anderson

3 pieces of advice from a 5-time oral cancer survivor

Floor of mouth cancer: Symptoms, diagnosis and treatment
What is erythroplakia? Symptoms, causes and treatment

What can dipping and chewing tobacco do to your body? 5 things to know

Cancer of the jaw: 8 things to know

Oral cancer survivor: 5 quality of life hacks that I didn’t learn until survivorship
Clinical Trials
UT MD Anderson patients have access to clinical trials offering promising new treatments that cannot be
found anywhere else.
Becoming Our Patient
Get information on patient appointments, insurance and billing, and directions to and around UT MD Anderson.
myCancerConnection
Talk to someone who shares your cancer diagnosis and be matched with a survivor.
Prevention & Screening
Many cancers can be prevented with lifestyle changes and regular screening.
Counseling
UT MD Anderson has licensed social workers to help patients and their loved ones cope with cancer.
Help #EndCancer
Give Now
Donate Blood
Our patients depend on blood and platelet donations.
Shop UT MD Anderson
Show your support for our mission through branded merchandise.
