request an appointment online.
- Diagnosis & Treatment
- Cancer Types
- Salivary Gland Cancer
The salivary glands produce saliva in the mouth, throat and nose. Saliva supports digestion, protects teeth and helps stop infections that could enter the body through the mouth and nose.
The salivary glands produce saliva in the mouth, throat and nose. Saliva supports digestion, protects teeth and helps stop infections that could enter the body through the mouth and nose.
The salivary glands produce saliva in the mouth, throat and nose. Saliva helps with digestion, protects teeth and helps stop infections that could enter the body through the mouth and nose.
Salivary gland tumors form when a cell in a salivary gland mutates and starts rapidly growing and dividing. Most salivary gland tumors are benign, meaning they are not cancer and do not spread to other parts of the body.
Some are malignant, or cancer. These tumors can spread beyond their original location to nearby tissue, lymph nodes and distant parts of the body.
Salivary gland cancer is rare. Only around 2,000 to 2,500 cases are diagnosed in the United States each year. The disease’s five-year survival rate is 76%. The survival rate changes for different subtypes of salivary gland cancer, though.
Salivary gland anatomy
Each person has hundreds of salivary glands. There are two types of salivary glands: the major salivary glands and the minor salivary glands. Most saliva is produced from the three pairs of major salivary glands. Most salivary gland tumors occur in the major glands.
The major salivary glands are:
- The parotid glands. These are the largest pair of salivary glands. Most salivary gland tumors form in these glands. The parotid glands are located just in front of each ear. The facial nerve, which is responsible for facial movement, runs through each parotid gland and divides it into two lobes:
- The superficial lobe: Most parotid tumors start in the superficial lobe.
- The deep lobe: Some tumors start in the deep lobe. Tumors that start in the superficial lobe can also spread to the deep lobe.
- The submandibular glands. They are the size of a walnut and located below the jaw. They can often be felt below the jaw on each side of the face.
- The sublingual glands. These are the smallest of the major salivary glands. They are about the size of almonds. They are located below the tongue in the floor of the mouth.
The minor salivary glands consist of hundreds of much smaller glands that line the mouth, throat, and sinuses. They are too small to be seen by the naked eye. Minor salivary gland tumors are rare, but they are more likely to be cancerous than major salivary gland tumors. Many minor salivary gland cancers start in the roof of the mouth.
Types of salivary gland tumors
Most salivary gland tumors are benign, or not cancer. Benign tumors do not spread. However, they often need treatment because they can become quite large, and a small number of them can develop into cancer.
There are more than 20 types of malignant, or cancerous, salivary gland tumors. Different types can require different treatment plans. The most common types include:
- Mucoepidermal carcinoma, the most common type of salivary gland cancer. These tumors can be categorized as low-grade, intermediate grade and high-grade. Tumors with lower grades are usually less aggressive than those with higher grades.
- Adenoid cystic carcinoma, the most common tumor of the minor salivary glands and second most common of the major salivary glands. This tumor tends to grow along nerves, particularly the facial and trigeminal nerves.
- Acinic cell carcinoma, a common salivary gland cancer that has a tendency to recur at its original location.
Salivary gland cancer risk factors
Risk factors increase your chances of developing a particular disease. Risk factors for salivary gland cancer include:
- Age: Most cases of salivary gland cancer are diagnosed in people aged 55 or older.
- Prior radiation to the head and neck: Patients who received radiation treatment to the head and neck for another cancer have a higher risk of developing salivary gland cancer. Fortunately, the benefits of radiation therapy far outweigh this risk.
- Smoking: Smoking is a risk factor for some benign salivary gland tumors. Doctors are studying its connection to salivary gland cancer.
- Chemical exposure: Exposure to chemicals in certain industries increases the risk of some rare subtypes of salivary gland cancer. These industries include plumbing, carpentry and manufacturing rubber products.
- HPV infection: Human papillomavirus (HPV) can cause several different cancers, such as throat cancer and cervical cancer. There is some limited evidence that HPV may be a risk factor for salivary gland cancer. Doctors are studying this link. Learn more about HPV.
Learn more about salivary gland cancer:
Learn more about clinical trials for salivary gland cancer.
UT MD Anderson is #1 in Cancer Care
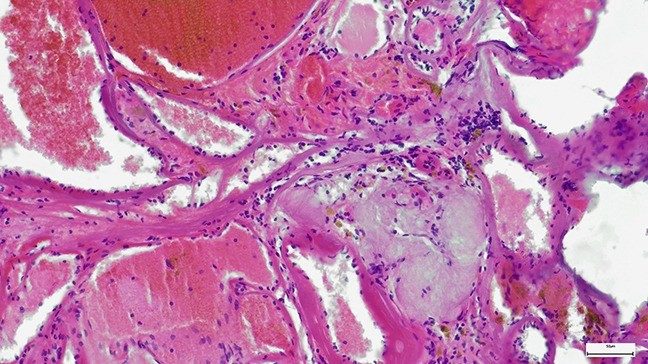
Understanding adenoid cystic carcinoma: Symptoms, treatment and outlook
Adenoid cystic carcinoma is a rare cancer of the secretory glands, which are glandular tissues that make and release substances such as saliva, tears and sweat. It can develop throughout your body, but it is most common in the salivary glands in your head and neck.
Here, I’ll share more about adenoid cystic carcinoma, including symptoms, prognosis and the research we’re doing to advance treatment.
How rare is adenoid cystic carcinoma?
Adenoid cystic carcinoma accounts for about 1% of all head and neck cancers. It is the most common tumor of the minor salivary glands and the second most common tumor of the major salivary glands.
What causes adenoid cystic carcinoma?
We’re not sure what causes adenoid cystic carcinoma. There are no known risk factors.
The median age of people diagnosed with adenoid cystic carcinoma is 50. It is slightly more common in women.
What are the symptoms of adenoid cystic carcinoma?
Adenoid cystic carcinoma typically grows very slowly. So, it may take years for symptoms to appear.
Your symptoms will depend on where the cancer is located and the size of the tumor.
The salivary glands are the most common site for adenoid cystic carcinoma. Your salivary glands produce saliva. Tumors in the salivary glands tend to grow along the nerves.
Your symptoms may include a painless lump in your mouth or throat, paralysis (weakened muscles) in the face or numbness in the face or neck.
Adenoid cystic carcinoma can also develop in the breast, ear canal, hard palate, lacrimal gland, nasal cavity, reproductive organs (male and female), skin, tongue and trachea. But these cases are much rarer.
These are the symptoms that adenoid cystic carcinoma in other organs can cause:
- Breast: lump in the breast that is sometimes sore or painful to the touch
- Ear canal: painless lump in or on the ear, ear pain, hearing loss
- Hard palate: painless lump, swelling or numbness in the roof of the mouth
- Lacrimal glands: watery eyes, bulging eyes, double vision
- Nasal cavity: congestion, facial pain or pressure, nosebleeds
- Reproductive organs: abnormal vaginal bleeding or discharge, mass in the vulvar area, difficulty initiating urination, frequent urination, blood in urine
- Skin: sensitive skin, lesions on the skin that may be painful, swollen or draining blood or pus
- Tongue: difficulty swallowing, speaking or moving your tongue
- Trachea (windpipe): wheezing, hoarseness, shortness of breath
How is adenoid cystic carcinoma diagnosed?
Doctors will usually order imaging tests, like a CT scan or MRI, to get images of the affected area. Depending on your symptoms, you may also have a PET scan, an ultrasound or swallowing tests. A biopsy is the only way to officially diagnose adenoid cystic carcinoma.
Getting the correct diagnosis is important
Because adenoid cystic carcinoma is so rare, it’s not uncommon for people to be misdiagnosed. The tumors can look very different under a microscope, so pathologists who don’t see as many of these tumors may not be able to identify them as adenoid cystic carcinoma. We’ve had patients who’ve gotten a biopsy elsewhere and are diagnosed with a different type of cancer. Then they come to UT MD Anderson, and our pathologists review the slides and determine that they actually have adenoid cystic carcinoma.
Delayed diagnosis is another challenge. The most common symptom of adenoid cystic carcinoma is a painless lump, which can mimic many other conditions, including benign tumors. Adenoid cystic carcinoma typically grows slowly, so doctors may not initially think of it when they see a new lump, and instead, opt to wait and see if it grows.
Misdiagnoses and delayed diagnoses can delay treatment or cause you to get the wrong treatment. That’s why it’s important to seek care at a comprehensive cancer center like UT MD Anderson that has pathologists who are experienced in diagnosing even the rarest of cancers.
How is adenoid cystic carcinoma treated?
Surgery followed by radiation therapy is the best treatment for localized adenoid cystic carcinoma tumors. “Localized” means the cancer is still confined to its original location in the body and has not metastasized, or spread.
The goal of surgery is to remove all or as much of the tumor as possible and then use radiation to kill any remaining cancer cells. If surgery is not an option, radiation is used to try to shrink the tumor or at least keep it from growing.
Adenoid cystic carcinoma can be tricky because it often comes back after treatment, sometimes years later. Most of the time, it returns as a distant recurrence. This means it has spread to other parts of the body. Adenoid cystic carcinoma typically does not spread to the lymph nodes.
Slow-growing adenoid cystic carcinoma usually comes back in the lungs. If you have lung metastases, your doctor may take a watch-and-wait approach to see if they grow larger and/or start causing symptoms. Your doctor may also recommend surgery or radiation to the lung metastases if there are only a few of them or if they are causing symptoms.
Chemotherapy or a type of targeted therapy called Vascular Endothelial Growth Factor Receptors (VEGFR) inhibitors may also be used to treat recurrent and metastatic adenoid cystic carcinoma.
Your care team will develop the best treatment plan for you.
Not all adenoid cystic carcinomas are the same
Adenoid cystic carcinoma is typically characterized as a slow-growing, stubborn cancer that often comes back in the lungs.
But that’s not always the case.
Researchers here at UT MD Anderson have identified a subgroup of patients who have an aggressive type of adenoid cystic carcinoma that grows quickly. This more aggressive type tends to spread to the bone and liver instead of the lungs.
If the cancer is caught early, we treat these patients right away.
What is the survival rate of adenoid cystic carcinoma?
Your prognosis will depend on many factors, including the cancer’s stage, the tumor’s characteristics and your overall health.
Your prognosis is better if you have a small tumor that can be cured with surgery and radiation rather than a metastatic tumor.
In general, people with early-stage adenoid cystic carcinoma have a 10-year survival rate of about 70%. In people with advanced disease, that 10-year survival rate can fall to around 30%.
Many patients can be cured. Not everybody has a recurrence, but when there is a recurrence, some people may live two years, while others may live more than 10 years.
We’re doing research at UT MD Anderson to find better markers to predict where patients are on that spectrum.
But remember, survival rates are just estimates of how long you will live after being diagnosed with or treated for cancer. It’s best to talk to your doctor about your specific prognosis.
What research is UT MD Anderson doing to advance adenoid cystic carcinoma treatment?
One of the challenges of adenoid cystic carcinoma treatment is that there is no real standard of care. So, we’ve been researching to understand more about the tumor biology. This will help us develop new therapies and classify patients, so they get appropriate surveillance and the best treatment based on how the tumor behaves.
We did molecular profiling on 54 adenoid cystic carcinoma patients and found two different groups:
- ACC1 is associated with solid histology and mutations in the NOTCH1 gene. It is more aggressive and more likely to metastasize, leading to poorer prognoses.
- ACC2 is typically not solid and has increased expression of the TP63 gene and receptor tyrosine kinases. ACC2 has better survival rates.
Based on this research, we have launched clinical trials tailored for each ACC group.
Adenoid cystic carcinoma clinical trials are not available everywhere. If you are diagnosed with adenoid cystic carcinoma, it’s important to seek treatment at a comprehensive cancer center like UT MD Anderson. Our experts take a multidisciplinary approach to your treatment, and we have research opportunities that might not be available elsewhere.
It’s really an exciting time. A decade ago, there were no clinical trials available for these patients. Now, I’m leading or co-leading five active clinical trials for adenoid cystic carcinoma that are showing real promise. Through my research, I plan to develop targeted therapies to help treat aggressive adenoid cystic carcinoma. I want to have better treatments – given to the right patients – that help extend patients’ lives and increase their quality of life.
Renata Ferrarotto, M.D., is a head and neck medical oncologist who specializes in treating salivary gland cancers and other rare head and neck cancers. She is also director of Head and Neck Medical Oncology Clinical Research at UT MD Anderson.
Request an appointment at UT MD Anderson online or call 1-877-632-6789.
Why choose MD Anderson for your salivary gland cancer care?
Choosing where to go for cancer treatment is one of the most important decisions a patient can make.
Every patient with salivary gland cancer is different. Treatment plans can change drastically based on the cancer’s subtype, as well as the tumor’s exact location. Just a few millimeters can make a huge difference. The right treatment plan can greatly reduce the chance that the cancer returns and help maintain your quality of life, including your ability to speak, swallow and hear.
At MD Anderson you’ll get care from a team of salivary gland cancer experts. As a top-ranked cancer center, our doctors see more salivary gland cancer patients in a year than most treat in a career. They have experience treating this rare cancer and understand how to deliver care in anatomically complex areas like the head and neck. They use this expertise to design treatment plans that are tailored to each individual patient.
This team will include a surgical oncologist, radiation oncologist and medical oncologist. All specialize in treating salivary gland cancer, giving them an incredible amount of expertise to call upon when planning your care. They will work together closely to discuss your case and develop a treatment plan designed for you.
Treatments can include many cutting-edge approaches, such as proton therapy and advanced robotic surgery. As a leading cancer center, MD Anderson is also developing new salivary gland cancer treatments, such as targeted therapies and immunotherapies.
Caring for salivary gland cancer patients at MD Anderson goes far beyond just eliminating the cancer. It includes maximizing your quality of life during and after treatment. Salivary gland cancer and its care may affect eating, hearing, speaking and appearance. At MD Anderson you’ll be offered a full range of treatments and supportive therapies to help you overcome these challenges.
You may get occupational, physical and speech therapy. If needed, you’ll have access to MD Anderson’s renowned reconstructive surgeons, as well as expert dental surgeons who can design and place custom-made dental implants. You can also work closely with speech pathologists and audiologists who have expertise in restoring speech and swallowing after salivary gland surgery.
MD Anderson also offers dedicated survivorship care for salivary gland cancer patients. This care can help monitor for the disease’s return and offer interventions to maximize your quality of life.
And at MD Anderson you will be surrounded by the strength of one of the nation's largest and most experienced cancer centers. From support groups to counseling to integrative medicine care, we have all the services needed to treat not just the disease, but the whole person.
My care team sought to improve every aspect of my life — not just cure the cancer. And they plan for success right from the get-go.
Glen Haubold
Survivor
Treatment at MD Anderson
Salivary gland cancer is treated in our Head and Neck Center.
Clinical Trials
MD Anderson patients have access to clinical trials offering promising new treatments that cannot be
found anywhere else.
Becoming Our Patient
Get information on patient appointments, insurance and billing, and directions to and around UT MD Anderson.
myCancerConnection
Talk to someone who shares your cancer diagnosis and be matched with a survivor.
Prevention & Screening
Many cancers can be prevented with lifestyle changes and regular screening.
Counseling
UT MD Anderson has licensed social workers to help patients and their loved ones cope with cancer.
Help #EndCancer
Give Now
Donate Blood
Our patients depend on blood and platelet donations.
Shop UT MD Anderson
Show your support for our mission through branded merchandise.


