request an appointment online.
- Diagnosis & Treatment
- Cancer Types
- Liver Cancer
Get details about our clinical trials that are currently enrolling patients.
View Clinical TrialsLiver cancer is one of the most rapidly increasing types of cancer in the United States. Often aggressive, this disease occurs when tumor cells develop from cells in the liver and divide uncontrollably. Liver cancer may prevent the liver and other organs from working properly.
Liver cancer is one of the most rapidly increasing types of cancer in the United States. Often aggressive, this disease occurs when tumor cells develop from cells in the liver and divide uncontrollably. Liver cancer may prevent the liver and other organs from working properly.
Liver structure and function
The liver is the largest solid organ in the body. It is located under your right ribcage. It is pyramid-shaped and has two sections called lobes.
The liver has two blood sources. The hepatic artery brings in oxygen-rich blood, while the portal vein supplies nutrient-rich blood from the intestines.
The liver plays an important role in many of the body’s processes. Some of its functions are to:
- Break down and store nutrients from the intestine
- Create clotting factors that stop bleeding
- Make bile that helps the intestine absorb nutrients
- Help the body get rid of waste
Liver cancer types
Primary liver cancer
Cancers that begin in the liver are called primary liver cancers. They are named after the types of cells where the cancer begins. These include:
Hepatocellular carcinoma (HCC): HCC is the most common primary liver cancer. This tumor begins in the liver’s hepatocyte cells. Sometimes HCC begins as a single tumor. Other times, it starts in multiple spots in the liver (multifocal). Multifocal HCC is more common in people with liver inflammation, such as cirrhosis.
- Fibrolamellar HCC: This rare HCC subtype doesn’t typically have underlying liver inflammation or known risk factors. Fibrolamellar HCC is more common in younger patients. It often has a higher chance for successful treatment than HCC.
Angiosarcomas and hemangiosarcomas: These rare, fast-growing liver cancers begin in blood vessels in the liver. They are usually not diagnosed until advanced stages.
Hepatoblastoma: This is a very rare type of liver cancer most often found in children. The survival rate is more than 90% if caught early.
Some tumors in the liver are benign, or non-cancerous. These may be difficult to diagnose or grow large and cause problems. They sometimes require surgery.
Secondary (metastatic) liver cancer
Tumors that start elsewhere in the body and spread to the liver are called metastatic liver tumors. The liver is a common place where cancer spreads. Its large size and high blood flow make it a target for tumor cells moving through the bloodstream. Any tumor can spread to the liver but it is more common in colorectal, breast and lung cancers.
Liver Cancer Risk Factors
Anything that increases your chance of getting liver cancer is a risk factor. Risk factors for primary liver cancers are detailed below. For liver metastases risk factors, please refer to the cancer of origin website.
Cirrhosis of the liver: Cirrhosis, or scarring or damage to the liver, is the leading cause of HCC. Certain conditions or activities can cause cirrhosis. This also makes them risks for liver cancer. These include:
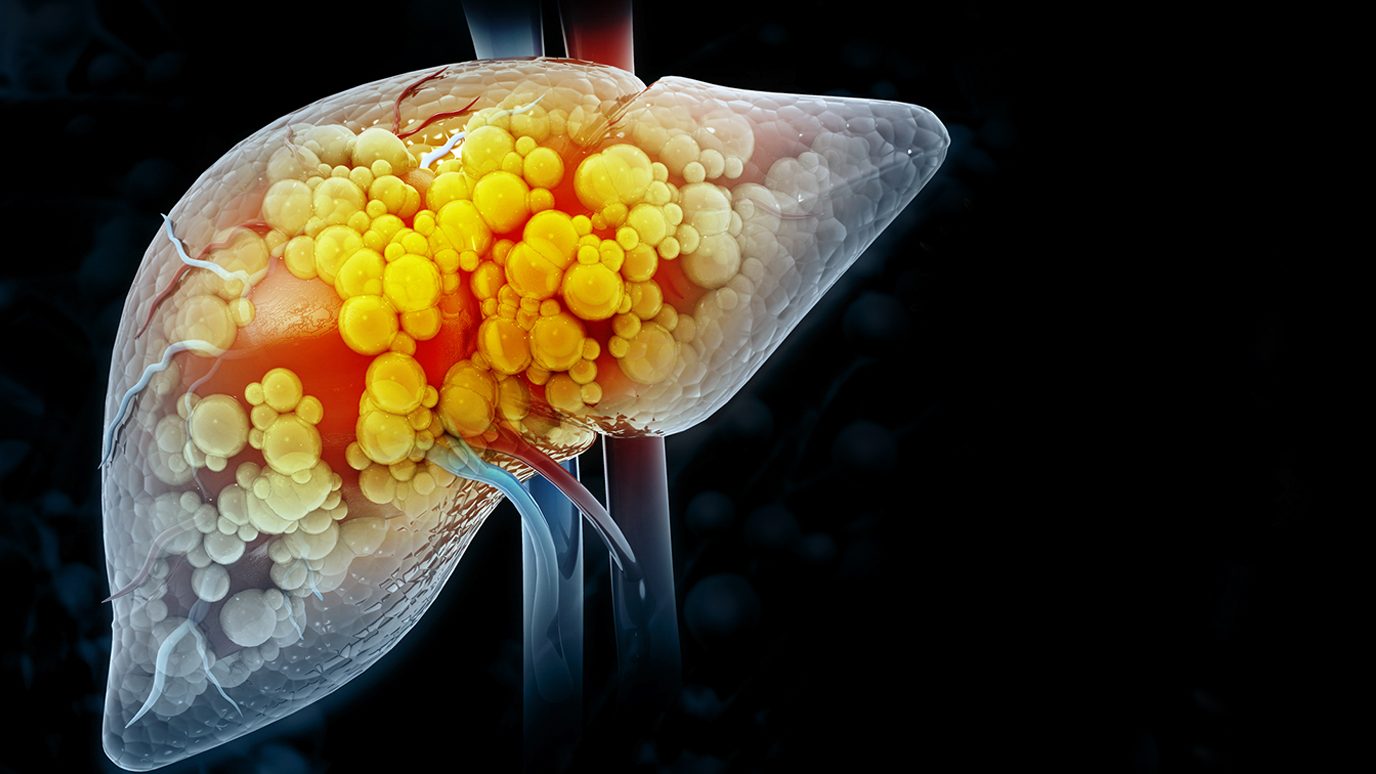
- Nonalcoholic steatohepatitis (NASH): Obesity, diabetes and high cholesterol can increase your risk of developing nonalcoholic steatohepatitis (NASH), a form of fatty liver disease. NASH causes fat to infiltrate your liver and can lead to cirrhosis.
- Chronic Hepatitis B or C virus infection: These infections are the most common risk factors for liver cancer worldwide.
- Alcohol use: Drinking excessive amounts of alcohol can lead to cirrhosis.
Age: Most individuals who get liver cancer are over 55. However, some rare types of liver cancer like fibrolamellar HCC and hepatoblastomas are almost always found in younger patients.
Ethnicity: Liver cancer rates in the United States are higher for Asian/Pacific Islanders and American Indian/Alaska Natives. Hispanic communities, including in South Texas, have one of the highest rates of HCC in the United States.
Geography: Liver cancer is more common in developing countries in sub-Saharan Africa and Southeast Asia than in the United States.
Gender: Primary liver cancers are more common in men than women. This may be because of differences in hepatitis carrier rates, environmental exposures, estrogen effects, or a combination of these factors.
Medical conditions: Any of the following may increase your risk for liver cancer:
- Obesity
- Diabetes
- High cholesterol
- Hereditary hemochromatosis
- Alpha-1 antitrypsin deficiency
- Acute intermittent porphyria
- Wilson disease
- Primary sclerosing cholangitis (PSC)
- Liver fluke infection
Exposure to chemicals and toxins: Exposure to certain chemicals and toxins may increase the risk of liver cancer. This is especially true when other risk factors are present. These include:
- Aflatoxins, a family of poisons produced by fungi found on some crops
- Betel nut chewing
- Arsenic
- Thorotrast
- Vinyl chloride
Tobacco: Using tobacco can increase your risk of liver cancer.
Anabolic steroids: Anabolic steroid use has been linked to benign (non-cancerous) liver tumors called adenomas. Some adenomas progress to HCC.
Family history: In rare cases, liver cancer can be passed down from one generation to the next. Genetic counseling may be right for you. Visit our genetic testing page to learn more.
Learn more about liver cancer:
MD Anderson is #1 in Cancer Care
11 things to know about liver biopsies
If you’ve been told you need a liver biopsy, you might have some questions. What will the liver biopsy reveal? Will the procedure hurt? How long will it take to recover?
Read on to find the answers to these and eight other questions patients ask me about liver biopsies.
What is a liver biopsy?
A liver biopsy is a procedure in which a doctor extracts a small amount of tissue from that organ using a needle and sends it off for examination under a microscope.
Why might I need a liver biopsy?
When an ultrasound, CT scan or MRI shows something unexpected in your liver that cannot be explained based on imaging alone, a biopsy can help us obtain an accurate diagnosis — whether that turns out to be liver cancer, a benign condition or something else entirely.
If a radiologist sees something suspicious in your liver on imaging and your physician is unsure of the cause, they may order a liver biopsy to figure out what’s going on. In patients with known cancer, the biopsy of cancerous lesions in the liver may also help guide treatment by looking for certain mutations.
Are there different kinds of liver biopsies?
Yes. At MD Anderson, our interventional radiologists perform about 140 image-guided liver biopsies per month. We use ultrasound, CT or MRI imaging during biopsy procedures to help us determine the best place to insert the needle and collect samples.
Most liver biopsies are performed targeting a specific lesion or abnormality. The rest are non-targeted, or not taken from any particular lesion within the liver. A fair number of liver biopsies are performed for reasons other than a cancer diagnosis.
Aside from liver cancer, what else can a liver biopsy detect?
Here are some conditions that a liver biopsy may reveal:
- abscess: a pus-filled pocket often caused by infection
- autoimmune disorders: includes inflammatory conditions such as auto-immune hepatitis
- cholangitis: inflammation of the bile ducts, which can be due to infection or inflammatory conditions like primary sclerosing cholangitis (PSC)
- cirrhosis: scar tissue in the liver
- cyst: a fluid-filled sac
- fatty liver disease: a build-up of fat within liver tissue; often seen with excess body weight
- focal nodular hyperplasia (FNH): a benign, or non-cancerous, lesion
- hemangioma: an abnormal collection of blood vessels that can mimic cancer on imaging
- hepatic adenoma: another type of benign tumor; uncommon
- infection
- inflammation
Keep in mind this isn’t an all-inclusive list; sometimes there are other things that a liver biopsy may reveal.
We also perform liver biopsies on patients who are in active cancer treatment because some therapies — such as chemotherapy and immunotherapy — can affect the liver. We monitor those patients’ liver function with blood tests, so we can quickly address any problems.
How long does a liver biopsy take?
The procedure itself usually takes 20 to 30 minutes, but sometimes it can take an hour or more. Depending on the complexity of the procedure, it could take as long as 45 to 90 minutes.
What are the risks of a liver biopsy?
The main risk is bleeding. We do everything we can to mitigate that risk and ensure patients can safely tolerate the biopsy. We use small needles specifically designed for biopsies. We typically ask patients taking blood thinners to stop these medications before a procedure. We also obtain bloodwork before any liver biopsy to assess clotting function and confirm that minimum parameters are met to allow for a safe procedure.
In most situations, bleeding due to a liver biopsy is minimal and resolves on its own. Rarely, additional procedures may be needed to stop the bleeding.
Another risk is pain. We may need to pass the needle in between ribs to access the liver, and there are many nerves there. In addition, the liver surface can be sensitive and may be an additional source of pain. Soreness after a liver biopsy can last for a few days. Most people will not have too much pain, though, and it’s easily treatable with over-the-counter pain relievers, such as ibuprofen or acetaminophen.
Infection is an additional risk, though it’s very uncommon.
Will I have to be put to sleep for a liver biopsy?
Not usually. Most patients only need local anesthetic and intravenous sedation to stay comfortable and relaxed during the procedure. Some people might need slightly deeper sedation than others, but it’s uncommon to need general anesthesia for a liver biopsy. The sedation needed for a liver biopsy may be administered by the Interventional Radiology team or a dedicated anesthesia team.
How painful is a liver biopsy?
The combination of local anesthetic and sedation usually keeps the process of getting to the liver itself fairly painless. Some people report feeling a little pain as the needle goes into the liver. That’s why a little soreness is common afterward.
Severe pain is unusual, though, and it can be a sign of something more serious, such as internal bleeding. In the rare cases when someone has a lot of pain after a liver biopsy, we will do a thorough examination, which may include additional ultrasound or CT imaging, to make sure we are not missing anything.
Is a liver biopsy considered a serious procedure?
Any procedure involving a major internal organ is serious by definition. The risk of any procedure is never zero. But liver biopsies are considered minimally invasive procedures that are safe with a relatively low rate of adverse events.
How long do you have to stay in the hospital after a liver biopsy?
The vast majority of liver biopsies are performed in outpatient facilities, and patients go home the same day. We usually monitor you afterward for at least three hours. You will be asked to stay in bed and not move around too much. This is usually not a problem, as most people are still tired from the sedation.
How long does it take to fully recover from a liver biopsy?
Patients can usually return to their desk jobs or those that don’t require any physical labor the next day. We advise patients to avoid heavy lifting for at least a couple of weeks. After that, they can return to their normal activities.
Zeyad Metwalli, M.D., is an interventional radiologist who specializes in minimally invasive, image-guided liver and vascular interventions.
Request an appointment at MD Anderson online or call 1-877-632-6789.
Liver cancer: What you should know
The liver is your body’s largest organ. It’s responsible for digestion, blood clotting and helping get rid of toxins. But unlike other organs, it has two blood sources. This makes the liver vulnerable to cancer cells moving through the bloodstream. The cancers that most commonly spread to the liver through the bloodstream are colorectal, breast and lung cancers.
When cancer starts in the liver, it’s called hepatocellular carcinoma. This type of liver cancer can start as a single tumor or as multiple spots on the liver caused by heavy drinking, obesity or a long-term hepatitis infection. These conditions cause scarring and permanent damage, known as cirrhosis of the liver.
To learn more about liver cancer symptoms, diagnosis and treatment, we spoke with Emma Holliday, M.D. Here’s what she had to say.
What are common symptoms of liver cancer?
Many patients don’t experience any symptoms in the early stages of liver cancer. When symptoms do develop, they may include abdominal pain or bloating, fatigue, nausea, vomiting, and yellowing of the skin or eyes, known as jaundice. Keep in mind that these symptoms vary from person to person.
Are some people more likely to develop liver cancer?
Hepatocellular carcinoma is more common in men than women, and the average age of diagnosis is 63.
Patients with cirrhosis of the liver are more likely to develop hepatocellular carcinoma, so it’s important to understand what can lead to cirrhosis:
- Alcohol consumption: Alcohol should be avoided. Talk with your doctor about what that means for you.
- Chronic hepatitis infection: Hepatitis B and C increase your risk, so it’s important to seek treatment if you have either of these infections. New antiviral medications can treat both types.
- Non-alcoholic fatty liver disease: This is caused by a buildup of fat in the liver. You can lower your risk by maintaining a healthy weight, eating a plant-based diet and staying active.
- Genetic conditions: Hemachromatosis, Wilson disease, Alpha 1-antitrypsin deficiency, porphyria and other rare conditions can lead to cirrhosis. If you have a family history of liver cancer, talk with your doctor about whether you should meet with a genetic counselor.
What are screening options are available for liver cancer?
National guidelines recommend routine screening liver cancer screening for patients with cirrhosis. This includes a blood test for a cancer marker called alphafetoprotein as well as an ultrasound looking for any suspicious liver masses. This screening regimen is typically done every six months. Your doctor can advise if this is right for you.
How is liver cancer diagnosed?
Talk to your doctor if you have any liver cancer symptoms. Your doctor may order a CT scan or an MRI along with an alphafenoprotein blood test to look for cancer. In some cases, CT scans or MRI results, along with blood test results, may be enough to make a diagnosis. But if the images aren’t clear, your doctor may remove a tissue sample for closer examination by doing a biopsy.
How is liver cancer treated?
The type of liver cancer treatment your doctor recommends will depend on the tumor’s size and location, whether you have cirrhosis, and your overall health.
If the cancer is early stage and your liver is healthy, surgery may be an option. If the tumors are small and haven’t spread to nearby blood vessels, your doctor may suggest a liver transplant.
Sometimes surgery isn’t an option, especially if the tumor is too large to be removed safely or is in a difficult location. In these cases, your doctors may recommend radiation therapy, which uses an external beam of X-rays or protons to destroy tumors. They may also suggest radiofrequency ablation, which uses a needle-thin probe to deliver electric currents directly to the tumor, heating it until it’s destroyed.
Another approach is to prevent blood flow from reaching tumors through a process called chemoembolization. A needle is inserted into an artery in the groin, and a tiny tube is threaded into the artery that leads to the liver to deliver drugs to the tumor. Afterward, the artery is blocked to prevent blood flow to the liver. In some cases, patients may instead undergo radioembolization, where the doctor injects liquid containing tiny radioactive spheres that treat the tumor.
Chemotherapy and immunotherapy may also be options for some patients.
What’s next for liver cancer treatment? Tell us about promising research developments and clinical trials here at MD Anderson.
Unfortunately, liver cancer is one of the most rapidly increasing types of cancer in the U.S. But we’re hopeful for the future based on new research. At MD Anderson, we have several clinical trials exploring new liver cancer treatments.
One clinical trial is comparing chemotherapy with a type of radiation called stereotactic body radiotherapy, which delivers a high dose of radiation precisely to the tumor while limiting exposure to healthy cells.
Another clinical trial is comparing proton therapy with intensity-modulated radiotherapy, and others are looking at T-cell therapy for patients with advanced liver cancer. MD Anderson is also investigating using microscopic glass beads called TheraSpheres to target tumors with internal radiation in a treatment called radioembolization.
What advice do you have for liver cancer patients?
There are many liver cancer treatment options, but not all options are right for all patients. And weighing through these treatment options can be overwhelming, so make sure you find a team of doctors you trust who can answer your questions and help you choose the right treatment for you.
Request an appointment at MD Anderson online or by calling 1-877-632-6789.
Why choose MD Anderson for your liver cancer treatment?
At MD Anderson, you're surrounded by the strength of one of the nation's largest and most experienced comprehensive cancer centers. Here, you’ll find support and wellness services that treat the whole person – not just the disease.
Personalized care
A team of experts work together to diagnose and treat your specific case. Your individualized liver cancer treatment plan includes the most advanced therapies while focusing on your quality of life. This includes the use of tumor mutational analysis and biomarkers to plan and guide your treatment.
Experience, innovation
Treatment for liver cancer can be complex. As one of the nation's most active cancer centers, MD Anderson has become a pioneer in the field of liver cancer staging and treatment. We have developed techniques and benchmarks that have been adopted by other cancer centers across the country and the world. These advances include immunotherapy, advanced surgical techniques, operations for liver disease that isn’t otherwise able to be treated with surgery, and embolization.
The goal? To make sure you are treated safely and effectively, recover quickly and can return to daily activities as soon as possible.
Pioneering the future of liver cancer care
MD Anderson researchers are devoted to learning more about liver cancer. MD Anderson’s Specialized Programs of Research Excellence (SPORE) grant is the only HCC SPORE grant funded by the National Institute of Health. Teams are studying the use of immunotherapy for earlier stages of HCC. They are also developing ways to screen high-risk patients for liver cancer and studying prevention strategies. Their goal is to improve patient outcomes and reduce death rates through early intervention.
MD Anderson offers clinical trials of new treatments for liver cancer. These include systemic therapy, radioembolization, chemoembolization, microwave ablation, SBRT, proton therapy, and more.
I feel there has to be some reason why I was left here. I think part of it was to share my story.
Mike Mason
Survivor
Treatment at MD Anderson
Featured Articles
Clinical Trials
MD Anderson patients have access to clinical trials offering promising new treatments that cannot be
found anywhere else.
Becoming Our Patient
Get information on patient appointments, insurance and billing, and directions to and around MD Anderson.
myCancerConnection
Talk to someone who shares your cancer diagnosis and be matched with a survivor.
Prevention & Screening
Many cancers can be prevented with lifestyle changes and regular screening.
Counseling
MD Anderson has licensed social workers to help patients and their loved ones cope with cancer.
Help #EndCancer
Give Now
Donate Blood
Our patients depend on blood and platelet donations.
Shop MD Anderson
Show your support for our mission through branded merchandise.