request an appointment online.
- Diagnosis & Treatment
- Cancer Types
- Myeloproliferative Neoplasms (MPN)
Get details about our clinical trials that are currently enrolling patients.
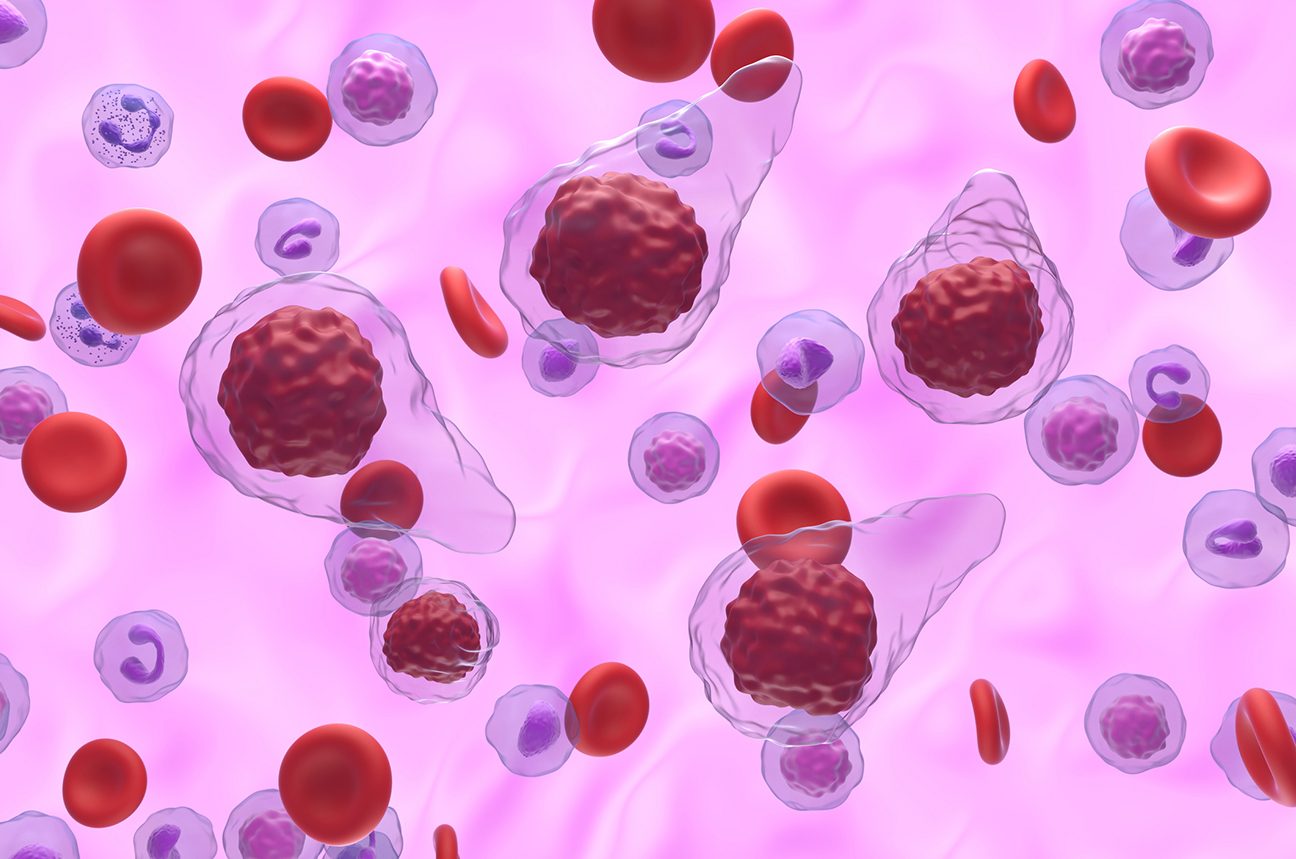
View Clinical TrialsMyeloproliferative neoplasms (MPN), previously called myeloproliferative disorders, are diseases of the bone marrow and blood. They can strike at any age, have no known cause and a wide range of symptoms and outlooks.
Myeloproliferative neoplasms (MPN), previously called myeloproliferative disorders, are diseases of the bone marrow and blood. They can strike at any age, have no known cause and a wide range of symptoms and outlooks.
Sometimes the disease progresses slowly and requires little treatment; other times it develops into acute myeloid leukemia (AML).
To understand what happens to your blood when you have MPN, it helps to know what makes up normal blood and bone marrow. There are three major types of blood cells: red blood cells (RBCs), white blood cells (WBCs) and platelets. These cells are made in the bone marrow and flow through the bloodstream in a liquid called plasma.
Red blood cells (RBCs), the major part of your blood, carry oxygen and carbon dioxide throughout your body. The percentage of RBCs in the blood is called hematocrit. The part of the RBC that carries oxygen is a protein called hemoglobin. All body tissues need oxygen to work properly. When the bone marrow is working normally, the RBC count remains stable. Anemia occurs when there are too few RBCs in the body. Symptoms of anemia include shortness of breath, weakness and fatigue.
White blood cells (WBCs) include several different types. Each has its own role in protecting the body from germs. The three major types are neutrophils, monocytes, and lymphocytes.
- Neutrophils (also known as granulocytes or polys) destroy most bacteria.
- Monocytes destroy germs such as tuberculosis.
- Lymphocytes are responsible for destroying viruses and for overall management of the immune system. When lymphocytes see foreign material, they increase the body’s resistance to infection.
WBCs play a major role in fighting infection. Infections are more likely to occur when there are too few normal WBCs in the body.
Absolute Neutrophil Count (ANC) is a measure of the number of WBCs you have to fight infections. You can figure out your ANC by multiplying the total number of WBCs by the percentage of neutrophils (“neuts”). The K in the report means thousands. For example:
- WBC = 1000 = 1.0K
- Neuts = 50% (0.5)
- 1000 X 0.5 = 500 neutrophils
Also, when you receive your blood counts, this equation may be written as polys plus bands = neutrophils. Further, while anyone can catch a cold or other infections, this is more likely to occur when your ANC falls below 500. Your WBC count generally will fall within the first week you start chemotherapy, but it should be back to normal between 21 and 28 days after starting chemotherapy.
Platelets are the cells that help control bleeding. When you cut yourself, the platelets collect at the site of the injury and form a plug to stop the bleeding.
Bone marrow is the soft tissue within the bones where blood cells are made. All blood cells begin in the bone marrow as stem cells.
The bone marrow is made up of blood cells at different stages of maturity. As each cell fully matures, it is released from the bone marrow to circulate in the bloodstream. The blood circulating outside of the bone marrow in the heart, veins and arteries is called peripheral blood.
Stem cells are very immature cells. When there is a need, the stem cells are signaled to develop into mature RBCs, WBCs or platelets. This signaling is done with “growth factors.”
Myeloproliferative neoplasm types
There are several types of myeloproliferative neoplasms. The main types are:
Primary myelofibrosis affects the red blood cells and granulocytes, a type of white blood cell. The cells don't mature normally and are irregularly shaped. Primary myelofibrosis also causes thickening or scarring of the fibers inside bone marrow, which can decrease the production of red blood cells and cause anemia.
Polycythemia vera (PV) is caused by the overproduction of red blood cells in the bone marrow, which then build up in the blood. Often, the spleen swells as extra blood cells collect there, causing pain or a full feeling on the left side. Itching all over the body is a symptom of PV.
Essential Thrombocythemia (ET) means that the number of platelets in the blood is much higher than normal, while other blood cell types are normal. The extra platelets make the blood "sticky," which slows down blood flow.
Chronic eosinophilic leukemia/hypereosinophilic syndrome (HES) is characterized by a higher than normal number of the white blood cells responsible for fighting allergic reactions and some parasitic infections (eosonophils). You may experience itching, swelling around the eyes and lips or swollen hands and/or feet. In some patients, HES may quickly progress to acute myelogenous leukemia.
Systemic mastocytosis (SM) affects mast cells, which are found in skin, connective tissue and in the lining of the stomach and intestines. Mast cells serve as a sort of alarm system by signaling disease-fighting blood cells to target areas of the body where they're needed. They may also play a role in wound healing. SM is caused by too many mast cells accumulating in the body's tissues, which can eventually affect the spleen, bone marrow, liver or small intestine.
Myeloproliferative neoplasm risk factors
Anything that increases your chance of getting myeloproliferative neoplasms is a risk factor. These include exposure to:
- Intense radiation, such as a nuclear bomb
- Petrochemicals, such as benzene or toluene
- Electrical wiring
Many people with myeloproliferative neoplasms have a mutation in the JAK2 gene.
Learn more about myeloproliferative neoplasms:
- Myeloproliferative neoplasm symptoms
- Myeloproliferative neoplasm diagnosis
- Myeloproliferative neoplasm treatment
Some cases of myeloproliferative neoplasm can be passed down from one generation to the next. Genetic counseling may be right for you. Learn more about the risk to you and your family on our genetic testing page.
Learn more about clinical trials for myeloproliferative neoplasms.
UT MD Anderson is #1 in Cancer Care
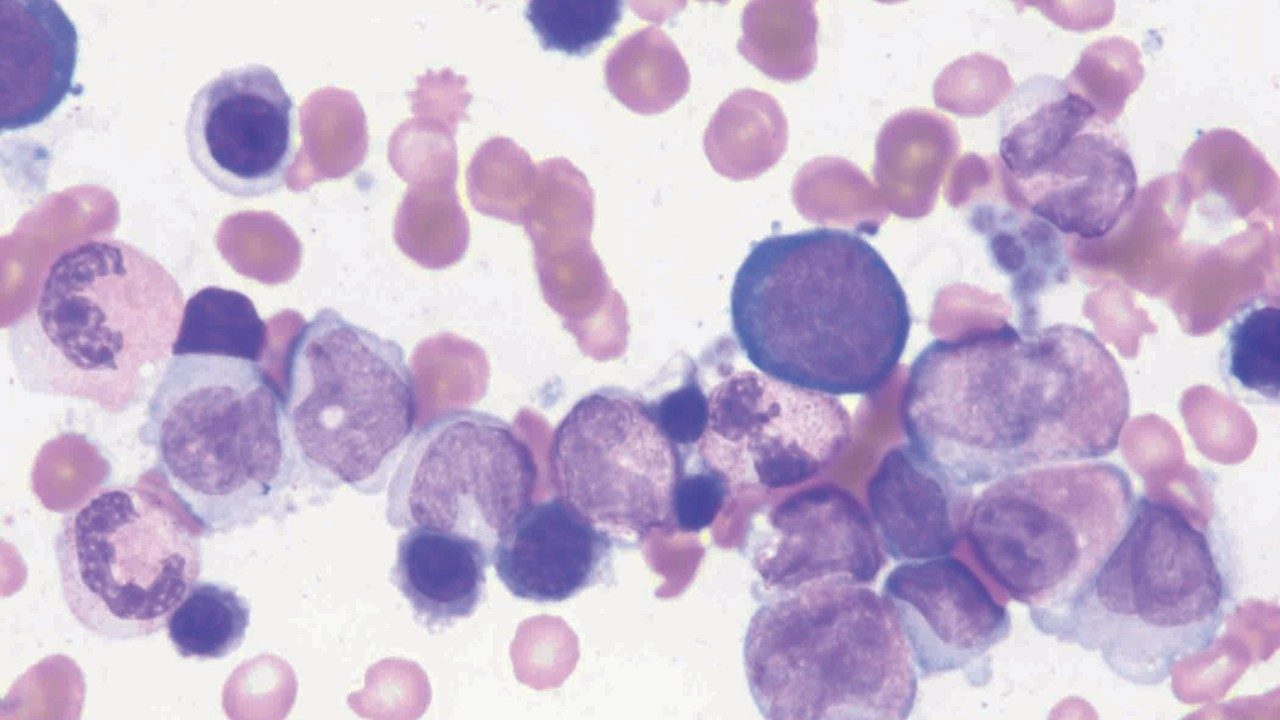
Chronic myelomonocytic leukemia (CMML): What to know about this rare cancer
Chronic myelomonocytic leukemia is a rare cancer with features that overlap both myelodysplastic syndromes and myeloproliferative neoplasms.
But what distinguishes this particular type of leukemia from others? How do its symptoms differ? And, is it curable? Read on for the answers to these questions and more.
What makes chronic myelomonocytic leukemia unique?
Chronic myelomonocytic leukemia is not a single entity. It’s more like a group of diseases. That’s why it shares features with both myelodysplastic syndrome and myeloproliferative neoplasms. All of these are chronic bone marrow disorders that affect stem cells.
Here’s how I usually explain them to my patients:
Myelodysplastic syndrome (MDS)
Genetic errors prevent stem cells from maturing properly, so they look abnormal under a microscope and patients tend to have low white blood cell counts, hemoglobin values or platelet counts.
Myeloproliferative neoplasms (MPN)
Genetic errors cause bone marrow to overproduce different types of blood cells, such as red blood cells in polycythemia vera or platelets in essential thrombocythemia. In other cases, myelofibrosis, which is scarring of the bone marrow, can develop.
Chronic myelomonocytic leukemia (CMML)
Genetic errors in stem cells can simultaneously reduce the bone marrow’s ability to produce normal levels of red blood cells or platelets, causing low blood counts, and over-produce white blood cells. In CMML, there is a significant increase in a unique type of white blood cell called monocytes. Because of these overlapping aspects, in cases where CMML shows more of the low counts without white blood cell increase, the disease is called myelodysplastic. On the other hand, if CMML causes an elevation in white blood cells, it is called myeloproliferative.
Keep in mind that chronic myelomonocytic leukemia is very rare. It is most common among the elderly, and typically occurs between ages 68 and 70. About 60% of those diagnoses occur in men.
What are the earliest signs of chronic myelomonocytic leukemia?
Chronic myelomonocytic leukemia is usually found through abnormalities in routine bloodwork. Someone might discover they have anemia during an annual physical, for instance, or their monocyte count may be consistently elevated, and that will lead to a diagnosis.
Chronic myelomonocytic leukemia is also associated with various rheumatologic disorders, including rheumatoid arthritis and lupus. These can mimic the symptoms of CMML. So, sometimes, it is found that way, when someone seeks treatment for one of those diseases.
How do the symptoms of chronic myelomonocytic leukemia differ from others?
Because CMML is not a single entity and occurs on a spectrum, how the disease looks in a particular individual depends entirely on what type of CMML a patient has. And that is determined by the type of mutations that led to the disease emerging.
Patients whose blood counts are low, for instance, might show no symptoms at all for several years, or only those associated with low blood counts, such as fatigue, anemia or bruising easily. Patients with more proliferative features, on the other hand, might have an enlarged spleen and show more “B symptoms,” such as night sweats, weight loss, fevers, or skin rashes.
Symptoms can vary greatly, depending on the person. That’s why it’s so important to see a specialist at a place like MD Anderson, which does research on this disease.
CMML is very rare. But how it’s managed can differ quite dramatically, depending on your symptoms and whether the disease is considered high-risk or low-risk. Some patients only need observation, while others need an immediate allogeneic stem cell transplant or a clinical trial using new drugs or drug combinations. The possibilities are very broad.
What are the final stages of chronic myelomonocytic leukemia?
With time, chronic myelomonocytic leukemia can potentially evolve in one of three ways.
- Bone marrow failure: This requires repeated blood transfusions and makes infections more likely. People with bone marrow failure usually die from complications of chronically low blood counts.
- Transformation into acute myeloid leukemia: Once this happens, the disease becomes more aggressive, and an allogeneic stem cell transplant should always be considered.
- Unrelated complications: These are considered a result of the disease, but not necessarily a feature of the disease. Examples include heart or kidney failure.
Unfortunately, there are no approved and effective standard treatments for any of these scenarios. That’s why seeking care in centers where clinical trials are available becomes critical. Research directed at understanding how CMML occurs and progresses continues to expand rapidly, thanks to academic centers like MD Anderson. This is helping us develop novel clinical trials.
What’s the average life expectancy for someone with chronic myelomonocytic leukemia?
That depends on the person. Everyone is different. It can range from a median of 1.5 years after diagnosis up to about 8 years. More aggressive variations of the disease will require more involved and prompt treatments. With slower-moving variations, often we can just monitor patients and treat their symptoms.
Is chronic myelomonocytic leukemia curable?
The only potentially curative treatment for chronic myelomonocytic leukemia right now is an allogeneic stem cell transplant. Although its success rate is not 100%, it is currently the best option we have and can lead to good results.
That’s why we’re exploring different treatments through clinical trials. We have several underway right now that target this disease specifically. One involves a new drug called STX-0712 that uses the immune system to kill CMML cells. Others combine decitabine or azacitidine with new drugs that affect the ways leukemia cells mature, such as seclidemstat or EP36170. Other treatments rely on new chemotherapies to kill the leukemia cells.
Because CMML is so rare and the way it behaves can vary so greatly, we are trying to approach the disease from many different angles. That’s why every patient with CMML would benefit from seeing a specialist at a facility that does research, like MD Anderson. Treatment options are already so limited for CMML that expertise is required to fully understand your disease and give you the best possible outcome.
Guillermo Montalban Bravo, M.D., is a leukemia specialist with a particular interest in chronic myelomonocytic leukemia.
Request an appointment at MD Anderson online or call 1-877-632-6789.

Understanding the types of leukemia
How many types of leukemia are there? What makes each one unique, and are they treated any differently?
We went to leukemia specialist Naveen Pemmaraju, M.D., for answers to these questions and more. Here’s what he shared.
How many different types of leukemia are there?
Quite a few. Leukemia is not just a single disease. It’s actually a diverse group of blood-based cancers that originate in the bone marrow.
All leukemias fall into one of two major categories: acute or chronic.
- Acute leukemias are blood cancers that generally appear suddenly or over a very short period of time. The classic scenario is someone who was just fine at their annual physical, but is diagnosed with leukemia a few months later.
- Chronic leukemias generally develop much more slowly, so they’re usually found in one of two ways: either a young patient is being evaluated for something else, or an older patient is having problems with recurrent infections, bleeding or abnormal lab work.
Examples of younger patients’ situations might include an athlete getting lab work done before having knee surgery, or a person having blood tests done in order to obtain a new life insurance policy. Young patients with chronic leukemia often have no symptoms, so they tend to be diagnosed unexpectedly.
Is leukemia broken down any further, beyond those two categories?
Yes. They’re further subtyped by the kind of white blood cell involved: either myeloid or lymphocyctic. The four main types of leukemia are:
- Acute myeloid leukemia (AML) is most commonly diagnosed among people in their 60s and 70s. It only affects about 21,000 people a year, but it’s among the most aggressive of all cancers. Still, there is much cause for hope. Because we can now subdivide these cancers in a way that we previously couldn’t, using molecular markers, protein receptors and other attributes. This allows us to treat them using personalized targeted therapy. And there’s been a ton of progress in this area over the last five years or so, with much of it led by our own Farhad Ravandi M.D., along with Courtney DiNardo, M.D., Tapan Kadia, M.D., Naval Daver, M.D. and Gautam Borthakur, M.D. These cancers may also be treated with chemotherapy, stem cell transplants or immunotherapy. We have a large number of clinical trials available as well.
- Acute lymphocytic leukemia (ALL) is most common among children, though adults can develop it, too. It’s a fairly rare cancer, affecting fewer than 10,000 people a year. At MD Anderson, we’ve developed highly curable regimens for this disease, under the guidance of Hagop Kantarjian, M.D. and Elias Jabbour, M.D. Some patients don’t even need a stem cell transplant to get long-term results. The type of blood cell involved (T-cell or B-cell) determines the treatment, which could be a combination of chemotherapy, immunotherapy, or targeted therapy.
- Chronic myeloid leukemia (CML) is extremely rare, with only several thousand diagnoses each year. All patients with CML will have the Philadelphia chromosome translocation, making their leukemia “Philadelphia-positive.” Historically, this has been a very deadly disease, with median survival rates of only 5 to 7 years after diagnosis. But now, with tyrosine kinase inhibitors like imatinib, dasatinib, nilotinib, ponatinib, and bosutinib, we’re seeing patients going into complete molecular remission over time. This is one area in which oral targeted therapy has really revolutionized the lives of many leukemia patients.
- Chronic lymphocytic leukemia (CLL) is one of the most common leukemias among adults. Previously, CLL patients had to be treated with intravenous chemotherapies. Today, oral targeted therapy agents, including BTK inhibitors and venetoclax, have been showing a lot of promise. And the vast majority of patients with this disease can now take oral chemotherapy as a part of their treatment regimens, instead of just IV-based drugs. Nitin Jain, M.D. and William Weirda, M.D. have been pioneering this combination-therapy approach here.
What is Philadelphia-positive leukemia?
Philadelphia-positive leukemia is characterized by the translocation of chromosomes 9 and 22. This happens when a part of chromosome 9 breaks off and attaches itself to chromosome 22, which results in the generation of abnormal cells.
Philadelphia-positive was one of the first types of leukemia to prove amenable to oral chemotherapy, and the leukemia team here at MD Anderson was the first to combine that approach with immunotherapy, which has led to some very high cure rates. Interestingly, the Philadelphia chromosome occurs in 100% of CML cases, but it’s also present to a lesser extent in AML and ALL.
What are the other types of leukemia that people should know about?
- Myelodysplastic syndrome (MDS): This used to be called “pre-leukemia,” because it could sometimes lead to leukemia. But today, doctors understand it as a unique blood cancer in and of itself. It happens when the bone marrow produces too many immature blood cells, causing a shortage of platelets, a condition known as thrombocytopenia. MDS can be life-threatening and requires its own separate approach. Guillermo Garcia-Manero, M.D. is leading our investigation in this field.
- Myeloproliferative neoplasms (MPN): This used to be called myeloproliferative disorder (MPD), but various discoveries led to a better understanding of it as a family of blood cancers in and of itself, so it was renamed. MPN is usually treated with oral chemotherapy, but our Srdan Verstovsek, M.D. is the worldwide leader in this field, and several of his clinical trials are exploring combination treatments.
- Aplastic anemia: This is a stem cell disorder caused by bone marrow failure. It is typically treated with a combination of chemo and immunotherapy. Our leader in this area, Dr. Kadia, has been conducting clinical trials that address the unique aspects of this disease.
- Blastic plasmacytoid dendritic cell neoplasm (BPDCN): This was originally thought to be a type of lymphoma, but now it’s considered its own subtype of leukemia/dendritic cell cancer. BPDCN results from an overexpression of the CD123 protein. It usually appears as a skin disorder, which is quite uncommon, but our group developed the first — and so far, only — drug to be approved by the Food and Drug Administration (FDA) to treat it: tagraxofusp-erzs.
- Hairy cell leukemia: This is a rare form of chronic leukemia that only affects about 1,000 people a year. We’ve had a lot of success in treating it with a combination of rituximab and cladribine that was pioneered here under Dr. Ravandi.
- Chronic Myelomonocytic Leukemia (CMML): This has now been recognized as it is own subtype in the MDS/MPN area, and is an emerging field of scientific breakthroughs through clinical trials, led here by Guillermo Montalban Bravo, M.D.
What’s the one thing you want people to know about leukemia treatment right now?
Some of these leukemia types are either rare or ultra-rare, but each one has developed its own field of study due to various discoveries. Many patients can live for decades now with some of these subtypes, thanks to our personalized approach to treatment. And our common goal among all of these diseases is to maximize patients’ response to treatment while also improving their quality of life.
Request an appointment at MD Anderson online or by calling 1-877-632-6789.

Acute myeloid leukemia: What to know
Acute myeloid leukemia (AML) is a cancer of the blood and bone marrow. “Acute” means that this leukemia can progress rapidly if not treated, and “myeloid” refers to the type of cell this leukemia starts from.
While AML typically occurs in adults with median age of 67, MD Anderson does treat many adolescent and young adult AML patients.
If you or a loved one has been diagnosed with AML, you have many questions. We spoke with Naveen Pemmaraju, M.D., to get answers to some common questions he hears about AML.
What is leukemia?
Leukemia is the name for a very large, complex, diverse group of malignant tumors that arise from the bone marrow and involve the blood.
Can you explain the different types of leukemia?
Leukemias are grouped by the type of cell affected and the rate of cell growth.
Acute leukemia involves an overgrowth of very immature blood cells. There are two main types of acute leukemia:
- Acute lymphocyte leukemia (ALL)
- Acute myeloid (or myelogenous) leukemia (AML)
Chronic leukemia involves an overgrowth of mature blood cells. The main types of chronic leukemia are:
- Chronic lymphoblastic leukemia (CLL)
- Chronic myeloid (or myelogenous) leukemia (CML)
We also treat many patients with other subtypes of leukemia, such as myelodysplastic syndrome (MDS), myeloproliferative neoplasms (MPN), aplastic anemia, blastic plasmacytoid dendritic cell neoplasm (BPDCN) and hairy cell leukemia.
What are the symptoms of AML?
There is generally a wide range of symptoms and presentations. Some patients may not have many symptoms and may only be diagnosed through blood testing when presenting in the clinic, through the emergency room, or in the hospital.
Others may experience common symptoms, such as fatigue, fevers/infections, bleeding and easy bruising. Some patients may be so ill that they present directly through the emergency room to the intensive care unit.
Are some people more likely to develop AML?
The exact cause of AML is unknown. Some associations/risk factors include:
- Exposure to ionizing radiation or specific chemical exposure
- Certain genetic/familial syndromes, such as familial platelet disorders with propensity to myeloid malignancies or inherited bone marrow failure syndromes
- Prior cancer treatment with either radiation or chemotherapy
- Patients with antecedent hematologic malignancy, such as MDS, MPN, aplastic anemia, BPDCN
How is AML typically treated?
Unfortunately, there’s not yet a reliable, standard therapy for most patients with AML. Many patients undergo chemotherapy and/or a stem cell transplant, which is a procedure that replaces defective or damaged cells in patients whose normal blood cells have been affected by cancer.
But stem cell transplants often aren’t an option for patients older than age 70, and some of the most common intensive chemotherapy regimens used for patients at younger ages may not work for all older patients. Often the best options may include a clinical trial.
What clinical trials is MD Anderson offering for older AML patients?
At MD Anderson, we have a number of different AML clinical trials, some of which are part of our MDS/AML Moon Shot. Some of the frontline AML clinical trials we have for older patients include:
- A hypomethylator agent (such as Azacytidine, Decitabine or SGI-110) alone or with another agent
- Novel clinical trial drugs alone or in combinations, including targeted therapies based on a particular patient’s mutational profile (FLT3, IDH 1 or 2, or CD123, for example)
- Immunotherapy agents or immunotherapy in combination with chemotherapy
What other new research is on the horizon for AML?
Besides the clinical trials I just mentioned, we’ll soon be looking at targeted therapy agents aimed at a particular molecular mutation or aberrant molecular pathways
Other approaches will soon include newer forms of immunotherapy, such as chimeric antigen receptor (CAR) T-cell therapy, bi-specific antibody therapies and others via upcoming clinical trials.
Why are patients with acute leukemia at increased risk of infection?
If the white blood cell count, specifically the neutrophil count, is very low, this can weaken the immune system’s functioning and make it harder for a patient to fight off infections.
This can happen because of the leukemia itself or as a result of the cancer treatment. Generally, patients in active therapy may be placed on preventive antibiotics to help protect against some of the more common infections.
What’s your advice for newly diagnosed AML patients?
Every patient is unique and each patient should have a serious conversation with their oncologist when diagnosed with AML. It’s important that you receive treatment from someone with a lot of experience treating AML and who has access to the latest clinical trials. I encourage new AML patients to schedule an appointment with an experienced hematologist at a comprehensive cancer center such as MD Anderson.
I also recommend finding out about your clinical trial options upfront, whether you have a new AML diagnosis or you have relapsed AML.
Why come to UT MD Anderson for your myeloproliferative neoplasm treatment?
As one of the world's largest programs devoted to blood diseases, UT MD Anderson's Leukemia Center sees many more patients with a myeloproliferative neoplasm (MPN) than other programs or doctors.
While most oncologists see only a few patients with a myeloproliferative neoplasm in their careers, we see hundreds every month. This translates into a remarkable depth of experience and expertise, which we draw upon to give you personalized treatment.
Myeloproliferative neoplasms, or myeloproliferative disorders, can be challenging to diagnose and treat, often requiring years of follow-up care and treatment. At UT MD Anderson, a team of experts, which may include hematologists, pathologists, advanced practice nurses and physician's assistants, as well as a specially trained support staff, plans your treatment for myeloproliferative disease by drawing upon the very latest advancements and therapies. It all begins with precise diagnosis by our specialized pathologists, who use advanced technology and skill to pinpoint the exact disorder.
Innovation and research
At UT MD Anderson's Leukemia Center, you benefit from the most active research program in the United States. We have helped pioneer many advancements in MPN treatment, and we offer a wide range of clinical trials (research studies) on innovative treatments. The Leukemia department has established the Hanns A. Pielenz Clinical Research Center for Myeloproliferative Neoplasms, which has become the largest center in the world for MPN patient referral and research. This center leads the clinical development of novel, effective MPN medications and pursues a comprehensive approach to understanding the biology of MPN through translational research studies.
Somehow, some way, you'll get through this. And no matter the outcome, you'll be grateful for the gift of time.
Judy Overton
Caregiver
Treatment at UT MD Anderson
Myeloproliferative neoplasms are treated in our Leukemia Center.
Clinical Trials
UT MD Anderson patients have access to clinical trials offering promising new treatments that cannot be found anywhere else.
Becoming Our Patient
Get information on patient appointments, insurance and billing, and directions to and around UT MD Anderson.
myCancerConnection
Talk to someone who shares your cancer diagnosis and be matched with a survivor.
Prevention & Screening
Many cancers can be prevented with lifestyle changes and regular screening.
Counseling
UT MD Anderson has licensed social workers to help patients and their loved ones cope with cancer.
Help #EndCancer
Give Now
Donate Blood
Our patients depend on blood and platelet donations.
Shop UT MD Anderson
Show your support for our mission through branded merchandise.