request an appointment online.
- Diagnosis & Treatment
- Cancer Types
- Eye Cancer
Get details about our clinical trials that are currently enrolling patients.
View Clinical TrialsMore than two dozen types of cancer can develop in the different structures in and around the eye. Among these are subtypes of melanoma, lymphoma, sarcoma and carcinoma.
More than two dozen types of cancer can develop in the different structures in and around the eye. Among these are subtypes of melanoma, lymphoma, sarcoma and carcinoma.
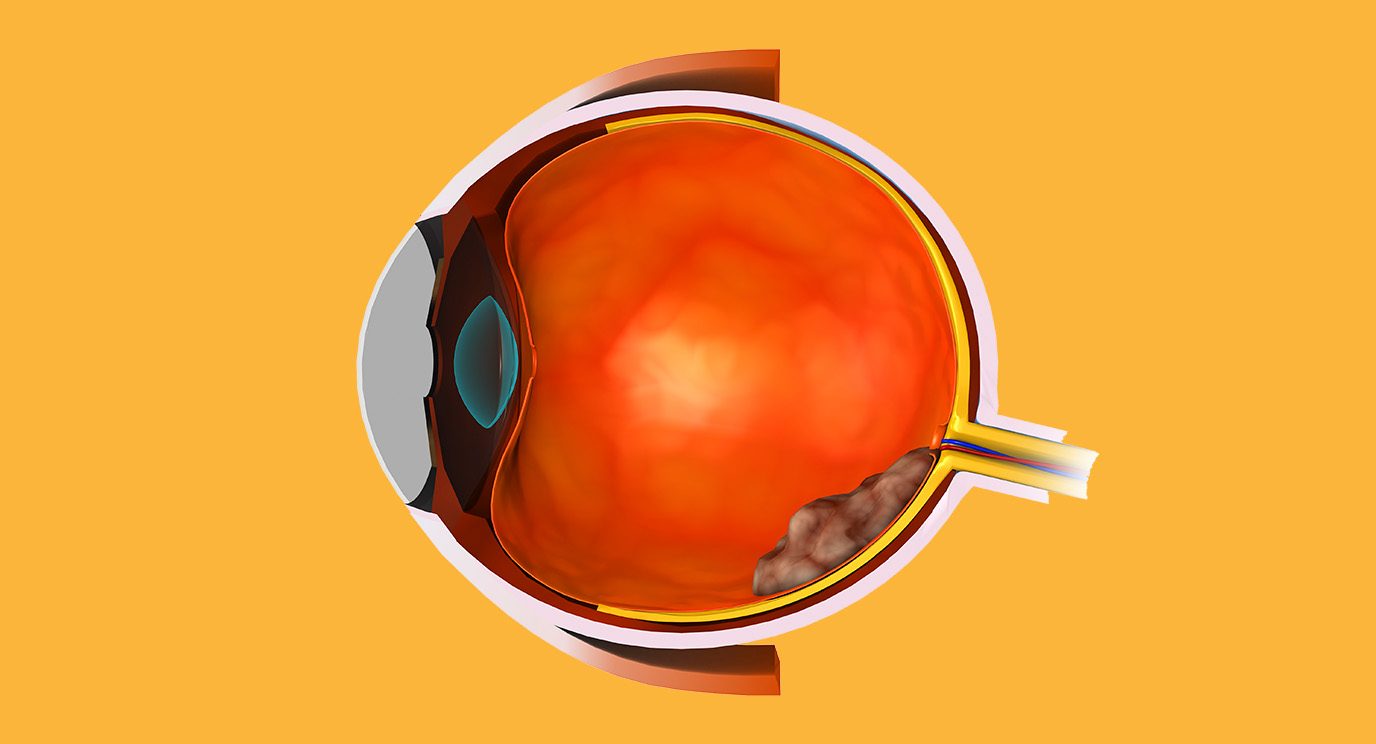
The structures that make up the eye and its surrounding area include:
Eyeball: The structures inside the eye where cancer can develop include the uvea (made up of the choroid, ciliary body and iris), retina and vitreous.
Uvea: The middle layer of the eyeball. It contains the following:
- Iris: The colored part of the eye. The pupil, a small opening that lets light come into the eyeball, is in the middle of the iris.
- Choroid: Thin layer around the eyeball that provides the eye with nutrients
- Ciliary body: A structure made of muscles inside the eye that help it focus and cells where aqueous humor (clear liquid in front of eye) is formed
Vitreous: The gel-like fluid that fills the eyeball.
Retina: A layer of cells in the back of the eye that is connected by the optic nerve to the brain. These cells are sensitive to light and help us see images. When light comes into the eye, it passes through the lens. This makes an image on the retina, which is then sent by the optic nerve to the brain.
Orbit: This space around and behind the eye has bony walls and contains important nerves, including the optic nerve, the lacrimal gland and muscles that move the eye.
Lacrimal gland: This gland makes tears and is located is in the upper outer quadrant of the orbit.
Eyelid: Tumors that affect eyelids can be on the skin of the eyelid or on the inside layer of the eyelid (tarsus and conjunctiva).
Conjunctiva: Surface covering of the eye that also covers the inside of the eyelid
Lacrimal sac/duct: This structure, which drains the tears, is in the inner lower quadrant of the orbit near the nose.
Types of eye cancer
Cancers inside the eyeball
Uveal melanoma: Also called choroidal melanoma, this is the most common primary intraocular eye cancer in adults. It accounts for about 5% of all melanoma cases. The uvea is behind the sclera (the white of the eye) and the cornea (the window at the front of the eye). It has three parts: the iris (the colored part of the eye); the ciliary body (a ring of tissue with muscle fibers that change the size of the pupil and the shape of the lens); and the choroid, also known as the posterior uvea (the back part of the eye under the retina). Learn more about uveal melanoma.
Retinoblastoma: Retinoblastoma is a cancer of the retina, a light-sensitive layer of tissue in the eye. Among children, it is the most common malignant tumor that starts in eye. It usually occurs before age five, and most of these cases occur in children under two. Visit our retinoblastoma disease page to learn more.
Circumscribed choroidal hemangioma: This is a non-cancerous growth that poses no risk to the patient’s life. It is often discovered during routine eye exams. If it is not impacting the patient’s vision, doctors often recommend the growth be monitored instead of treated. If vision is affected, treatment usually includes laser therapy and occasionally radiation.
Retinal hemangioblastoma: Retinal hemangioblastoma is a non-cancerous tumor of the retina. It is often the first symptom of von Hippel Lindau disease, a hereditary cancer syndrome that causes tumor formation in multiple parts of the body. The tumor sometimes has no symptoms. Other times it causes blurry vision, flashing lights and floaters. If not caught early, it can lead to vision loss, blindness or loss of the eye. Retinal hemangioblastoma can be treated with laser therapy or cryoablation. It is sometimes also treated with surgery or radiation therapy.
Metastatic intraocular tumors: Many cancers can metastasize, or spread, to the eyeball. The most common are breast, lung and gastrointestinal cancers. Patients with metastatic tumors receive personalized care that may include chemotherapy, targeted therapy, radiation therapy and laser therapy.
Cancers of the eyelid
Basal cell carcinoma: More than 90% of eyelid cancers are basal cell carcinomas, a type of skin cancer. The lower eyelids are involved in more than 70% of cases, followed by the inner corner of the eye, upper eyelid and the outside corner of the eye. This cancer is usually not aggressive and does not spread to lymph nodes or distant organs.
The disease is treated with surgery to remove the tumor. The eyelid tissue will also be reconstructed to preserve the patient’s vision, maintain comfort and restore the eye’s appearance. In advanced cases, targeted therapy and adjuvant radiation therapy may be appropriate.
Squamous cell carcinoma: This is also a type of skin cancer, though it occurs less often on the eyelid than basal cell carcinoma, but it is more aggressive. It can spread to nearby lymph nodes and other parts of the body.
The main treatment for this type of eye cancer is surgical removal. Radiation therapy or other treatments may be used in addition to surgery if a large area is affected or if the tumor cannot be fully removed.
Cutaneous melanoma: This type of skin cancer accounts for about 1% of eyelid cancers. It is potentially life-threatening. It can affect the eyelid skin or the conjunctiva.
Melanomas of the eyelid are surgically removed. The eyelid is then reconstructed in a separate procedure, usually done the next day. If the patient has a high-risk tumor, doctors may perform a lymph node biopsy to see if the cancer has spread. A sentinel lymph node biopsy can find microscopic signs of metastasis, which can help doctors diagnose and treat metastatic melanomas in the early stages.
Sebaceous carcinoma (meibomian gland carcinoma): This rare type of eyelid carcinoma is also known as sebaceous gland or sebaceous cell carcinoma. It affects the meibomian glands of the eyelids, as well as of the conjunctiva or other surface structures of the eye. These glands produce the oily layer of liquid that covers the eye.
Sebaceous carcinoma of the eyelid can be mistaken for non-cancerous conditions like a chalazion, a small cyst known as a sty. If a sty does not heal with medical treatment or surgical drainage, doctors should perform a biopsy on the growth.
Sebaceous cancer in the eyelid is surgically removed, and the eyelid is reconstructed. Sometimes patients are given topical chemotherapy in the form of eye drops to use after the surgical area has healed.
Sebaceous carcinoma can spread to the regional lymph nodes. In these cases, patients can be treated with radiation therapy. For larger sebaceous carcinomas, doctors can perform a sentinel lymph node biopsy to look for microscopic signs of the disease’s spread.
Merkel cell carcinoma: This rare but aggressive cancer usually shows up as a fast-growing purplish or flesh-colored mass. Treatment for this cancer typically starts with surgery to remove the mass and reconstruct the eyelid. Radiation therapy can also be used after surgery in some cases. Because of toxicity issues, radiation is typically used only on lower eyelid tumors. Doctors may perform a sentinel lymph node biopsy to determine if the cancer has spread to nearby lymph nodes.
Metastatic eyelid tumors: Many cancers can metastasize, or spread, to the eyelid. Patients with metastatic tumors receive personalized care that may include chemotherapy, targeted therapy, radiation therapy and laser therapy.
Cancers of the conjunctiva
Squamous cell carcinoma: This is the most common type of conjunctival eye cancer. It can affect the area around the cornea on the eye surface or the inner conjunctival layer of the eyelids. It has a very low risk of spreading to the lymph nodes.
This eye cancer is most often treated with surgery, and the eye is typically preserved. At the time of surgery, doctors usually perform cryoablation (freezing treatment) along the edges of the surgical area. Topical chemotherapy in the form of eyedrops is also a treatment. This may be offered instead of surgery or prescribed after surgery.
If this cancer returns in an aggressive form, the eye and eye socket may have to be removed.
Conjunctival Melanoma: Melanoma can occur on the conjunctiva on the surface of the eyeball (bulbar conjunctiva) or on the conjunctival covering of the inside of the eyelid (palpebral conjunctiva). Conjunctival melanomas can spread to the lymph nodes and other parts of the body. This risk is higher for thicker melanomas.
Conjunctival melanoma is treated with surgery combined with cryotherapy along the surgery’s edges. At the time of surgery, doctors may perform a sentinel lymph node biopsy to look for signs of early metastasis. Doctors use this procedure to determine the cancer’s stage and plan additional treatments. Sometimes doctors use chemotherapy eye drops after surgery to reduce the chance of recurrence.
Metastatic conjunctival tumors: Many cancers can metastasize, or spread, to the conjuctiva. Patients with metastatic tumors receive personalized care that may include chemotherapy, targeted therapy, radiation therapy and laser therapy.
Cancers of the orbit
Orbital sarcoma: Sarcomas arise from muscles or fatty tissue. The most common sarcoma in the orbit is rhabdomyosarcoma, which is found most frequently in children.
The most common type of orbital rhabdomyosarcoma can be treated with a combination of chemotherapy and proton therapy. This combination can prevent the removal of the eye and orbital content in the majority of patients.
Orbital and optic nerve meningiomas: These tumors are benign, meaning they are not cancerous and do not spread. They can be associated with other syndromes, including neurofibromatosis. They can be associated with the optic nerve. They can also form in the meninges (membranes that line the skull and enclose the brain and top of the spinal cord) in the base of the skull and extend into the orbit. The symptoms of these tumors may include a gradual loss of vision or visual field.
These tumors are usually diagnosed with an imaging exam, such as an MRI of the orbit. Surgical biopsies usually are not necessary and are avoided if possible to minimize risk of visual loss. Treatment usually includes radiation therapy, particularly proton therapy through the Proton Therapy Center.
Metastatic orbital tumors: Many cancers can metastasize, or spread, to the orbit. Patients with metastatic tumors receive personalized care that may include chemotherapy, targeted therapy, radiation therapy and laser therapy.
Lacrimal gland tumors
Adenoid cystic carcinoma: This rare cancer has the potential to spread and become life-threatening. For smaller or less aggressive tumors, eye-preserving surgery followed by proton therapy, offered through the Proton Therapy Center. may be used. When the disease is more advanced or aggressive, the eye and surrounding soft tissue may need to be removed.
Pleomorphic adenoma: This is the most common benign (non-cancerous) tumor of the lacrimal gland. It is diagnosis based on clinical signs and imaging studies. The entire tumor should be surgically removed. The eye should always be spared in these procedures.
Other lacrimal gland carcinomas: Other forms of carcinoma include adenocarcinoma or squamous carcinoma or mucoepidermoid carcinoma of lacrimal gland. They are managed similarly to adenoid cystic carcinoma.
Metastatic lacrimal gland tumors: Many cancers can metastasize, or spread, to the lacrimal gland. Patients with metastatic tumors receive personalized care that may include chemotherapy, targeted therapy, radiation therapy and laser therapy.
Lacrimal sac and nasolacrimal duct cancers
Squamous cell carcinoma: As with squamous cell carcinomas in other locations, surgery is the main treatment. Radiation therapy, specifically proton therapy, is used after surgery to decrease the likelihood of recurrence. Usually it is to preserve the eye, though in some cases it may have to be removed, depending on the extent of disease.
Transitional cell carcinoma: This is a cancer of the lacrimal sac. Symptoms may include excessive tearing, bloody tears, frequent nosebleeds or a mass in the inner bottom corner of the orbit. Treatment for transitional cell carcinoma of the lacrimal sac includes surgery, followed by radiation therapy or proton therapy.
Metastatic lacrimal sac and nasolacrimal duct tumors: Many cancers can metastasize, or spread, to the lacrimal sac and nasolacrimal duct. Patients with metastatic tumors receive personalized care that may include chemotherapy, targeted therapy, radiation therapy and laser therapy.
Lymphomas of the eye
Lymphoma is a cancer of the white blood cells, which are part of the immune system. It can affect many parts of the eye and surrounding structures, including:
- the vitreous
- the choroid
- the conjunctiva
- the adnexa, or structures surrounding the eyeball, such as muscles, eyelids and tear glands.
There are several types of lymphoma that affect the eye, including:
Diffuse large B-cell lymphoma: Diffuse large B-cell lymphoma (DLBCL) is an aggressive (fast growing) non-Hodgkin lymphoma. It is the most common type of lymphoma affecting the vitreous and can also involve the orbit.
Symptoms of DLBCL in the vitreous include painless floaters, or dark spots in the field of vision.
If a biopsy of any part of the eye shows DLBCL, patients should undergo additional testing to rule out the presence of lymphoma outside the eye, especially in the brain. Treatment depends on the locations of the lymphoma and requires a multidisciplinary evaluation in a specialized center. Treatment often includes a combination of immunotherapy and chemotherapy, as well as radiation therapy.
Marginal zone lymphoma and follicular lymphoma: Marginal zone lymphoma and follicular lymphoma are both indolent (slow growing) non-Hodgkin lymphomas.
Marginal zone lymphoma can involve the conjunctiva and often causes a salmon-colored or light orange growth on the surface of the eye. It can also develop in the adnexa or the choroid. Follicular lymphoma can involve the adnexa.
Marginal zone lymphoma and follicular lymphoma may show up as a nodule in the eyelid or around the eye. They can also develop in the lacrimal gland and the orbit. Symptoms may include a bulging eye. These types of cancer usually do not cause pain.
If a biopsy of any part of the eye shows marginal zone lymphoma or follicular lymphoma, patients should undergo additional testing to rule out the presence of lymphoma outside the eye. Marginal zone lymphoma and follicular lymphoma usually do not affect the brain.
Treatment for these cancers depends on the locations of the lymphoma and requires multidisciplinary evaluation in a specialized center. Treatment options include immunotherapy, a combination of immunotherapy and chemotherapy, and radiation therapy. In some cases, doctors may recommend active surveillance instead of treatment. This approach is used for some slow-growing cancers. It involves closely monitoring the disease and only beginning treatment if it progresses.
What are eye cancer's risk factors?
A risk factor is anything that increases your chance of getting a specific disease. Risk factors for cancers of the eye include:
- Having light skin and/or blue eyes
- Exposure to sun or tanning salons may increase risk of carcinomas or melanomas on your eyelid.
- Nevus of Ota: A large birthmark associated with a high number of melanocytes. This condition causes dark patches to form on the skin or in the eyes.
- Exposure to certain viruses such as human papilloma virus (HPV) may increase the risk of squamous cell carcinoma of conjunctiva.
- Atypical mole and melanoma syndrome (AMS): Previously known as dysplastic nevus syndrome, AMS is characterized by large numbers of atypical moles.
- Certain genetic conditions can increase the risk of developing specific eye cancers, including Von Hippel Lindau disease and mutations to the RB1 and BAP-1 genes, which help suppress tumor formation. Learn more about hereditary cancer syndromes.
Patients with these risk factors may benefit from cancer screenings by an ophthalmologist trained in diagnosing cancer.
Not everyone with these risk factors gets ocular cancers. However, if you have risk factors and eye cancer symptoms, it’s a good idea to discuss them with your health care provider.
Learn more about eye cancer:
Why come to UT MD Anderson for your eye cancer treatment?
Eye cancer is a rare disease. It’s important to get care from doctors who have experience treating this disease. UT MD Anderson’s uveal melanoma program is amongst the oldest eye cancer programs in the in the nation and one of the only based entirely in a dedicated cancer hospital.
At UT MD Anderson's Ophthalmology Clinic, you’ll be treated by highly skilled and renowned experts. They have helped conduct some of the most important studies of different eye cancers and have served as leaders of international healthcare organizations, including the American Society of Clinical Oncology, the International Society of Ocular Oncology, the American Association of Ophthalmic Oncologists and Pathologists and the American Society of Ophthalmic Plastic & Reconstructive Surgery.
These physicians tailor your eye cancer care specifically for you. They work together in teams, collaborating at every step, to be sure you receive the most advanced therapies while making every effort to preserve ocular function and vision.
Most cancers affecting the eye and orbital area are rare and require treatment at centers familiar with the best treatment and diagnosis options. Our ophthalmologists have special training in surgical and medical treatment of all cancers of the eye and eye area. They work closely with radiation oncologists, medical oncologists, pathologists and plastic surgeons, all trained to treat eye cancer, to deliver the best outcomes.
Advanced treatments and clinical trials
UT MD Anderson's ophthalmologists customize your treatment to include the latest technology and methods to treat eye cancer, which may include:
- Surgery
- Radiation therapy, including proton therapy
- Targeted therapies
- Immunotherapy
- Ophthalmic reconstructive procedures to preserve function and appearance in the eye and facial area
- Clinical trials of new treatments that may not be offered anywhere else
If surgery is needed, it is performed by some of the nation’s top ophthalmic surgeons and highly specialized eye reconstructive surgeons.
And we are constantly researching new ways to diagnose and treat eye cancer. This means we are able to offer clinical trials of new therapies, including targeted therapy, immunotherapy and new chemotherapy treatments.
And at UT MD Anderson, you're surrounded by the strength of the nation's largest and most experienced comprehensive cancer center. From physical therapy to support groups to integrative medicine, we have all services needed to treat the whole person — not just the eye.
At UT MD Anderson, I landed exactly where I needed to be. I have no doubt that I received the best, most comprehensive care available.
Eileen Brzoska
Survivor
Treatment at UT MD Anderson
Cancers of the eye are treated in our Ophthalmology Clinic in the Head and Neck Center.
Clinical Trials
UT MD Anderson patients have access to clinical trials offering promising new treatments that cannot be found anywhere else.
Becoming Our Patient
Get information on patient appointments, insurance and billing, and directions to and around UT MD Anderson.
myCancerConnection
Talk to someone who shares your cancer diagnosis and be matched with a survivor.
Prevention & Screening
Many cancers can be prevented with lifestyle changes and regular screening.
Counseling
UT MD Anderson has licensed social workers to help patients and their loved ones cope with cancer.
Help #EndCancer
Give Now
Donate Blood
Our patients depend on blood and platelet donations.
Shop UT MD Anderson
Show your support for our mission through branded merchandise.