request an appointment online.
- Diagnosis & Treatment
- Cancer Types
- Bile Duct Cancer
Get details about our clinical trials that are currently enrolling patients.
View Clinical TrialsBiliary cancers (also called cholangiocarcinoma or bile duct cancers) are relatively uncommon in the United States. Different types of biliary cancer are named after where the cancer forms. Intrahepatic bile duct cancer starts in the bile ducts inside the liver. Extrahepatic bile duct cancer starts in the bile ducts outside the liver. Gallbladder cancer begins in the walls of the gallbladder.
Biliary cancers (also called cholangiocarcinoma or bile duct cancers) are relatively uncommon in the United States. Different types of biliary cancer are named after where the cancer forms. Intrahepatic bile duct cancer starts in the bile ducts inside the liver. Extrahepatic bile duct cancer starts in the bile ducts outside the liver. Gallbladder cancer begins in the walls of the gallbladder.
Bile duct structure and function
The biliary system produces a fluid called bile, which helps digest food. Bile is made in the liver and stored in the gallbladder. The bile ducts are tree-like structures within and around the liver and gallbladder. They carry bile from the liver to the upper part of the small intestine (duodenum).
Biliary cancer types
Intrahepatic bile duct cancer: Intrahepatic bile duct cancer, or intrahepatic cholangiocarcinoma, occurs in the bile ducts within the liver. It accounts for about 10% of bile duct cancer cases. It is often misdiagnosed as liver cancer. Although rare, the number of intrahepatic bile duct cancer cases is increasing.
Extrahepatic bile duct cancers: Extrahepatic bile duct cancers occur in bile ducts outside the liver. There are two types of extrahepatic bile duct cancer:
- Perihilar bile duct cancer: This is the most common type of extrahepatic bile duct cancer. It accounts for 40 to 60% of all bile duct cancer cases. The disease occurs where the bile ducts exit the liver. It is sometimes called perihilar cholangiocarcinoma or a Klatskin tumor.
- Distal bile duct cancer: This disease starts in the part of the bile ducts that passes through the pancreas and connects with the small intestine. It makes up 20 to 40% of bile duct cancer cases.
Gallbladder cancer: A cancer that arises in the wall of the gallbladder. Gallbladder cancer is often found when looking for or doing surgery to remove gallstones.
Bile duct & gallbladder cancer risk factors
Anything that increases your chance of getting biliary cancer is a risk factor. Bile duct and gallbladder cancer risk factors include:
Age: Most cases of biliary cancer in the United States are diagnosed in people between the ages of 50 and 70.
Ethnicity: In the U.S., Native Americans are more likely to get biliary cancers.
Medical conditions: Having any of the following may increase your risk for biliary cancer:
- Primary sclerosing cholangitis (PSC): A progressive autoimmune disease which scars the bile ducts over time.
- Chronic liver diseases, including:
- Cirrhosis
- Bile duct stones
- Cholangitis
- Non-viral chronic liver disease
- Polycystic liver disease
- Hepatitis B or hepatitis C infection
- Inflammatory bowel diseases, including:
- Crohn’s disease
- Ulcerative colitis
- A history of bile duct cysts (choledochal) which are prone to chronic inflammation.
- Liver fluke infection: Liver flukes are parasites that are more common in South and Southeast Asia. Infection may arise due to the consumption of raw or undercooked fish.
- Exposure to thorotrast, a medical contrast agent that is no longer in use.
Smoking: Smoking increases the risk of many cancers, including bile duct cancer.
Excessive consumption of alcohol: Excessive consumption of alcohol likely increases the risk of biliary cancer. This is especially true for people who have alcohol-associated liver damage.
Family history: Several genetic disorders, including Lynch syndrome, may increase the risk of biliary tract cancers.
Learn more about bile duct cancer:
Learn more about clinical trials for bile duct cancer.
UT MD Anderson is #1 in Cancer Care
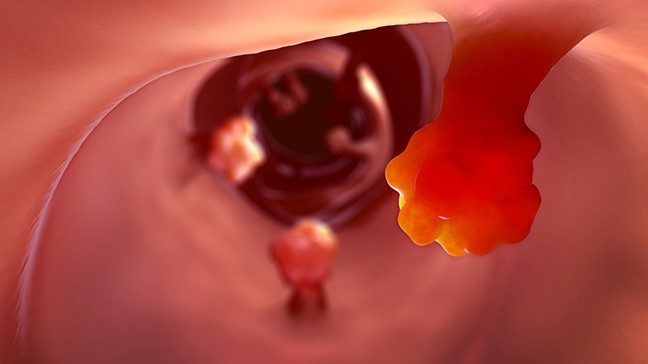
What are polyps?
You may already have heard about colon polyps. These abnormal cell growths are more likely to develop as we age. They occur in the colon and are removed during colonoscopies. The most common type resembles broccoli, with a stalk and a bulbous growth at the end.
But can polyps form anywhere else? What causes them? And, are polyps cancerous?
Read on to learn the answers to these questions and more.
Where can polyps appear in the body?
Polyps can form in any organ that has a hollow space where they can grow. This means polyps may develop virtually anywhere along your gastrointestinal, urinary or respiratory tracts, as well as in the female reproductive organs. This includes the:
- esophagus
- stomach
- gallbladder
- small intestine
- colon
- nasal cavity
- trachea (windpipe)
- vocal cords
- lungs
- kidneys
- ureters
- bladder
- urethra
- fallopian tubes
- uterus
- cervix
- vagina
Polyps can’t form in the liver because that organ is not hollow and its tissue is too dense. But the gallbladder has room, despite being filled with bile.
What causes polyps?
A polyp is an abnormal cluster of cells that multiplies and heaps up on itself in response to some kind of stimulus. That stimulus could be either environmental or genetic.
If the source is environmental, it’s usually connected to inflammation. Nasal polyps, for instance, often develop due to chronic irritation, whether that’s because of allergies or repeated exposure to inhaled chemicals.
If the source is genetic, though, it could be due to an inherited condition, including:
- Lynch syndrome
- Familial adenomatous polyposis
- MUTYH-associated polyposis
- Peutz-Jeghers syndrome
But mutations in many genes can cause or fail to suppress polyp formation. So, polyps aren’t always related to one of these disorders.
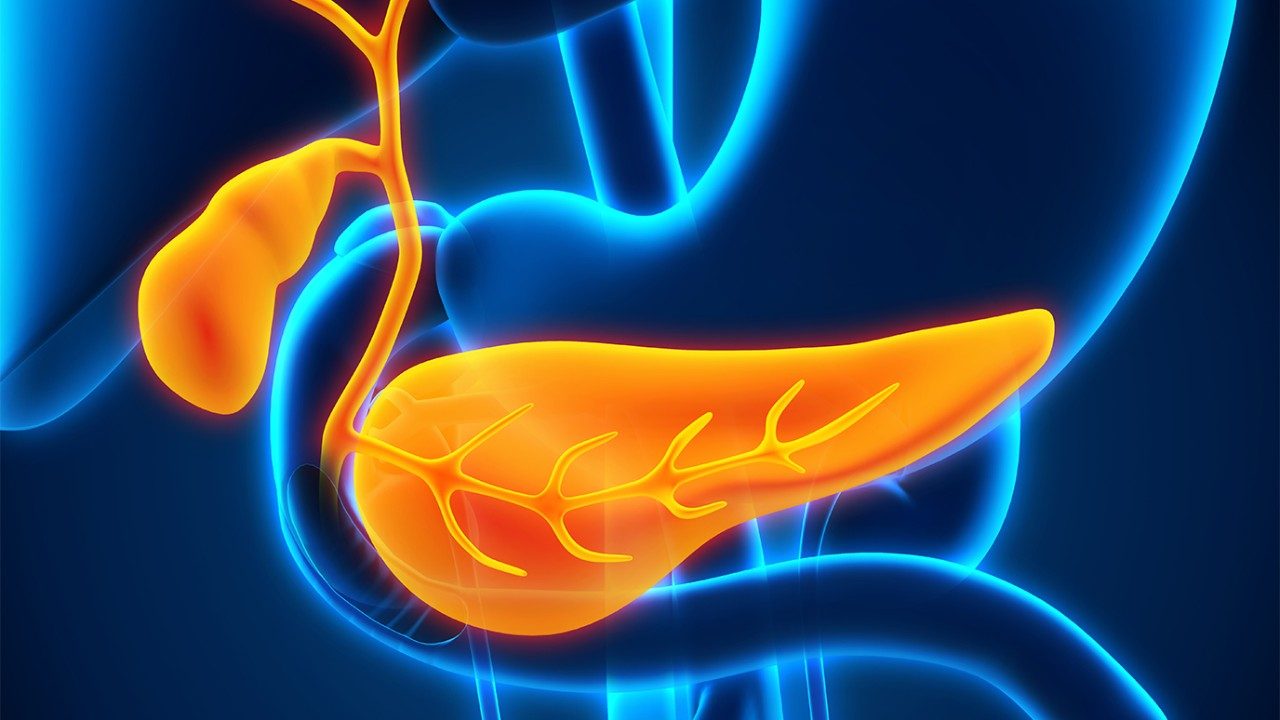
Pancreatic cysts: What they are and how they’re treated
The pancreas is part of the digestive system which helps your body regulate blood sugar and digest food. Sometimes cysts can develop inside the pancreas. These small, fluid-filled sacs usually don’t cause any symptoms, and most people don’t even realize they have them.
“About 10% to 20% of people over the age of 60 have pancreas cysts,” says surgical oncologist Michael Kim, M.D. Most of these are benign and will never cause problems.
But if you have pancreas cysts, you are more likely to develop pancreatic cancer.
Symptoms of pancreatic cysts
Although most cysts don’t cause symptoms, there are some signs to watch for. These include nausea, vomiting, abdominal bloating and pain in the abdomen.
“If you experience any of these symptoms without relief for more than two weeks, you should talk to your doctor,” Kim says.
How a pancreas cyst diagnosis is made
Most of the time, pancreatic cysts are found during medical treatment for other conditions. “You may experience back pain and go to the emergency room,” Kim says. “Or, if you get a CT scan after an injury, your care team may find cysts that way,” he adds.
If you have pancreatic cysts, your care team will also look at the size of the cyst. “Cysts smaller than 2 centimeters usually don’t require treatment, unless they’re causing pain or other symptoms,” Kim says.
Your care team will also look to see if you have any of the following:
Dilation of the main duct of the pancreas
Nodules inside the cyst
Enhancement of the cyst walls during an IV contrast test
Your care team will likely perform a biopsy to learn about features and the type of cyst if you have any of these risk factors.
Looking for a genetic link to pancreatic cysts
After a biopsy, fluid from inside the cyst may be sent for genetic sequencing.
There are two main genes associated with cysts in the pancreas: KRAS and GNAS. Kim says other genes associated with higher cancer risk, like BRCA mutations, can also play a role in cyst development.
“We’re not sure why some people have cysts that develop into cancer and some don’t,” Kim says. That’s why he and his team are working to better understand the genetic link between pancreatic cysts and cancer.
Types of pancreatic cysts
There are several types of pancreatic cysts. Some are more likely to develop into cancer than others.
- Intraductal Papillary Mucinous Neoplasms (IPMNs) are the most common type of cyst found in the pancreas. These are also divided into different categories depending on where they’re found within the system of ducts that helps the pancreas secrete digestive enzymes.
- Main duct IPMNs are the most likely to become cancerous and are found in the main duct to the pancreas.
- Side branch IPMNs are most common and are found in the branches off the main duct.
- Mixed IPMNs can be found in both the side branches and the main duct.
- Mucinous cystic neoplasms tend to develop in younger healthy women. These typically develop inside the pancreas, not in the ducts.
- Solid pseudo papillary neoplasms may look like cysts, but they’re solid masses made up of cells.
- Serous cystadenomas are benign but can sometimes become quite large and need to be removed.
- Pseudo cysts are benign and caused by inflammatory responses in the pancreas. These generally don’t cause problems unless they’re very large and cause symptoms.
Pancreatic cyst treatment options
For most pancreatic cysts, surveillance is a good option. “We can watch cysts through routine scans for a long time,” Kim says.
Cysts that are cancerous or pre-cancerous are most commonly treated with surgery, depending on the patient’s age and risk factors. “We can take out the cyst, as well as the part of the pancreas where it was found, to reduce the risk of cancer growing or spreading,” Kim says.
The exact type of surgery will depend on the cyst’s location.
If the cyst is located in the head of the pancreas, patients will undergo a type of surgery called the Whipple procedure.
A procedure called a distal pancreatectomy is used to remove cysts located in other parts of the pancreas. Talk to your care team about which treatment is right for you.
“It’s important to seek care at a center like MD Anderson that has specialized expertise in diagnosing and treating pancreatic cysts,” Kim says.
New research focuses on pancreatic cyst prevention and growth
Kim and his colleagues, including Florencia McAllister, M.D., are working on designing a clinical trial to detect precancerous cysts or to develop vaccines to prevent pancreatic cyst growth or progression.
“If we can get the immune system to attack antigens on the surface of problematic cysts, we could potentially keep them from growing, or get rid of them altogether,” Kim says.
Kim credits the volume of patients MD Anderson sees with the ability to build upon clinical trial data. “We're in a position where we can make our guidelines for informing our practices, based on the results we’ve seen so far,” he says.
Request an appointment at MD Anderson online or by calling 1-877-632-6789.
Why choose UT MD Anderson for biliary cancer treatment?
UT MD Anderson's Gastrointestinal Center treats biliary cancer patients as individuals, not statistics.
UT MD Anderson is working to improve survival rates for biliary cancer through innovative treatments like targeted therapies, new surgical techniques and high-dose radiation therapy. Our team of experts meets weekly to review patient cases and treatment plans.
Not only do we offer the most cutting-edge treatments and techniques—we pioneer them. UT MD Anderson has developed new interventional radiology, chemotherapy and targeted therapy treatments.
We also offer innovative clinical trials. These include new treatment combinations and therapies that target mutations that drive biliary cancer.
As an UT MD Anderson patient, you will receive world-class expertise at every step of your cancer journey. Our teams also provide supportive care and management for bile duct cancer side effects like bile duct obstruction, malnutrition and digestive issues.
Treatment at UT MD Anderson
Bile duct cancer is treated in our
Gastrointestinal Center.
Featured Articles

Stage III bile duct cancer survivor: ‘I can’t imagine being anywhere but MD Anderson’
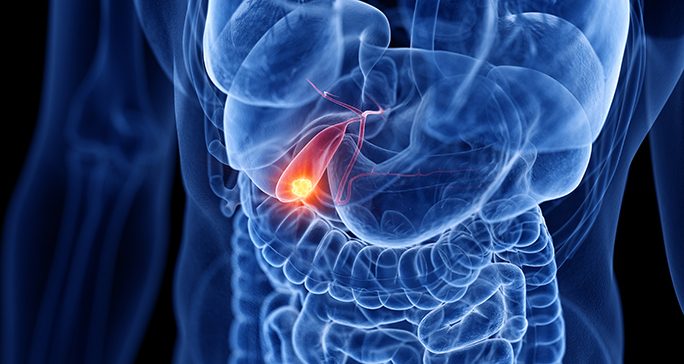
Gallbladder cancer: 9 facts about symptoms, diagnosis and treatment
A next-generation treatment for bile duct cancer

Biliary tract cancer survivor: Come to MD Anderson first

Singing surgeon puts liver cancer patient at ease during COVID-19 pandemic
Clinical Trials
UT MD Anderson patients have access to clinical trials offering promising new treatments that cannot be
found anywhere else.
Becoming Our Patient
Get information on patient appointments, insurance and billing, and directions to and around UT MD Anderson.
myCancerConnection
Talk to someone who shares your cancer diagnosis and be matched with a survivor.
Prevention & Screening
Many cancers can be prevented with lifestyle changes and regular screening.
Counseling
UT MD Anderson has licensed social workers to help patients and their loved ones cope with cancer.
Help #EndCancer
Give Now
Donate Blood
Our patients depend on blood and platelet donations.
Shop UT MD Anderson
Show your support for our mission through branded merchandise.
