request an appointment online.
- Diagnosis & Treatment
- Cancer Types
- Bone Cancer
Get details about our clinical trials that are currently enrolling patients.
View Clinical TrialsIn the United States, more than 3,200 people each year are diagnosed with primary cancer of the bones and joints. These make up 0.2% of all cancers in this country.
In the United States, more than 3,200 people each year are diagnosed with primary cancer of the bones and joints. These make up 0.2% of all cancers in this country.
What is bone cancer?
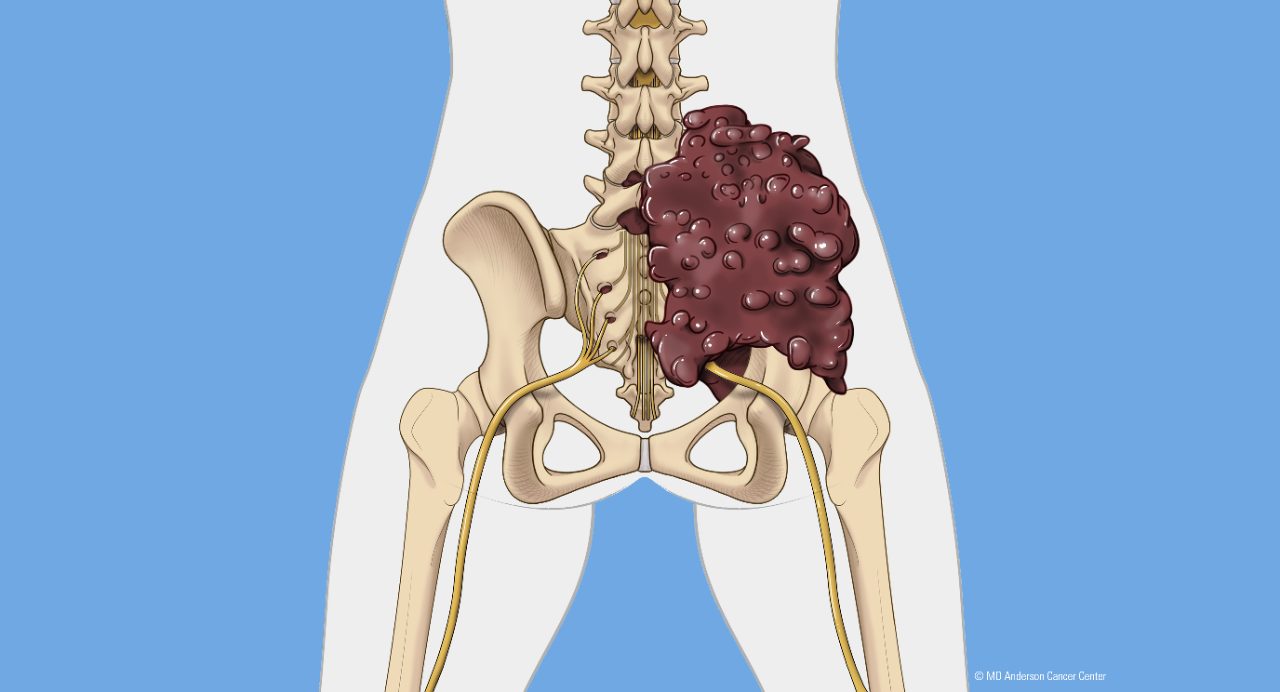
Bone cancer occurs when cells in the bone mutate and begin to grow uncontrollably. These cancer cells can damage normal bone tissue, interfere with blood cell production and weaken bones, increasing the risk of fractures. Other cancers may affect bones, including cancers that spread from other parts of the body, non-Hodgkin lymphoma and multiple myeloma. This page focuses on primary bone cancers.
Types of bone cancer
There are several types of bone tumors classified by the tissue or cell type in which they originate. Bone tumors can be benign (non-cancerous) or malignant (cancerous). Common types of primary bone cancer include:
- Osteosarcoma (osteogenic sarcoma): The most common bone cancer in children and adolescents, accounting for about one-fourth of adult bone cancers. It typically develops in the pelvis, arms or legs, especially near the knee but can involve any bone in the body. About 1,000 people are diagnosed each year in the U.S., with males more commonly affected than females. It can occur in adults as well but that is less common.
- Chondrosarcoma: Cancer of cartilage cells, accounting for more than 40% of adult bone cancers. It is most common in people over 40 and often diagnosed at an early stage. Tumors tend to develop in areas such as the pelvis, arms or legs.
- Ewing’s sarcoma: The second most common bone cancer in children and adolescents and third most common in adults. It accounts for about 8% of adult bone cancers and can start in bones, soft tissue or organs, particularly the pelvis, chest wall, legs or arms.
Less common types include:
- Chordoma: Typically arises in the spine or base of the skull, accounting for roughly 10% of adult bone cancers.
- Undifferentiated pleomorphic sarcoma: Usually starts in connective tissue but can also start in bone.
Who gets bone cancer?
Primary bone cancer is rare and can affect people of all ages. Osteosarcoma is most common in teenagers and young adults and is often associated with growth spurts. Chondrosarcoma primarily affects adults over 40 while Ewing’s sarcoma is more common in children and adolescents.
Symptoms of bone cancer
Symptoms can vary depending on tumor type, location and size but common signs include:
- Persistent bone pain that worsens at night or with activity
- Swelling or a lump near a bone or joint
- Fractures that occur with minimal trauma
- Fatigue, fever or unintended weight loss
- Decreased mobility in affected limbs
Learn more about bone cancer symptoms.
Treatments for bone cancer
Treatment depends on cancer type, location, stage and overall health and may include one or more of the following:
- Chemotherapy: Chemotherapy drugs kill cancer cells, control tumor growth or relieve symptoms. It is commonly used for osteosarcoma and Ewing’s sarcoma.
- Surgery: Surgery is often the main therapy to remove the tumor while preserving as much healthy bone and tissue as possible. In some cases, limb-sparing surgery or amputation may be necessary.
- Radiation therapy: Radiation therapy uses high-energy beams to destroy cancer cells, sometimes used for Ewing’s sarcoma, chordoma or tumors not fully removable by surgery.
- Targeted therapy: Drugs that interfere with specific molecules or genes that promote tumor growth, sometimes used in certain bone sarcomas.
- Clinical trials: Investigational treatments, including new drugs, immunotherapies or surgical techniques.
- Active surveillance (“watch and wait”): Careful monitoring with imaging and lab tests for tumors that are slow-growing or are not causing symptoms.
Learn more about bone cancer treatments.
Survival rates
Survival depends on tumor type, stage at diagnosis and response to treatment:
- Osteosarcoma: The five-year survival rate is approximately 70% for localized tumors. Survival rates are lower if the cancer has spread or is in a location that cannot be removed by surgery.
- Chondrosarcoma: The five-year survival rate ranges from 80–90% for low-grade tumors, which are slow-growing and less likely to spread. Survival rates are lower for high-grade tumors, which grow more quickly, are more aggressive, and are more likely to spread to other parts of the body.
- Ewings sarcoma: The five-year survival rate is approximately 70% for localized disease and decreases to 15–30% when the cancer has spread.
Risk factors for bone cancer
Several factors can increase a person’s risk of developing bone cancer. Having one or more risk factors does not mean you will get bone cancer, but it can help identify people who may need closer monitoring or genetic counseling.
Genetic and familial risk factors
Some inherited conditions or family history can slightly increase the risk of bone cancer, including:
- Li-Fraumeni syndrome: a rare inherited disorder that increases the risk of several types of cancer, including bone cancer
- Rothmund-Thompson syndrome: a genetic condition associated with a higher risk of osteosarcoma
- Retinoblastoma: an eye cancer in children; survivors and their relatives may have an increased risk of bone cancer later in life
- Multiple osteochondromas: a condition where multiple benign bone growths increase the risk of malignant transformation
Genetic counseling may be appropriate for individuals with these conditions or a family history of bone cancer. A genetic counselor can help assess personal and family risk and discuss whether genetic testing is recommended.
Other risk factors
- Other conditions or exposures that may increase the risk of bone cancer include:
- Paget’s disease of bone: a chronic condition that interferes with your body's normal recycling process, in which new bone tissue gradually replaces old bone tissue.
- Prior radiation therapy: Previous radiation treatment at a young age or treatment with high doses in the past can increase the risk of developing bone sarcomas years later.
- Bone marrow transplant: Patients who have undergone a transplant may have an elevated risk of developing bone-related cancers.
Learn more about bone cancer:
Learn more about clinical trials for bone cancer.
MD Anderson is #1 in Cancer Care
Orthopedic oncologist passionate about helping patients regain mobility
Valerae Lewis, M.D., always knew she wanted to be a doctor. Math and science fascinated her. She liked working with her hands. As a child, she already had her career planned out.
“I was going to be a doctor Monday through Friday, a carpenter at my workshop on Saturday and, on Sunday, I would own a gas station, so that I could wipe down all the drivers’ car windows,” Lewis recalls with a laugh.
Today, she may not be a carpenter or own a gas station, but Lewis is living out her doctor dreams as chair of MD Anderson’s Department of Orthopaedic Oncology.
Road to becoming an orthopedic oncologist
With a father who was an internal medicine doctor and a mother with a master’s degree in education, Lewis and her two older sisters learned the value of education early.
“As a child, I remember working in my dad’s doctor’s office, though I probably hindered more than I actually helped!” she says. “My dad always emphasized the importance of education, and he ended every conversation with ‘study hard and get good grades.’”
That she did. When it was time to select a college, Lewis weighed acceptances to both Harvard and Yale. She ultimately decided to attend Yale.
“My mom’s wish was to have one of her daughters go to Harvard, so I promised her I would attend Harvard after I graduated from Yale,” says Lewis.
A few years later, Lewis made good on her promise when she enrolled in Harvard Medical School.
“I wanted to be a surgeon because I really liked working with my hands,” she says. “To me, surgery was like fixing something, and that gave me immediate gratification.”
She fell in love with orthopedics at Harvard.
“I had two mentors in medical school, and they were both orthopedic oncologists,” she says. “They made orthopedic oncology exciting. As an orthopedic oncologist, you operate anywhere in the body, and no operation is ever the same. You are always challenged because a tumor changes the anatomy of the body.”
Lewis also liked the camaraderie she experienced with the orthopedic surgeons.
“Doctors often go into their specialty because they like the people in that specialty,” she says. “I felt like the orthopedic surgeons were very team-oriented. We always supported each other.”
A leader in orthopedic surgery
At MD Anderson, Lewis is an orthopedic oncology surgeon with specific expertise in limb salvage and pelvic sarcoma surgery in adult and pediatric cancer patients. Lewis is part of a small number of Black female orthopedic surgeons in the United States. She is also the first Black woman to chair an orthopedic surgery department in the United States.
“I encourage anyone who’s interested to consider pursuing orthopedic surgery as a profession," Lewis says.” It is truly rewarding.”
Making sure patients have a voice
In the operating room, Lewis leads a team of surgeons performing complex surgeries.
“I really love and respect the anatomy of the human body,” she says. “The resilience of the human body is unbelievable. I like being challenged in the operating room. That really drives me.”
Challenging operations could include anything from a rotationplasty on a 10-year-old osteosarcoma patient to a hemipelvectomy on a 17-year-old Ewing’s sarcoma patient.
“One of the mottos in our department is ‘We keep kids running,’” says Lewis. “Getting rid of the cancer is always the first goal. But the reconstruction and getting patients – child or adult – back to participating in the activities they enjoy is incredibly important. It helps with prognosis and longevity of life. If we can get you back up and moving, you’re definitely going to do better.”
And Lewis makes sure every patient has a say in what their surgical treatment looks like.
“Before surgery, we talk to the patient about their life and expectations,” says Lewis. “With younger kids, I encourage them to tell me how they feel because they have to be comfortable with their decision, whether that’s amputation, a rotationplasty, limb salvage, prosthesis or something else. I present the options and explain the pros and cons of each. Then we work together to decide the best option.”
A fulfilling purpose
For more than 20 years, Lewis has been helping MD Anderson patients with cancers of the bone and soft tissue get back to walking, running, jumping and being active.
“I love my patients and the relationships we develop,” she says. “There are patients I worked with decades ago who I’ve watched grow up. I’m always happy to hear about their families, watch them graduate high school and college, get married and have children of their own.”
Lewis is excited about sarcoma research and other advances that will help MD Anderson better treat patients with cancer of the bone and soft tissue.
“3D modeling and 3D printing are examples of exciting new tools,” says Lewis. “They not only guide us in the operating room, but they help patients better understand their tumor.”
Lewis started MD Anderson’s Multidisciplinary Pelvic Sarcoma Program in 2011. Through this program, she has been critically evaluating the oncologic and functional outcomes of pelvic sarcoma surgery.
“I like that we’ve been performing these procedures long enough that we can evaluate what we do and how we do it,” she says. “For example, with hemipelvectomies where we remove part of a patient’s pelvis, one option is to reconstruct with custom 3D prosthesis. Another approach is to reconstruct without a metal prosthesis, using only soft tissue. By critically evaluating our approach and outcomes, we have shown that both approaches can provide a patient with the ability to ambulate and perform their daily activities – even some sports. In some cases, we're going back to what we used to do years ago, but with better technique.”
While the most enjoyable part of Lewis’ job is being in the operating room, the most fulfilling part of her job is seeing patients get better.
“Seeing patients at two years out, five years out and then discharging them from clinic at 10 years – that’s the best,” she says. “I love seeing them reach those milestones. I always tell patients that my goal is to get them old.”
Request an appointment at MD Anderson online or call 1-877-632-6789.
Understanding chondrosarcoma: symptoms, treatment and prognosis
Chondrosarcoma is a rare type of bone cancer that develops in cartilage cells. It is the most common bone cancer in adults.
Conventional chondrosarcoma is the most common type of chondrosarcoma. These tumors are often located in the pelvis and the top part of the thigh and arm.
To learn more about chondrosarcoma, including symptoms to look out for, treatment options and prognosis, we tapped the experts: sarcoma medical oncologist Anthony Conley, M.D., and orthopedic oncology surgeon Justin Bird, M.D.
What are the different types of chondrosarcoma?
Conventional chondrosarcoma makes up about 80% of cases and usually occurs in people in their 50s and 60s, says Conley. These tumors tend to be slow-growing.
Other, rarer types of chondrosarcoma are:
- dedifferentiated chondrosarcoma
- mesenchymal chondrosarcoma
- clear cell chondrosarcoma
These types can grow quickly and spread. This often makes them harder to treat.
What causes chondrosarcoma?
It’s not known what exactly causes chondrosarcoma.
“We think sometimes cells in the bone get reprogrammed for reasons that are not clearly understood,” says Conley.
Some conditions can increase your chance of developing chondrosarcoma. These include:
Enchondromatosis
This is a rare disorder in which benign growths called enchondromas form in the bone. Sometimes, these growths can transform into chondrosarcoma.
Ollier disease
This is when people develop enchondromas all over the body, usually in the hands and feet. About 10% or fewer cases transform into chondrosarcoma.
Maffuci syndrome
This happens when people develop enchondromas as well as benign growths in their blood vessels, causing them to become enlarged.
Osteochondromatosis
This is a condition in which abnormal bone growths occur on the ends of long bones in the arms or legs. It can sometimes lead to chondrosarcoma. Osteochondromatosis can be hereditary, meaning it can be passed down from a parent to a child.
Primary synovial chondromatosis
This is when benign growths form in the synovium, the soft connective tissue that lines joints like the knee and elbow. Most can be removed with surgery, but sometimes a person will have one that degenerates and becomes a chondrosarcoma.
What are the symptoms of chondrosarcoma?
The most common symptoms of chondrosarcoma are:
- a lump
- pain or swelling near the tumor
- change in function, such as the ability to move your arm or leg correctly
“It’s easy for people to tolerate pain to a certain extent, but you should see a doctor if you feel a lump on your body that’s new and/or growing quickly,” says Conley. “Some doctors may assume it’s benign, like a lipoma. But if it continues to grow, cause pain or change in any way, go back to your doctor or seek a second opinion. At the end of the day, you are your best advocate.”
How is chondrosarcoma diagnosed?
If you have symptoms of chondrosarcoma, your doctor may order diagnostic tests. These could include:
X-ray
If you have symptoms related to the bone, an X-ray can provide information about the edges of the bone, the center of bone marrow and the bone’s overall architecture. If there is bone loss or bone growth where there shouldn’t be, that’s the trigger to get imaging done.
MRI or CT scan
An MRI is preferred, but you may get a CT scan if you have a medical device in your body that keeps you from getting an MRI. If doctors find a suspicious lesion during the scan, a biopsy is the next step.
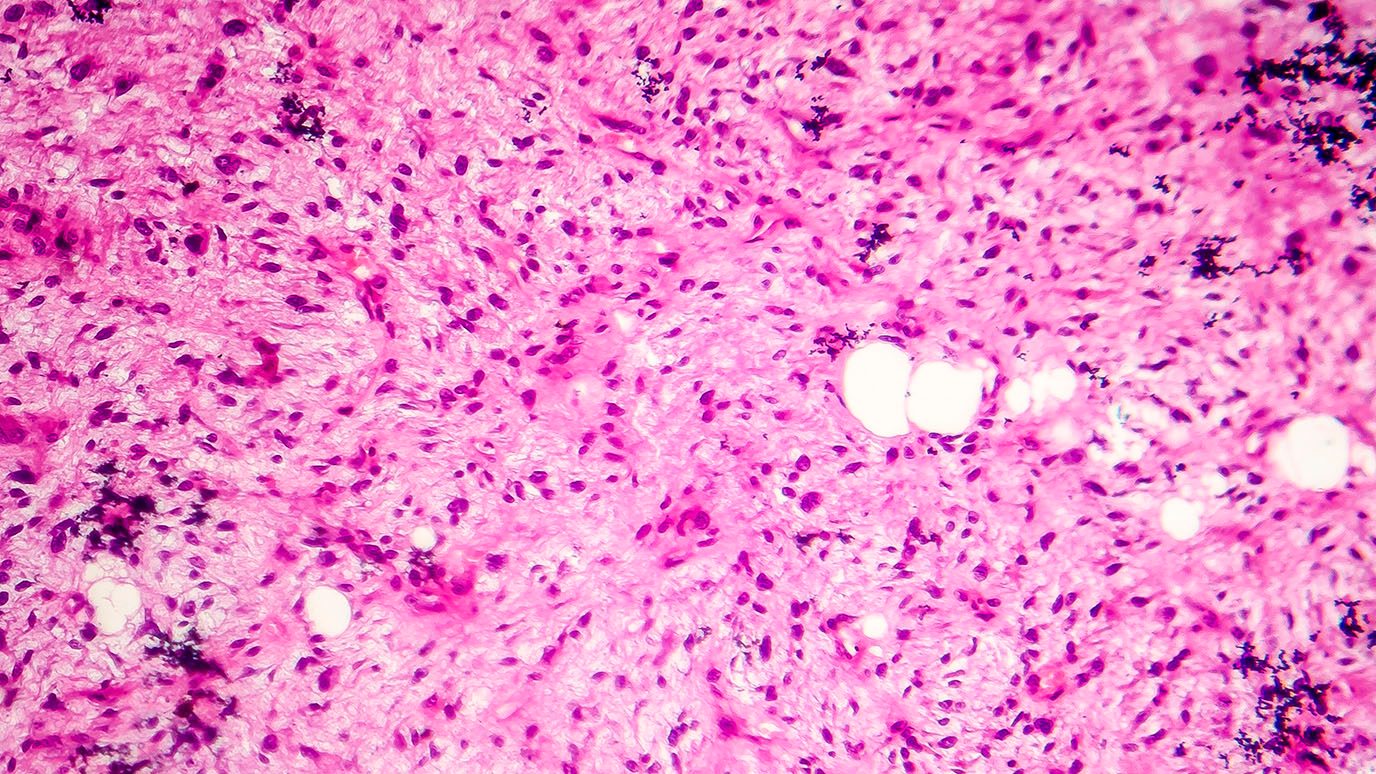
Biopsy
During the biopsy, a piece of tissue is taken to be reviewed by a pathologist. The pathology results will determine if you have chondrosarcoma.
“After a diagnosis is made, the next step is staging the disease,” says Conley. “Is it localized? Are we dealing with one spot, or has it moved to other parts of the body? That’s when it becomes necessary to get imaging of the chest, preferably the abdomen and pelvis because chondrosarcomas can move to other organs.”
How is chondrosarcoma treated?
Treatment for chondrosarcoma depends on several factors, including the disease stage and grade, and whether the tumor can be removed surgically. Your care team will work together to find the best treatment plan for you.
Surgery
Surgery is the most common treatment for chondrosarcoma.
“Some conventional chondrosarcomas can be cured with surgery,” says Conley.
Bird, who specializes in spine and pelvic tumors, often uses 3D modeling to help design the surgeries.
“We’re dealing with complex anatomy,” says Bird. “The models provide a physical representation of the tumor that is easier to process than MRI and CT scans because you don’t have to scroll through all the different imaging slices to get a sense of the entire tumor and relevant anatomy.”
3D printing also assists with stereotactic navigation during surgery by allowing for more precision and accuracy.
“Surgery may be a good option for someone with a primary tumor, or single site of disease,” says Bird. “If you have a low-grade tumor in the finger, for example, we may surgically scrape it out. This is called an intralesional procedure where we remove the lesion piece by piece.”
But this type of surgery isn’t ideal for higher-grade tumors.
“We surgically remove high-grade tumors by taking it out all in one piece as well as the tissue around it to achieve negative margins,” says Bird. “This helps lower the chance for recurrence.”
Surgical treatment can also be more aggressive like amputation to remove a limb or a weight-bearing bone. These patients may receive physical therapy or occupational therapy after surgery.
Surgery is typically not an option for those with metastatic disease. At this point, the cancer cannot be cured.
“We’re researching to find new ways to treat metastatic chondrosarcoma that can’t be removed with surgery,” says Conley. “We’ll talk with the patient to see if they’d be a good fit for a clinical trial.”
Chemotherapy
More aggressive types of chondrosarcoma, like dedifferentiated chondrosarcoma and mesenchymal chondrosarcoma, often respond well to chemotherapy.
Patients with these types of diseases are given chemotherapy before surgery. They receive more chemotherapy after surgery to kill any residual microscopic disease.
Radiation therapy
Sometimes, patients with localized disease, or cancer that is just in one area, are unable to get surgery for medical reasons. In those cases, radiation therapy may be used to treat the tumor.
What is the prognosis for people with chondrosarcoma?
How chondrosarcoma will affect you long-term depends on many factors, including the:
- location of the disease
- type of surgery you have
- technical skill of your doctors
Each patient is unique, so it’s important to discuss your prognosis with your doctor.
“It’s more common to see patients with localized disease, which can be stage I or stage II,” says Conley. “Overall survival for these patients can exceed 80% at five years, depending on the situation. And if you have stage I chondrosarcoma, your chance of surviving five years is going to be closer to 90% to 95%.”
Recurrent chondrosarcoma has a different prognosis
Prognosis becomes a bit trickier for patients who develop recurrent disease.
“The higher the grade, the higher the chance the chondrosarcoma will recur,” says Bird. “Low-grade tumors are less likely to recur, and when they do, they often grow back as low-grade. But sometimes things can change, and over time a low-grade tumor can transform and come back more aggressive.”
Not all stage IV disease is the same.
“Some people can relapse with 50 lumps, and some may relapse with only one lump. But, if it’s in a different organ, it’s classified as stage IV,” explains Conley. “The most common site of metastasis is the lung. If I have a relapsed patient with one or two spots on their lung, I believe we can potentially cure them. For relapsed patients with more advanced disease, curing the disease may not be possible. In those cases, our goal is to keep patients alive as long as possible with a preserved quality of life.”
TP53 mutation can affect chondrosarcoma prognosis
In recent years, genetic testing has helped to advance chondrosarcoma treatment.
For patients with recurrent chondrosarcoma, surgery and systemic therapies are not an option. In these cases, Conley says, MD Anderson will analyze the patient’s tumor tissue. What they find from the tissue can help them select targeted trials best suited for the patient.
An MD Anderson study published in 2023 found that patients with conventional and dedifferentiated chondrosarcoma who have the TP53 gene mutation have a poorer prognosis.
“For years, the only prognostic factor was the grade of the tumor,” says Conley. “But what we’ve proven through research is that the TP53 mutation can help determine prognosis as well. This helps us counsel patients during treatment.”
What should people keep in mind when deciding where to seek chondrosarcoma treatment?
If you are diagnosed with chondrosarcoma, it’s important to seek care at a comprehensive cancer center like MD Anderson with experts who have seen this type of cancer multiple times.
“At MD Anderson, there’s a multidisciplinary team of experts who deal with bone tumors,” says Conley. “They say it takes a village to raise a person. Similarly, it takes a village to treat chondrosarcoma. Each year, we see more than 200 bone tumor patients, including people with chondrosarcoma. When you see this disease as often as we do, you start to pick up patterns. We’re always researching new ways to treat chondrosarcoma and building upon that research to help more patients and their families.”
Request an appointment at MD Anderson online or call 1-877-632-6789.
How interventional radiology is used to manage cancer-related bone pain
Many types of cancers can spread to the bone, leading to areas of damage called lesions. 80% of patients with metastatic prostate cancer develop bone lesions, but it’s also common in patients with many other types of cancer including metastatic breast cancer and metastatic renal cell carcinoma. These lesions leave patients in pain and sometimes impact mobility. They’re most commonly found in the ribs, the pelvis and the spine. Bone metastases occasionally occur in the shoulders and legs.
Usually, chemotherapy or immunotherapy can treat a bone lesion, and radiation therapy and pain medicine help manage their associated cancer pain. But these traditional methods don’t always work or aren’t an option for all patients.
MD Anderson is leading a new approach for patients with bone metastases that uses interventional radiology. These techniques offer patients a new option for pain management that can provide fast relief with few side effects. Interventional radiologist Rahul Sheth, M.D., shares how these minimally invasive procedures are changing the way we manage cancer bone pain.
What is interventional radiology?
Interventional radiology combines diagnostic imaging techniques like X-rays or CT scans with therapeutic procedures done inside the body. The procedures are performed through small pinholes in the skin and can help address a variety of medical concerns – not just cancer. The diagnostic imaging tools allow us to take pictures in real-time during the procedure. That way, we know exactly where everything is at all times without having to make a big incision to open the patient up.
Instead, patients receive small punctures, similar to needles through the skin. And, there are no stitches afterward. We essentially put a Band-Aid on top while the punctures heal over the next couple of days.
For patients with bone metastases, interventional radiology can provide a real benefit in managing pain. Although each patient is different, most people go home the same day or the next day, and they feel relief a few days after the procedure.
Reasons for cancer bone pain
Bone tumor-related pain can be caused by one or a combination of three things. The first is the cancer cells themselves. When the tumor’s cells take root inside the bone, their presence releases inflammatory proteins, which cause local inflammation. The brain perceives that inflammation as pain.
Second, as the cancer cells erode the bone, they can cause inflammation at the lining of the bone, which is where nerve fibers are found. As the tumor grows and the lining of the bone stretches, and the tumor can break out of the bone and cause pain.
Lastly, if the tumor is on a weight-bearing bone like the spine or the pelvis, it can cause pain. It’s just like when you break your wrist: There are fractures in the bone, and the fragments move around. As you move, the fragments rub against each other and can’t heal. This leads to inflammation that causes pain.
With interventional radiology, we tailor our treatment approach to address which of these three – or all three – are causing the pain.
When pain medicine and radiation therapy aren’t an option, interventional radiology may be
Even when prescribed at a high dosage, an opioid may not relieve bone cancer pain for a patient. Interventional radiology procedures can help wean patients off opioids while offering long-term pain relief.
Radiation therapy is another common approach for addressing pain, but it’s not an option for everyone. If a patient has already received radiation in that area, this treatment can’t typically be used again. But another benefit of interventional radiology is that the procedures can be repeated. Also, if a patient is receiving chemotherapy, they may have to pause the drugs to schedule radiation therapy. If the cancer is aggressive, this could be an issue. Interventional radiology is conveniently combined with other treatments since the procedures and recovery are quick.
Some cancer types are known to be resistant to radiation therapy. In those cases, we try to be more aggressive with treatment. At MD Anderson, we’re conducting a clinical trial that’s investigating stereotactic body radiation therapy combined with interventional radiology techniques. Our goal is to speed up how soon patients feel relief and maximize how long that relief lasts.
Interventional radiology helps destroy a bone tumor
The best way to address pain directly caused by a tumor on the bone is to eliminate the tumor. Two interventional radiology approaches we commonly use are ablation and embolization.
- Ablation: We destroy a tumor by subjecting it to extreme temperatures – either hot or cold. We insert a needle through the skin and into the tumor. That needle generates heat at its tip to heat the tumor, or it freezes the tumor into a ball of ice. We monitor the size of the ice ball with imaging techniques. This allows us to ensure we’re treating the entire tumor and avoiding surrounding normal tissue. At MD Anderson, we’re also exploring using ablation to improve systemic cancer treatments like immunotherapy.
- Embolization: By working with a patient’s blood vessels, we can destroy a tumor. Like the way cardiologists place stents in the blood vessels supplying blood to the heart, we do the same thing to the blood vessels supplying blood to a tumor. We enter the body, often through the leg or the wrist, and navigate to the tumor inch by inch, using X-rays to follow along. Next, we pack the blood vessels with thousands of microscopic plastic beads that float deep into the tumor and block the blood flow. This cuts off oxygen and nutrients and leads to the tumor’s death.
We often combine these techniques to maximize their benefit.
Bone cement stabilizes the bone to relieve pain
If the pain is caused by a tumor destroying the bone, we have a different approach. Much like a cast helps hold together broken bone so that it can heal, we do the same thing on the inside with bone cement. We glue together the bone fragments to hold them in place and speed up healing. The cement stops the constant motion of the fractured bone, and the patient feels relief soon after the procedure. In our recovery area, patients often already start to feel improvement in their pain levels.
This pain is a huge quality of life factor for our patients, and it’s gone within a few hours, thanks to these approaches. Personally, it's very fulfilling and rewarding work.
Request an appointment at MD Anderson online or by calling 1-877-632-6789.
Why choose MD Anderson for bone cancer treatment?
MD Anderson's Sarcoma Center treats more osteosarcoma, or bone cancer, patients than any other cancer center in the nation. In fact, we are one of the few teams in the world devoted to bone cancer, and our patients have an 80% five-year event-free survival rate.
We bring together a team of experts that includes specialists from many areas to give you personal, customized care. We use specialized therapies and technologies to be sure you receive the most advanced treatment with the least impact on your body.
If possible, it is best to have a biopsy to diagnose bone cancer at the same place you receive treatment. It is essential to go to a specialized cancer center that has experience in osteosarcoma biopsy. If the biopsy is done incorrectly, it may make it more difficult later for the surgeon to remove all of the cancer without having to also remove all or part of the arm or leg. A biopsy that is not done correctly also may cause the cancer to spread.
As one of the world's leading cancer centers, we constantly work to discover new treatments and innovations. We helped pioneer:
- Embolization for localized unresectable giant cell tumor of bone
- Activity of interferon in metastatic giant cell tumor of bone
- Limb-sparing surgery to help save arms and legs
- Targeting a cell receptor known to play a part in the spread of cancer to the bones may enable chemotherapy drugs to be delivered directly to the cells
Being positive is the best medicine you can take.
Maggie Howard
Survivor
Treatment at MD Anderson
Bone cancer (osteosarcoma) is treated in our Sarcoma and Orthopaedic Center.
Clinical Trials
MD Anderson patients have access to clinical trials offering promising new treatments that cannot be found anywhere else.
Becoming Our Patient
Get information on patient appointments, insurance and billing, and directions to and around MD Anderson.
myCancerConnection
Talk to someone who shares your cancer diagnosis and be matched with a survivor.
Prevention & Screening
Many cancers can be prevented with lifestyle changes and regular screening.
Counseling
MD Anderson has licensed social workers to help patients and their loved ones cope with cancer.
Help #EndCancer
Give Now
Donate Blood
Our patients depend on blood and platelet donations.
Shop MD Anderson
Show your support for our mission through branded merchandise.