request an appointment online.
- Diagnosis & Treatment
- Cancer Types
- Fallopian Tube Cancer
Get details about our clinical trials that are currently enrolling patients.
View Clinical TrialsFallopian tube cancer typically forms in the cells that line the inside of the fallopian tubes, the two small ducts that connect the ovaries to the uterus.
Fallopian tube cancer typically forms in the cells that line the inside of the fallopian tubes, the two small ducts that connect the ovaries to the uterus.
If a woman has not gone through menopause, her ovaries produce eggs (ova) that travel through the fallopian tubes to the uterus. They help move the eggs to the uterus.
Fallopian tube cancer types
The main type of primary fallopian tube cancer is high grade serous adenocarcinoma. These cancers start in the cells lining the fallopian tubes.
Primary fallopian tube cancers are often indistinguishable from primary ovarian cancers because women present at very advanced stages. In fact, studies have demonstrated that most high grade serous ovarian cancers likely arose from fallopian tube epithelium.
Fallopian tube cancer risk factors
Fallopian tube cancer risk factors are similar to ovarian cancer risk factors. Risk factors may include:
- Age, race and number of children: Fallopian tube cancer can occur in women of any age, but it most often is found in women between 60 to 66 years old.
- Family history of fallopian tube or ovarian cancer
- Gene mutations: Women who have certain gene mutations may have a higher risk of fallopian tube cancer. These include:
- BRCA gene mutations, particularly BRCA1, which cause high risk of breast and ovarian cancer
- One of the genes that cause hereditary nonpolyposis colorectal cancer (HPNCC), also called Lynch syndrome
Some women have a lower risk of getting fallopian tube cancer. These include women who have:
- Used birth control pills
- Delivered and breast-fed children. The more children you have had, the lower your risk of fallopian tube cancer.
Not everyone with risk factors gets fallopian tube cancer. However, if you have risk factors, it’s a good idea to discuss them with your health care provider.
If you are concerned about inherited family syndromes that may cause fallopian tube cancer, learn more about the risk to you and your family on our genetic testing page.
Learn more about fallopian tube cancer:
- Fallopian tube cancer symptoms
- Fallopian tube cancer diagnosis
- Fallopian tube cancer stages
- Fallopian tube cancer treatment
Learn more about clinical trials for fallopian tube cancer.
UT MD Anderson is #1 in Cancer Care
Fallopian tube cancer
This episode discusses fallopian tube cancer, a very rare tumor, and how it compares to typical ovarian cancer. Topics include treatment, diagnosis, and symptoms.
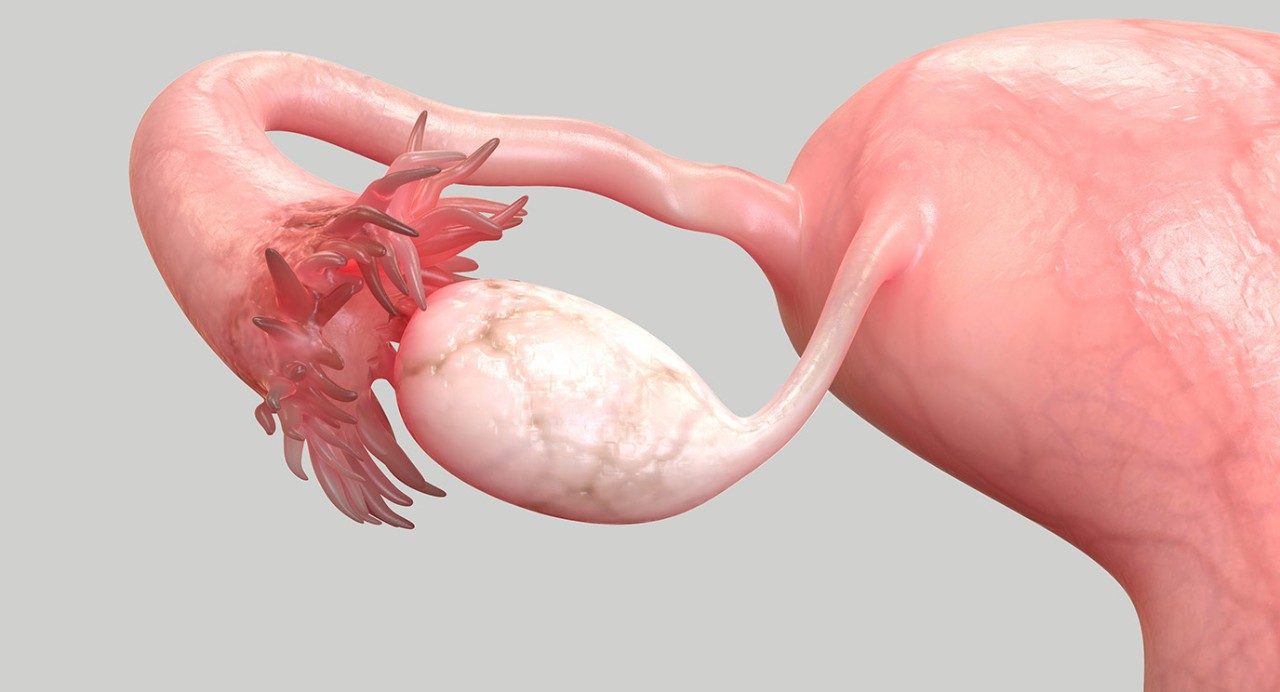
Should you have your fallopian tubes removed to reduce your ovarian cancer risk?
A woman could have her fallopian tubes removed for any number of reasons. Sometimes, it’s necessary to treat an ectopic pregnancy or to resolve an infection caused by pelvic inflammatory disease. In other cases, it’s done as a form of permanent birth control.
But a growing body of evidence suggests that the distal fallopian tube — or flower-shaped section located nearest the ovary — is the site of many cases of high-grade serous ovarian cancer, the most common type of ovarian cancer and one of the most aggressive.
Research also suggests that an opportunistic salpingectomy — the complete removal of the fallopian tubes during an unrelated pelvic surgery — could help reduce the chances of one day developing ovarian cancer.
So, who should consider having their fallopian tubes removed, and when? And, should anyone who’s finished childbearing seek out the procedure, even if they’re only at average risk of ovarian cancer? We asked Michaela Onstad-Grinsfelder, M.D., a surgeon specializing in gynecologic cancers.
Why do women typically have their fallopian tubes removed?
Women don’t usually go in just to have their fallopian tubes removed unless it’s for permanent birth control or to treat an ectopic pregnancy.
Having the fallopian tubes removed is one form of surgical sterilization, or “having your tubes tied.” Until fairly recently, it was more common for surgeons to use a metal clip or a ring to constrict and physically block the tubes, rather than removing the structures themselves.
Why has that changed?
A growing body of data suggests that the fallopian tubes may be the origin of many ovarian cancers. So, a lot of surgeons have changed their practice to remove the fallopian tubes entirely to give patients additional protection against ovarian cancer.
In the United States, the Society for Gynecologic Oncology and the American College of Obstetricians and Gynecologists both support the removal of fallopian tubes as permanent sterilization for women at average risk for ovarian cancer, but it’s also recommended by professional organizations in Australia, Canada, Germany and New Zealand.
How was this information discovered?
After the BRCA gene was linked to an increased risk for breast and ovarian cancers, doctors started removing the ovaries and fallopian tubes as a type of risk-reduction surgery, once BRCA-positive women were finished with childbearing.
Most ovarian cancers are diagnosed at stage III or IV, so we don’t usually see the disease in its earliest stages. But what we noticed when we started performing these surgeries is that there were often pre-cancerous lesions present in the fallopian tubes.
This was a really exciting discovery because, before that, we hadn’t known there was a lesion that could one day become ovarian cancer. So, we were able to start finding ovarian cancers really early that we hadn’t been able to catch before.
How did that discovery lead to the recommendation of opportunistic salpingectomies?
There was a lot of excitement in the medical community at that point about the possibility of reducing the risk of ovarian cancer by removing the fallopian tubes during hysterectomies or when patients were having their “tubes tied.” Before that, whenever someone had a hysterectomy, we would normally only take out their fallopian tubes if we were also taking out their ovaries.
But as the new data emerged, there was an increased interest in removing the fallopian tubes along with the uterus when performing hysterectomies. Because if a woman is pre-menopausal, her ovaries might still be benefitting her. But once she’s finished childbearing, the fallopian tubes serve no real purpose.
So, who should consider having their fallopian tubes removed?
People who are at increased risk of developing ovarian cancer, such as those who carry the BRCA genetic mutation, are recommended to have a stand-alone surgery to remove fallopian tubes with both ovaries (called a risk-reducing salpingo-oophorectomy).
Otherwise, it’s only recommended as an opportunistic salpingectomy: something to be done when you’re already having another type of gynecologic procedure, such as a hysterectomy.
Are any related clinical trials available?
We have a clinical trial going on right now for BRCA-positive women who are done with childbearing but are not quite ready to have their ovaries removed.
In this clinical trial, participants will have their fallopian tubes removed now, but delay the removal of their ovaries until later (between the ages of 35 and 45 for patients with BRCA1 and between the ages of 40 and 50 for those with BRCA2). The goal is to determine if it may be safe to delay the removal of both ovaries for women at high risk of developing ovarian cancer.
Do you ever foresee a time in which an opportunistic salpingectomy could be combined with another procedure, such as an appendectomy or a hernia repair?
Right now, we don’t typically bundle other types of surgeries with the removal of fallopian tubes. That’s partially because only OB-GYNs are specifically trained in that procedure.
But we’re actively looking for ways to team up with other surgeons to offer this service together. It could be an exciting strategy in the future to further reduce patients’ risk of ovarian cancer.
Request an appointment at MD Anderson online or by calling 1-877-632-6789.
Why come to UT MD Anderson for your fallopian tube cancer care?
Fallopian tube cancer treatment at UT MD Anderson's Gynecologic Oncology Center includes comprehensive, multidisciplinary care that is planned by some of the nation's top experts. Your care team may include medical, surgical and radiation oncologists; pathologists; and diagnostic radiologists, all working toward the best possible treatment outcome. UT MD Anderson diagnoses and treats more patients with fallopian tube cancer than most oncologists in the United States.
UT MD Anderson uses the latest, most advanced technology and techniques to treat fallopian tube cancer. Among these are innovative surgical techniques, including minimally invasive options for some patients.
Studies have shown that the success of any surgery depends a great deal on the skill of the surgeon. UT MD Anderson's renowned surgeons have some of the highest levels of experience and expertise in fallopian tube cancer procedures and treating recurring cases.
Pioneering fallopian tube cancer research
If you are at high risk for fallopian tube cancer because of inherited genetic conditions, such as BRCA or HNPCC, UT MD Anderson offers complete genetic testing. Results can help you learn if you or your family members are at risk of certain types of cancer, including fallopian tube cancer.
Fallopian tube cancer is like ovarian cancer in some ways. Many studies in our renowned ovarian cancer research program are open to women with fallopian tube cancer. This enables us to offer a wider range of clinical trials than many other cancer centers.
And, at UT MD Anderson you're surrounded by the strength of one of the nation's top comprehensive cancer centers. We have all the support and wellness services needed to treat not just the disease, but the whole person.
Treatment at UT MD Anderson
UT MD Anderson fallopian tube cancer patients can get treatment at the following locations.
Clinical Trials
UT MD Anderson patients have access to clinical trials offering promising new treatments that cannot be found anywhere else.
Becoming Our Patient
Get information on patient appointments, insurance and billing, and directions to and around UT MD Anderson.
myCancerConnection
Talk to someone who shares your cancer diagnosis and be matched with a survivor.
Prevention & Screening
Many cancers can be prevented with lifestyle changes and regular screening.
Counseling
UT MD Anderson has licensed social workers to help patients and their loved ones cope with cancer.
Help #EndCancer
Give Now
Donate Blood
Our patients depend on blood and platelet donations.
Shop UT MD Anderson
Show your support for our mission through branded merchandise.
