Cascone Laboratory
Tina Cascone, M.D., Ph.D.
Principal Investigator
Areas of Research
- Lung Cancer
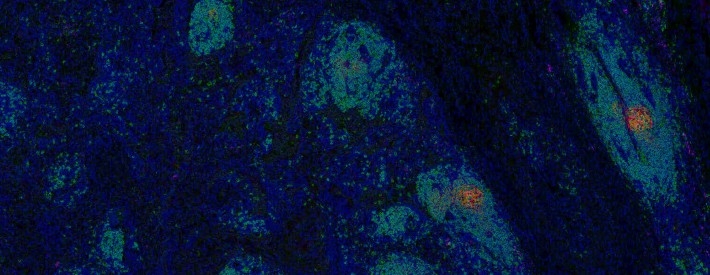
The Cascone Laboratory is focused on identifying immune-mediated mechanisms of tumor response and resistance to immune checkpoint therapies.
Scroll Ahead
- Departments, Labs and Institutes
- Labs
- Cascone Laboratory
The Cascone Laboratory uses information generated from preclinical models of spontaneously metastatic non-small cell lung cancer (NSCLC) and samples derived from patients with operable NSCLC treated with perioperative immune-based therapies to identify determinants of tumor resistance to immune-based therapies, discover predictive biomarkers of therapeutic response in primary resected and metastatic NSCLCs, and discover novel therapeutic targets and strategies that may improve the cure rates of patients with operable non-small cell lung cancer by preventing tumor recurrence, enhancing antitumor immunity and augmenting the efficacy of immunotherapies.
Join Our Lab
We are hiring highly motivated and driven postdoctoral fellows
Selected Publications
-
Cell Metabolism
Increased Tumor Glycolysis Characterizes Immune Resistance to Adoptive T Cell Therapy Opens a new window
Cascone T, McKenzie JA, Mbofung RM, Punt S, Wang Z, Xu C, Williams LJ, Wang Z, Bristow CA, Carugo A, Peoples MD, Li L, Karpinets T, Huang L, Malu S, Creasy C, Leahey SE, Chen J, Chen Y, Pelicano H, Bernatchez C, Gopal YNV, Heffernan TP, Hu J, Wang J, Amaria RN, Garraway LA, Huang P, Yang P, Wistuba II, Woodman SE, Roszik J, Davis RE, Davies MA, Heymach JV, Hwu P, Peng W. (2018).
-
Nature Medicine
Neoadjuvant nivolumab or nivolumab plus ipilimumab in operable non-small cell lung cancer: the phase 2 randomized NEOSTAR trial Opens a new window
Cascone, T., William Jr, W. N., Weissferdt, A., Leung, C. H., Lin, H. Y., Pataer, A., Godoy, M. C. B., Carter, B. W., Federico, L., Reuben, A., Khan, M. A. W., Dejima, H., Francisco-Cruz, A., Parra, E. R., Solis, L. M., Fujimoto, J., Tran, H. T., Kalhor, N., Fossella, F. V., ... Sepesi, B. (2021).
-
Nature Communication
Nodal immune flare mimics nodal disease progression following neoadjuvant immune checkpoint inhibitors in non-small cell lung cancer Opens a new window
Cascone, Tina & Weissferdt, Annikka & Godoy, Myrna & William, William & Leung, Cheuk & Lin, Heather & Basu, Sreyashi & Yadav, Shalini & Pataer, Apar & Mitchell, Kyle & Khan, Md & Shi, Yushu & Haymaker, Cara & Solis, Luisa & Parra, Edwin & Kadara, Humam & Wistuba, Ignacio & Sharma, Praneal & Allison, James & Sepesi, Boris. (2021).
In the News
Combination immunotherapy treatment effective before lung cancer surgery
Combination immunotherapy with the anti-PD-L1 monoclonal antibody durvalumab and other novel agents outperforms durvalumab alone in the neoadjuvant (pre-surgical) setting for early-stage non-small-cell lung cancer (NSCLC), according to researchers from The University of Texas MD Anderson Cancer Center.
The findings, published today in Cancer Discovery, were first presented at the American Association for Cancer Research (AACR) Annual Meeting 2022.
The multicenter, randomized Phase II NeoCOAST clinical trial evaluated neoadjuvant durvalumab alone and in combination with each of the following novel immunotherapies: the anti-CD73 monoclonal antibody oleclumab, the anti-NKG2A monoclonal antibody monalizumab and the anti-STAT3 antisense oligonucleotide danvatirsen. While the study was not statistically powered to compare arms, all combinations resulted in numerically higher major pathological response (MPR) rates than with durvalumab monotherapy.
“This study builds on the growing evidence that combination immunotherapy has a role in the neoadjuvant setting for this patient population,” said Tina Cascone, M.D., Ph.D., assistant professor of Thoracic/Head and Neck Medical Oncology and lead author of the study. “Ultimately, we want to give patients a chance to live longer without their cancer returning.”
The NeoCOAST trial adds to recent progress in neoadjuvant treatment for NSCLC, including the Phase II NEOSTAR study results that Cascone reported last year showing nivolumab and ipilimumab together induced higher responses than nivolumab alone, and the March 2022 approval of nivolumab combined with platinum-based chemotherapy from the Checkmate-816 study. The durvalumab combinations tested previously in the Phase II COAST trial were shown to be effective in unresectable stage III NSCLC, providing rationale for testing in earlier stage disease.
The NeoCOAST study enrolled 84 patients with untreated, resectable (>2cm), stage I-IIIA NSCLC, between March 2019 and September 2020. Most patients were male (59.5%) and had a smoking history (89%). The median age was 67.5, and the racial breakdown was 89% white, 6% Black, 2% Asian and 2% other. Eighty-three patients received one 28-day cycle of neoadjuvant durvalumab alone or combined with another therapy.
The primary endpoint was investigator-assessed MPR, defined as ≤10% residual viable tumor cells in the resected tumor tissue and sampled nodes at surgery. The investigators assessed pathological complete response (pCR), or complete disappearance of viable tumor cells, as a secondary endpoint. Exploratory endpoints included tumor, fecal and blood biomarkers.
All combinations had numerically higher rates of MPR and pCR than monotherapy, and there were no statistically significant differences in responses between the combination arms:
- For the patients who received durvalumab monotherapy, MPR occurred in 11.1% and pCR in 3.7%, which is comparable to results from other monotherapy studies.
- MPR rates for combination therapy ranged from 19% (oleclumab) to 31.3% (danvatirsen), and pCR rates ranged from 9.5% (with oleclumab) to 12.5% (with danvatirsen). For combination therapy with monalizumab, MPR was 30% and pCR was 10%.
The safety profile in the durvalumab monotherapy arm (treatment-related adverse events in 34.6% of patients) was similar to previously published data for anti-PD-1/PD-L1 antibodies. No new safety signals were identified with any of the combination regimens (treatment-related adverse events seen in 43.8% to 57.1% of patients).
MPR was associated with baseline tumor PD-L1 expression of ≥1% in the oleclumab and monalizumab combination arms. In the oleclumab (anti-CD73) combination arm, high baseline CD73 expression was associated with pathological tumor regression, and treatment decreased CD73 expression on tumor cells, as previously observed in other studies. The oleclumab combination also was associated with greater natural killer (NK) and CD8 T cell density in the tumor center on treatment compared with baseline, suggesting an increased infiltration of effector cells in the tumor microenvironment.
Updated translational studies on tumor tissues and blood samples revealed the impact of neoadjuvant treatment on the immune system. Transcriptome analysis on pre- and post-treatment samples showed an upregulation of genes associated with cytotoxicity, tertiary lymphoid structures and lymphocyte recruitment, all indicators of an activated immune response.
The number of patients with no detected circulating tumor DNA (ctDNA) increased progressively from pre-to post-treatment and post-surgery follow up, highlighting the relationship between decreasing ctDNA levels and improved patient outcomes. Notably, surgery was the most effective intervention to result in clearance of ctDNA. Researchers also found an enrichment of beneficial bacteria in the gut microbiome of patients who achieved MPR. These bacteria were previously associated with a favorable immunotherapy response across several cancer types.
“Our study is a testament to how clinical trials designed with translational findings in mind can support the rapid advancement of novel immune-based combinations to larger scale studies,” Cascone said. “I’m encouraged by these early findings as we work toward reducing the risk of recurrence and increasing cure rates for patients with early-stage non-small cell lung cancer.”
Limitations of the study include the exploratory nature of the endpoints, small sample sizes and investigator-assessed outcomes without central review.
Based on these results and the recent approval of neoadjuvant nivolumab plus chemotherapy, the team has launched a follow-up randomized clinical trial, NeoCOAST-2, with Cascone serving as the global principal investigator. The trial is now enrolling patients with resectable, stage IIA-IIIA NSCLC to receive neoadjuvant durvalumab combined with chemotherapy and either oleclumab or monalizumab, followed by surgery and adjuvant durvalumab plus oleclumab or monalizumab.
The study was funded by AstraZeneca, which developed durvalumab, oleclumab and monalizumab (with Innate Pharma). Cascone reports a consulting/advisory role and contracted institutional support/research consulting for MedImmune/AstraZeneca. A full list of co-authors and disclosures can be found here.
Neoadjuvant combination immunotherapy improves outcomes for early stage non-small cell lung cancer
The first randomized Phase II clinical trial to report on single and combined neoadjuvant immune checkpoint inhibitor therapy in stage I-III non-small cell lung cancer (NSCLC) found combination therapy produced a significant clinical benefit, as assessed by major pathologic response (MPR) rate, as well as enhanced tumor immune cell infiltration and immunological memory. Researchers from The University of Texas MD Anderson Cancer Center published the study results today in Nature Medicine.
The NEOSTAR trial tested combined neoadjuvant therapy of nivolumab plus ipilimumab, as well as neoadjuvant nivolumab monotherapy in patients with operable NSCLC. The trial met its prespecified primary endpoint efficacy threshold in the combination arm, with eight of 21 treated patients (38%) achieving major pathological response, defined as ≤10% viable tumor at surgery. MPR has been shown to correlate with improved survival outcomes after neoadjuvant chemotherapy in NSCLC. The prespecified efficacy boundary for each treatment to be considered promising for further testing was six or more MPRs in 21 evaluable patients. With MPR in five of 23 treated patients (22%), monotherapy did not meet the efficacy boundary.
While combination immunotherapy has been approved for a subset of patients with metastatic NSCLC, this is the first randomized study to report on the role of combination checkpoint inhibitors for operable, early stage disease.
“More than 50% of patients with localized non-small cell lung cancer will relapse if treated with surgery alone. Adding chemotherapy produces only a modest improvement in overall survival, and it comes with toxicity,” said Tina Cascone, MD., Ph.D., assistant professor of Thoracic/Head & Neck Medical Oncology and lead author of the study. “The results from our study with neoadjuvant combination immunotherapy are particularly encouraging in that we found that this dual treatment can induce higher pathologic responses and trigger immunological memory. This may translate into a reduced risk for tumor relapse in more patients with early stage non-small cell lung cancer.”
Study design and secondary endpoints
The Phase II single-institution study enrolled 44 patients with surgically resectable stage IA to IIIA NSCLC between June 2017 and November 2018. The median age of trial participants was 66 years old, and 64% were male. Participants were 84% white, 9% Black and 5% Asian. Most participants had a history of smoking: 23% identified as current smokers and 59% as former smokers.
Patients were randomized to one of two treatment arms with immune checkpoint inhibitors prior to surgery: 23 received three doses of nivolumab alone and 21 received three doses of nivolumab plus one dose of ipilimumab. Each arm was compared against historical controls of neoadjuvant chemotherapy. Overall, 41 patients completed the planned three doses of therapies, 37 patients had surgery on trial and two patients underwent surgery off trial after additional therapies.
Among the 37 patients who had surgical resection on the study, the combination arm showed higher MPR rates (50% versus 24%) and fewer viable tumor cells at resection than monotherapy (a median of 9% versus 50%). Combination therapy also showed better pathological complete response rates than monotherapy (38% versus 10%). After a median follow-up of 22 months, median overall survival and lung cancer-related recurrence-free survival were not reached.
Toxicities were manageable overall, with no new safety concerns compared to known adverse event profiles of either drug. The median time to surgery was 31 days after the last dose of nivolumab. Some patients experienced nodal immune flare (NIF), or the appearance of nodal disease progression on radiographic imaging, which invasive node biopsy revealed to be immune cell infiltration rather than malignant disease.
Exploratory analyses reveal immune impact, potential biomarkers
In an exploratory analysis of resected tissues, investigators found ― and reported for the first time ― higher levels of immune cell infiltration in tumors treated with combination therapy, including an abundance of CD3+ and CD3+CD8+ T lymphocytes, tissue-resident memory and effector memory T cells. Tumors that responded better to treatment had higher PD-L1 expression at baseline, but responses were also observed in those without PD-L1 expression in tumor cells.
The researchers analyzed the gut microbiome, as well, and found that pathologic response to combination therapy was associated with the presence of certain fecal microbes that also have been correlated with immunotherapy response in melanoma and other cancers. Immune checkpoint inhibitor therapy did not significantly affect the diversity or composition of the microbiome in this study.
“Our exploratory results suggest the gut microbiome may play a role in responses to neoadjuvant immune checkpoint inhibitors in lung cancer,” Cascone said. “The immune microenvironment findings also give us an opportunity to look at immune cell populations and potential biomarkers that can be evaluated in the future to identify those patients who are most likely to benefit from these agents in new prospective trials.”
The NEOSTAR trial has been amended to a modular platform design, which provides the opportunity to add treatment arms to rapidly test and advance promising new neoadjuvant therapeutic combinations. Results from a third arm testing neoadjuvant nivolumab plus chemotherapy are expected later this year. A fourth arm testing the combination of dual immunotherapy plus chemotherapy is ongoing.
“The NEOSTAR trial results set the stage for evaluating the role of dual immunotherapy added to neoadjuvant chemotherapy, which we are currently exploring, and expediting the investigation of novel agents in the perioperative setting,” Cascone said. “This is a population with potentially curable disease. We should do whatever it takes to minimize the risk of relapse and increase the cure rates for these patients.”
The NEOSTAR trial was supported by the Lung Cancer Moon Shot®, part of MD Anderson’s Moon Shots Program®, a collaborative effort designed to accelerate the development of scientific discoveries into clinical advances that save patients’ lives. Boris Sepesi, M.D., associate professor of Thoracic and Cardiovascular Surgery, served as co-principal investigator of the study. A full list of co-authors and author disclosures can be found in the paper.
Additional research support was provided by Bristol Myers Squibb, the National Institutes of Health/National Cancer Institute (5P50CA070907, P30 CA016672), the American Society of Clinical Oncology’s Conquer Cancer Foundation Career Development Award, the Connie Rasor Endowment for Cancer Research, the Bruton Endowed Chair in Tumor Biology, the Translation Molecular Profiling Immuno-profiling Laboratory, the MD Anderson Physician Scientist Program, the Khalifa Bin Zayed Al Nahyan Foundation, the Ford Petrin Donation, Rexanna’s Foundation for Fighting Lung Cancer and the Bob Mayberry Foundation.
Contact Us
Tina Cascone, M.D., Ph.D.
Thoracic Head & Neck Medical Oncology
MD Anderson Cancer Center
1515 Holcombe Blvd.
Houston, Texas 77030
TCascone@MDAnderson.org
Michelle Earnest
Administrative Contact
713-792-1256
Laboratory Contact
Room number: T8.3950
Phone: 713-792-1367 / 713-792-6363
Give Now
Research Areas
Find out about the four types of research taking place at UT MD Anderson.
