request an appointment online.
- Diagnosis & Treatment
- Cancer Types
- Hodgkin Lymphoma
Get details about our clinical trials that are currently enrolling patients.
View Clinical TrialsLymphoma is a general term for cancers that develop in the lymphatic system, a part of the body’s immune system. Hodgkin lymphoma usually starts in B lymphocytes, a type of immune system white blood cell.
Lymphoma is a general term for cancers that develop in the lymphatic system, a part of the body’s immune system. Hodgkin lymphoma usually starts in B lymphocytes, a type of immune system white blood cell.
Between 8,000 and 9,000 people are diagnosed with Hodgkin lymphoma in the United States each year and the disease is most frequently diagnosed among people between the ages of 20-34, according to data from the National Cancer Institute.
What are the parts of the lymphatic system?
The lymphatic system carries disease-fighting white blood cells throughout the body. It includes:
Lymph: Fluid that carries lymphocytes, a type of white blood cell, through the body in a network of lymph vessels, which are like tiny veins. Lymph helps fight against infection and cancer.
Lymph nodes: Tiny, bean-shaped masses found in several parts of the body, including in the underarm, pelvis, neck, abdomen and groin. They filter lymph and store white blood cells to help the body fight disease.
Spleen: An organ on the left side of the abdomen that helps lymphocytes develop, stores blood cells and gets rid of old blood cells.
Thymus: Located in the chest, this tiny organ helps make and develop lymphocytes.
Tonsils: Nodes in the back of the throat that store white blood cells.
Bone marrow: Material in bones that produces blood cells, including white blood cells.
Hodgkin lymphoma diagnoses have been trending down over the last decade and the survival rate is relatively high. The average five-year survival rate across all stages is close to 87%, with a survival rate of greater than 91% in cases confined to a single region (stage I).
Almost all Hodgkin lymphoma cases contain Reed-Sternberg cells, a specific type of large cancer cell that is not found in non-Hodgkin lymphomas. While Hodgkin lymphoma can start in the lymph nodes, it can spread to almost any organ or tissue, including the liver, bone marrow and spleen.
Hodgkin Lymphoma Types
Hodgkin lymphoma is divided into two major types according to how the lymph cells look under a microscope and whether Reed-Sternberg cells are present. Knowing the type of lymphoma helps doctors determine your best treatment.
Classic Hodgkin Lymphoma is the most common type in the United States. It accounts for about 95% of cases and is the most curable Hodgkin lymphoma. Subtypes include:
- Nodular Sclerosing Hodgkin Lymphoma: The affected lymph nodes have mixed areas of normal cells, Reed-Sternberg cells and prominent scar tissue. This is the most common type, making up 60% to 80% of cases. It is more common in adolescents and young adults, but it can occur atany age.
- Mixed Cellularity Hodgkin Lymphoma: The affected lymph nodes contain many Reed-Sternberg cells in addition to several other cell types. Mixed cellularity accounts for about 25% to 30% of cases of Hodgkin lymphoma. It primarily affects people with HIV, but also children and older adults.
- Lymphocyte-Rich Hodgkin Lymphoma: This recently created subtype in the past was sometimes confused with lymphocyte-predominant lymphoma. It is similar to mixed cellularity Hodgkin lymphoma.
- Lymphocyte Depletion Hodgkin Lymphoma: Large numbers of Reed-Sternberg cells, but very few other cell types, are found in the lymph nodes. This is the least common form of Hodgkin lymphoma, and it is seen more often in people who are elderly or have HIV.
Nodular Lymphocyte-Predominant Hodgkin Lymphoma: This rare disease accounts for just 5% of Hodgkin lymphoma diagnoses and is most common among men between age 35 and 40. Unlike other types of Hodgkin lymphoma, it produces no Reed-Sternberg cells. It is usually diagnosed at an early stage and has an excellent survival rate.
Hodgkin Lymphoma Risk Factors
Anything that increases your chance of getting Hodgkin lymphoma is a risk factor. Although Hodgkin lymphoma usually develops in people who have no risk factors, the following things may mean you are more likely to develop it:
- Age: Hodgkin lymphoma is most common in young adults (15 to 40 years old) and older adults (over 55 years old).
- Gender: Males are slightly more likely to develop Hodgkin lymphoma.
- Viruses: The risk is small, but some viruses may make you more likely to get Hodgkin lymphoma. These include:
- Epstein-Barr virus (EBV)
- Infectious mononucleosis (mono)
- Human immunodeficiency virus (HIV)
- Human T-cell lymphocytotropic virus (HTLV)
- Family history: If you have a parent, brother or sister with Hodgkin lymphoma, you have an increased risk of developing the disease.
Not everyone with risk factors gets Hodgkin lymphoma. However, if you have risk factors, you should discuss them with your doctor.
Learn more about Hodgkin lymphoma:
UT MD Anderson is #1 in Cancer Care
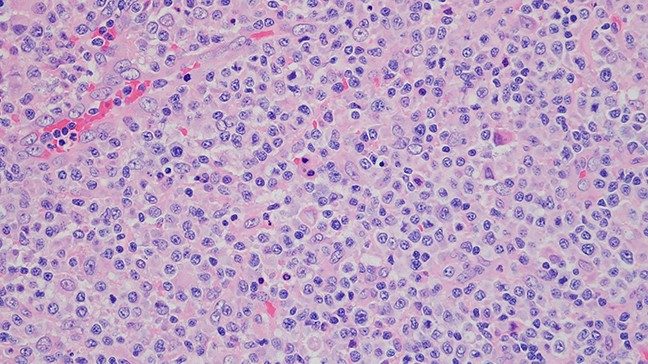
Understanding the different types of lymphoma
You may have already heard about non-Hodgkin lymphoma. But are there other kinds of lymphoma? What makes each one unique? And, are some symptoms common to all types of lymphoma?
We went to lymphoma specialist Ranjit Nair, M.D., for answers to these and other questions. Here’s what he shared.
What is lymphoma?
Because of its name, you might assume that lymphoma is a cancer of the lymph nodes. But lymphoma is actually a cancer of lymphocytes, which are a type of white blood cell. These white blood cells originate in the bone marrow. Once they mature, they are deployed to live and work within the lymphatic system — primarily the lymph nodes, spleen and thymus.
When a mature lymphocyte becomes cancerous, it tends to settle and multiply in the areas where it was designed to work. That’s why swollen lymph nodes are the most common symptom of lymphoma.
The name itself actually provides a road map of the disease: “lymph” refers to the fluid and system these cells inhabit, while the suffix, “-oma,” is the medical term for a swelling or tumor.
How many different types of lymphoma are there?
Many. But generally speaking, lymphomas are classified as either Hodgkin or non-Hodgkin. They were named in honor of Thomas Hodgkin, the 19th century British physician who first described these abnormalities in 1832. For a long time, any lymphoma that didn’t fit his specific description was simply classified as “non-Hodgkin.”
How is lymphoma broken down beyond those two categories?
Lymphoma is further categorized by the specific type of immune cell involved and its behavior. There are two main types of lymphocytes — B cells and T cells — so each cancer is classified accordingly.
- Hodgkin lymphoma is almost exclusively a B cell malignancy. It has four different subtypes.
- Non-Hodgkin lymphoma, however, is a mix of both B and T cell varieties. It serves as a much larger umbrella for approximately 140 different diseases.
B cell lymphomas are the most common, while T cell lymphomas are extremely rare. Despite the many varieties, though, lymphoma remains a rare disease. It makes up only about 4% to 5% of all new cancer diagnoses annually.
What are the most common types of lymphoma?
Lymphomas can be further described as either indolent (slow-growing) or aggressive (fast-growing).
The most common type of aggressive lymphoma is diffuse large B cell lymphoma, which actually includes 15 to 20 different genetic varieties. The most common indolent variety is follicular lymphoma.
Some of the rarer types include mantle cell lymphoma, marginal zone lymphoma, cutaneous T-cell lymphoma and double-hit lymphoma.
Why choose UT MD Anderson for your Hodgkin lymphoma treatment?
Our team of experts is one of the few focused only on lymphoma. While most oncologists see only one or two Hodgkin lymphoma patients a year, we treat hundreds annually, giving us a remarkable depth of experience and expertise.
At UT MD Anderson, you are cared for by a team of some of the nation's top authorities on lymphoma. They draw upon the latest and most-advanced treatments for all stages of Hodgkin lymphoma, examining you carefully to determine the best approach and communicating every step of the way.
Innovative, Advanced Options
As one of the world's leaders in lymphoma advances, we constantly work to pioneer new treatments that are effective and have the least impact on your body. For instance, UT MD Anderson has helped advance the development of several new targeted therapies for Hodgkin lymphoma. And we are studying several biomarkers to guide the future development of even more personalized therapies.
Whether you recently have been diagnosed with Hodgkin lymphoma or have battled the disease for years, we can help.
Become an expert on your disease. Be able to verbalize it to your providers and don't take 'no' for an answer when they tell you nothing's wrong. Keep going until you find someone who will listen.
Kimberly Hill
Survivor
Treatment at UT MD Anderson
Featured Articles

Hodgkin lymphoma, leukemia survivor: Targeted therapy clinical trial put me in remission

Stage IV Hodgkin lymphoma survivor: An immunotherapy clinical trial put me in remission
Hodgkin vs. non-Hodgkin lymphoma: What’s the difference?

Cancer treatment during the COVID-19 pandemic: FaceTime keeps couple connected

How MD Anderson exceeded my expectations
Clinical Trials
UT MD Anderson patients have access to clinical trials offering promising new treatments that cannot be found anywhere else.
Becoming Our Patient
Get information on patient appointments, insurance and billing, and directions to and around UT MD Anderson.
myCancerConnection
Talk to someone who shares your cancer diagnosis and be matched with a survivor.
Prevention & Screening
Many cancers can be prevented with lifestyle changes and regular screening.
Counseling
UT MD Anderson has licensed social workers to help patients and their loved ones cope with cancer.
Help #EndCancer
Give Now
Donate Blood
Our patients depend on blood and platelet donations.
Shop UT MD Anderson
Show your support for our mission through branded merchandise.
