request an appointment online.
- Diagnosis & Treatment
- Cancer Types
- Non-Hodgkin Lymphoma
Get details about our clinical trials that are currently enrolling patients.
View Clinical TrialsLymphoma is a general term for cancers that develop in the lymphatic system, which is part of the body’s immune system. Non-Hodgkin lymphoma can start from multiple types of lymphocytes (a kind of white blood cell), including B and T lymphocytes.
Lymphoma is a general term for cancers that develop in the lymphatic system, which is part of the body’s immune system. Non-Hodgkin lymphoma can start from multiple types of lymphocytes (a kind of white blood cell), including B and T lymphocytes.
They may start in the bone marrow, spleen, thymus or lymph nodes and spread to other parts of the body.
Non-Hodgkin lymphoma is the seventh most common cancer in men and women in the nation. According to the National Cancer Institute, more than 77,000 new cases of non-Hodgkin lymphoma are diagnosed each year in the United States.
With early diagnosis and advanced treatment methods, non-Hodgkin lymphoma has a high survival rate. If the cancer is confined to a single region, it has about an 83% survival rate. Even the most advanced stage of non-Hodgkin lymphoma has a survival rate greater than 60%.
What are the parts of the lymphatic system?
The lymphatic system carries disease-fighting white blood cells throughout the body. It includes:
Lymph: Fluid that carries lymphocytes, a type of white blood cell, through the body in a network of lymph vessels, which are like tiny veins. Lymph helps fight against infection and cancer.
Lymph nodes: Tiny, bean-shaped masses found in several parts of the body, including in the underarm, pelvis, neck, abdomen and groin. They filter lymph and store white blood cells to help the body fight disease.
Spleen: An organ on the left side of the abdomen that helps lymphocytes develop, stores blood cells and gets rid of old blood cells.
Thymus: Located in the chest, this tiny organ helps make and develop lymphocytes.
Tonsils: Nodes in the back of the throat that store white blood cells.
Bone marrow: Material in bones that produces blood cells, including white blood cells.
UT MD Anderson is #1 in Cancer Care
Non-Hodgkin Lymphoma Types
B-cell lymphoma
B-cell lymphoma is the most common type of non-Hodgkin lymphoma and makes up 85% of Non-Hodgkin lymphoma cases. Learn about the types of B-cell lymphoma.
T-cell lymphoma
Precursor T-lymphoblastic lymphoma/leukemia
This extremely rare type of lymphoma can either be considered a form of acute lymphoblastic leukemia (ALL) or lymphoma, depending on the amount of bone marrow involvement. This disease tends to start behind the breastbone, in front of the heart. It can grow into a large tumor in the chest that can cause difficulty breathing. It is typically treated with chemotherapy.
Peripheral T-cell lymphomas
The lymphomas in this group are all rare and are derived from mature T-cells.
Cutaneous T-cell lymphomas (CTCL)
These are lymphomas of the skin, and topical therapy may be used as an initial treatment. There may be simultaneous or progressive involvement of blood or lymph nodes. CTCL is treated in the Cutaenous T-cell Lymphoma Clinic.
Adult T-cell leukemia/lymphoma
This lymphoma is directly related to infection with HTLV-1 virus and is mostly limited to countries where that virus is more common, such as the Caribbean, Japan and parts of Africa. It’s rare in the U.S.
Angioimmunoblastic T-cell lymphoma
This type of T-cell lymphoma makes up roughly 4% of all lymphomas. It involves the lymph nodes and liver or spleen. It can cause fever, skin rashes, weight loss and infection. It progresses quickly and often recurs.
Extranodal natural killer/T-cell lymphoma
This disease is usually found in the nose and upper throat, but can attack the skin and other organs. It’s more heavily concentrated in South America and parts of Asia.
Enteropathy-associated intestinal T-cell lymphoma (EATL)
This is a type of lymphoma found in the lining of the digestive tract and can cause abdominal pain, nausea and vomiting. It can occur in the colon, but is more common in the small intestine. Two subtypes exist:
- Type 1 EATL – This subtype can occur in people with celiac disease – an auto-immune disease that causes gluten consumption to prompt the body’s immune system to attack the intestinal lining. It’s more common in people with adult-onset celiac disease.
- Type II EATL – This type is less common, with no link to celiac disease.
Anaplastic large cell lymphoma (ALCL)
This is a fast-growing T-cell lymphoma. It occurs more often in young people than adults and accounts for about 2% of lymphomas. It is categorized by subtype.
- Primary cutaneous ALCL – This subtype only affects skin.
- Systemic ALCL – This can affect the skin, as well as other organs. It is further categorized based on whether there is a change in the ALK gene. ALK-positive trends younger and carries a more favorable prognosis than ALK-negative.
- Implant-associated ALCL – This is a rare lymphoma that develops in the breasts of people who have had implants. Smooth, as opposed to textured, implant surfaces carry a reduced risk. Learn more about implant-associated ALCL.
Peripheral T-cell lymphomas, not otherwise specified
This is a catch-all term for T-cell lymphomas that don’t fit into the other categories. These lymphomas can involve the digestive tract, spleen, liver, skin and bone marrow, but often involve lymph nodes. They are more likely to be found in patients in their 60s. They are generally widespread, fast-growing and over time become difficult to treat even after initially responding well to treatment.
Non-Hodgkin lymphoma is classified also by how quickly it spreads.
Low-grade non-Hodgkin lymphoma includes:
- Marginal zone lymphoma
- Mucosa-associated lymphoid tissue (MALT) lymphoma
- Follicular lymphoma
- Mantle cell lymphoma
Intermediate grade non-Hodgkin lymphoma includes:
- Diffuse large cell lymphoma
- Primary mediastinal large cell lymphoma
- Anaplastic large cell lymphoma
High-grade non-Hodgkin lymphoma includes:
- Burkitt’s lymphoma
- Lymphoblastic lymphoma
Relapsed non-Hodgkin lymphoma is disease that comes back after you have been successfully treated for Non-Hodgkin lymphoma.
Refractory non-Hodgkin lymphoma is new or relapsed disease that does not respond to treatment.
Non-Hodgkin Lymphoma Risk Factors
Anything that increases your chance of getting non-Hodgkin lymphoma is a risk factor. Although scientists don’t know yet what causes non-Hodgkin lymphoma, some factors seem to make you more likely to develop non-Hodgkin lymphoma. These include:
- Gender: Non-Hodgkin lymphoma is slightly more common in men
- Race: Non-Hodgkin lymphoma is slightly more common in Caucasians
- Living in a farming community. Some studies suggest that certain herbicides and pesticides may play a part in lymphoma, but this has not been proven
- Bacteria or viruses, including human immunodeficiency virus (HIV), Epstein-Barr virus (EBV), human T-lymphotropic virus (HTLV) and the bacterium Helicobacter pylori
- Hereditary cancer syndromes
Not everyone with risk factors gets non-Hodgkin lymphoma. However, if you have risk factors, you should discuss them with your doctor.
Learn more about non-Hodgkin lymphoma:
In rare cases, non-Hodgkin lymphoma can be passed down from one generation to the next. Genetic counseling may be right for you. Visit our genetic testing page to learn more.
Why choose UT MD Anderson for non-Hodgkin lymphoma treatment?
At UT MD Anderson's Lymphoma and Myeloma Center, our goal is to treat non-Hodgkin lymphoma with methods that are strong on the disease, but as gentle as possible on your body.
Our Lymphoma and Myeloma Center handles more than 35,000 patient visits each year, placing UT MD Anderson among the nation’s most active and experienced programs. Our doctors, nurses, and advanced practice providers are focused and specialize only in lymphoma or myeloma.
Drawing upon a wide range of treatments for every stage of disease, and clinical trials of novel agents, our physicians design a treatment plan that is uniquely yours. We're constantly working to bring new treatments to patients, including targeted biological agents that help your body fight the cancer.
Through our wide range of over 100 clinical trials, we have access to many treatments that are not available other places. Many of these are treatments that our experts developed or led.
For many patients with non-Hodgkin lymphoma, the goal of treatment is cure – to completely wipe out the disease so that it never comes back. For other patients, the most effective course is to keep knocking back the disease over a period of many years. In these cases, personalized long-term care plans are especially important. In these situations, in addition to thinking about what to do to treat the cancer now, it is important to also think about what to do next and what other things to consider long-term.
Our multidisciplinary approach brings together teams of specialized physicians, nurses, physician assistants, dietitians, social workers and many others, who work closely together – and with you – to improve your chances for successful treatment.
Groundbreaking Research
UT MD Anderson has helped advance the treatment of non-Hodgkin lymphoma in many areas, including development of new, leading-edge treatments. And we continue to research ways to improve your health and quality of life.
At UT MD Anderson's Lymphoma and Myeloma Center, you benefit from one of the most active research programs in the United States. This means we are able to offer a wide range of clinical trials (research studies) for every type and stage of non-Hodgkin lymphoma.
Life is beautiful. I am drinking it all in and savoring every little sip.
Jennifer Ponce
Survivor
Treatment at UT MD Anderson
Featured Articles
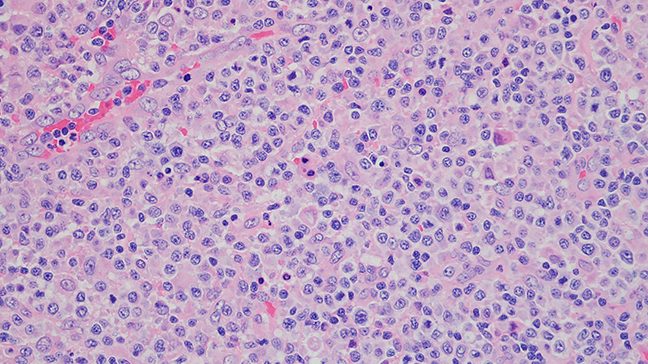
Understanding the different types of lymphoma

Stage IV non-Hodgkin lymphoma survivor: Why I’m excited about UT MD Anderson coming to Austin

CAR NK cell therapy clinical trial puts follicular lymphoma survivor into remission

Non-Hodgkin lymphoma survivor thankful for clinical trial
What is MALT lymphoma? 6 things to know
Central nervous system (CNS) lymphoma: What you need to know

Double-hit lymphoma survivor: ‘If I hadn’t gone to MD Anderson, I wouldn’t be here’
Clinical Trials
UT MD Anderson patients have access to clinical trials offering promising new treatments that cannot be found anywhere else.
Becoming Our Patient
Get information on patient appointments, insurance and billing, and directions to and around UT MD Anderson.
myCancerConnection
Talk to someone who shares your cancer diagnosis and be matched with a survivor.
Prevention & Screening
Many cancers can be prevented with lifestyle changes and regular screening.
Counseling
UT MD Anderson has licensed social workers to help patients and their loved ones cope with cancer.
Help #EndCancer
Give Now
Donate Blood
Our patients depend on blood and platelet donations.
Shop UT MD Anderson
Show your support for our mission through branded merchandise.
