News
Featured Articles
Our experts share the work of IDSO and the advanced, data-driven approaches to cancer care and research.

3 things to know about AI and cancer care
Artificial intelligence (AI) has the potential to shape nearly every aspect of our lives – including cancer care. At UT MD Anderson, we see the opportunities and risks associated with the emergence of AI and an ever-increasing amount of data being generated by our cancer research, patient care and clinical operations.
“AI has promise to improve outcomes and experiences for our patients,” says Caroline Chung, M.D. “However, simply enabling AI capabilities within a technology or workflow because they are available will not necessarily drive to impact and is not our approach. We are focused on utilizing the right data-driven decision-making across all our mission areas.”
As a clinician-scientist and co-director of UT MD Anderson’s Institute for Data Science in Oncology, Chung is an active voice within AI communities and consortia that span federal institutions, academic organizations and industry partners. She’s active in National Institutes of Health (NIH) AI workshops and leads the AI Community of Practice for ASCO, among others.
Here, Chung shares how our expert clinicians, scientists and technology teams are guiding UT MD Anderson’s approach to AI and what’s on the horizon for our patients.
Data quality determines impact
“If you drive a luxury sports car with a powerful engine and you fill up the tank with regular gasoline instead of premium, your car’s performance will be subpar and over time you’ll damage the engine,” says Chung. “The same goes for the data that is used to fuel AI systems and models.”
AI technology solutions learn patterns and make predictions based on processing and analyzing large amounts of data. To ensure that the data UT MD Anderson uses will yield good results when coupled with AI, Chung has steered the organization to focus on laying foundational elements and governance approaches.
“What we can accomplish with AI depends upon data quality – ensuring that when data is captured it has the appropriate context and metadata, can be found easily and understood so that it is appropriately used,” says Chung. “We also acknowledge that not all data is useful for all purposes. To get answers for important questions, we must consider the context and focus on the most opportune and useful data for development and implementation of solutions.”
Chung ensures teams across UT MD Anderson contribute to a data ecosystem that encompasses not only data but also technologies, processes, policies, culture and people. This holistic approach leads to collaboration and connectivity — from data generation through to clinical impact — avoiding siloed clusters of data and ensuring we can unlock the power of complex information to advance our mission to end cancer.
We’re guided by impactful questions to yield meaningful changes
As a professor in Radiation Oncology and Diagnostic Imaging with a clinical practice focused on central nervous system malignancies and a computational imaging lab focused on quantitative imaging and modeling to detect and characterize tumors and toxicities of treatment, Chung regularly leverages AI-based technology to enable personalized cancer treatment.
“Across UT MD Anderson we are evaluating uses for AI with the aim of driving greater efficiencies, novel insights and where we can make the most impact,” says Chung. “Rather than asking what can we do with AI, we are critically asking if AI is an effective solution to the particular prioritized goal – considering the teams involved, processes, data and technology.”
AI is a broad umbrella term that covers different approaches of using computer science and data to enable problem-solving in machines, such as:
- generative AI
- deep learning
- natural language processing
- predictive analytics
- data algorithms
At UT MD Anderson, our interdisciplinary teams across Technology, Data and Innovation, clinical operations, research, and patient care are using all of these to potentially develop at-scale solutions for patients and clinical providers. Questions we’re trying to answer using AI include:
How can we lessen physicians’ administrative burden so they can spend more 1-on-1 time with patients and less time in front of a computer screen?
An ambient listening pilot aims to relieve administrative burden by using generative AI to capture discussions between providers and patients to chart and document outpatient visits with notes in patients’ electronic health records.
How can we reduce patient falls, the most commonly reported patient safety incident in acute hospital settings, according to the NIH?
A predictive analytics tool is in development to identify our most at-risk patients based on a host of health factors to support operational and clinical decision-making and ultimately lessen the potential for patient falls to occur.
How can we share our clinical expertise in radiation therapy – a core treatment option for many cancer patients – with underserved countries?
Our teams have developed novel deep learning technologies to bring UT MD Anderson’s expertise to communities who could benefit from our standards of care but are unable to access them due to distance and a lack of resources.
As one of the largest providers of oncology clinical trials, how can we connect patients more efficiently with options tailored to their unique diagnoses?
By using natural language processing, automatic review of specific provider notes and other data in our electronic health record system, we seek to expedite patient matches and enrollment in relevant clinical trials.
With more than 15,000 surgical cases manually scheduled each year, how can we address inefficiencies that can lead to delays in care?
Novel algorithms are in development to accurately predict surgery length and time spent in outpatient care. The goal is to yield more efficient surgical workflows and reduce patient wait times.
Ensuring safe and responsible use is imperative
“With the promise of AI solutions to impact clinical decisions and the use of patient data, coupled with an evolving regulatory landscape, we are choosing to establish a strong foundational approach to AI that assures it will positively impact our patients, our team members and our mission,” says Chung. “There is no quick route or shortcut.”
Make no mistake: there is a sense of urgency to leverage AI. At UT MD Anderson, we’re balancing this excitement for the future with a safe, sustainable, ethical, value-based and risk-managed approach to protect patient data and avoid bias. And with this emergence, the role of human decision-making and how humans interact with this technology to understand, validate and verify results is a critical aspect.
“As a leader in cancer care and research, we have the responsibility to harness AI’s potential to make an impact on quality of care, patient safety, research and streamlined operational processes,” says Chung. “This is an exciting time and it’s only the beginning.”
Learn about UT MD Anderson’s Institute for Data Science in Oncology.
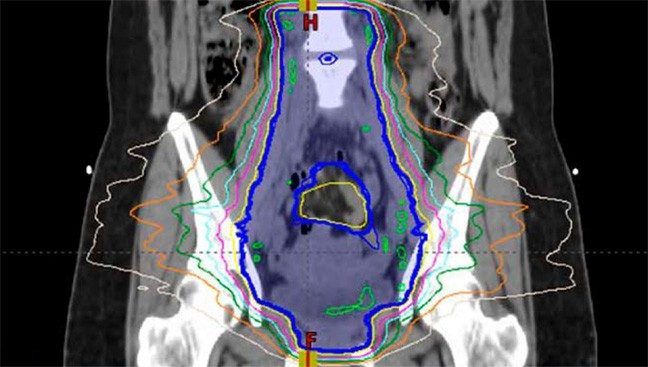
Radiation Planning Assistant: Delivering on the promise of AI
Adoption of radiation therapy technology has increased around the world to the point that access to the technology itself is often no longer the main barrier for many patients to receive care. Instead, it's the lack of qualified specialists available to do the treatment planning.
Planning is a multi-step process where clinicians analyze medical images to design a personalized radiation treatment plan that includes where the radiation is targeted, specific areas to avoid targeting and how much radiation will be delivered. The more complicated the case, the longer this process can take.
For many cases, however, the process is relatively routine. This makes radiation planning an ideal process for artificial intelligence (AI) to assist.
That’s the goal of the Radiation Planning Assistant, a web-based AI tool developed by Laurence Court, Ph.D., that launched earlier this year and aims to streamline radiation planning for clinics around the world.
AI saves time in treatment planning
The International Atomic Energy Agency recommends one oncologist for every 250 to 300 patients. To reach that number, the world would need tens of thousands of new graduates in a field that is so highly specialized most programs only produce a handful each year.
“Many areas have one or two consultants for several thousand patients,” Court says. “Doing things the traditional way is just not feasible.”
But unlike many fields where the lofty promises of AI have far outpaced its actual current capabilities, processing medical images is an area that AI has already proven valuable.
“This is something that AI is very good at,” Court says. “The algorithms we have developed can quickly take CT scans and develop very accurate treatment plans so that all the clinic has to do is review the plans and sometimes make minor changes instead of developing entirely new plans for each patient.”
To use the platform, clinicians upload a CT scan and complete a service request form, the deidentified data is then uploaded to the Radiation Planning Assistant servers. For complex cases, the system first does the contouring plan, which is then reviewed and finalized by the clinician before the system delivers the final treatment plan. For simpler cases, the plan is automatically created without this step. Once the plan is sent back to the clinician, they recalculate the dosages and make any necessary edits before the plan is utilized in the clinic.
After receiving clearance from the Food and Drug Administration (FDA) in 2023, the team launched the Radiation Planning Assistant earlier this summer. It has already been used to develop plans for patients being treated in clinics in South Africa, and other clinics are in the process of being added.
AI as an assistant, not a replacement
Court stresses that the Radiation Planning Assistant, as the name indicates, assists in the process. It can’t replace the experience and expertise the clinicians have.
Alicia Sherriff, M.D., head of oncology at the University of the Free State in Bloemfontein, South Africa, has been involved with the development and launch of the Radiation Planning Assistant.
While her clinic is a leading oncology program in the region, her staff still faces issues of limited resources, namely time.
“The Radiation Assistant Platform allows us to focus on refining the plans and gives us the capacity to spend our time more appropriately in clinical service delivery, teaching, training and to be more involved in the complex cases in our departments and multi-disciplinary meetings,” Sherriff says. “It also allows our team to add to our research capacity.”
Improving radiation therapy access around the world
Similar platforms are already in use at MD Anderson and other cancer centers but can be prohibitively expensive and often require trained specialists. Court and his collaborators developed the Radiation Planning Assistant to be affordable and easy to use.
According to him, the platform can create more than 100,000 radiation therapy plans per year at a cost of around $10 per patient. MD Anderson intends to offer the service for free to clinics in other countries who would otherwise not be able to afford commercial solutions.
“This has been a multi-year process, so our team was beyond excited when the first person was treated with a plan developed by the Radiation Planning Assistant earlier this year,” Court says. “Now our focus is on expanding access to the platform in other parts of the world.”
The Radiation Planning Assistant will be the focus of multiple presentations at the 2024 American Society for Radiation Oncology (ASTRO) Annual Meeting, including an educational presentation by Court on strategies for adopting AI in resource-limited settings. He is also a senior author on two posters that will present data on treatment planning workflow and CT simulator downtime gathered since the initial launch in South Africa.
Court is an affiliate of MD Anderson's Institute for Data Science in Oncology (IDSO), which assisted in the development of the Radiation Planning Assistant by helping lay the groundwork for data access and information infrastructure, accelerating high-impact projects like this one while ensuring they meet MD Anderson's high-quality standards for patient care.
Request an appointment at MD Anderson online or call 1-877-632-6789.

What does a data scientist do?
Theoretically, anyone who analyzes data to do science could call themselves a data scientist. But to me, that term also implies the use of computers. So, it’s data plus computers that makes someone a data scientist in my mind.
I also tend to apply a slightly narrower definition: I think of a data scientist as someone who’s concerned with deriving hidden knowledge from data trends and then making predictions based upon them.
To accomplish those goals, you need two things. The first is the ability to handle, organize, standardize, label, test, move and make data amenable to analysis. The second is the ability to make predictions based on that data, and to develop the artificial intelligence (AI) tools needed to analyze it, learn from it and evolve as an organization.
What makes a good data scientist?
You don’t have to be an oncologist to be a good data scientist. In fact, very few data scientists at MD Anderson come from an oncology background. My team consists of everything from astrophysicists to shopping website analysts. But many of their skillsets are completely transferrable, so I am thrilled to have their talents here.
I didn’t even study oncology myself — just pure computer science and molecular biology. I applied data science to drug discovery when I started out in the biotech industry. It wasn’t until I became junior faculty in academia that I started developing the oncology knowledge I use today.
It’s easy to fall into the trap of thinking you’re poised for success in the field of data science, just because you’ve gotten some training on the most recent technologies. But the tools being used today are very different from the tools that will be used two years from now. So, if all you know how to do is push buttons on the latest fad, you’re going to get lost straightaway.
To be a good data scientist, you’ve got to have a good grasp of the fundamentals of math and computer science — and a really solid understanding of the underlying methodologies to identify trends and make predictions. You’ve also got to understand the limitations of any tools you’re using and how to design questions to make sure your experiment is both unbiased and testing the actual hypothesis.
“Bilingual” people who can “speak” both oncology and data science — and take complex biological problems and translate them into computational questions — are what I call “translational” data scientists. That’s what I consider myself. And that’s what I try to help each of my new team members to become, if they’re not one already.
How MD Anderson is harnessing the power of data
As a drug discovery scientist trained in molecular biology, I’ve always been fascinated by the idea of doing things at scale. Bringing all the data together and identifying hidden patterns in it that no one else can see — then using those insights to inform drug discovery efforts — is much more satisfying to me than trying to find the answers to very specific questions. But we need both types of science to advance medicine, of course.
I just love the process of drug discovery. It brings together experts from so many different disciplines, including genomics, physics and chemistry, to name a few. It’s a really complex field.
It’s also exciting to be exploring drug discovery here at MD Anderson, where I get to work with people like Andy Futreal, Ph.D., who is leading initiatives to collect data and profile patients in really meaningful ways; and with Tim Heffernan, Ph.D. ,who is leading our Therapeutics Discovery teams to explore new ideas through experiments that lead to the development of new drugs.
MD Anderson already has so many phenomenal initiatives— like the Patient Mosaic™ — that don’t exist anywhere else. All that was lacking was a cohesive way to harness its collective data to effectively drive our decision-making. That’s why I was recruited: to develop a kind of “information superhighway” that sits right in the middle, allowing a continuous feedback loop to keep us all on track.
Although it’s still early, we have already been able to harness knowledge from our rare tumor patient samples and identify potential “Achilles heels” genes using our cutting-edge AI methods. We then demonstrated these genes’ importance using our Therapeutics Discovery's translational biology expertise, and we are moving them to the drug discovery stage. This shows how MD Anderson’s unique capabilities enable us to quickly change the way we make advances that benefit patients.
As a co-lead for Computational Modeling for Precision Medicine in our Institute for Data Science in Oncology (IDSO), I’m spearheading that initiative with the Adaptive AI-Augmented Drug Discovery and Development program, “A3D3a.” I contrived the name deliberately so that we could call it “Ada.” It’s a tribute to one of my heroes, Ada Lovelace, the world’s first computer programmer.
The daughter of British aristocrat and Romantic poet Lord Byron, Lovelace worked with inventor Charles Babbage on machines that could make calculations at great scale. Then one day, she said to him, “Why don’t we make a machine that can be programmed to do whatever calculation we want it to?” She wrote the first computer program and with that, the era of computer programming was born.
Why I joined MD Anderson
The collective brain power at MD Anderson is truly unequaled. It simply doesn’t exist anywhere else. Neither does the ability to make advances benefit patients more quickly. That’s why I believe MD Anderson is the only place on the planet where we can do this. But to be successful, our work needs to start and end with the patient. That means:
- coming up with each hypothesis based on the existing patient data
- validating it in an experimental setting relevant to patients
- taking it to the preclinical and clinical trial stages in our own hospital
- bringing it to our patients at the bedside and in the clinic, and
- using the feedback generated by that process to refine any new drug therapy or patient care practices.
For me, personally, that also means developing algorithms to help us learn more about cancer, and uncovering new information that can further refine our decision-making processes. Using AI to inform each and every one of the thousands of decisions our faculty and staff make each day is what I’ve dedicated my career to — and precisely why I joined MD Anderson.
A lot of drugs that get approved to treat cancer today are considered “me, too” drugs. This means they ride the coattails of the ones that came before them. But when you see a brand-new drug that you helped develop enter a Phase I clinical trial to be tested for the first time — and you know that it will soon start directly benefiting patients — it really is the most exciting thing in the world. That’s where I get my buzz every morning, and it’s my favorite part of the job.
It’s too soon for anything I’ve been working on here to be entering Phase I clinical trials yet. But by applying data science, we’ve already identified several targets for potential therapy development in very rare cancers, such as metastatic uveal melanoma, which is really difficult. And that’s exactly the kind of thing we can only do at MD Anderson, because you need all the unique components of the entire pathway in one spot.
Now, with the help of AI knowledge bases like the CanSAR platform I created, we’ll soon be able to make drug discoveries that even places like MD Anderson couldn’t possibly have made on their own.
Related Articles and News
MD Anderson News Releases
-
MD Anderson’s Institute for Data Science in Oncology establishes internal advisory council to maximize impact
June 2024
-
MD Anderson’s Institute for Data Science in Oncology announces appointment of inaugural IDSO Affiliates
March 2024
-
MD Anderson, TACC and the Oden Institute announce funding for the next round of collaborative cancer research projects
December 2023
-
Collaboration on Data and Computational Sciences Announces Next Round of Projects to Advance Cancer Breakthroughs
November 2021
-
MD Anderson advances data collaboration through technology agreement with Syntropy
April 2021
-
MD Anderson and UT Austin collaboration to end cancer welcomed enthusiastically by state and federal stakeholders
November 2020
Articles
-
"Cancer Needs a robust 'metadata supply chain' to realize the promise of artificial intelligence"
Elsevier Pure
-

"35 chief digital officers of health systems to know | 2022"
Becker's Hospital Review
-

"MD Anderson researchers harness AI to transform cancer care"
NVIDIA
-
"MD Anderson launches $100M data science institute"
Becker's Hospital Review
-
"MD Anderson names first chief data officer"
Modern Healthcare
-
52 hospitals and health systems with great innovation programs | 2024
-
"Realizing the power of data science to advance cancer research and cancer care"
MD Anderson (Cancerwise)
-
Advancing cancer surgery through data science
MD Anderson (Cancerwise)
MD Anderson News
The MD Anderson Newsroom provides information about studies and findings from our cancer researchers.
Give Now
Research Areas
Find out about the four types of research taking place at UT MD Anderson.