Research
Research efforts in the Fuller Lab have resulted in several contributions to science, specifically in the fields of image registration, segmentation, quality assurance, radiation planning margin assessment for radiotherapy planning purposes, radiotherapy-associated toxicity, patterns of failures, and clinical outcomes assessment, as well as imaging biomarker development. These efforts were essential to develop all the imaging component framework and workflow process in multiple head and neck cancer clinical and translational studies. We produced a series of projects related to benchmarking and quality improvement of manual, automated and semi-automated image acquisition processes for head and neck cancers. This work has served to define novel practices in image-guided radiotherapy, as well as investigation of innovative MRI imaging methods for radiation therapy, such as intravoxel incoherent motion (IVIM) for oropharyngeal cancers.
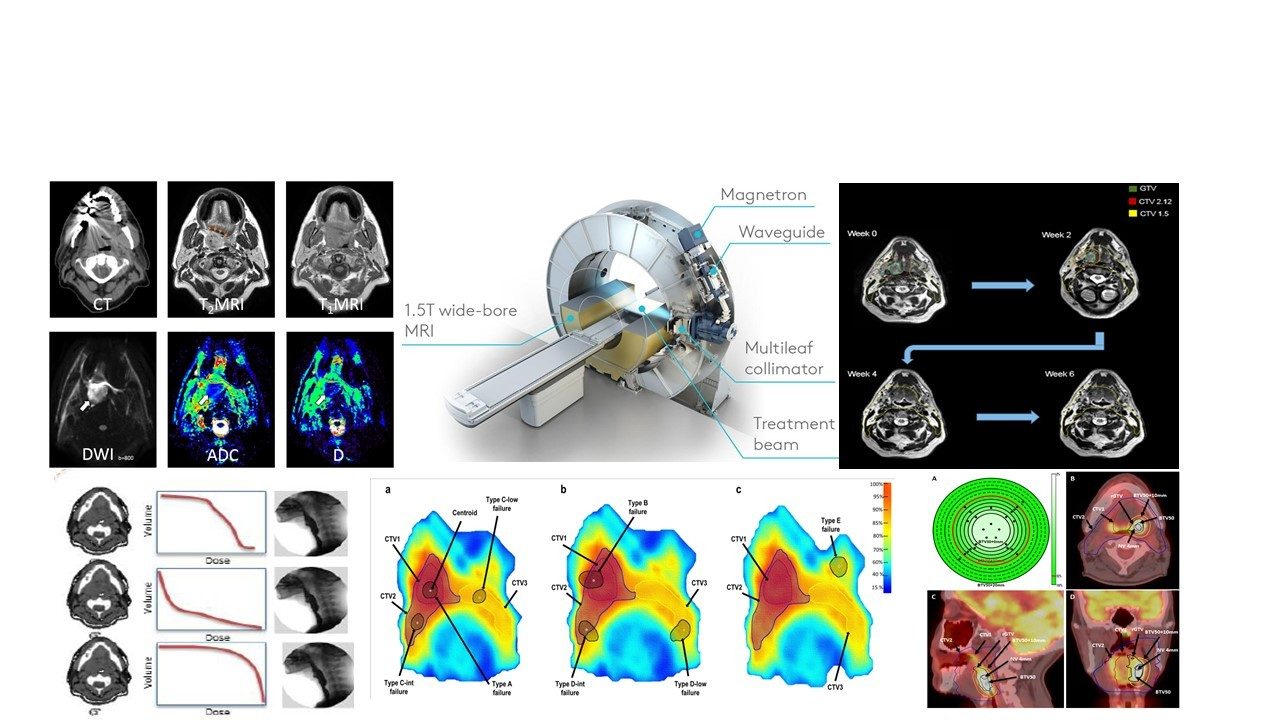
To track longitudinal quantitative changes in imaging parameters in relation to dosimetric parameters on a three-dimensional voxel-wise level, automated frameworks that rely on deformable image registration (DIR) are of paramount importance. We have developed a quality assurance framework to assess different image registration algorithms and software. I also played a critical role in the development of protocols to reduce motion-induced MR artifacts, thereby improving positional variance for RT applications. The expertise we have acquired in imaging analytics was necessary for imaging biomarkers development and validation. These biomarkers allow to stratify cancer patients for dose adaptation at simulation, and mid-treatment. IVIM data may have translational applications in adaptive treatment planning, prediction of outcome and monitoring of treatment response.
We have, in addition, significant contribution in the characterization of IMRT-induced normal tissue toxicity, impact on quality of life, as well as the role of MRI as a biomarker for toxicity prediction. We have published a series of articles that characterized IMRT beam path toxicity, particularly dose-response relationship between; brain stem centers and radiation-associated nausea and vomiting, swallowing muscles and chronic radiation- associated dysphagia. We also actively investigating dose-MRI parameter response kinetics. In one study, we showed that serial MRI acquisitions enable the identification of both early and late radiation-induced changes in swallowing structures after definitive IMRT. More recently, we characterized dynamic contrast-enhanced MRI (DCE-MRI) derived parameters changes in healthy muscles before, during, and after chemoradiation.
We are studying the nature history of osteoradionecrosis and the role of DCE-MRI as a biomarker to predict this morbidity as follows. These efforts were key preliminary data for successful NIH/NIDCR R01 application (1R56DE025248-01). We have been also involved in several projects and protocols related to the development of MRI-Linear Accelerator devise at MD Anderson. Additionally, we have played a major role of a multi-institutional projects for integration of imaging, demographic, clinical, and outcome data to create spatial-nonspatial multidimensional “Big-data” based treatment decision tools.
Give Now
Research Areas
Find out about the four types of research taking place at UT MD Anderson.
