request an appointment online.
- Diagnosis & Treatment
- Cancer Types
- Melanoma
Get details about our clinical trials that are currently enrolling patients.
View Clinical TrialsMelanoma is a skin cancer that starts in melanocytes (cells that make melanin), which give skin its pigment, or color. Sometimes these cells change, often because of damage caused by sun exposure. Over time, this damage may result in cancer.
Melanoma is a skin cancer that starts in melanocytes (cells that make melanin), which give skin its pigment, or color. Sometimes these cells change, often because of damage caused by sun exposure. Over time, this damage may result in cancer.
While melanoma accounts for only 3% of all types of the skin cancer, it has the highest death rate of all types and is more likely to spread (metastasize) in the body. It is also one of the most frequently occurring cancers in young adults ages 20 to 30, and is the main cause of cancer death in women 25 to 30 years old.
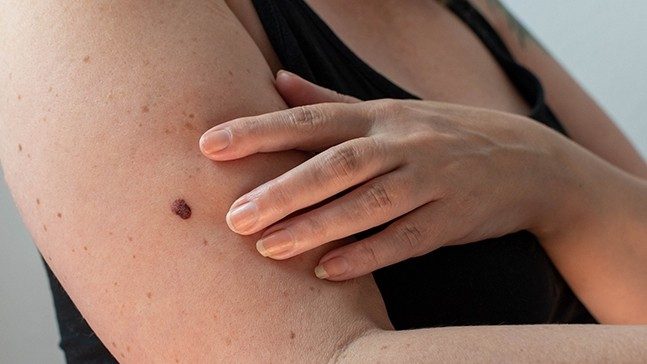
Melanoma usually appears as an:
- Irregular brown, black and/or red spot or
- Existing mole that begins to change color, size or shape
Melanoma appears most commonly on the trunk area in fair-skinned men and on the lower legs in fair-skinned women. In dark-skinned people, melanoma appears most frequently on the palms, the soles of the feet and the skin under nails. If caught early, melanoma is often curable.
Melanoma Types
Melanoma typically falls into one of the following three types:
- Cutaneous melanoma
- Mucosal melanoma
- Ocular melanoma
Cutaneous Melanoma
There are four major types of cutaneous melanoma:
Superficial spreading melanoma:
- Most common melanoma type
- About 70% of cases
- Usually starts in a pre-existing mole
Nodular melanoma:
- Second most common melanoma type
- 15% to 30% of cases
- More aggressive and usually develops quicker than superficial spreading melanomas
Lentigo maligna melanoma:
- Appears as large, flat lesions
- Most commonly found on the faces of light-skinned women over 50
- 4% to 10% of cases
- Lower risk of spreading than other melanoma types
Acral lentiginous melanoma:
- Occurs on the palms, soles of the feet or beneath the nail beds
- 2% to 8% of melanomas in fair-skinned patients
- Up to 60% of melanomas in darker-skinned patients
- Large, with an average diameter of 3 centimeters
Mucosal Melanoma
- About 1% of melanoma cases
- Occurs in mucosal tissue, which lines body cavities and hollow organs
- Most common sites are head and neck region (including the nasal cavity, mouth and esophagus), rectum, urinary tract and vagina
- Can be very difficult to detect
- Even when diagnosed and treated, prognosis is often poor
Ocular Melanoma
Because the eyes contain melanocytes, they can be susceptible to melanoma. Read more about the two types of ocular melanoma:
Some cases of melanoma can be passed down from one generation to the next. Genetic counseling may be right for you. Learn more about the risk to you and your family on our genetic testing page.
Some people have an elevated risk of developing melanoma. Review the melanoma screening guidelines to see if you need to be tested.
Behavioral and lifestyle changes can help prevent melanoma. Visit our prevention and screening section to learn how to manage your risk.
Melanoma Risk Factors
Anything that increases your chance of getting melanoma is a risk factor.
Sun damage, especially a history of peeling sunburns, is the main risk factor for melanoma. Artificial sunlight from tanning beds causes the same risk for melanoma as natural sunlight.
Other risk factors for melanoma include:
- Fair complexion: People with blond or red hair, light skin, blue eyes and a tendency to sunburn are at increased risk.
- Previous melanoma
- Moles (nevi): Having a lot of benign (non-cancer) moles
- Family history of melanoma
- Atypical mole and melanoma syndrome (AMS): Previously known as dysplastic nevus syndrome, AMS is characterized by large numbers of atypical moles. If you have AMS, you and your family members should be screened regularly
Not everyone with risk factors gets melanoma. However, if you have risk factors, it’s a good idea to discuss them with your health care provider.
Learn more about melanoma:
Learn more about clinical trials for melanoma.
MD Anderson is #1 in Cancer Care
5 things to know about raised moles
When people talk about moles, they are usually referring to a variety of skin growths, including true moles — which are also called nevi — freckles and other growths. However, in dermatology, a mole is a very specific type of skin growth that looks a certain way under a microscope.
Ahead, I’ll share more facts you might not know about moles, including how to tell if they are healthy.
Raised or flat doesn’t mean healthy or unhealthy
We can’t rely solely on whether a mole is raised or flat to determine if it is healthy. Some moles and skin lesions naturally grow vertically rather than horizontally. Moles that grow up and down are going to feel more raised than moles that grow laterally.
Instead of whether a mole is raised or not, start with the ABCDE rule to help determine if your mole may be healthy or may be exhibiting signs of melanoma, a type of very high-risk skin cancer.
A is for asymmetry, or whether one half of the mole looks different from the other half.
B is for border. You can tell if your mole has an unusual border if it would be challenging to outline.
C is for color. Note if your mole is multiple colors.
D is for diameter. Is your mole larger than the size of a pencil eraser, or about 6 millimeters?
E is for evolving. Has your mole rapidly grown or begun to hurt, itch or bleed? If something is bleeding or painful, those are my signs that it should prompt attention.
You can also use the Ugly Duckling rule to determine if a mole may be abnormal. Ugly Duckling moles look different than your other spots. This could look like developing a black mole when all of the other moles on your body are brown.
If your mole meets any of the ABCDE criteria or follows the Ugly Duckling rule, make an appointment with a dermatologist for a skin cancer screening exam.
Having a high number of moles may increase your skin cancer risk
Having more moles — especially 50 or more — can increase your risk for melanoma.
If you have more than 50 moles, you are considered to have a higher risk for skin cancer and could benefit from an annual skin check with a dermatologist.
It is rarer to develop moles after age 40
Usually, after around age 40, people stop developing new moles. You can certainly develop other skin lesions after this age, though! Don’t be afraid to see a dermatologist about any type of new or rapidly changing spot on your skin, or a spot that bleeds, hurts or itches.
It’s possible to remove raised moles, but not always recommended
While it is possible to remove raised moles, many dermatologists prefer not to remove healthy-looking moles unless they bother or worry the patient. That’s because removing a mole can leave a scar. Moles can also grow back after they are removed, which can look atypical.
I also warn patients against getting moles removed by providers who aren’t dermatologists. While it isn’t common, it is possible to get a skin lesion partially removed that turns out to be cancerous. This can complicate and delay a skin cancer diagnosis.
If you have a mole that bothers or concerns you, talk to your dermatologist about the best way to proceed.
When in doubt, see a dermatologist
Check your skin every month. It can be hard to notice skin changes on a daily or weekly basis, but monthly check-ins allow you to note if a mole or other spot on your skin is dramatically changing.
If you wonder if a skin spot requires a trip to the dermatologist, I always recommend making an appointment. It can be hard to figure out what skin spots are normal on your own, not to mention challenging to check your own scalp or back.
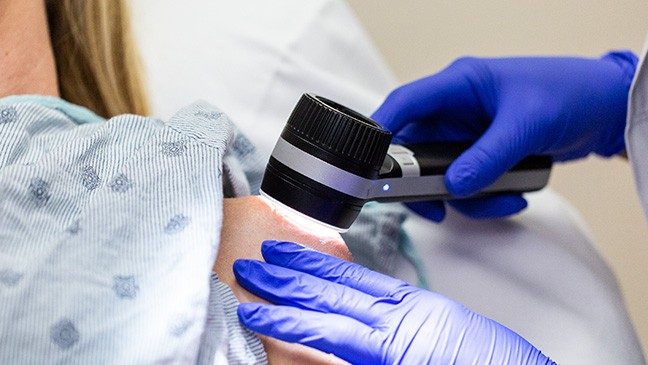
At a skin screening, a dermatologist will look at your skin, sometimes with the help of a magnifying tool called a dermatascope. They may ask you questions about the history of the spot, how long it has been there and the changes that prompted your visit.
If your dermatologist sees any concerning spots, they may perform a biopsy. This involves removing a mole and looking at it underneath a microscope to diagnose if it is cancerous.
Another benefit of making an appointment with a dermatologist for a full body skin assessment? Your dermatologist can keep an eye on any skin changes that happen over time. In this case, preventive care is as simple as taking a look at your skin.
Request an appointment at MD Anderson online or call 1-877-632-6789.
Melanoma caregiver: 3 ways MD Anderson has exceeded our expectations
As a retired teacher, I really appreciate the importance of “checking for understanding.”
That’s one reason I’ve been so impressed with MD Anderson. Everyone my husband Rod and I have encountered there so far has done just that. They’ve all wanted to make sure we understood precisely what was going on and why, at every step of his treatment for stage IV melanoma. That’s not something you find at every hospital.
Here’s a more detailed look at the ways they’ve exceeded our expectations.
Checking for understanding
Any time we’ve had questions about some aspect of Rod’s treatment, someone would take the time to explain whatever was confusing us and make sure we understood their answers. That was true whether we asked why a doctor made a particular recommendation or how to deal with a certain side effect. And, if they couldn’t do it, they’d bring in other people who could explain it better.
One nurse sat in a room with us for 45 minutes explaining targeted therapy, as well as how the specific drugs being recommended for Rod would work and what we could expect once he started taking them.
When I had to call Patient Advocacy one time because I didn’t understand a few terms on Rod’s pathology report, they connected me with a doctor who spent 20 minutes on the phone explaining it until I understood. That’s exceptional customer service.
Reducing scanxiety while waiting for results
MD Anderson is thoughtful in other ways, too. They know that patients and caregivers can get very anxious while waiting to hear the results of tests and scans. So, if it was going to be more than a few minutes before Rod’s doctor could see us, his care team would have a physician’s assistant pop into our exam room, just to let us know when his scans were OK. Then we could relax and not worry so much!
That level of consideration also helped us understand why Rod’s doctors might be running late in the first place. Our own experience had taught us that they took as much time as necessary with each patient. So, one day, Rod turned to me after we’d been waiting a while and said, “Maybe the reason is that somebody’s getting bad news.”
I asked one of the nurses later if that was the case, and she said it probably was. Then, I asked her, “How do you deal with that when it happens?” She told me that sometimes, care teams all got together at the end of the day and just cried. They really do care about their patients.
Convenient locations and personalized treatments
When Rod and I first came to MD Anderson in 2014, we considered it a true blessing that we only lived about five hours away from the Texas Medical Center Campus. But when MD Anderson The Woodlands opened in October 2019, we were even more thrilled.
Being able to get some of Rod’s treatments and checkups there has been wonderful. That location shaves two full hours off our drive time. Everyone there is just as personable and knowledgeable. And, the parking’s free!
The staff there even learned what type of music Rod likes best, so that they could have it queued up and ready to go whenever he came in for treatments. That’s the kind of thoughtful care that MD Anderson is known for. And that’s what has made us fans for life.
Request an appointment at MD Anderson online or call 1-877-632-6789.
How can you tell if a mole is cancerous?
Maybe a new spot catches your eye while you’re drying off from your shower. Or maybe the spot you swear used to be flat has suddenly started catching on your clothes.
Skin changes can be confusing at best and concerning at worst. It can be hard to tell whether a spot is harmless or something that requires medical attention.
As a dermatologist, I often get questions from people who are concerned about skin changes. Here, I’ll share advice and steps you can take if you’re worried a mole might be skin cancer.
Why choose MD Anderson for your melanoma treatment?
Our team of internationally recognized experts provides customized treatment for melanoma to ensure you receive the most advanced care with the least impact on your body.
Multidisciplinary Melanoma Treatment
Each person and each melanoma are different, and at MD Anderson's Ben Love/El Paso Corporation Melanoma and Skin Center, we use our unique multidisciplinary approach to tailor treatment for melanoma skin cancer specifically to your unique situation.
More than 10,000 melanoma patients –– among the most of any program in the world –– are evaluated here each year. Caring for this large and diverse patient population has helped us develop an outstanding team of melanoma specialists with wide-ranging expertise and experience in treating all types of melanoma.
Comprehensive, Specialized Melanoma Treatment
Your personal team of experts in melanoma skin cancer may include melanoma surgical oncologists, melanoma medical oncologists, pathologists, dermatologists and dermatologic surgeons, head and neck surgeons, neurosurgeons, plastic surgeons and other surgeons, radiation oncologists, diagnostic radiologists, and other specialists if needed. They work together closely, collaborating and communicating at every step of your treatment.
Several innovative treatments for melanoma skin cancer are offered at MD Anderson, and many of them were discovered here. Your personalized treatment may include:
- Lymphatic mapping and sentinel node biopsy
- Minimally invasive limb perfusion
- Targeted therapies that capitalize on our improved understanding of the molecular alterations within melanoma tumor cells
- Adjuvant radiation therapy to help reduce the risk of melanoma coming back after surgery
- Treatments for rare forms of melanoma, such as those that begin in the eye (uveal melanoma) or mucosa (for example, vaginal, rectal or sinonasal)
Pioneering Research
And we're constantly researching ways to help the body fight the cancer, including:
- Immunotherapy, including the latest agents such as ipilimumab, PD-1 and PDL-1 inhibitors, interleukin-2 and adoptive T-cell therapy
- Targeted therapies such as BRAF, MEK, multikinase and KIT inhibitors
- Combination regimens
- Vaccines
Since 2004, the National Cancer Institute has awarded MD Anderson a multimillion-dollar Specialized Programs of Research Excellence (SPORE) grant. This means we are able to offer a broad array of clinical trials for melanoma skin cancer.
New targeted therapies are improving and bringing hope to our patients.
Jeffrey Gershenwald, M.D.
Physician
After two melanoma diagnoses, a family reflects on their experiences at MD Anderson
Sam Gee was preparing for a wrestling tournament his freshman year of high school when a referee pointed out a suspicious spot on his back. He didn’t worry much about the spot, a mole he first noticed after an injury as a small child. Still, if Sam wanted to compete that season, he would need to get it checked out. A few weeks after a shave biopsy, Sam and his family learned he had melanoma, an aggressive form of skin cancer.
His dermatologist recommended that Sam seek treatment at MD Anderson. Soon, Sam and his mother, Ashley, were making frequent trips from San Antonio to Houston so he could receive immunotherapy and undergo surgery at MD Anderson.
“The first time we visited, walking up to the front door felt intimidating,” Ashley says. “But once we were there, everyone made us feel so welcome. After that, there was no question in my mind that we were in the right place.”
Sam agrees, recalling how his care team made him feel at ease during a turbulent time. “There's just something about it that you can't see in an advertisement,” he says. “MD Anderson is the place to be.”
Adapting to a melanoma diagnosis as a teenager
Sam recalls how as a 14-year-old, cancer was the last thing he expected. He didn’t know anyone else his age who was facing a cancer diagnosis. “It was a feeling of great shock. I had no idea what to think,” he recalls. “I quickly realized things were going to start changing.”
His mindset became: “Things are going to be different now. Time to adapt.”
And indeed, life did change drastically – not only for Sam but for everyone. Just a few weeks after his cancer diagnosis in early 2020, the COVID-19 pandemic began.
“The world shut down, and I was shutting down with it,” he says. “Right as I quit being able to attend school, everybody quit being able to attend school. Everybody kind of hid away during COVID-19, and that was definitely what I wanted to do during my cancer experience. I just wanted to put a hood on, duck down and finish it out.”
In addition to having several lymph nodes removed, Sam underwent several rounds of immunotherapy, including ipilimumab and nivolumab.
“I remember one of his doctors saying that 10 years ago this was a death sentence, but now with immunotherapy, it was something that could be cured,” Ashley says. “That gave me hope throughout his treatment. I always hung onto those words.”
After months of treatment, Sam was declared cancer-free in 2021. He still visits MD Anderson for check-ups several times a year, but his day-to-day life looks much more typical than it was three years ago. He is currently wrapping up his senior year of high school and preparing to study computer science at Texas A&M University at Galveston in the fall.
A second melanoma diagnosis in the family
Less than two years after Sam’s diagnosis, his grandmother, Suzan Taff, was diagnosed with acral lentiginous melanoma, a rare type of skin cancer not caused by sun exposure. After the family’s positive experience at MD Anderson during Sam’s treatment, Suzan says she knew exactly where she wanted to go for her own treatment.
“I admired how Sam went through it all so well. I told him that he would be my guide,” says Suzan. “I was so pleased with his success that I never was afraid of anything. I knew I was going to be alright because I could see that Sam was alright.”
Suzan’s cancer has responded well to surgery and immunotherapies, such as ipilimumab, nivolumab, TVEC and pembrolizumab. She says the treatments are not painful and that she’s been able to continue doing the activities she enjoys. Although her tumors respond well to immunotherapy, new ones continuously emerge, so she remains on maintenance therapy with nivolumab. Suzan remains confident her doctors are providing her with the best possible care.
“My time at MD Anderson has been extremely positive and productive,” she says. “Even though some of my results have been mixed, I still feel like everybody there is working toward my benefit. I can’t say enough good things about them.”
A special encounter
In November 2022, Sam and his family got to meet Jim Allison, Ph.D., at MD Anderson’s “A Conversation With A Living Legend” event in San Antonio. At the event, Dr. Allison shared his story of pioneering immunotherapy, for which he was awarded the 2018 Nobel Prize in Physiology or Medicine, and his continuing research at the Allison Institute. For Sam and Suzan, meeting Dr. Allison was especially meaningful.
“Dr. Allison has changed the entire way of treating cancer, especially melanoma,” Suzan says. “I was thrilled to have the opportunity to express our gratitude for his persistence. He spent all of Sam’s lifetime working on these drugs, and by the time Sam needed them, they were available. I told Dr. Allison that I thought he did all that work just for Sam.”
Sam calls Dr. Allison one of his role models. “It was quite the experience to be able to look face-to-face with the man and tell him, ‘Thank you for saving my life,’” Sam says. “It was incredible to shake his hand and take a photo with the man who is responsible for saving me and so many others through his discoveries.”
Sam often reflects on the medical advances, like Dr. Allison’s, that made his recovery possible and gave his family hope for his grandmother.
“I have so much hope that we’re close to the cure now,” he says. “Not long ago, you had three main treatment methods: cut, kill, burn. But now with immunotherapy, we’re teaching the body to fight cancer itself. That’s why we must continue to dive deeper through research because the treatments are going to keep getting better.”
Request an appointment at MD Anderson online or by calling 1-877-632-6789.
Melanoma Treatment at MD Anderson
Featured Articles

Mucosal melanoma survivor: 4 reasons I joined a clinical trial at MD Anderson

15-year stage IV melanoma survivor: ‘This is the best I’ve felt in years’

Anoscopy explained: Purpose, process and results
What to expect when you have a mole removed

What happens when you get a sunburn

4-time cancer survivor and employee: Why I chose MD Anderson for my treatment

Stage IV melanoma survivor: Dark skin won’t protect you from skin cancer
Clinical Trials
found anywhere else.
Becoming Our Patient
Get information on patient appointments, insurance and billing, and directions to and around MD Anderson.
myCancerConnection
Talk to someone who shares your cancer diagnosis and be matched with a survivor.
Prevention & Screening
Many cancers can be prevented with lifestyle changes and regular screening.
Counseling
MD Anderson has licensed social workers to help patients and their loved ones cope with cancer.
Help #EndCancer
Give Now
Donate Blood
Our patients depend on blood and platelet donations.
Shop MD Anderson
Show your support for our mission through branded merchandise.