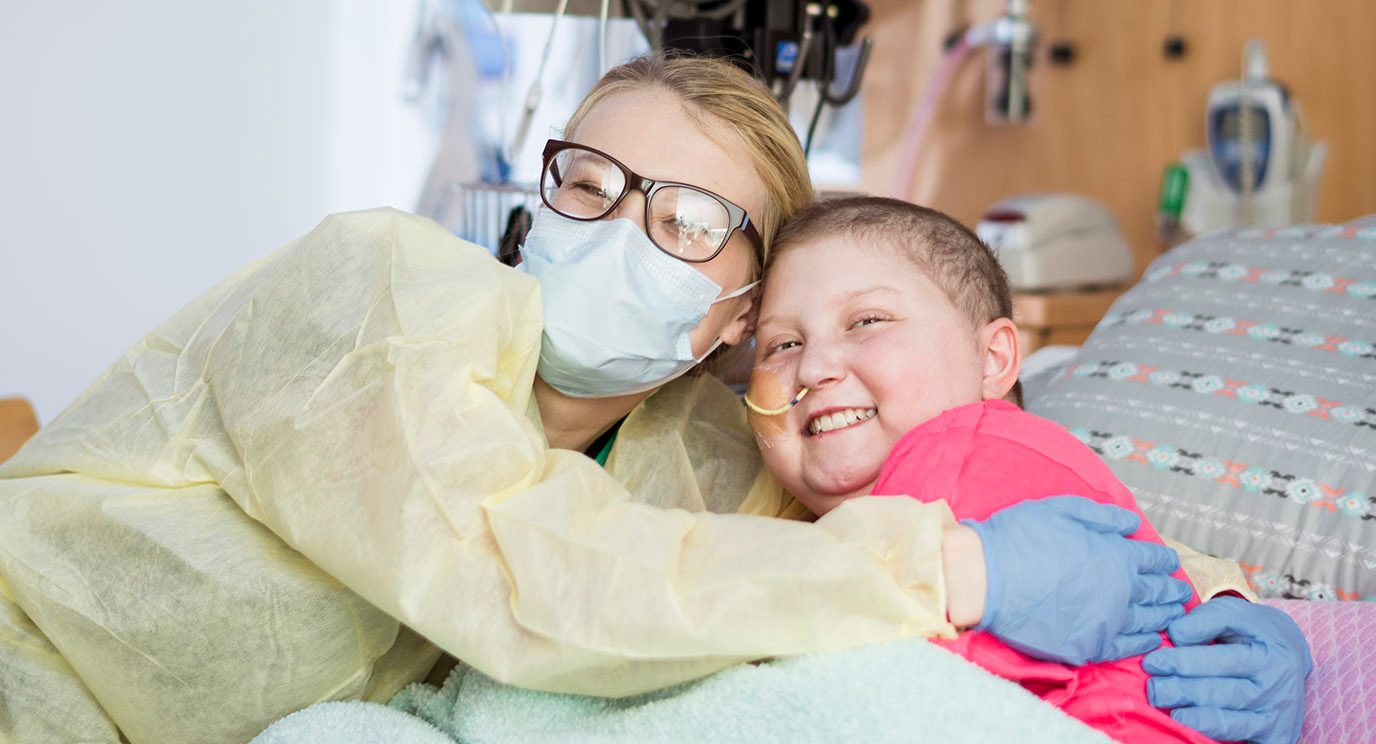
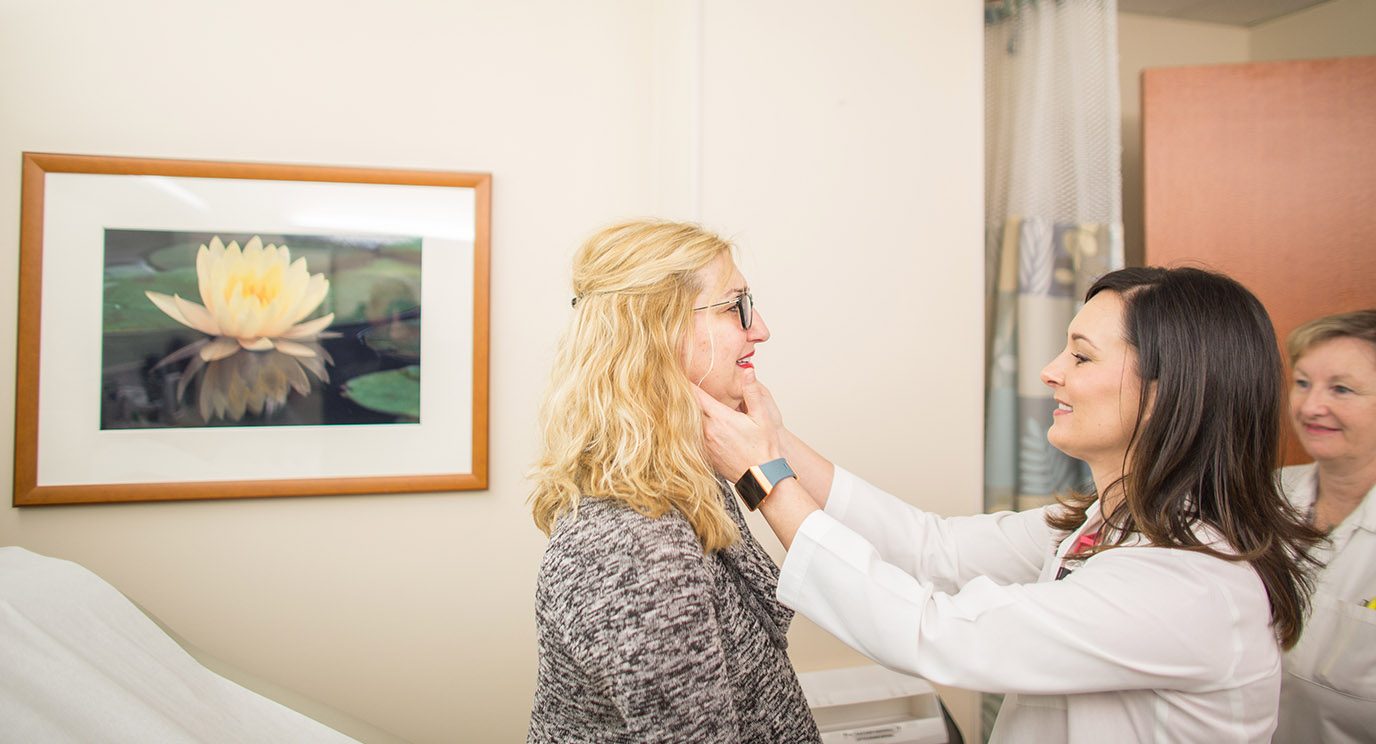From pain management to nutrition, surgical protocol quickens recovery
Patients are rebounding faster from surgery and having fewer complications thanks to a new program that improves the post-surgical experience.
“The recovery from my first surgery in Dallas was difficult,” recalls Bridgette Fleming, who underwent laparoscopic colon resection in late March 2018 to treat her colon cancer.
“After the surgery, I was on hydrocodone around the clock for two weeks. My doctor told me it was important to gain weight, but the surgery messed up my taste buds, and nothing tasted good.”
Previous CT scans had shown uncharacterized spots in her liver, so Fleming traveled to Houston in April to get a second opinion at MD Anderson Cancer Center.
“My doctors at MD Anderson discovered that the cancer had metastasized to my liver, and recommended chemotherapy.”
A much better recovery
In May, Fleming moved to the small town of Spring, just outside of Houston, to live with her aunt and uncle while undergoing treatment. Chemotherapy alone was not enough to treat the liver lesions, so Fleming scheduled what is known as an open central hepatectomy for this past October.
“This is a rare procedure because of the magnitude of the surgery,” says Ching-Wei D. Tzeng, M.D., Fleming’s surgeon at MD Anderson, in describing the 6-hour surgery that left Fleming with an 11-inch incision on her abdomen.
This time, however, her postoperative experience was dramatically different.
“I was really worried about the recovery,” she recalls, “but I was surprised that even after a major abdominal surgery, I only had to use the pain pump twice a day for a few days. I didn’t need any narcotic pills. My hospital room had aromatherapy, and the lavender smell really helped me relax and fall back to sleep at night, despite the usual hospital interruptions. When I left the hospital three days after the surgery, I was worried about getting to my second-floor bedroom at my aunt and uncle’s house, but I didn’t have any trouble navigating the stairs.”
The power of enhanced recovery
Fleming’s use of opioid pain medication, her hospital stay and her recovery time all were minimized thanks to MD Anderson’s Enhanced Recovery Program (ERP). The cancer center first implemented the ERP model in 2012, and now 19 teams incorporate the five principles of enhanced recovery: patient education and engagement, multimodal opioid-sparing analgesia, rational fluid therapy (ensuring patients receive the correct amount of intravenous fluids), risk-adjusted pathway based postoperative care, and rapid rescue from postoperative complications.
The ERP motto is “back to self, back to family, back to life, and back to work.” Two weeks after her surgery, Fleming was looking forward to enjoying the cool fall weather and walking around her neighborhood, which had been unthinkable two weeks after her colon surgery.
Collaboration is key to ERP’s success
Vijaya Gottumukkala, M.D., professor of Anesthesia and Perioperative Medicine and ERP co-lead at MD Anderson, describes the program as “patient-centric, recovery-focused, outcome-based, efficiency-driven, multidisciplinary care in the acute care setting, where all clinicians work together as a team around the patient’s needs. Instead of each group working in silos, we work as a team to get the patient back on track as safely, efficiently and quickly as possible,” Gottumukkala says.
The care teams follow standardized ERP protocols that minimize variation in practice. For the success of the program, it’s necessary that all team members agree to their roles in the protocol. Effective and timely communication is essential, so the care teams meet regularly to learn from each team member’s experience and continually optimize and improve the program.
Expanding to UT System and beyond
MD Anderson’s ERP model has been remarkably successful, allowing the Division of Surgery to lower the average length of stay from 7 and 1/2 days to 4 and 1/2 days — a major shift in surgery time frames.
“The ERP model, in my opinion, is the most important surgical intervention in the past 30 years,” says Thomas Aloia, M.D., associate professor of Surgical Oncology and ERP co-lead. “I know of no other intervention that has been implemented with this level of benefit, and without causing harm,” says Aloia, who also heads the Surgical Oncology department’s Institute for Cancer Care Innovation where the ERP program is housed.
Because of the success of the ERP, MD Anderson has received a $835,000 quality grant from The University of Texas System to help implement ERPs in colorectal surgery programs at all hospitals within the system.
“Every patient is in recovery of some kind,” says Aloia. “The goal is to expand the ERP model throughout the institution, to other UT system hospitals, to our cancer network partners and, ultimately, throughout the nation.”
Meet some of the team members
The surgeon: Ching-Wei D. Tzeng, M.D., assistant professor of Surgical Oncology
The ERP emphasizes collaboration among all members of the health care team. The day before a surgery, the surgeon checks in with the anesthesiologist to determine what regional block will be used during the surgery. This is crucial to avoiding use of narcotics after the surgery, which can slow down the patient’s gastrointestinal tract and prevent early intake of food and early ambulation — two important discharge criteria.
“In a traditional model of surgery, there is a lot of variation in practice, but ERPs provide clear protocols so that the healthcare team is on the same page,” Tzeng says. “Nurses and advanced practice providers know when patients can advance to solid foods and how to limit intravenous fluids.”
Similar patients are grouped together in the same unit so that the team is not spread out over the hospital. This physical proximity also helps promote communication.
“Ten years ago, this concept was called ‘fast-track,’ and the emphasis was on the cost-effectiveness and benefits for the hospital,” Tzeng says. “But at MD Anderson, the ERP model is about the benefits for the patients— for example, and helping patients proceed with lifesaving cancer treatments. Because we care about patient-centered outcomes, the ERP model has to be the standard of care.”
The anesthesiologist: Jose Soliz, M.D., associate professor of Anesthesiology and Perioperative Medicine
The ERP helps patients maintain excellent pain control while minimizing the use of opioid medications. MD Anderson’s reduction of opioid use by 70 percent in some ERPs is truly remarkable. The ERP model emphasizes anesthesiologists’ role as perioperative physicians who are involved in a patient’s care before, during and after surgery.
“We tailor anesthetics to minimize symptom burdens, to reduce intraoperative opioid use, and to increase functional recovery,” Soliz says. “For example, we use non-narcotic medications and nerve blocks, in addition to general anesthetics to reduce intraoperative and postoperative opioid use. This results in better pain control, fewer side effects and better recovery.”
For Soliz, one of the most important aspects of the ERP model is the ability to tailor treatments for each patient. For example, in the ERP for pancreatic surgery, patients are stratified according to their risk of developing pancreatic fistulas after surgery. Patients at low risk move through the process faster than patients at high risk. Adapting the program to patients in this way has reduced the median hospital stay from 10 days to six days.
The nurse: Luisa “Dee” Gallardo, executive director of Quality, Safety and Research for Nursing
Within the ERP model, Gallardo says “nurses are at the sharpest end of patient care delivery, applying their clinical expertise to all ERP patients through collaborative relationships.
“The ERP platform encourages patients to actively participate in activities that promote their well-being,” explains Gallardo, who serves as the nursing division’s executive leader for the ERP. “The ERP provides standardized algorithms designed to assist nurses as they work to progress patients along the road to recovery.”
For example, a nurse could choose from multiple opioid-sparing strategies such as aromatherapy, breathing techniques, warm compresses or meditation to manage symptoms. The nurse teaches patients coping techniques that can be applied during admission and post-discharge, ultimately contributing to reductions in hospital readmissions and lower complication rates.
“Being part of a collaborative team that returns patients to their preoperative functional state in a shortened time frame is both rewarding and energizing,” Gallardo says.
The dietician: Timothy Coleman, dietician, Clinical Nutrition
The ERP also prioritizes early food intake and nutritional preparation for surgery and for healing. In the traditional recovery model, patients aren’t allowed to eat anything after midnight the night before surgery, and aren’t allowed to eat after surgery until bowel function returns. This means patients’ bodies aren’t properly fueled for healing.
In the ERP model, patients can eat solid food up to six hours before surgery and can have clear fluids up to two hours before surgery. The ERP model also encourages patients to eat solid foods as early as possible after surgery. Traditionally, dieticians are consulted only at the discretion of the surgeon — usually to address postoperative complications. With the ERP, the dietician meets with the patient before surgery and makes recommendations to improve the patient’s nutritional status.
“We talk about carbohydrate loading, hydration, adequate protein intake and weight stability,” Coleman says. “We normally see patients immediately after surgery and help them with symptoms. For example, if they have post-operative nausea, we might recommend against spicy or greasy foods; we recommend bland foods, small frequent meals and plenty of fluids. Another good strategy is serving cooked foods cold to help with nausea.”
Coleman was involved in developing the protocols of MD Anderson’s ERPs.
“Sometimes nutrition is pushed to the side in the face of acute issues, but the ERP model integrates all components as equally important. I definitely feel like a valued part of the team.”