Surgical Oncology
Matthew H.G. Katz, M.D.
Department Chair
- Departments, Labs and Institutes
- Departments and Divisions
- Surgical Oncology
Clinical Care
Surgery is a vital part of care for many patients with cancer. It can help doctors diagnose and stage disease, treat it, relieve symptoms and prevent cancer from spreading or returning. The Surgical Oncology department at MD Anderson treats patients with a wide variety of malignant and benign tumors. The department comprises numerous specialty sections and services:
- Endocrine Surgery
- Gastric-Peritoneal Surface Surgery
- Hepatopancreatobiliary Surgery
- Melanoma Surgery
- Pediatric Surgery
- General, Acute and Palliative Care Surgery
- Sarcoma Surgery
These sections provide assessments, treatment planning and surgical services to cancer patients to improve survival, shorten recovery times and minimize treatment-related side effects. Each section strives to better identify patients who can benefit from surgery, and to advance and implement new surgical techniques. They are broadening the use of minimally invasive laparoscopic and robotic techniques to lessen the impact of surgery on patients. The department is comprised of clinical operations, educational programs and ground-breaking research efforts. These pillars support our collaborations with multi-disciplinary teams in the mission to end cancer.
Our surgeons are highly specialized clinicians who practice at an exquisitely high-level. They are international thought leaders who set the standards of care for patients with a variety of cancers through their groundbreaking research. They also share a deep commitment to train the next generation of leaders in surgical oncology.
Matthew H.G. Katz, M.D.
Chair, Surgical Oncology department
Research

The MD Anderson Surgical Oncology department focuses on providing exceptional patient care while conducting basic, translational and clinical research to develop the next generation of innovative approaches to the treatment and prevention of both common and rare cancers. We work to discover new ground-breaking surgical techniques, novel operating devices and methods to decrease cancer disparities and improve outcomes for patients.
Training Programs
Complex General Surgical Oncology Fellowship
The Complex General Surgical Oncology Fellowship is an ACGME-accredited two- to three-year program and hosts seven new fellows each year. It is directed by Brian Bednarski, M.D., professor of Colon and Rectal Surgery and Surgical Oncology. The program and its predecessors have graduated over 300 surgeons. The fellowship provides rich clinical and research experiences that prepare trainees to enter academic careers, establish successful surgical oncology programs at university centers, and develop productive research and training programs.
Learn more about the Complex General Surgical Oncology Fellowship.
Surgical Endocrinology Fellowship
The Surgical Oncology Department at MD Anderson offers a one-year advanced training fellowship in Surgical Endocrinology accredited by the American Association of Endocrine Surgeons (AAES). This unique fellowship is designed to provide a well-rounded clinical and research experience and a strong foundation for a career in academic endocrine surgery. The program was incepted in 2009 and is currently directed by Paul Graham, M.D., associate professor of Surgical Oncology.
International Surgical Oncology Fellowship
The International Surgical Oncology Fellowship is a one-year program directed by Jess Maxwell, M.D., assistant professor of Surgical Oncology. The fellowship has been dedicated to the training of international surgeons on the surgical management of solid tumors since 2013.
Learn more about the International Surgical Oncology Fellowship.
Hepatopancreatobiliary (HPB) Surgery Fellowship
The HPB Surgery Fellowship is directed by Ching-Wei Tzeng, M.D., associate professor of Surgical Oncology. Since 2013, fellows have trained to provide comprehensive, state-of-the-art medical and surgical care to patients with surgical diseases/disorders of the liver, pancreas and biliary tract.
Learn more about the Hepatopancreatobiliary Surgery Fellowship.
T32 Training Program
The department of Surgical Oncology has a grant to train eight academic surgical oncologists each year in cancer research under the collaborative leadership of Jennifer Wargo, M.D., and Ashley Holder, M.D. It provides research opportunities in a broad range of basic oncologic disciplines, in one of three training tracks: basic and translational research; quality, clinical effectiveness and outcomes; and clinical trials and biomarkers. The department also has surgery residents from six Houston programs who rotate through services each year and medical students who rotate through monthly.
Knox Family Foundation Visiting Residency
The Surgical Oncology department at MD Anderson offers a unique, funded program designed to provide exposure to surgical oncology to general surgery residents who may otherwise have limited access to a robust clinical experience in the field of complex general surgical oncology and/or who have a demonstrated interest in providing cancer care to medically underserved populations within the United States. The program is directed by Christopher Scally, M.D., and Celia Ledet, M.D. The experience will be tailored to the needs and interests of the participant.
Deadline to apply is April 1, 2026, for the 2026-2027 Academic Year. Interested applicants can submit a letter of interest and CV to Marshae Daniel.
Contact Us

Phone Number: 713-792-6940
Fax Number: 713-745-1462
The University of Texas MD Anderson Cancer Center
The Department of Surgical Oncology
1400 Pressler St., Unit 1484
Houston, TX 77030

Dr. Matthew H.G. Katz, Department Chair
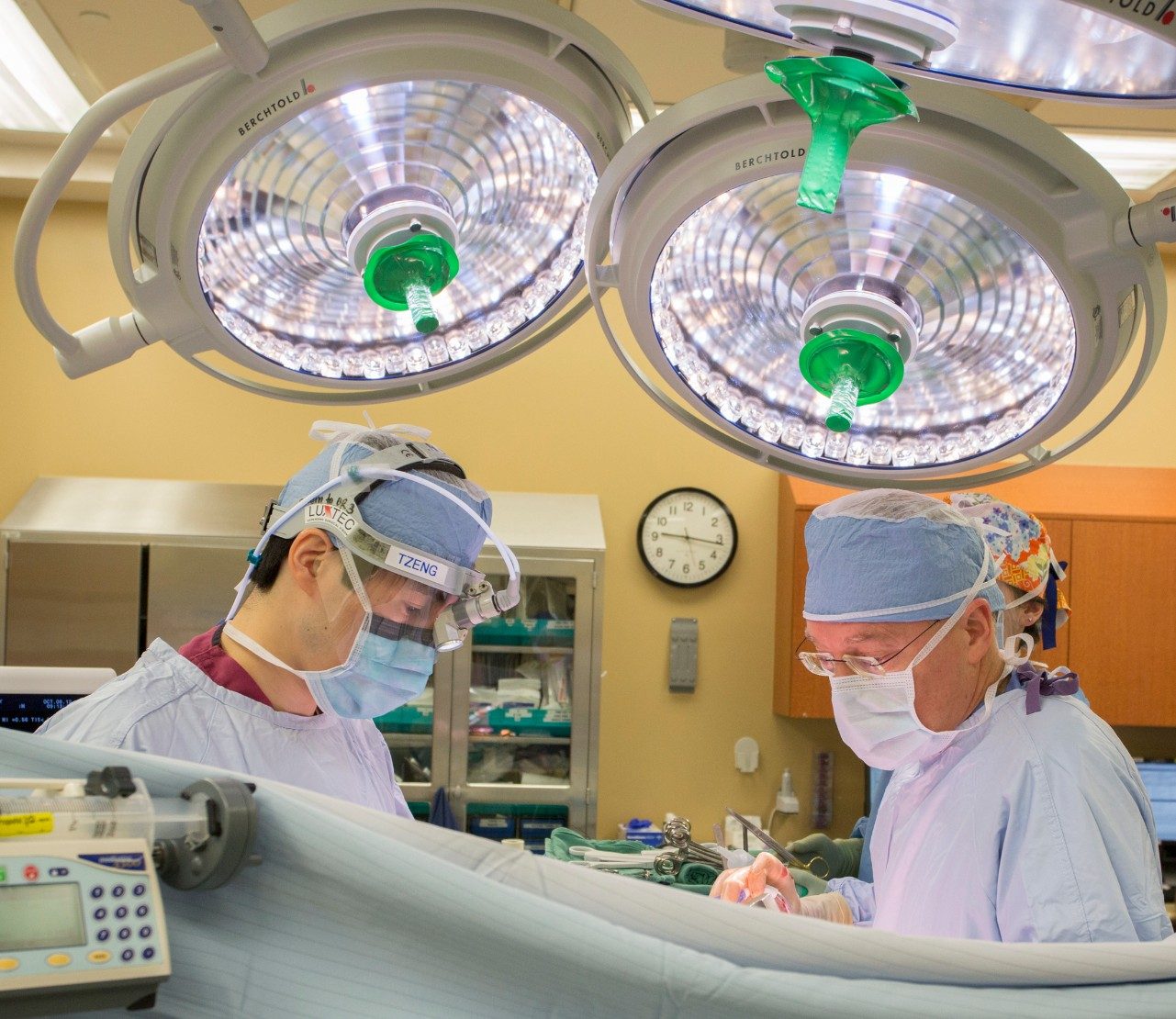
Dr. Jean-Nicolas Vauthey, HPB Surgery Section Chief (right)
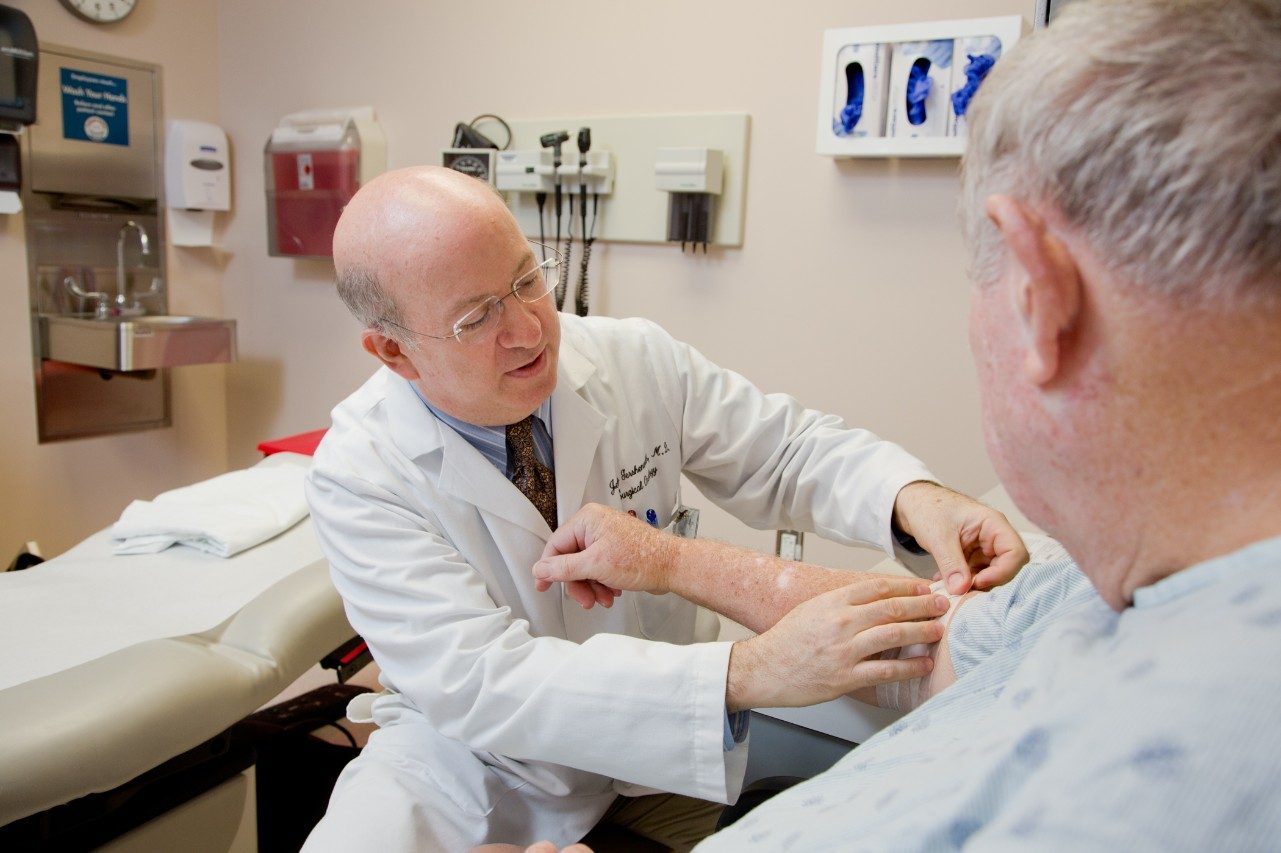
Dr. Jeffrey Gershenwald, Melanoma Surgeon
Give Now
Research Areas
Find out about the four types of research taking place at UT MD Anderson.
