Research
The Green lab focuses on intersections between ‘omics (genomics, transcriptomics, epigenomics) and immunology (germinal center development, anti-tumor immunity) as it pertains to mature B-cell malignancies. Our approach utilizes cutting-edge ‘omics and immunology methodology to interrogate patient tumors and immune cells, patient-derived xenograft models, genetically engineered mouse models, and CRISPR-engineered cell line models within different genetic or therapeutic contexts. There are two major intersecting areas of focus:
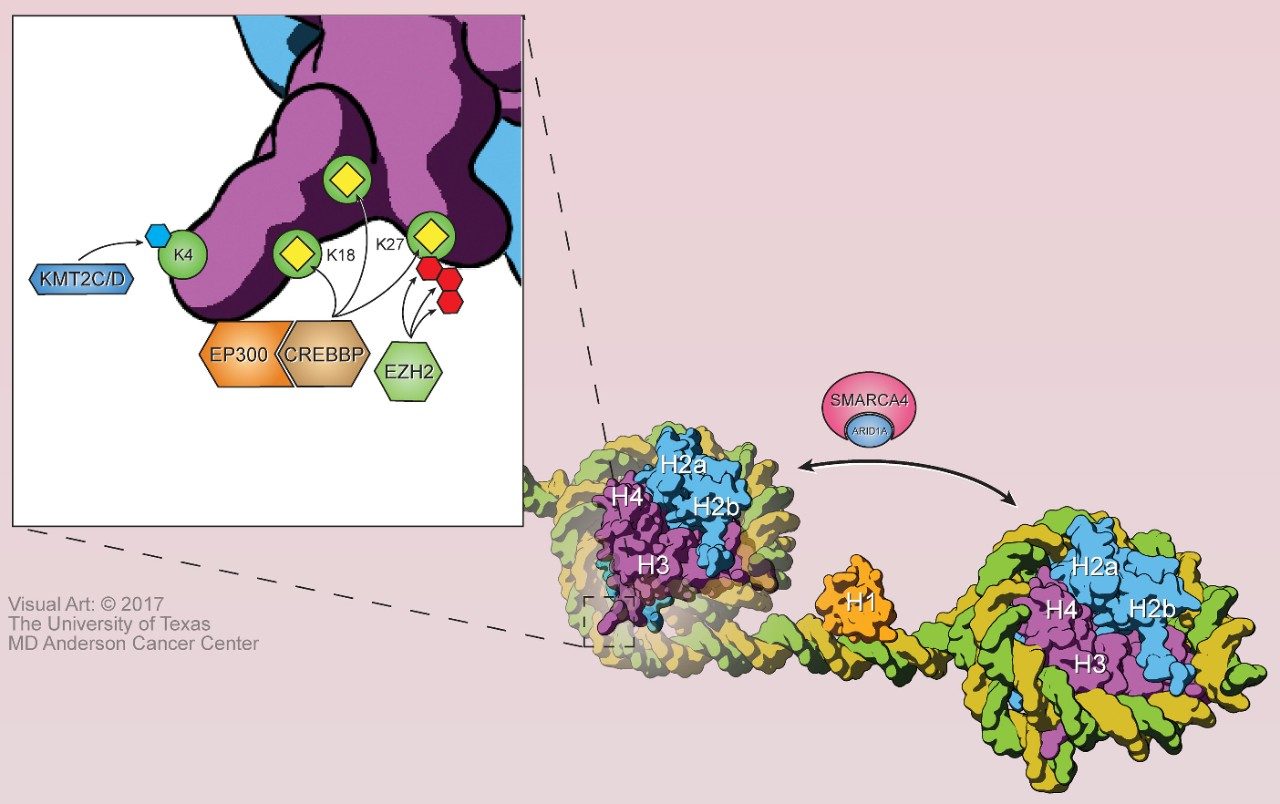
Epigenetics of B-cell development and lymphomagenesis
The majority of B-cell lymphomas originate from the germinal center (GC), a stage of development at which B-cells undergo rapid proliferation and affinity maturation of their immunoglobulin genes to produce memory B-cells and plasma cells. This process is regulated by broad and dynamic changes in the epigenome and transcriptome of B-cells as they progress through the GC reaction and respond to signals from other cells within the GC. Epigenetic dysregulation is a hallmark of GC-derived B-cell lymphoma, and includes the direct somatic mutations of genes with a role in the post-translational modification and conformation of chromatin – which we collectively refer to as chromatin modifying genes (Figure 1) [1]. A major focus of our lab is to understand the mechanism by which mutations of chromatin modifying genes cause lymphoma, how other genetic alterations and immunological signals contribute to the epigenetic etiology of lymphoma, and how associated dependencies can be therapeutically targeted [2]. A few examples include:
CREBBP mutations. The CREBBP gene encodes a histone acetyltransferase protein that is mutated in ~65% of follicular lymphoma (FL) and ~15% of diffuse large B-cell lymphoma (DLBCL). We have previously shown that CREBBP mutations arise early during disease genesis of FL, residing within a common progenitor cell (CPC) population that seeds disease relapse, and promoting immune evasion via loss of antigen presentation on MHC class II [3, 4]. Conditional knock-out of Crebbp in B-cells cooperates with Bcl2 over-expression to drive lymphomagenesis in mice, but lacked many of the characteristics of human FL [5]. We therefore models CREBBP catalytic domain point mutations in lymphoma cells using CRISPR and identified a possible dominant-negative role that removes antagonism to the BCL6 transcriptional repressor (Figure 2). This led to loss of epigenetic and transcriptional suppression of antigen presentation and interferon signaling via BCL6-associated HDAC3 activity, which could be targeted using an HDAC3-selective inhibitor [6]. We are extending upon this work under a recently renewed NIH R01 grant.
E2 transcription factor family. E2 transcription factors including TCF3 (E2A) and TCF4 (E2-2) play an important role in B-cell development and are deregulated in lymphoma. E2 transcription factors bind DNA as a dimer, and can be inhibited by Id proteins including Id3 and Id2. TCF3 and ID3 mutations occur in 10-25% and 35-58% of Burkitt lymphomas, respectively, but at a relatively low rate in other GC-derived lymphomas [7]. We also recently identified DNA copy number gains of the TCF4 gene that occur in ~40% of the ABC-like subtype of DLBCL and create a targetable dependency [8]. Ongoing work funded through an NIH R01 grant is aimed at understanding the dynamics of E2 transcription factors in the germinal center reaction and how genetic alterations of these factors lead to lymphoma.
BAF complex. A newer focus of our lab is on the role of the BAF (aka. SWI/SNF) complex in regulating B-cell development and lymphomagenesis. The BAF complex is a multi-subunit chromatin remodeling complex that catalyzes the ATP-dependent mobilization and eviction of nucleosomes. We are interested in how specific stoichiometries of this complex regulates GC B-cell differentiation and contribute to the pathophysiology of lymphoma. This work is supported by CPRIT and NCI R01 (in collaboration with Drs. Chris Mason and Ari Melnick at Weill Cornell Medical College) grants and includes work with genetically engineered mouse models, CRISPR-modified cell lines, and patient-derived xenograft models.
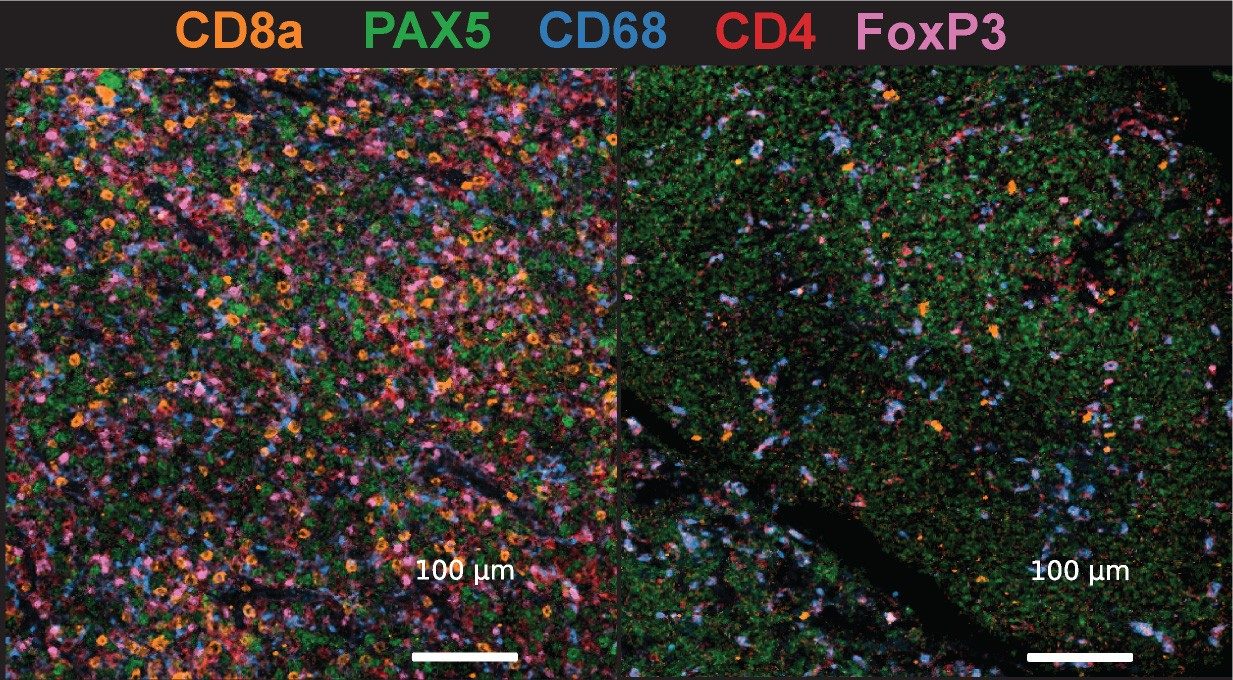
The role of the lymphoma microenvironment and perturbed immune interactions in modulating tumor immunity
Characterizing the lymphoma microenvironment. We have previously identified genetic mechanisms of immune escape in classical Hodgkin lymphoma and primary mediastinal large B-cell lymphoma through amplification of the PD-L1 and PD-L2 genetic locus [9], which can be effectively targeted using PD-1- or PD-L1-blocking antibodies. We have also shown that CREBBP mutations lead to loss of antigen presentation on MHC class II, which is associated with significant changes in the follicular lymphoma microenvironment including the differential expression of targetable immune checkpoints on tumor-infiltrating T-cells [10]. We are extending upon our previously published study of follicular lymphoma by characterizing the immune microenvironment of additional lymphoma subtypes, in various therapeutic contexts such as cellular therapy and T-cell engagers, and leverage genetically-engineered mouse models and PDX models to investigate novel approaches for targeting microenvironment-dependencies in lymphoma.
Chimeric antigen receptor (CAR) T-cell therapy. CD19 CAR T-cell therapy has been a breakthrough for large B-cell lymphoma, but the majority of patients do not have durable responses and treatment-associated toxicities are a clinical challenge that can delay recovery and affect outcomes [11]. Our aim is to improve patients outcomes by (i) identifying high-risk patients that require additional consolidative therapy; (ii) understanding the biology of CAR T-cell resistance to inform rationale approaches to improve responses; (iii) investigating the mechanistic drivers of toxicity to inform potential therapeutic interventions. We approach this by leveraging our large repository of patient samples and cutting-edge approaches such as single cell RNA-sequencing, cell-free DNA sequencing, and in vivo analysis with CAR T refractory PDX models. In doing so, we have identified characteristics in CAR T-cell infusion products that are associated with response and toxicity [12] and developed a clinico-genetic risk prediction model using low-pass whole genome sequencing from cell-free DNA to identify high-risk patients. We are expanding upon these studies in collaboration with industry partners to test rational therapeutic interventions that can be combined with CAR T-cell therapies to improve response and reduce toxicity.
Translational and Preclinical Research
Most clinical trials are developed empirically and have had variable success. Our model is to improve the likelihood of success using a three-pronged approach:
- basing drug selection and study design on firm mechanistic rational through “forward” translational research;
- performing thorough preclinical testing of novel therapeutics and combinations in disease-relevant models such as patient derived xenografts;
- incorporating robust correlative science into clinical studies to drive “reverse” translational research that validates mechanism of action and improves the design of future studies.
We achieve this through two sets of initiatives:
Developing Patient Derived Xenograft (PDX) Models for Translational and Preclinical Research
Supported by the Schweitzer Family Fund, we have developed a large repository of large B-cell lymphoma (LBCL) PDX models for translational and preclinical research. These models span the molecular spectrum of LBCL and include tumors from important clinical scenarios such as post-CAR T-cell relapse. All of the models have been validated against their primary tumor and confirmed to be EBV negative by EBER staining, in collaboration with Dr. Francesco Vega and Dr. Mario Marques-Piubelli. All models have also been extensively molecularly characterized, including RNA-sequencing, whole exome sequencing, low-pass whole genome sequencing and ATAC sequencing. We have also optimized the generation and in vivo modeling of CD19 CAR T-cell therapies to evaluate CAR T-cell combinations with other antibodies, T-cell engagers or small molecules. This allows us to select models and approaches based upon the proposed mechanisms of action for use in preclinical studies with academic or industry collaborators.
Industry Collaborations
We frequently engage with industry collaborators to perform translational and/or preclinical research using the cellular and molecular approaches that we have developed and the PDX models that we have available in-house. Some examples of industry collaborations include Sanofi, Kite/Gilead, Allogene, and Abbvie. For inquiries about collaborations, please email Michael Green, Ph.D.
References
- Green M. Chromatin modifying genes in follicular lymphoma. Blood 131(6):595-604. 2/2018. PMID: 29158360
- Yang H, Green M. Harnessing lymphoma epigenetics to improve therapies. Blood 136(21):2386-2391. 11/2020 PMID: 33206943
- Green MR, Gentles AJ, Nair RV, Irish JM, Kihira S, Liu CL, Kela I, Hopmans ES, Myklebust JH, Ji H, Plevritis SK, Levy R, Alizadeh AA. Hierarchy in somatic mutations arising during genomic evolution and progression of follicular lymphoma. Blood 121(9):1604-11, 2/2013. e-Pub 1/2013. PMCID: PMC3587323.
- Green MR, Kihira S, Liu CL, Nair RV, Salari R, Gentles AJ, Irish J, Stehr H, Vicente-Dueñas C, Romero-Camarero I, Sanchez-Garcia I, Plevritis SK, Arber DA, Batzoglou S, Levy R, Alizadeh AA. Mutations in early follicular lymphoma progenitors are associated with suppressed antigen presentation. Proc Natl Acad Sci U S A 112(10):E1116-25, 3/2015. e-Pub 2/2015. PMCID: PMC4364211.
- García-Ramírez I, Tadros S, González-Herrero I, Martín-Lorenzo A, Rodríguez-Hernández G, Moore D, Ruiz-Roca L, Blanco O, Alonso-López D, Rivas JL, Hartert K, Duval R, Klinkebiel D, Bast M, Vose J, Lunning M, Fu K, Greiner T, Rodrigues-Lima F, Jiménez R, Criado FJG, Cenador MBG, Brindle P, Vicente-Dueñas C, Alizadeh A, Sánchez-García I, Green MR. Crebbp loss cooperates with Bcl2 overexpression to promote lymphoma in mice. Blood 129(19):2645-2656, 5/2017. e-Pub 3/2017. PMCID: PMC5428458.
- Mondello P§, Tadros S§, Teater M, Fontan L, Chang A, Jain N, Singh S, Ma M, Yang H, Toska E, Alig S, Durant M, de Stanchina E, Mottok A, Nastoupil L, Neelapu S, Weigert O, Inghirami G, Baselga J, Dogan A, Younes A, Yee C, Scheinberg D, Melnick A*, Green M*. Selective inhibition of HDAC3 targets synthetic vulnerabilities and activates immune surveillance in lymphoma. Cancer Discovery, 2020;10(3):440-459. PMID: 31915197.
- Ma M, Tadros S, Bouska A, Heavican T, Yang H, Deng Q, Moore D, Akhter A, Hartert K, Jain N, Showell J, Ghosh S, Street L, Davidson M, Carey C, Tobin J, Perumal D, Vose J, Lunning M, Sohani A, Chen B, Buckley S, Nastoupil L, Davis R, Westin J, Fowler N, Parekh S, Gandhi M, Neelapu S, Stewart D, Bhalla K, Iqbal J, Greiner T, Rodig S, Mansoor A, Green M. Subtype-specific and co-occurring genetic alterations in B-cell non-Hodgkin lymphoma. Haematologica, 2022;107(3):690-701. PMID: 33792219.
- Jain N§, Hartert K§, Tadros S§, Fiskus W, Havranek O, Ma M, Bouska A, Heavican T, Kumar D, Deng Q, Moore D, Pak C, Liu C, Gentles A, Hartmann E, Kridel R, Smedby K, Juliusson G, Rosenquist R, Gascoyne R, Rosenwald A, Giancotti F, Neelapu S, Westin J, Vose J, Lunning M, Greiner T, Rodig S, Iqbal J, Alizadeh A, Davis R, Bhalla K, Green M. Targetable genetic alterations of TCF4 (E2-2) drive immunoglobulin expression in diffuse large B-cell lymphoma. Sci. Transl. Med. 2019; 11(497): eeav5599. PMID: 31217338. PMCID: PMC6724184.
- Green MR, Monti S, Rodig SJ, Juszczynski P, Currie T, O'Donnell E, Chapuy B, Takeyama K, Neuberg D, Golub TR, Kutok JL, Shipp MA. Integrative analysis reveals selective 9p24.1 amplification, increased PD-1 ligand expression, and further induction via JAK2 in nodular sclerosing Hodgkin lymphoma and primary mediastinal large B-cell lymphoma. Blood 116(17):3268-77, 10/2010. e-Pub 7/2010. PMCID: PMC2995356. (>1,000 citations)
- Han G, Deng Q, Dai E, Dang M, Ma J, Yang H, Kudryashova O, Meerson M, Isaev S, Kotlov N, Nomie K, Bagaev A, Parmar S, Hagemeister F, Ahmed S, Iyer S, Samaniego F, Steiner R, Fayad L, Lee H, Fowler N, Vega F, Flowers C, Strati P, Westin J, Neelapu S, Nastoupil L, Wang L§, Green M§. Follicular Lymphoma Microenvironment Characteristics Associated with Tumor Cell Mutations and MHC Class II Expression. Blood Cancer Discovery, 2022; 3(5):428-443. PMID: 35687817 (§Corresponding authors)
- Yang J, Chen Y, Jing Y, Green M*, Han L*. Advancing CAR T cell therapy through multi-dimensional omics data. Nat. Rev. Clin. Oncol. 2023 (In Press, *corresponding authors) PMID: 36721024
- Deng Q, Han G, Puebla-Osorio N, Ma M, Strati P, Chasen B, Jain N, Yang H, Wang Y, Zhang S, Wang R, Chen R, Showell J, Ghosh S, Patchva S, Zhang Q, Dai E, Hagemeister F, Fayad L, Saminiego F, Lee H, Nastoupil L, Fowler N, Davis R, Westin J, Neelapu S, Wang L, Green M. Characteristics of anti-CD19 CAR T-cell infusion products associated with efficacy and toxicity in patients with large B-cell lymphomas Nat. Med. 2020;26:878-1887. PMID: 33020644.
- Cherng H, Sun R, Sugg B, Irwin R, Le C, Yang H, Deng Q, Fayad L, Fowler N, Parmar S, Steiner R, Hagemeister F, Nair R, Lee H, Rodriguez M, Samaniego F, Iyer S, Flowers C, Wang L, Nastoupil L, Neelapu S, Ahmed S, Strati P, Green M§, Westin J§. Risk assessment with low pass whole genome sequencing of cell free DNA before CD19 CAR T-cells for large B-cell lymphoma. Blood 2022; 140(5):504-515. PMID: 35512184 (§Corresponding authors)
Give Now
Research Areas
Find out about the four types of research taking place at UT MD Anderson.
