Mentored Junior Faculty Fellowship Recipients
Training the next generation is as critical as supporting the current generation. For this reason, the Duncan Family Institute established its Mentored Junior Faculty Fellowship to support the earliest stages of a faculty member’s career and fill that critical gap in funding between a postdoctoral training position and a faculty tenure track position as the assistant professor level. The research of our current fellows ranges from the development of minimally invasive plasma-based biomarker panels for pancreatic ductal adenocarcinoma to investigations into additional risk factors for HPV infection, while looking for novel behavioral interventions for HPV prevention.
Nathan Parker, Ph.D. - Behavioral Science
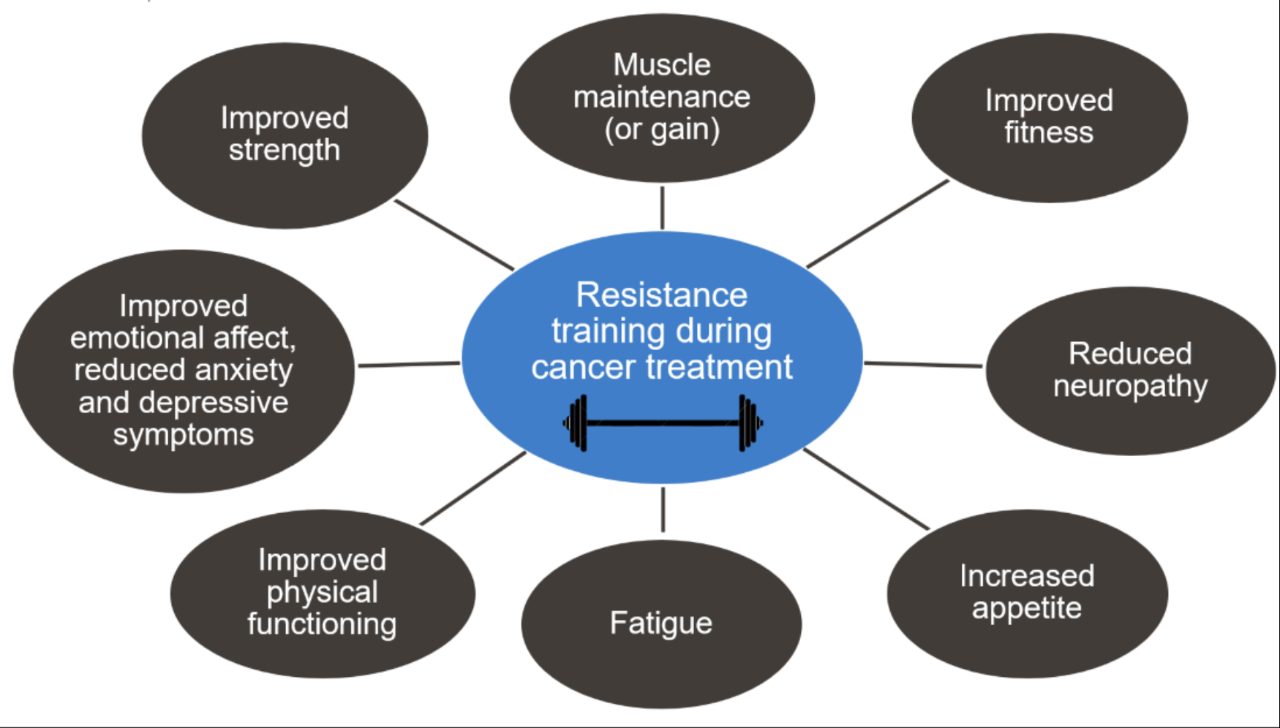
"Resistance Training During Cancer Treatment"
Muscle loss is a hallmark of several cancers and
frequently accelerates during cancer treatments. With the
ever-increasing population of older cancer survivors, it is important
to develop strategies to preserve functional independence and
performance status. Exercise, and particularly resistance training,
has enormous potential to mitigate muscle loss and
accompanying declines in strength, physical functioning, and
health-related quality of life among cancer survivors. In many
survivorship contexts, such as for individuals whose geographic
locations, local treatments, financial situations, or work and family
responsibilities make it difficult to attend in-person exercise
sessions
at major cancer centers, home-based exercise training
is more accessible. Survivors’ preferences also factor into the
feasibility of home-based training. However, unique barriers,
including survivors’ lack of familiarity with resistance training,
necessitate additional support and supervision to
maximize intervention benefits.
Dr. Parker will work to develop a novel and sustainable strategy to improve resistance training adherence and effectiveness among cancer survivors using a tele-supervision strategy. He will utilize video conferencing sessions with certified trainers to deliver and supervise a progressive strength training intervention to individuals undergoing chemotherapy for advanced pancreatic cancer. Dr. Parker will measure the safety, feasibility, and acceptability of the intervention and examine exploratory outcomes such as fitness, fatigue, and quality of life. His long-term goal is to help create permanent role for exercise programming in clinical cancer treatment, and his project is an important initial step in increasing the accessibility of resistance training and its benefits for pancreatic cancer survivors.
Dalnim Cho, Ph.D. - Health Disparities Research

“Improving Lifestyle Behaviors for Racial/Ethnic Minority Survivors and Their Partners”
Despite the fact that healthy lifestyle behaviors such as exercise and healthy diet enhance quality of life and reduce morbidity and mortality rates among cancer survivors, their lifestyle behaviors are far below optimal. Especially, racial/ethnic minority survivors report poorer lifestyle behaviors than non-Hispanic white survivors. However, lifestyle interventions for racial/ethnic minority survivors are seriously lacking and effects of the existing interventions were often small. Innovative lifestyle interventions that have the high potential for increasing lifestyle behaviors adoption and maintenance, potentially reducing health disparities among minority survivors, are urgently needed. Cancer is often considered a “we-disease” as survivors’ health is often tied to their partners’ health and vice versa. Thus, if we include partners into survivorship care, expand the focus of lifestyle interventions from the individual to the survivor-partner couple and target joint behavioral change, lifestyle behaviors may be more easily adopted and potentially maintained.
Dr. Cho is interested in investigating multiple levels of influence such as individual, family/social, and environmental for health and lifestyle behaviors and develop multilevel interventions to maintain behavioral change and reduce unnecessary health disparities. During the DFI fellowship, she will especially focus on the family/social level of influence. She will determine the feasibility of recruiting and implementing a couple-based, culturally-tailored lifestyle intervention among minority survivors and their partners and evaluate its preliminary efficacy in improving physical activity, diet, quality of life, and inflammatory markers. If proven effective, interventions targeting the survivor-partner dyads as a single unit of care may have significant public health impacts by promoting primary and tertiary prevention: decreased likelihood of developing cancer in partners (primary prevention) and decreased likelihood of morbidity and mortality in survivors (tertiary prevention).
Johannes Fahrmann, Ph.D. - Clinical Cancer Prevention

"Metabolomic Profiling for Cancer Risk Assessment and Early Detection"
Achieving significant reductions in cancer mortality will be largely contingent upon realization of improved strategies to determine cancer risk and implementation of preventive intervention strategies. This is exemplified in lung cancer, the leading cause of cancer mortality in both men and women in the United States. While risk factors such as smoking status, age, genetic predisposition and infectious lung diseases are known to increase susceptibility to lung cancer, there is a need to identify additional subjects at increased risk beyond the current risk stratification profiles. The current screening strategy by low-dose computerized tomography (LDCT) is largely confined to high-risk smokers with 30+ packs per year smoking history, current smoking status or having quit in the last 15 years and that are between 55 and 80 years old. However, these criteria are only applicable to ~27% of all lung cancer subjects. Consequently, there is a critical need to identify subjects at increased risk of developing or harboring lung cancer that do not meet current screening criteria. Additionally, despite reductions in mortality, LDCT-positive scans are heavily confounded by high false positive rates (96%) due to its inability to adequately distinguish indolent (benign) solid pulmonary nodules (SPNs) from malignant SPNs. Moreover, over-diagnosis is a major source of controversy surrounding LDCT screening. Thus, there are two distinct but related clinical predicaments: identification of subjects at increased risk of developing lung cancer independent of pack-years of smoking and improved strategies for early diagnosis of lung cancer and stratification of LDCT-positive nodules into benign or malignant SPNs. For these applications there is immediate clinical need for biomarkers with high sensitivity and specificity to effectively reduce mortality through early detection.
Metabolites are small molecules (e.g. <1200 Da) and biochemical intermediates (metabolites) that serve as the end-products of cellular processes, highly responsive to both pathological and environmental stimuli and, as such, are particularly well suited for biomarker discovery to address clinical needs such as those mentioned above. Metabolomics represents a global unbiased approach to the profiling of such small molecules.
Using metabolomics technology as his primary platform, Dr. Fahrmann will pursue a research path aimed at the development of minimally invasive plasma-derived biomarker panels for lung cancer risk assessment and early detection. Achieving this global goal will have significant implications on reducing lung cancer mortality and guiding treatment strategies. Of special interest is the integration of metabolomics with other ‘omic’ technologies and basic research methodologies to better link observations in blood to tumor origin, thereby increasing the robustness of candidate biomarkers and their probability of successful translation into clinical utility.
Yue Liao, Ph.D. - Behavioral Science

"Use Wearable Sensor Technologies to Develop Next-gen Cancer Prevention Interventions"
High levels of blood glucose and insulin are associated with an increased risk of developing several types of cancers, such as the breast, endometrium, colon, liver, kidney, and pancreas. In addition to avoiding foods (e.g., sugar sweetened foods and beverages) that could lead to a spike in blood glucose levels, physical activity (ranging from a 10-minute session of high-intensity workout to half-hour slow walking) or mere interruption of prolonged sitting have shown effects in reducing post-meal blood glucose and glucose variability within the following day. Besides the acute beneficial changes in glucose levels, regular physical activity also improves functional and mental well-being, helps with weight management, and prevents a number of chronic diseases such as type 2 diabetes and cardiovascular disease. However, about half of American adults are not sufficiently active to achieve these health benefits.
Dr. Liao’s research focus on developing personalized and adaptive behavioral interventions using mobile and wearable sensor technologies. Her project aims to incorporate wearable body sensors to provide objective and actionable data on the biological antecedents and consequences of daily physical activity and sedentary behaviors. Dr. Liao plans to integrate data from continuous glucose monitors and heart rate monitors to educate high-risk population (i.e., overweight and obese prediabetics) about the acute benefits of physical activity and increase their motivation in physical activity engagement. Dr. Liao’s research goal is to provide insights and guidance at critical decision points to help individuals modify their daily health-related behaviors to reduce their cancer risks.
Michela Capello, Ph.D. - Clinical Cancer Prevention

"Challenges and Opportunities to Reduce Mortality Associated with Pancreatic Cancer"
Reduction in cancer mortality requires significant advances in risk assessment, preventive interventions, and early detection. This is particularly applicable to pancreatic ductal adenocarcinoma (PDAC), which, with a 5-year survival rate of 7% and a mortality rate comparable to its incidence rate, represents the fourth leading cause of cancer death in the United States. 15-20% of PDAC patients present with localized disease and have a 5-year survival rate approaching 30%, suggesting that mortality could be reduced by early diagnosis. Given the low incidence of disease, imaging technologies such as CT/MRI/EUS are not practical in terms of cost effectiveness and invasiveness for screening. The only accepted blood based biomarker for PDAC, CA19-9, is informative for symptomatic PDAC patients, but lacks specificity needed for early detection in asymptomatic subjects.
Dr. Capello will pursue a research path aimed at the development of minimally invasive plasma-based biomarker panels for PDAC risk assessment and early detection. Success in this endeavor will further allow pursuit of research beyond early detection and address the more challenging goal of preventive intervention. Achieving these objectives will have a significant impact on reducing PDAC mortality. Of special interest is profiling the anti-tumor immune response as a source of biomarkers in the form of autoantibodies to tumor antigens. Identification of such antigens could also allow for development of immunotherapeutic approaches and vaccines.
Matthew Cox, Ph.D. - Behavioral Science

"Cancer Prevention Through Physical Activity: Optimizing a Self-regulation Intervention"
Exercise has been shown to decrease the risk of colon, endometrial, and breast cancer. Despite the positive effects of physical activity (PA), PA levels among Americans remain low. The current recommendations for PA in healthy individuals is 150-250 min/week in order to prevent weight gain receive and other health benefits. Estimates from 2012 suggest that only 48% of Americans report they are meeting the minimum recommended levels of PA and 23% say they do not engage in any physical activity. However, self-reporting of PA is often exaggerated and a study using objectively measured PA via accelerometers identified less than 4% of adults engaging in the recommended levels. African Americans in particular have been shown to be less physically active and more obese compared to non-African Americans.
Dr. Cox' research, will design an intervention targeting self-regulation for PA and develop and test this intervention using the Multiphase Optimization Strategy (MOST) to create a culturally-relevant optimized intervention for PA among sedentary African-Americans. By giving several previously developed measures of self-regulation for PA, he will identify overlap and discrepancies between questions and constructs of self-regulation in order to fully separate and identify the relevant constructs related to PA. Hypothesized constructs include goal setting, goal planning, self-monitoring, feedback, and managing barriers to achieving goals, just to name a few. MOST is an engineering-based design that tests individual intervention components via randomized control trials. Utilizing the MOST design will allow examination the individual effects, and the interaction effects among the constructs. This line of research has great potential for optimizing the effectiveness of interventions to increase physical activity, thus reducing risk of some of the most common cancers in the US. Dr. Cox' research goal is to identify the causal mechanism of PA interventions so as to create the most effective interventions for cancer prevention.
Thanh Bui, M.D., Dr.P.H. - Behavioral Science

"Hygienic Sexual Practices and HPV Prevention"
Infection with human papillomavirus (HPV) is an established cause of more than 30,000 cases of cancers each year in the United States (US), including cancers of the cervix, vagina, vulva, penis, oropharynx and anal canal. Typical risk factors associated with oral HPV infection include oral sex, number of lifetime sex partners, and cigarette smoking. One major “frame” in HPV research is that HPV is often considered a sexually transmitted infection (STI), and it is the most common STI in the world. Although this is true, viewing HPV in this manner is somewhat constraining because it drives the focus of intervention research on safe sexual practices (e.g. condom use, reducing numbers of sexual partners), and other means of preventing HPV transmission than safe sex then remain unexplored or underemphasized.
Dr. Bui’s main research focus is to explore additional risk factors for HPV infection, and to look for novel behavioral interventions for HPV prevention. Specifically, Dr. Bui’s research examines the effect of hygiene practices and their interactions with sexual practices on HPV infection at different body sites. Examining these behavioral factors is important because they are all modifiable. Thus, the research’s results will inform future novel widely-usable interventions to change the behaviors in order to reduce HPV infection, persistence, and subsequent HPV-related cancers. Dr. Bui is also interested in applying innovation generation tools to the development and assessment of other behavioral interventions to promote early cancer prevention.
Diana Hoover, Ph.D. - Health Disparities Research

"Reducing Tobacco-Related Cancer Disparities in the Underserved"
One-third of U.S. cancer-related deaths and 90% of lung cancer cases result from tobacco smoking. Although smoking prevalence has declined in recent years, it remains high for certain populations such as racial/ethnic minorities and those with low income, education, and employment. Such high-risk groups are less likely to quit smoking and often have less access to cessation resources. Thus, smoking has a major impact on cancer-related morbidity and mortality within these vulnerable populations.
The primary focus of Dr. Hoover’s research project is to evaluate a model exploring mediators (i.e., depression, social support)of the relation between health literacy and smoking cessation outcomes in low-SES, racially/ethnically diverse smokers enrolled in cessation treatment. Findings will elucidate the effects of health literacy on depression and cessation outcomes, and will be critical for informing and improving cessation programs, thus reducing tobacco-related health disparities. Dr. Hoover is also conducting a qualitative study to examine ways of enhancing the adoption and implementation of Ask Advise Connect (AAC), an evidence-based approach linking smokers in healthcare settings with treatment, in the Harris Health System community health centers. These findings have the potential to increase cessation rates at the population level.
Meng Chen, Ph.D. - Epidemiology

“Gene set enrichment analysis of bladder cancer genome wide scan”
Bladder cancer is the fourth most common cancer in men in the United States. It is an excellent model of studying genetic susceptibility and gene-environmental interaction. Smoking is responsible for about half of all the bladder cancer cases and occupational exposure accounts for approximately one fifth of the cases. Candidate gene approach has shown that genetic variants in carcinogen metabolism genes (e.g., NAT2 and GSTM1) predispose individuals to bladder cancer. Recent genome wide association studies (GWAS) have identified over 10 additional novel bladder cancer susceptibility loci. However, these confirmed bladder cancer susceptibility loci only explain a small fraction of the genetic heritability of bladder cancer. Identifying additional loci through innovative approaches is needed. Dr. Meng Chen has been involved in bladder cancer susceptibility, gene-smoking interaction, and clinical outcome research for several years by using candidate gene, pathway-based, and GWAS approaches. She will continue to focus on bladder cancer susceptibility study during her Duncan fellowship. One of her particular interests is to finding novel genes and pathways involved in bladder cancer susceptibility through the gene-set enrichment analysis (GSEA). A recurring problem in traditional GWAS analysis (i.e., single SNP analysis) is the lack of consideration of biological pathways that contain network of genes with subtle, undetectable effect at single SNP or single gene level. Application of innovative secondary analyses focusing on genes and pathways will complement and expand traditional GWAS analysis and identify genes and pathways that associate with bladder cancer risk. Dr. Chen has explored the genome wide scan data from MD Anderson bladder cancer case control study, the largest bladder cancer case-control study in U.S., to identify critical and novel pathways involved in bladder cancer etiology. She will validate her findings in independent populations. She will further analyze gene-gene and gene-environment interaction, and cumulative effect of these identified pathways.
The completion of this study may not only enhance the understanding of the overall gene networks involved in bladder cancer susceptibility but also offer additional etiologic insights highlighting the specific genes and pathways involved. It may identify druggable targets for cancer prevention and treatment and potentially improve the risk prediction model of bladder cancer. GSEA (gene set enrichment analysis) method will be a complementary tool to identify the “missing heritability” from previous GWAS, and can be widely applied in cancer association study and clinical outcome study.
Claire Adams, Ph.D. - Health Disparities Research

“Mindfulness-Based Strategies for Improving Cancer Risk Behaviors”
Tobacco use, alcohol use, and unhealthy eating have each been linked to increased risk of cancer and/or cancer-related mortality. Because these health risk behaviors tend to cluster together (e.g., smokers display more, and more serious, health risk behaviors than nonsmokers), there is an urgent need to target multiple health risk behaviors to prevent cancer. Dr. Adams' research seeks to inform behavioral interventions to reduce unhealthy behaviors (i.e., smoking, at-risk alcohol use, and unhealthy eating) linked to cancer risk and cancer-related mortality. She is interested in commonalities underlying disparate health risk behaviors and targeting these shared pathways to improve evidence-based interventions for multiple health behavior change (MHBC). In particular, her work focuses on mindfulness (paying attention to present-moment experience with an attitude of non-judgment and acceptance) as one promising avenue for targeting multiple health risk behaviors. Although preliminary research supports mindfulness-based treatments for improving smoking cessation, reducing relapse to alcohol use disorders, and promoting healthier eating, this area of research is in its infancy, and the mechanisms of mindfulness for health behavior change are unclear. There is also a lack of research on mindfulness in racial/ethnic minorities, who often have higher rates of cancer risk and related mortality.
Dr. Adams' research centers on developing and testing a moderated mediation model of mindfulness, negative affect, and health behavior to integrate different lines of mindfulness and health behavior research, elucidate mechanisms of mindfulness, and apply to racially/ethnically diverse populations.
Jian Wang, Ph.D. - Epidemiology

“Risk modeling using mediation analysis and Bayesian network recovery with application to smoking cessation study”
There are evidences that cigarette smoking is associated with cancers of lung, oral cavity, bladder, kidney, pancreas, stomach, etc. Smoking cessation results in decreased incidence and mortality from cancers, and therefore, is an important component of cancer prevention. Despite ever-increasing anti-smoking legislation and social pressure, the proportion of successful smoking cessation attempts is still low. Over 40% of current smokers make a serious cessation attempt each year, but only less than 3% of them successfully quit. The success of smoking cessation is associated with various genetic risk factors (e.g. genes related to dopamine pathways and nicotinic receptors), pharmacological treatments (e.g. bupropion), as well as the negative affect caused by quitting attempts (e.g. depression, irritation, and nervousness). The identification of novel risk factors and their interactions (gene-gene and gene-environmental interactions) can help our overall understanding of the complex mechanism for nicotine dependence, and therefore, help identify individuals at highest risk for the nicotine addition and response to therapy on the basis of their personal exposure patterns and their genetic risk profiles. The gene-environmental interaction is often defined as joint participation in the causal mechanism leading to disease. But more complex interactions exist, such as genetic factors that have no impact on disease risk alone but become risk factors when combined with environmental factors or genetic factors that have an impact on disease by dual pathways, independently and through interaction with environmental factors. Therefore, it is crucial to identify the complex relationships among risk factors and their effects on smoking cessation.
Dr. Wang’s research proposes to develop new statistical approaches for modeling the risk of smoking cessation, which will identify the complex relationships among genetic variants, environmental risk factors (e.g., number of smokers in family and social context), and smoking cessation based on two rigorous statistical approaches: mediation analysis and Bayesian network recovery approaches. Specifically, she will identify the mediating/moderating effects of the negative affect due to quitting attempts and pharmacological treatments on the association between genetic variants and smoking cessation. The resulting statistical model will provide a novel tool for the development and tailoring of both prevention strategies for individuals at risk and effective pharmacologic interventions for current smokers and, therefore, contribute to the prevention of related cancers.
Larkin Strong, Ph.D. - Health Disparities Research

"An ecological approach to cancer prevention: Reducing disparities in physical activity through research and action"
Physical inactivity represents one of the few modifiable risk factors for cancer. Regular physical activity is associated with a reduced risk of breast and colon cancers and has also been linked to reductions in prostate, lung, and endometrial cancer risk. Inactivity is also an important determinant of overweight and obesity, which are believed to contribute to 15-20% of all cancer deaths in the U.S. Given that physical activity behaviors established in youth may continue into adulthood, enhancing physical activity in youth has the potential to greatly reduce the cancer burden in the U.S through direct and indirect pathways. Furthermore, since physical activity tends to decline dramatically during adolescence, adolescence represents a critical age during which to identify the factors that contribute to or inhibit participation in physical activity.
The focus of Dr. Strong’s research project is to delineate how factors at different levels influence adolescent physical activity (PA) behaviors in a group of 1,154 Mexican American adolescents in Houston, TX, drawn from the Duncan Family Institute’s Mexican American Cohort. In this research project, Dr. Strong and colleagues seek to understand the independent contributions and interactions of multiple factors on physical activity: adolescent characteristics & behaviors, parental characteristics and behaviors, neighborhood socioeconomic context and density of neighborhood PA resources; and identify potential targets for interventions to enhance physical activity in this population. By drawing on unique data that includes parental and adolescent measures of linguistic and behavioral acculturation and characteristics of adolescents’ neighborhood environments, findings from this research will have important implications for the design of family-based physical activity interventions for Mexican American families and will help to identify the importance of community physical activity resources to adolescent physical activity. Furthermore, this research may identify segments of the population who may be more affected by local environmental features, helping policy makers and funders target public health investments to where they will have the greatest impact.
Francesco Versace, Ph.D. - Behavioral Science

“Putting smoking addiction in the affective context: Event-related potentials to emotional and neutral stimuli during a smoking cessation intervention”
Tobacco use is associated with approximately 80 percent of all lung cancer deaths and increases the risk of many other types of cancer, including cancers of the throat, mouth, pancreas, kidney, bladder and cervix (NCI, 2008). Although the harmful effects of tobacco on human health have been known since the 1964 Surgeon General Report (Smoking and Health, 1964), approximately 20% of USA population continue to smoke (CDC, 2007). In fact, most smokers identify tobacco use as harmful and express a desire to reduce or stop using it. For example, annually nearly 35 million smokers express a desire to quit in national surveys. Unfortunately, more than 85 % of those who actually try to quit on their own will relapse, often within the first week following the cessation attempt (NIDA, 2009). The reasons underlying the maintenance of addiction are diverse, but most theoretical models attribute the difficulties in quitting to the smoker’s altered emotional processes. Where theories differ is in the different emphasis that they attribute to specific emotional components to explain drug addiction and relapse.
The overarching theme of Dr. Versace’s research and the project described here is to investigate the role that emotional processes have in smoking addiction and relapse by taking advantage of the theoretical models, the experimental designs, and the measurement techniques developed within the field of affective neuroscience. Specifically, Dr. Versace and colleagues will evaluate attentional and emotional processes in the presence of cigarette-related and other intrinsically motivating cues using event-related brain potentials (ERP). These ERP assessments will be carried out before and after a smoking cessation and will allow the evaluation of pharmacological smoking cessation aids (varenicline, bupropion and placebo) and their altering effects on emotional processes.
Our Labs
Learn more about our faculty and research taking place in our labs.
Conferences
View conferences available for continuing education credit.
