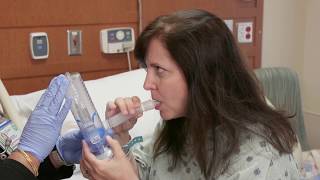
Research

Gynecologic Oncology and Reproductive Medicine focuses on providing exceptional patient care while linking basic science with clinical and translational research to develop the next generation of innovative approaches to the treatment and prevention of gynecologic cancers.
From our work on the HPV-related cancers to the development of the Anderson Algorithm and implementation of our Enhanced Recovery After Surgery (ERAS) program, our pioneering research aims to rapidly translate new knowledge into clinical trials for improved treatment or prevention strategies.
Developmental therapeutics & immunotherapy
Focused on innovation in cancer treatment, the Gynecologic Oncology and Reproductive Medicine department has a robust portfolio of ongoing clinical trials. Our researchers are developing new agents for the treatment of ovarian cancer, recurrent and advanced endometrial cancer, conservative treatment and management of precancerous lesions, and using the exciting new approach of immunotherapy to improve responses across disease sites.
Read more about our current clinical trials.
Innovative surgery
The Gynecologic Oncology and Reproductive Medicine department is leading in surgical research with a series of ongoing trials to advance treatment options for gynecologic cancer patients and improve their quality of life. Our surgeons focus on improving outcomes by minimally invasive or advanced robotic techniques.
Since the initiation of the Innovative Surgery Working Group in 2005, the department and its investigators have generated a significant number of multi-institutional studies with high scientific impact.
Among the current surgical studies is sentinel lymph node (SLN) surgery for women with high-risk endometrial cancers. The less-invasive procedure could serve as a staging tool for endometrial cancers, decrease morbidity and change the standard of care.
Additionally, the team is conducting a prospective randomized clinical trial of laparoscopic or robotic radical hysterectomy versus abdominal radical hysterectomy in patients with early stage cervical cancer, evaluating recurrence-free survival and overall survival.
The Enhanced Recovery After Surgery (ERAS) program in Gynecologic Oncology was implemented in November 2014 as a quality improvement initiative with an important goal in mind: to optimize perioperative outcomes for cancer patients. The program uses evidence-based practice and innovative research to enhance recovery after surgery.
Health Services Research
The multidisciplinary field of health services research explores the delivery of care, improving access to care in underserved populations, patient-reported outcomes and survivorship. The driving force behind this extensive research is improving the patient experience.
Prevention
Providing comprehensive care means our researchers investigate all facets of gynecologic cancer, including prevention. Prevention research is key to reducing the number of women diagnosed with gynecologic cancers worldwide.
The department's prevention services include:
- Colposcopy clinic for pre-invasive cervix, vaginal and vulvar disease
- High-risk clinic for women at inherited risk for ovarian and endometrial cancer
- Education and HPV vaccination clinics for HPV-related cancers
- Global initiatives to assist low- and middle-income countries in their efforts to prevent and diagnose cervical cancer
Additionally, the department has an Oncofertility clinic to give men and women options to preserve fertility before cancer treatment.
Basic Science & Translational Research
With the goal of improving treatment or prevention strategies, our clinically-driven basic science investigators have a mature research portfolio which includes:
- Microenvironment - exploring the interaction between the tumor and its surroundings
- Biology – angiogenesis, nanoparticles for delivery of therapeutics
- Hereditary cancer syndromes – understanding the genetics of risk and mechanisms of prevention
- Biology of rare tumors
ERAS GYN Program by the Numbers
25%
reduction in length of stay
72%
reduction in postoperative opioid consumption
14%
decrease in cost of perioperative care
ERAS GYN Program
Overview
The Enhanced Recovery After Surgery (ERAS) program in Gynecologic Oncology, led by Larissa A. Meyer, M.D., M.P.H., was implemented in November 2014 as a quality improvement initiative with an important goal in mind: to optimize perioperative outcomes for cancer patients. The program uses evidence-based practice and innovative research to enhance recovery after surgery.
Due to its comprehensive scope spanning the entire perioperative period, our dedicated ERAS team is a multidisciplinary group including gynecologic oncologists, anesthesiologists, nurses, pharmacists, physical therapy teams, nutritionists, research data coordinators and statisticians.
The ERAS Program in Gynecologic Oncology was initially implemented on all open surgeries, and expanded to minimally invasive surgery in February 2017. Currently, all patients undergoing open, laparoscopic or robotic surgery in our department are on the ERAS program. To date, we have operated on over 1,200 patients.
Patients undergoing care under the ERAS program benefit from shorter patient stays, improved patient-reported outcomes, decreased postoperative opioid consumption and reduced costs. These successes have led to the implementation of ERAS as the standard of care in surgery in Gynecologic Oncology at MD Anderson.
Videos
Previous Practice vs. ERAS GYN
Pre-op |
Previous Practice |
ERAS GYN |
| Diet | NPO @ MN until surgery |
Nutritional counseling, no solids after midnight, clear liquids 2 hours prior to surgery, carbohydrate loading |
| Bowel preps | Physician discretion | None |
| Pre-meds | Anesthesia discretion | Tramadol (Ultram), Pregabalin (Lyrica), Celecoxib (Celebrex), Acetaminophen, Heparin |
| IVF therapy | Fluids after IV place | Saline lock IV |
Intra-op |
Previous Practice |
ERAS GYN |
| Antibiotics | Prophylaxis per ACOG guidelines | Neomycin PO*, Metronidazole PO*, Ertapenem IV [*Anticipated bowel procedures] |
| Anesthesia | Anesthesia discretion | Total intravenous anesthesia, no epidurals, local wound infiltration |
| IVF therapy | Anesthesia discretion | Goal-directed (non-invasive cardiac monitoring) |
| NGT/drain placement | Surgeon discretion | None |
| Foley catheter | Physician discretion | Remove POD1 |
Post-op |
Previous Practice |
ERAS GYN |
| IVF therapy | IVFs 100mL/h | IVFs 40mL/h |
| Analgesia | Patient control analgesia vs. epidural | Acetaminophen, Ibuprofen, Pregabalin, Oxycodone, Hydromorphone IV |
| Diet | Gradual advancement at physician discretion | Dietitian counseling, regular diet POD0, oral hydration |
| Ambulation | Patient and physician discretion | Ambulate 8x/day, all meals in chairs, out of bed 8h/daily |
| Transfusions | Physician discretion | Restrictive, transfuse for Hb < 7 |
| Abbreviations: NPO, nothing by mouth; MN, midnight; IVF, intravenous fluids; ACOG, American Congress of Obstetricians and Gynecologists; PO, by mouth; POD, post-operative day; PCA, patient control analgesia; Hb, hemoglobin. |
||
Publications
Members of our ERAS team have contributed to a number of high-impact publications, including:
- Guidelines for pre- and intra-operative care in gynecologic/oncology surgery: Enhanced Recovery After Surgery (ERAS®) Society recommendations - Part I
- Guidelines for postoperative care in gynecologic/oncology surgery: Enhanced Recovery After Surgery (ERAS®) Society recommendations - Part II
- A call for new standard of care in perioperative gynecologic oncology practice: Impact of enhanced recovery after surgery (ERAS) programs
- Perioperative trajectory of patient reported symptoms: A pilot study in gynecologic oncology patients
- Enhanced recovery after surgery (ERAS®) in gynecologic oncology - Practical considerations for program development
- Effect of Enhanced Recovery After Surgery Program on Opioid Use and Patient-Reported Outcomes
Funding
- Marie Hall Foundation award to fund the Gyn Onc ERAS program through clinical, research and training support
- NIH R01 grant: Improving Recovery After Major Surgery Using Patient-Reported Outcomes. R01CA205146. PI: Xin Shelley Wang
- Minimally invasive gynecologic surgery: Can further improvements in recovery be made? MD Anderson Minimally Invasive Technology Oncologic Surgery (MINTOS) Program, 6/1/2015-5/31/2016, PI: Larissa Meyer
- MD Anderson Holiday Giving Program grant to fund "ERAS and the Road to Recovery" patient education video
- Foundation for Women's Cancer: "Randomized pilot of self-hypnosis to improve post-operative pain outcomes and reduce opois intake in an ERAS program"
Clinical Trials
- HERO trial: The goal of this clinical research study is to evaluate the use of self-hypnosis/guided relaxation prior to surgery to improve pain and anxiety associated ith surgery. This trial is open to women undergoing OPEN gynecologic oncology surgery.
Retrospective
- PA16-0939 Assessing Compliance with an Enhanced Recovery After Surgery (ERAS) Program after Gynecologic Surgery
- PA16-0082 Implementation of an Enhanced Recovery After Surgery (ERAS) Program: How much did intra-operative opioid administration decrease in first year post implementation
- PA16-0076 Implementation of an Enhanced Recovery After Surgery (ERAS) Program: An approach for all ages or just for the young at heart?
- PA16-0079 A comprehensive evaluation of different risk-assessment models to predict 30-day postoperative complications in gynecologic oncology patients undergoing surgery under an Enhanced Recovery After Surgery (ERAS) Program
- PA16-0080 Bowel surgery in an Enhanced Recovery After Surgery (ERAS) Program for gynecologic oncology surgery: Is recovery still enhanced or a need to take a step back?
- PA16-0077 Correlation of body mass index (BMI) and perioperative outcomes in patients on an Enhanced Recovery After Surgery (ERAS) Program: Are the obese patients at a disadvantage or do all share the same benefit?
- PA16-0078 Impact of an Enhanced Recovery After Surgery (ERAS) Program on postoperative renal function: Is euvolemia ideal for all or only a select few?
- PA16-0086 Implementation of an Enhanced Recovery After Surgery (ERAS) Program: Has the development of a preoperative order set improved compliance for preventive analgesia and deep venous thromboembolic (DVT) prophylaxis?
- PA17-0049 Implementation of an Enhanced Recovery After Surgery (ERAS) Program: Impact on Return to Intended Oncologic Therapy (RIOT)
Completed
- PACIRA - The goal of this clinical research study is to compare the effects of bupivacaine to those of liposomal bupivacaine when given to patients who are having gynecologic surgery. Researchers are seeking to determine whether liposomal bupivacaine can decrease the amount of opioids used by patients after surgery. In addition, they seek to determine the impact of liposomal bupivacaine on Patient Reported Outcomes in the postoperative period.
Resources
- ERAS® Society website
- REDCap (ERAS-GYN program database)
- ERAS TED talk by Olle Ljungqvist, M.D., Ph.D.
FAQ
What is ERAS?
ERAS stands for Enhanced Recovery After Surgery. It is a care pathway designed to help prepare your body for surgery, recover better and safer from surgery, and get you home as soon as possible after surgery.
How is ERAS different from a non-ERAS surgery?
There are 3 key parts to the ERAS pathway that make it different:
1) It requires less time for fasting (eating and drinking) and includes a special carbohydrate drink before surgery.
2) We use non-narcotic pain medicines to keep your pain level under control before and after surgery.
3) You are able to eat, drink and resume activity as soon as possible after surgery.
Will my doctor use ERAS?
All MD Anderson patients undergoing elective gynecologic surgery receive care under the ERAS pathway.
What do I need to do before my ERAS surgery?
At your preoperative visit, a nurse will explain your role in the ERAS pathway. You will receive information and education about what to expect before, during and after your ERAS surgery. If you smoke or drink alcohol, we strongly suggest you to stop before surgery. Programs are available to help you stop smoking. Ask your doctor or nurse for more information.
Unless you have certain nutrition precautions, we will instruct you to drink a special carbohydrate drink (100 grams) the night before surgery and a second one (50 grams) 2 hours before you arrive for surgery. Please refer to the nutrition section for more information about nutrition precautions and the carbohydrate drink.
Please note that no bowel preparation is required before your surgery, unless your doctor instructs otherwise.
What happens before I go into the operating room (OR) and during my ERAS surgery?
We will take you to the preoperative holding area to begin your non-narcotic pain medicines. By starting these medicines early, we help to reduce the amount of narcotic medicine you will need during your surgery, as well as the amount of non-narcotic pain medicines after surgery. Our goal is to use short-acting medicines to help speed up your recovery time from the anesthesia, so you can begin your recovery from the surgery sooner.
The anesthesia team will begin the medicines to keep you asleep and comfortable. Warm blankets, warm IV fluids and air warmers are used to keep you warm. You may also receive other medicines during your surgery to help control your blood pressure and prevent nausea and vomiting after surgery.
We will use goal-directed fluid therapy to give you the precise amount of fluids you need during your surgery.
What medicines are used to treat pain?
The primary cause of pain is inflammation. Therefore, we will use medicines that treat inflammation for your pain. These medicines may include: Tylenol® (acetaminophen), Celebrex® (celecoxib), Lyrica® (pregabalin), and Toradol® (ketorolac). During surgery, you will receive local anesthetics that will be injected into your incision. This will help with pain control. You may be given other pain medicines, like narcotics, if you need them for pain. Your medical team will work with you on which combination of medicines will be best for you.
What happens after my ERAS surgery?
After surgery, your active participation is vital. We will encourage you to be out of bed as much as possible and to eat all your meals while seated in a chair. You will be asked to walk 8 times per day. Food and fluid intake will start about 4 hours after surgery. You will be on a special diet of bland, low fat and low fiber food. A dietitian will visit with you in your hospital room to help you with your diet and any other nutrition issues you may have. Your urinary catheter will be removed the next day after surgery, unless there is a medical reason to leave it.
How does ERAS benefit me?
Most patients in our ERAS program experience the following benefits:
- Have a shorter hospital stay after surgery. For example, most ERAS patients go home in 3 days versus 4 days for non-ERAS patients.
- Take less narcotic pain medicine during their hospital stay and are able to manage their pain comfortably.
- Have fewer problems with nausea, sleep, constipation, sudden urge to urinate and difficulty with memory during their hospital stay,
- Have shown better recovery outcomes and less problems returning to their daily life after surgery.
What happens when I go home?
When you are discharged to go home, you will follow a specific plan to help with your recovery. This plan includes:
- Managing your pain with non-narcotic pain medicine
- Eating a diet that excludes high-fat, fried, greasy and spicy foods and foods that are high in fiber and added sugar for 1 to 2 weeks after surgery. We suggest drinking at least 8 eight-ounce glasses of water a day.
- Walking a little more each day as this helps with the healing process.
Where can I find more information about ERAS?
Visit http://erassociety.org/ to learn more about Enhanced Recovery After Surgery.
Larissa Meyer, M.D.
Gynecologic Oncologist
Javier Lasala, M.D.
Anesthesiologist
Gabriel Mena, M.D.
Anesthesiologist
Katy French, M.D.
Anesthesiologist/Prehabilitation Program
An Thuy Huang, D.O.
Prehabilitation Program
Katie Cain
Clinical Pharmacy Specialist
Lorenzo Cohen, Ph.D.
Integrative Medicine
Melinda Harris
Outpatient Advanced Practice Registered Nurse
Lakisha Washington
Inpatient Nurse
Grace Kilikadavil
Inpatient Nurse
Alita Campbell
PACU Nurse
Mark Munsell
Statistician
Maria Iniesta-Donate
Research Team
Tina Suki
Research Team
Gladys Estrada
Research Team
Support
To make a donation to the ERAS program in Gynecologic Oncology:
1. Access the online Donation Form and enter the desired amount.
2. In the billing information area, select "I'd like to choose where my donation will go."
3. In the "Select an Option" drop-down menu, choose "Other."
4. In the box that appears, type: Enhanced Recovery Program – Larissa Meyer
5. Complete the payment information and click the red "Give Now" button to complete your contribution.
Contact
For more information, email our team:
EnhancedRecovery_GYN@mdanderson.org
Give Now
Research Areas
Find out about the four types of research taking place at UT MD Anderson.